

Original Article - Year 2012 - Volume 27 -
Comparative analysis of the evolution and postoperative complications of body contouring plastic surgeries after massive weight loss in young and elderly patients
Análise comparativa da evolução e das complicações pós-operatórias nas cirurgias plásticas do contorno corporal em pacientes idosos e jovens com perda ponderal maciça
ABSTRACT
BACKGROUND: Increasing numbers of procedures are being used to treat elderly ex-obese patients after bariatric therapies. However, reliable data regarding the evolution and complications of this population are scarce in the literature. In this study, we aimed to analyze the evolution and complications of abdominoplasty performed in patients with advanced age after massive weight loss and compare them to the corresponding data from younger patients. Methods: We retrospectively reviewed patients who experienced massive weight loss and underwent surgery for abdominal contouring between July 2005 and July 2011 in the State Hospital Sapopemba (HESAP). An age of > 60 years was used as a criterion for advanced age, in order to divide patients into groups to analyze the postoperative period and complications of abdominoplasty performed after massive weight loss.
RESULTS: We analyzed 264 patients, 19 of whom were 60-75 years of age (Group I) and 245 of whom were 22-59 years of age (Group J). Group I had a major complication rate of 10.5% (P > 0.999) and a minor complication rate of 41.1% (P = 0.280), whereas Group J had a major complication rate of 10.6% (P > 0.999) and a minor complication rate of 30.2% (P = 0.280).
CONCLUSIONS: Patients > 60 years of age do not have a higher rate of complications than younger patients after abdominoplasty.
Keywords: Plastic surgery. Bariatric surgery. Aged. Obesity.
RESUMO
INTRODUÇÃO: Os procedimentos aplicados a pacientes ex-obesos idosos após terapêuticas bariátricas estão em ascensão. Dados fidedignos quanto à evolução e às complicações nesse grupo populacional ainda são escassos na literatura. O objetivo do presente estudo é analisar a evolução e as complicações em abdominoplastias realizadas em pacientes com idade mais avançada após perda ponderal maciça, e compará-las às de pacientes mais jovens.
MÉTODO: Foram analisados, retrospectivamente, pacientes com perda ponderal maciça submetidos a cirurgia para contorno da região abdominal, entre julho de 2005 e julho de 2011, no Hospital Estadual Sapopemba (HESAP). Como critério para divisão dos grupos, a fim de analisar o período pós-operatório e as complicações das abdominoplastias realizadas após perda ponderal maciça, foi estabelecida idade > 60 anos. Resultados: Foram analisados 264 pacientes, 19 deles com idade entre 60 anos e 75 anos (grupo I) e 245 entre 22 anos e 59 anos (grupo J). O grupo I apresentou 10,5% de complicações maiores (P > 0,999) e 41,1% de complicações menores (P = 0,280), enquanto o grupo J obteve 10,6% de complicações maiores (P > 0,999) e 30,2% de complicações menores (P = 0,280).
CONCLUSÕES: Os pacientes com > 60 anos de idade não apresentaram maior número de complicações que o grupo mais jovem.
Palavras-chave: Cirurgia plástica. Cirurgia bariátrica. Idoso. Obesidade.
Bariatric surgery is one of the treatments for morbid obesity1. After massive weight loss, patients commonly experience distorted body contouring due to excessive sagging skin. Plastic surgery is used to treat these deformities2.
Progressive increases in life expectancy accompanied by decreases in fertility and mortality have led to a sharp change in the age composition of the population in our country, highlighting the number of individuals aged > 60 years and > 80 years, and those who are centenarians.
The Brazilian Institute of Geography and Statistics (IBGE) conducted 2 nutritional surveys at the population level in the years 1974-1975 and 2002-2003, which showed a distinct change in standard food and nutrition practices over the past 29 years. The data show that the combined prevalence of overweight and obesity is approximately 60% for men and women; this is also noted for individuals in their late 80s3. Accordingly, the number of procedures that are used to treat elderly ex-obese patients after bariatric therapies is increasing. However, reliable data regarding outcomes and complications in this population are scarce in the literature4. Therefore, in this study, we aimed to analyze the evolution and complications of abdominoplasty performed in patients with advanced age after massive weight loss and compare them to the corresponding data from younger patients.
METHODS
We retrospectively analyzed patients who underwent surgery for abdominal contouring between July 2005 and July 2011. All surgeries were performed by the same professional team at Hospital Estadual Sapopemba, with the plastic surgery group consisting of doctors from the Faculdade de Medicina da Universidade de São Paulo.
We analyzed a total of 264 patients who underwent abdominoplasty. We used the anchor-line or classic technique depending on the degree of sagging5. Among the patients studied, 95.5% previously underwent gastric bypass (with clinical evidence of technical success), whereas the other 4.5% experienced non-surgical weight loss. Each patient must have maintained their weight loss for at least 6 months for inclusion into the study.
To analyze the postoperative period and complications of abdominoplasty performed after massive weight loss, a cutoff of 60 years of age was established to create the groups. Fisher's exact test (test of association) was used to analyze the data, whereas the chi-square test was used to analyze minor complications.
RESULTS
We analyzed a total of 264 patients; of these, 19 were 60-75 years of age (Group I) and 245 were 22-59 years of age (Group J).
The average surgical time was 3 hours and 5 minutes in Group I and 3 hours and 25 minutes in Group J. We used vacuum drains in all cases. The average duration of hospital stay was 2 days in Group J and 2.2 days in Group I.
Complications were divided into minor and major. Major complications included those that required subsequent surgery (such as bruising, significant suture dehiscence, and marginal skin necrosis) or new hospitalization, along with postoperative infection with systemic repercussions and deep vein thrombosis. The rate of major complications was 10.5% in Group I and 10.6% in Group J.
Minor complications including seroma, slight suture dehiscence, hypertrophic scars, localized infections around the wound, and foreign body granulomas in the subcutaneous tissue occurred at an incidence of 41.1% in Group I and 30.2% in Group J (Tables 1 and 2). Major or minor complications (Figures 1 and 2) were combined with absolute and relative values for Groups I and J (Table 2).
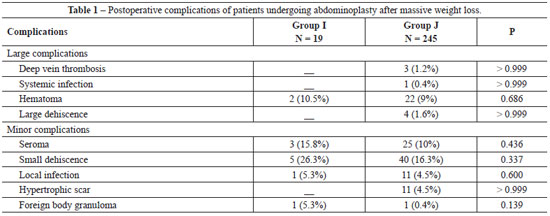
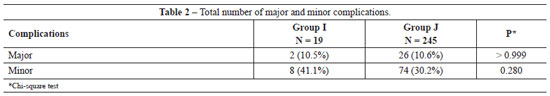
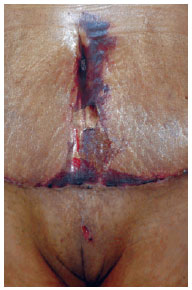
Figure 1 - Minor complication (small dehiscence) after abdominoplasty observed in a patient in Group J.
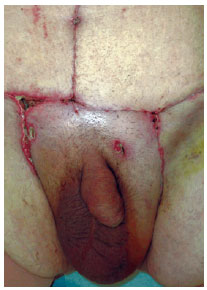
Figure 2 - Minor complication (small dehiscence) after abdominoplasty observed in a patient in Group I.
DISCUSSION
As the indications for bariatric surgery increase, there is an increased demand for plastic surgery to correct body contour deformities4. Moreover, as the global population ages, increasing numbers of geriatric patients are also undergoing surgical procedures.
When managing patients after massive weight loss in obese patients, one should be aware of the associated clinical peculiarities and risks of complications, both of which are higher than those in patients who were never obese6. The risks and benefits of the procedures should be evaluated to ensure that a surgical procedure is indicated only once the underlying diseases, if any, have healed or are under control7-9.
Shermak et al.10 demonstrated that patients with hypothyroidism had higher rates of incisional dehiscence after surgery and that patients with asthma had an increased requirement for blood transfusions during plastic surgery body contouring after massive weight loss. Neaman et al.11 presented similar rates of major complications (16%) and minor complications (26.7%) to those presented here, which approach the levels in literature worldwide.
Regarding plastic surgery, there exists the myth (without scientific evidence) that older patients have worse outcomes and more complications than younger patients. However, it was observed in the present study that patients > 60 years of age did not have increased numbers of complications compared to patients < 60 years of age. Because of the small sample size in Group I (19 patients), there was no evidence of statistical significance in this study, which prevents us from making strong conclusions.
CONCLUSIONS
The findings of this study demonstrate that patients > 60 years of age do not have higher complication rates than patients < 60 years of age. These results should help to exclude the effect of age alone as a risk factor for patients undergoing abdominoplasty after massive weight loss.
REFERENCES
1. Hamad GG. The state of art in bariatric surgery for weight loss in the morbidly obese patient. Clin Plast Surg. 2004;31(4):591-600.
2. Heddens CJ. Body contouring after massive weight loss. Plast Surg Nurs. 2004;24(3):107-15.
3. Instituto Brasileiro de Geografia e Estatística (IBGE). Diretoria de Pesquisas. Coordenação de Índices de Preços. Pesquisa de Orçamento Familiar 2002-2003. [online]. Ministério da Saúde. São Paulo: IBGE. Disponível em: www.ibge.gov.br/home/estatistica/populacao/condicaodevida/pof/2002/pof2002.pdf
4. Kitzinger HB, Abayev S, Pittermann A, Karle B, Kubiena H, Bohdjalian A, et al. The prevalence of body contouring surgery after gastric bypass surgery. Obes Surg. 2012;22(1):8-12.
5. Gemperli R, Munhoz A, Queipo N. Abdominoplastia: otros aspectos. In: Veja LM, Gil OV, eds. Coiffman cirugía plástica, reconstructiva y estética. Tomo IV. 3ª ed. Bogotá: Amolca; 2008. p. 3254-63.
6. Fraccalvieri M, Datta G, Bogetti P, Verna G, Pedrale R, Bocchiotti MA, et al. Abdominoplasty after weight loss in morbidly obese patients: a 4-year clinical experience. Obes Surg. 2007;17(10):1319-24.
7. Cintra W Jr, Modolin ML, Gemperli R, Gobbi CL, Faintuch J, Ferreira MC. Quality of life after abdominoplasty in woman after bariatric surgery. Obes Surg. 2008;18(6):728-32.
8. Michaels 5th J, Coon D, Rubin JP. Complications in postbariatric body contouring: postoperative management and treatment. Plast Reconstr Surg. 2011;127(4):1693-700.
9. Warner JP, Stacey DH, Sillah NM, Gould JC, Garren MJ, Gutowski KA. National bariatric surgery and massive weight loss body contouring survey. Plast Reconstr Surg. 2009;124(3):926-33.
10. Shermak MA, Chang D, Magnuson TH, Schweitzer MA. An outcomes analysis of patients undergoing body contouring surgery after massive weight loss. Plast Reconstr Surg. 2006;118(4):1026-31.
11. Neaman KC, Hansen JE. Analysis of complications from abdominoplasty: a review of 206 cases at a university hospital. Ann Plast Surg. 2007;58(3):292-8.
1. Resident Physician of the Department of Plastic Surgery of the Hospital das Clínicas da Faculdade de Medicina da Universidade de São Paulo, São Paulo, SP, Brazil.
2. Plastic Surgeon of the Hospital das Clínicas da Faculdade de Medicina da Universidade de São Paulo, São Paulo, SP, Brazil.
3. Associate Professor of Plastic Surgery of the Faculdade de Medicina da Universidade de São Paulo, São Paulo, SP, Brazil.
4. Professor of Plastic Surgery of the Faculdade de Medicina da Universidade de São Paulo, São Paulo, SP, Brazil.
Correspondence to:
Pedro Henrique de Souza Smaniotto
Rua Abílio Soares 666, 21B - Paraíso
São Paulo, SP, Brazil - CEP 04005-002
E-mail: pedrofmusp@yahoo.com.br
Submitted to SGP (Sistema de Gestão de Publicações/Manager Publications System) of RBCP (Revista Brasileira de Cirurgia Plástica/Brazilian Journal of Plastic Surgery).
Article received: May 18, 2012
Article accepted: August 21, 2012
This study was performed at the Service of Plastic Surgery of the Hospital das Clínicas da Faculdade de Medicina da Universidade de São Paulo - Hospital Estadual Sapopemba, São Paulo, SP, Brazil.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter