

Case Report - Year 2012 - Volume 27 -
Orbital hemangiopericytoma
Hemangiopericitoma de órbita
ABSTRACT
Hemangiopericytomas are rare tumors arising from the proliferation of pericytes. They may be found in the lungs, bones, skull, deep soft tissue or limbs. The tumor has an unpredictable prognosis and when it affects the orbital region, may have an aggressive behavior, with high incidence of recurrence. We report a case of orbital hemangiopericytoma and highlight clinical, surgical, and histopathological features of these tumors. Orbital hemangiopericytomas usually are solid, slow-growing tumors. They should be considered in the differential diagnosis of well-defined orbital masses along with epidermoid cysts, schwannomas, neurofibromas, fibrous histiocytomas, lipomas, and vascular malformations. The diagnosis is confirmed by anatomopathologic examination and sometimes complemented by immunohistochemistry. Complete excision of the tumor with wide margins is usually curative; however, radiotherapy and chemotherapy may be required for recurrent lesions.
Keywords: Hemangiopericytoma. Neoplasms, vascular tissue. Orbit/surgery.
RESUMO
Hemangiopericitomas são tumores raros originados a partir da proliferação de pericitos, ou seja, células que envolvem os capilares. São encontrados em ossos, pulmões, crânio, partes moles profundas ou membros inferiores, principalmente na coxa. É considerado um tumor com potencial de malignidade incerto e quando afeta a região orbitária pode apresentar um comportamento biológico agressivo, com grande chance de recidiva. O objetivo deste trabalho é relatar um caso de hemangiopericitoma orbital e destacar suas características clínicas, cirúrgicas e histopatológicas. Usualmente, os hemangiopericitomas da órbita são tumores sólidos, únicos e de crescimento lento. Devem ser lembrados no diagnóstico diferencial dos tumores orbitários bem delimitados, como cistos epidermoides, schwannomas, neurofibromas, fibro-histiocitomas, lipomas e malformações vasculares. A confirmação diagnóstica é realizada pelo exame anatomopatológico e, por vezes, complementada pelo estudo imuno-histoquímico. O tratamento deve ser realizado com exérese completa do tumor, com margens amplas, sendo a radioterapia e a quimioterapia reservadas para casos de lesões reincidentes.
Palavras-chave: Hemangiopericitoma. Neoplasias de tecido vascular. Órbita/cirurgia.
Hemangiopericytomas are rare tumors that develop due to the proliferation of pericytes, i.e., the cells that surround the capillaries. They were originally described by Stout and Murray1 in 1942, and account for approximately 1% of vascular tumors. Intraorbital hemangiopericytomas are even less common, with an incidence of 0.8-3%2.
Hemangiopericytomas can be found in the bones, lungs, and even the skull, but the majority of these tumors originate in the deep soft tissues or lower limbs, especially in the thighs. Although it may behave like a benign tumor, it has an uncertain malignant potential and when it affects the orbital region presents potentially aggressive biological behavior, with high chance of relapse. There are reports of relapses up to 18 months after surgical resection3.
The objective of this paper is to report a case of orbital hemangiopericytoma and to highlight this tumor's clinical, surgical, and histopathological features.
CASE REPORT
A 70-year-old woman presented to our hospital with a right infraorbital tumor and a history of previous excision of a bulky lesion in the same region 10 years previously; she was unaware of the pathologic diagnosis of the previous tumor.
The patient reported slow growth of the lesion, starting approximately 6 years previously. The lesion started to disrupt the visual field in the year before treatment, because of the bulging right lower eyelid. The patient denied the existence of comorbidities.
On physical examination, the tumor was oval and approximately 10 cm in diameter, with fibroelastic consistency. It was not tender to palpation, and it affected the entire right lower region of the eyelid causing significant proptosis (Figure 1).
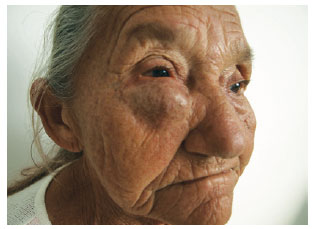
Figure 1 - Preoperative appearance of the tumor, affecting the entire right lower eyelid.
The tarsal senile laxity associated with the lesion's excessive volume, which pulled the eyelid inferiorly, caused significant ectropion. Visual acuity was normal. The differential diagnosis of the lesion initially included lipoma, epidermoid cyst, and neurofibroma.
After the clinical preoperative examination, surgery was performed at the Hospital Irmã Dulce (Praia Grande, SP, Brazil) in order to remove the tumor. We found a single solid tumor, measuring approximately 10.2 × 9.7 × 9.2 cm, encapsulated in a blood-covered, very shiny surface that was behind the orbicularis oculi. The lesion was resected and canthopexy was performed for correction of ectropion.
After resection, the diagnosis of vascular malformation was suggested, along with neurofibroma, schwannoma, and hemangiopericytoma. On histopathologic examination, the tumor consisted of cellular proliferation with mild pleomorphism, and exhibited a peculiar pattern characterized by numerous angulated vessels interspersing tumor cells. Mitotic activity was mild and there was no evident necrosis. The diagnosis of hemangiopericytoma was made (Figure 2).
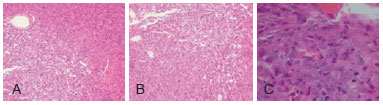
Figure 2 - Histopathologic examination. In A, B, and C indicate cellular proliferation with mild pleomorphism, along with a characteristic vascular pattern, characterized by numerous vessels intercalated with tumor cells.
Despite the canthopexy, the patient developed swelling in the lower eyelid and tarsal region, along with ectropion. She refused any further treatment for the tumor (such as radiotherapy or chemotherapy), and continues to be followed up as an outpatient (Figure 3).
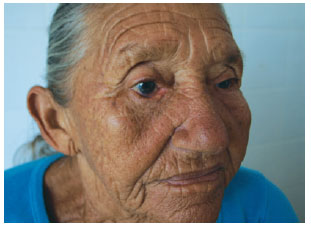
Figure 3 - Postoperative appearance after tumor excision.
DISCUSSION
Orbital hemangiopericytoma is generally a solid, slowgrowing tumor, without apparent predilection for race and gender. Although it preferentially affects adults between the third and sixth decades of life, it can also occur in children3,4.
Symptoms usually include slowly progressive unilateral proptosis, which may be accompanied by mild pain and decreased visual acuity5. It can be found anywhere in the orbit but has a predilection for the upper orbit. Although there may be benign biological behavior, there are reports of recurrences and metastases (lung, bone, and liver), with incidences of 43% and 15%, respectively, especially in cases where surgical excision is incomplete5-7. There is no way to predict, unequivocally, from histological examination, which tumors will exhibit more aggressive behavior8.
Imaging studies are not pathognomonic, but the tumor most often appears as a well-defined lesion that may or may not be enhanced with the use of contrast agents9. The diagnosis is confirmed by histopathologic examination and sometimes complemented by immnohistochemistry.
The characteristic histopathology is cell proliferation with mild to moderate pleomorphism, arranged in bundles interspersed with numerous angulated vessels; on staining with reticulin, an apparent plot - isolating individual cells and vessels - is noted. On immunohistochemical study, the immunoreactivity of CD34 and factor VIII favors the diagnosis9-12.
With regard to treatment, there is unanimity on the need for complete excision with wide margins. Both radiotherapy and chemotherapy have shown controversial results, and are usually used only in cases of relapse6,13,14.
Radiotherapy and chemotherapy as initial treatments should be reserved for cases where surgical excision presents very high risk. In a retrospective study, Carew et al.15 reported a survival rate of 87.5% in a case series of 11 patients treated with total surgical excision, of whom, 4 received postoperative radiotherapy for having tumors histologically classified as high grade. Recurrences and distant metastases are rare in patients treated with complete surgical excision, but the majority of patients who had metastases or recurrences were diagnosed after more than 40 months follow-up, which suggests that the postoperative follow-up for all patients should be longer, regardless of the histological findings16.
Although it is rare, hemangiopericytoma should be considered in the differential diagnosis of well-defined orbital tumors along with epidermoid cysts, schwannomas, neurofibromas, fibrous histiocytomas, lipomas, and vascular malformations.
REFERENCES
1. Stout AP, Murray MR. Hemangiopericytoma: a vascular tumor featuring Zimmermann's pericytes. Ann Surg. 1942;116(1):26-33.
2. Henderson JW, Farrow GM. Primary orbital hemangiopericytoma. An aggressive and potentially malignant neoplasm. Arch Ophthalmol. 1978;96(4):666-73.
3. Karcioglu ZA, Nasr AM, Haik BG. Orbital hemangiopericytoma: clinical and morphological features. Am J Ophthalmol. 1997;124(5):661-72.
4. Kapoor S, Kapoor MS, Aurora AL, Sood GC. Orbital hemangiopericytoma: a report of a three-year-old child. J Pediatr Ophthalmol Strabismus. 1978;15(1):40-2.
5. Jakobiec FA, Howard GM, Jones IS, Wolff M. Hemangiopericytoma of the orbit. Am J Ophthalmol. 1974;78(5):816-34.
6. Croxatto JO, Font RL. Hemangiopericytoma of the orbit: a clinicopathologic study of 30 cases. Hum Path. 1982;13(3):210-8.
7. Rodgers IR, Grove Jr AS. Vascular lesions of the orbit. In: Albert DM, Jacobiec FA, eds. Principles and practice of ophthalmology: clinical practice. Philadelphia: WB Saunders; 1994. p.1971-2.
8. Jacobiec FA, Bilyk JR, Font RL. Vascular tumors and malformations. In: Spencer WH, ed. Ophthalmic pathology: an atlas and textbook. Philadelphia: WB Saunders; 1996. p.2545-9.
9. Alves APX, Félix PR, Velasco e Cruz AA. Hemangiopericitoma de órbita. Arq Bras Oftalmol. 2001;64(2):159-62.
10. Karcioglu ZA, Nasr AM, Haik BG. Orbital hemangiopericytoma: clinical and morphologic features. Am J Ophthalmol. 1997;124(5):661-72.
11. Middleton LP, Duray PH, Merino MJ. The histological spectrum of hemangiopericytoma: application of immunohistochemical analysis including proliferative markers to facilitate diagnosis and predict prognosis. Hum Pathol. 1998;29(6):636-40.
12. Khouqeer ZA, Figueiredo AP, Correia CP, Oliver KM, Burnier Jr MN. Immunohistochemical profile of hemangiopericytoma of the orbit. IOVS 2000;41(Suppl):S125.
13. Walike JW, Bailey BJ. Head and neck hemangiopericytoma. Arch Otolaryngol. 1971;93(4):345-53.
14. Shields JA. Vasculogenic tumors and malformations. In: Shields JA, ed. Diagnosis and management of orbital tumors. Philadelphia: WB Saunders; 1989. p.132-4.
15. Carew JF, Singh B, Kraus DH. Hemangiopericytoma of the head and neck. Laryngoscope. 1999;109(9):1409-11.
16. Enzinger FM, Smith BH. Hemangiopericytoma. An analysis of 106 cases. Hum Pathol. 1976;7(1):61-82.
1. Plastic surgeon, associate member of the Sociedade Brasileira de Cirurgia Plástica/Brazilian Society of Plastic surgery (SBCP), Assistant physician in the Plastic Surgery Department of the Faculdade de Medicina do ABC, Master in Health Sciences by Faculdade de Medicina do ABC, Santo André, SP, Brazil.
2. Plastic surgeon, associate member of the SBCP, professor of the Universidade Cidade de São Paulo, São Paulo, SP, Brazil.
3. Plastic surgeon, associate member of the SBCP, São Paulo, SP, Brazil.
4. Full professor of Plastic Surgery in the Faculdade de Medicina do ABC, Master and Doctor by Escola Paulista de Medicina (UNIFESP/EPM), full member of SBCP, Santo André, SP, Brazil.
5. Professor of the Pathology Department of the UNIFESP/EPM, São Paulo, SP, Brazil.
Correspondence to:
Sidney Zanasi Junior
Av. Lauro Gomes, 2.000 - Vila Sacadura Cabral
Santo André, SP, Brazil - CEP 09060-870
E-mail: sidneyzanasijunior@ig.com.br
Submitted to SGP (Sistema de Gestão de Publicações/Manager Publications System) of RBCP (Revista Brasileira de Cirurgia Plástica/Brazilian Journal of Plastic Surgery).
Article received: April 8, 2010
Article accepted: July 26, 2010
Work performed at the Plastic Surgery Department of the Faculdade de Medicina do ABC, Santo André, SP, Brazil.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter