

Original Article - Year 2012 - Volume 27 -
Detection of venous thrombosis in free flaps by measurement of capillary blood glucose
Detecção de trombose venosa em retalhos livres por medidas de glicemia capilar
ABSTRACT
BACKGROUND: Monitoring of free flaps after surgery is vitally important, especially in the first few hours because the timing of reoperation can determine flap salvage or loss. To date, no study has examined the decision to reoperate on a flap based on the objective measure of glycemia or a comparison between flaps that showed good outcomes and those that showed vascular damage. The objective of this study was to evaluate the validity of blood glucose measurements within the flap as a method for monitoring free flaps and to compare the efficacy of this method with that of clinical assessments.
METHODS: The study was prospective, included 16 patients with free flaps, and was conducted from May 2012 to July 2012. A team of professionals not involved in the surgery evaluated capillary glycemia. Flaps were clinically evaluated during the immediate postoperative period, on ICU admission, at every 3 hours, and as needed.
RESULTS: Of the 16 patients, 5 (31.3%) had venous thrombosis in the first 24 hours. Statistically significant differences were noted in capillary glycemia in patients with or without venous thrombosis in measurements obtained 6, 9, and 12 hours after surgery (P < 0.05).
CONCLUSIONS: The measurement of capillary glycemia was not superior to clinical evaluation by an experienced professional for the detection of venous thrombosis within free flaps.
Keywords: Microsurgery. Surgical flaps. Venous thrombosis.
RESUMO
INTRODUÇÃO: A monitorização do retalho livre após a cirurgia é de vital importância, especialmente nas primeiras horas de pós-operatório, pois o momento de reabordagem pode ser o definidor entre o salvamento ou a perda do retalho. Até o momento, não existe trabalho na literatura estudando a decisão de abordagem do retalho baseada em medidas objetivas ou a comparação da glicemia entre retalhos que evoluíram bem com os que sofreram sofrimento vascular. O objetivo deste estudo é avaliar a validade da medida da glicemia capilar do retalho como método de monitorização de retalhos microcirúrgicos comparando com a avaliação clínica.
MÉTODO: Foram estudados prospectivamente 16 pacientes portadores de retalhos livres, realizados de maio de 2012 a julho de 2012. A glicemia capilar foi avaliada por equipe formada por profissionais não envolvidos com a cirurgia realizada. A avaliação clínica do retalho foi realizada no pós-operatório imediato, na chegada à UTI, a cada 3 horas e sempre que necessário.
RESULTADOS: Dos 16 pacientes, 5 (31,3%) apresentaram complicações nas primeiras 24 horas. Todas as complicações observadas foram trombose venosa. Foi observada diferença estatisticamente significante na glicemia capilar de portadores de retalhos que apresentaram trombose venosa em comparação àqueles que não tiveram a complicação, nas medidas realizadas 6 horas, 9 horas e 12 horas após a operação (P < 0,05).
CONCLUSÕES: A medida da glicemia capilar não foi superior à avaliação clínica por profissional experiente na detecção de trombose venosa de retalhos livres.
Palavras-chave: Microcirurgia. Retalhos cirúrgicos. Trombose venosa.
Monitoring of free flaps after surgery is of vital importance, especially during the first few hours, because the timing of reoperation can define flap salvage or loss1.
However, monitoring parameters and reoperation decisions are challenging for surgeons. Classically, flap viability is evaluated based on clinical parameters such as temperature, color, turgor, capillary refill, and bleeding after scarification. Wilson et al.2 recommend flap evaluation by trained nurses every 30 minutes in the first 24 postoperative hours and every 4 hours thereafter.
Although physical examination is essential in a reoperation decision, findings of physical examination may be faulty if the surgical team lacks experience or if other non-ideal factors such as inadequate lighting or visualization difficulties are present. This limitation led to the study and development of other monitoring methods such as assessment of temperature differences between the flap and the adjacent skin2, Doppler ultrasonography of the vascular pedicle3, measurement of tissue oxygenation4, analysis by microdialysis5, use of intra-arterial or intravenous catheters6, and quantitative spectral imaging (which measures distance, oxyhemoglobin, deoxyhemoglobin, total hemoglobin, and tissue saturation)7. Using objective measures, health professionals who are inexperienced in microsurgery can monitor the flap.
The use of capillary glycemia can be useful because it provides objective data without requiring complex apparatus. Glucometers are routinely used in all intensive care units and cost less than other monitoring systems.
The objective of this study was to evaluate the validity of the measurement of capillary glycemia of the flap as a method for monitoring free flaps and compare its efficacy with that of clinical evaluation.
METHODS
This study was prospective and included 16 patients who had undergone free flap surgery performed by the Division of Plastic Surgery and Burns, Hospital das Clínicas da Faculdade de Medicina da Universidade de São Paulo (Hospital das Clinicas, Faculty of Medicine, University of São Paulo), between May 2012 and July 2012.
The institutional research ethics committee approved this project. All patients were informed about the project's objectives and procedures and participated voluntarily after signing an informed consent form.
A team of professionals not involved in the surgery evaluated capillary glycemia and temperature. A physician performed clinical evaluation of the flap during the immediate postoperative period, on ICU admission, at every 3 hours, and when necessary.
Measurements of capillary glycemia were always obtained using the same device (One Touch® Ultra, LifeScan, Inc., Milpitas, CA, USA). The evaluator collected a drop of blood from each flap for each measurement. The team performing clinical monitoring of the flap had no access to the blood glucose monitoring results to prevent influencing the medical caregivers' decisions and maintain a standard treatment for all patients.
RESULTS
Of the 16 patients, 5 (31.3%) had complications (venous thrombosis) in the first 24 hours (Table 1). Figures 1 and 2 illustrate the flap capillary glycemia of patients with and without complications, respectively. Figure 3 shows the average flap capillary glycemia of patients with and without complications. A nonparametric Mann-Whitney U-test showed that the differences were statistically significant (P < 0.05) at 6, 9, and 12 hours (Table 2).
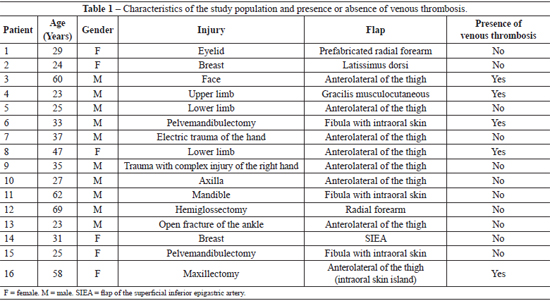
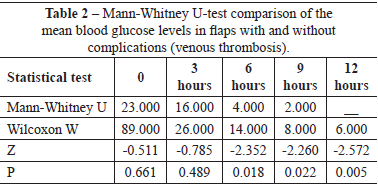
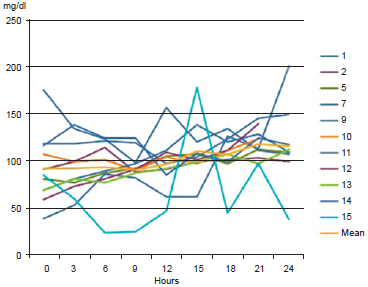
Figure 1 - Flap capillary blood glucose (mg/dL) of the patients without venous thrombosis.
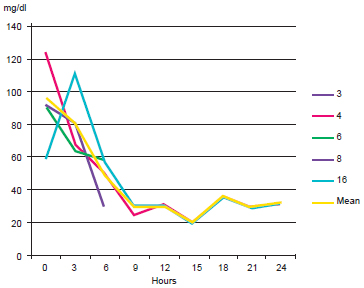
Figure 2 - Flap capillary blood glucose (mg/dL) of the patients with venous thrombosis.
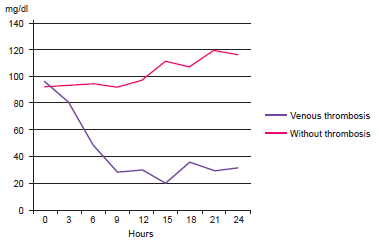
Figure 3 - Mean flap capillary blood glucose (mg/dL) in patients with and without venous thrombosis.
Because of the limited number of patients with complications, it was not possible to determine a flap glycemia value that was indicative of venous thrombosis. Moreover, it was not possible to determine whether measurement of capillary glycemia before clinical diagnosis of thrombosis would identify the flaps that would present a complication.
DISCUSSION
Although free flaps enable transfer of various tissues and rebuilding of complex architectures, surgeons face the challenge of microvascular anastomosis. Anastomosis of small-diameter structures, some measuring < 1 mm, requires refinement of suture techniques. Because handling and introduction of the needle into the vessel wall can be thrombogenic, venous thrombosis is the most feared complication8. Therefore, monitoring the flap after surgery is of vital importance, especially during the first few hours, because the timing of reoperation may determine flap salvage or loss1.
Surgeons experienced in microsurgery usually monitor these flaps. However, these highly specialized professionals may not be available in all hospitals. Therefore, the use of an objective measurement technique can reduce the need for human resources, thereby reducing cost.
Flap glycemia has been studied as a diagnostic method for venous thrombosis by other authors, but none of the studies used a blinded system. In 2012, Hara et al.9 reported that a blood glucose level of 62 mg/dL had a sensitivity of 88% and specificity of 82% for the detection of venous thrombosis. In their study, 3 false positives and 1 false negative were considered indicative of venous thrombosis. More studies with larger data series are needed to determine the exact value that is indicative of thrombosis.
The present study confirms that there is a decrease in capillary glycemia in flaps with venous thrombosis; however, evaluation of this parameter did not enable earlier detection of complications. Therefore, if experienced microsurgery professionals conduct postoperative monitoring of flaps, such routine measurements are unnecessary.
Finally, in this study, only 5 complications were observed in the first 24 hours after surgery, most within the first 12 hours. Moreover, all complications were venous thrombosis. Other complications such as hematomas did not occur, and possibly cannot be detected using capillary blood glucose measurements. Therefore, evaluation by a professional experienced in postoperative changes in flap condition is still highly recommended.
CONCLUSIONS
The measurement of free flap capillary glycemia was not superior to clinical evaluation by an experienced professional for the detection of venous thrombosis.
REFERENCES
1. Novakovic D, Patel RS, Goldstein DP, Gullane PJ. Salvage of failed free flaps used in head and neck reconstruction. Head Neck Oncol. 2009;1:33.
2. Wilson JL, Morritt AN, Morrison WA. Avoiding complications. In: Wei FC, Mardini S, eds. Flaps and reconstructive surgery. Philadelphia: Saunders; 2009. p.117-24.
3. Wise JB, Talmor M, Hoffman LA, Gayle LB. Postoperative monitoring of microvascular tissue transplants with an implantable Doppler probe. Plast Reconstr Surg. 2000;105(6):2279-80.
4. Kamolz LP, Giovanoli P, Haslik W, Koller R, Frey M. Continuous free-flap monitoring with tissue-oxygen measurements: three-year experience. J Reconstr Microsurg. 2002;18(6):487-91.
5. Jyränki J, Suominen S, Vuola J, Bäck L. Microdialysis in clinical practice: monitoring intraoral free flaps. Ann Plast Surg. 2006;56(4):387-93.
6. Sakurai H, Nozaki M, Takeuchi M, Soejima K, Yamaki T, Kono T, et al. Monitoring the changes in intraparenchymatous venous pressure to ascertain flap viability. Plast Reconstr Surg. 2007;119(7):2111-7.
7. Pharaon MR, Scholz T, Bogdanoff S, Cuccia D, Durkin AJ, Hoyt DB, et al. Early detection of complete vascular occlusion in a pedicle flap model using quantitative [corrected] spectral imaging. Plast Reconstr Surg. 2010;126(6):1924-35.
8. Evans BC, Evans GR. Microvascular surgery. Plast Reconstr Surg. 2007;119(2):18e-30e.
9. Hara H, Mihara M, Iida T, Narushima M, Todokoro T, Yamamoto T, et al. Blood glucose measurement for flap monitoring to salvage flaps from venous thrombosis. J Plast Reconstr Aesthet Surg. 2012;65(5):616-9.
1. Preceptor Physician of the Hospital das Clínicas da Faculdade de Medicina da Universidade de São Paulo (Hospital of the Faculty of Medicine, University of São Paulo - HCFMUSP), Assistant Physician Plastic Surgery Service at Hospital do Servidor Público Estadual de São Paulo (Hospital for State Civil Servants of St. Paul), Associate Member of the Sociedade Brasileira de Cirurgia Plástica (Brazilian Society of Plastic Surgery - SBCP), São Paulo, SP, Brazil.
2. Doctor, full member of the SBCP, Physician, Division of Plastic Surgery HCFMUSP, São Paulo, SP, Brazil.
3. Resident in General Surgery HCFMUSP, São Paulo, SP, Brazil.
4. Resident of Plastic Surgery HCFMUSP, São Paulo, SP, Brazil.
5. Physician Group of Hand and Reconstructive Microsurgery, Institute of Orthopaedics and Traumatology HCFMUSP, São Paulo, SP, Brazil.
6. Livre docente, Associate Professor of the University of São Paulo, Head of Group of Hand and Reconstructive Microsurgery, Institute of Orthopaedics and Traumatology HCFMUSP, São Paulo, SP, Brazil.
7. Professor, Chief of the Division of Plastic Surgery and Burns HCFMUSP, full member of the SBCP, São Paulo, SP, Brazil.
Submitted to SGP (Sistema de Gestão de Publicações/Manager Publications System) of RBCP (Revista Brasileira de Cirurgia Plástica/Brazilian Journal of Plastic Surgery).
Article received: September 26, 2012
Article accepted: November 11, 2012
Correspondence to:
Lincoln Saito Millan
Av. Doutor Enéas Carvalho de Aguiar, 255 - 8º andar - sala 8128
São Paulo, SP, Brazil - CEP 05403-900
E-mail: lincolnsaito@gmail.com
This study was performed in the Division of Plastic Surgery and Burns, Hospital das Clínicas da Faculdade de Medicina da Universidade de São Paulo (Hospital das Clinicas, Faculty of Medicine, University of São Paulo), São Paulo, SP, Brazil.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter