

Case Report - Year 2012 - Volume 27 -
Mondor's disease associated with gynecomastia and nipple surgery
Doença de Mondor associada à cirurgia de ginecomastia e do mamilo
ABSTRACT
Mondor's disease is a rare condition characterized by thrombophlebitis of the superficial vessels of the thoracoabdominal region that occurs as a complication of breast surgery. The aim of this study is to review the scientific literature on Mondor's disease in light of the currently reported clinical case. In this article, we describe the case of a 38-year-old man with hypertrophy of the mammary glands, which produced aesthetic and psychological effects. After an initial evaluation, the patient underwent partial resection of the right nipple and the mammary glands by inferior periareolar approach. In the postoperative period, the patient developed painful, erythematous cords in the bilateral inframammary thoracic region following the topography of the thoracoepigastric veins. The findings were consistent with Mondor's disease. The patient was treated with gel-based heparin and oral analgesics. After treatment, a hard line remained on the right side. Mondor's disease is a rare and benign complication of breast surgery that should be treated symptomatically. It is important that surgeons are able to diagnose and counsel patients about the self-limiting characteristics of Mondor's disease.
Keywords: Thrombophlebitis. Fibrosis. Gynecomastia.
RESUMO
A doença de Mondor é uma rara afecção, caracterizada pela tromboflebite dos vasos superficiais da região toracoabdominal, ocorrendo como uma complicação da cirurgia de mama. O objetivo deste estudo é, a partir de um caso clínico, fazer uma revisão da literatura científica sobre a doença de Mondor. O presente artigo é o relato de caso de um paciente do sexo masculino, de 38 anos de idade, portador de hipertrofia das glândulas mamárias e do mamilo direito, com prejuízos estéticos e psicológicos. Após avaliação inicial, o paciente foi submetido à ressecção parcial do mamilo direito e das glândulas mamárias por via periareolar inferior. No período pós-operatório, o paciente desenvolveu cordões dolorosos e eritematosos na região torácica inframamária bilateralmente, na topografia das veias toracoepigástricas. Os achados eram compatíveis com doença de Mondor. O paciente foi tratado com gel à base de heparina e analgésicos por via oral. Após tratamento, o paciente permaneceu com uma linha endurecida à direita. A doença de Mondor representa rara e benigna complicação da cirurgia da mama, que deve ser tratada de forma sintomática. É importante que o cirurgião esteja apto para o diagnóstico e para orientar o paciente sobre o caráter autolimitado da doença de Mondor.
Palavras-chave: Tromboflebite. Fibrose. Ginecomastia.
Mondor's disease is characterized by the development of self-limiting thrombophlebitis of the veins of the thoracoabdominal wall. Although there are reports of Mondor's disease developing in the penis as well as in various locations of the human body, it was first described in the thoracic region. The disease is included in a set of postoperative complications of breast surgery.
This condition rarely occurs, and there are fewer than 400 cases reported in the literature worldwide. At present, Mondor's disease is still reported in the literature pertaining to plastic surgery1-3.
In the present report, we describe the case of patient with Mondor's disease that manifested after surgery for the correction of gynecomastia and nipple hypertrophy in a male patient. This is a rare presentation of the disease and a possible complication of this type of surgery.
CASE REPORT
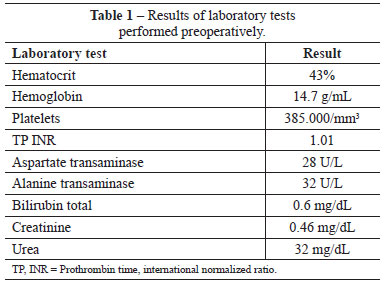
A 38-year-old man presented to our clinic with increased growth of tissue in the breast region. Physical examination showed moderate bilateral gynecomastia and hypertrophy of the right nipple without palpable nodules, nipple discharge, or pain. The patient had no other complaints, and there were no other noticeable changes on physical examination. There was no history of medication use, smoking, alcohol, or illicit drug abuse. The results of biochemical laboratory examinations are shown in Table 1.
The patient reported that the condition had caused difficulties in interpersonal relationships as well as clothing choices. With patient consent, we opted to resect both mammary glands and repair the right nipple. The consent form was discussed and signed.
Lower periareolar incisions were made, and the entire glandular tissue of the breast was resected. Reduction of the right nipple was performed by the removal of a wedge bottom.
In the immediate postoperative period, we noted the appearance of lines and a bilateral painful erythematous thoracoabdominal region, consistent with phlebitis in the right and left thoracoepigastric veins, as well as ecchymosis in the operated regions.
Local treatment was initiated with gel heparin and oral analgesics. The phlebitis on the left side responded to treatment, whereas that on the right side progressed to thrombophlebitis and fibrosis and formed a fibrous cord 5 months after surgery. This cord was visible and painful, and it stretched from the areola to the upper right ipsilateral quadrant, resulting in the formation of a groove on the skin in the middle third of the line. As the fibrous cord did not affect the patient, no treatment was initiated.
Ten months after the surgery, the fibrous cord was still present; however, it did not limit the patient's movements, was painful only upon compression, and resulted in the formation of a groove of dark skin (Figures 1 and 2).
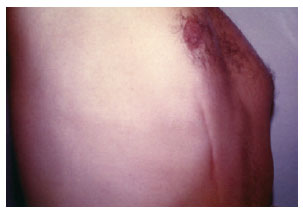
Figure 1 - Fibrous chord: sequelae of Mondor's disease (lateral view).
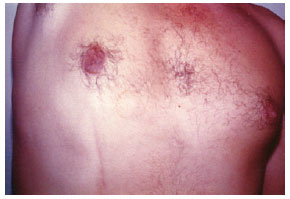
Figure 2 - Fibrous chord: sequelae of Mondor's disease (anterior view).
DISCUSSION
Mondor's disease is a rare condition that is characterized by thrombophlebitis of the subcutaneous veins of the thoracoabdominal wall1. The disease was first reported in 1869 by Fagge4; however, the author had initially suspected this case to be scleroderma. In 1922, Fiessinger & Mathieu5 published the first paper reporting this type of vascular inflammation in the abdominal wall. In 1939, Mondor6 reported a series of 4 cases of subacute subcutaneous anterolateral band of the chest wall; in 1944, he termed this disease as cordonal phlebitis of the chest wall, and subsequently, it became known as Mondor's disease.
The etiology of Mondor's disease is not well defined. In cases reported in the scientific literature, 50%-60% cases are of unknown etiology5. The most common etiological factors identified include trauma of the affected region, excessive physical activity, breast surgery, breast infections, and inflammatory processes. Mondor's disease can occur as a postoperative complication after any invasive procedure in the breast region.
Some authors have associated Mondor's disease with malignancy since it resembles an early sign of neoplastic disease and commonly occurs without any apparent cause7-11. Therefore, it is recommended that women with Mondor's disease without apparent cause should undergo a mammography1.
Clinically, the disease presents as a palpable and painful subcutaneous cord located in the thoracoabdominal wall, adjacent to a region subjected to an invasive procedure. Erythema and edema area also present in the affected region and can create a well-defined erythematous line that can be up to 150 mm long. The time of symptom onset averages from 2 to 4 weeks after surgery. The vessels most affected are the thoracoepigastric veins, including the lateral thoracic and upper epigastric veins. Mondor's disease can also occur in the dorsal veins of the penis2. In certain cases, there may be itching, bruising, and fever8. The condition can be diagnosed by patient history and physical examination, and biopsy is not needed. The main conditions to consider during differential diagnosis are lymphangitis and Behçet's disease.
The treatment of Mondor's disease can be both conservative and symptomatic. The application of local heat, rest, and analgesics can help reduce the pain. Some authors recommend the use of anti-inflammatory non-steroids and prescribe oral anticoagulants8. The benign and self-limiting nature of Mondor's disease is well known, and its clinical picture is usually resolved between 2 and 8 weeks.
Mondor's disease is a rare complication of breast surgery that should be treated medically. Surgeons should be able to reassure patients about its benign and self-limiting nature.
REFERENCES
1. Duprap E, Milliez PY, Auquit-Auckbut I, Bony-Rerolle S. Mondor's disease and breast plastic surgery. Ann Chir Plast Esthet. 2010;55(3):233-7.
2. Mayor M, Burón I, de Mora JC, Lázaro TE, Hernández-Cano N, Rubio FA, et al. Mondor's disease. Int J Dermatol. 2000;39(12):922-5.
3. Soler-González J, Ruiz MC. Images in clinical medicine. Mondor's disease. N Engl J Med. 2005;352(10):1024.
4. Fagge CH. Remarks of certain cutaneous affections. Guy's Hosp Rep. 1869;15:295-364.
5. Fiessinger N, Mathieu P. Thrombophlébites des veins de la paroi thoraco-abdominale. Bull Soc Med Hôp Paris. 1922;46:352.
6. Mondor H. Tronculite sous-cutané subaigue de la paroi thoracique antero-laterale. Mem Acad Chir. 1939;65:1271-8.
7. Pugh CM, DeWitty RL, Mondor's disease. J Natl Med Assoc. 1996;88(6):359-63.
8. Chiedozi LC, Aghahowa JA. Mondor's disease associated with breast cancer. Surgery. 1988;103(4):438-9.
9. Kartsaklis P, Konstantinidis C, Thomas C, Tsimara M, Andreadakis S, Gekas A. Penile Mondor's disease: a case report. Cases J. 2008;1(1):411.
10. Catania S, Zurrida S, Veronesi P, Galimberti V, Bono A, Pluchinotta A. Mondor's disease and breast cancer. Cancer. 1992;69(9):2267-70.
11. Veronesi P, Zurrida S. Mondor's disease: is there any correlation with breast cancer? Breast. 1995;4(3):170-1.
1. Full member of the Sociedade Brasileira de Cirurgia Plástica/Brazilian Society of Plastic Surgery (SBCP), Scientific Director of the SBCP-RS, Preceptor of Residence of the Plastic Surgery Service of the Hospital Universitário da Pontifícia Universidade Católica do Rio Grande do Sul/ University Hospital of the Catholic University of Rio Grande do Sul (PUC-RS), Director of the Clínica Integrada de Cirurgia Plástica e Psicologia/Integrated Clinic of Plastic Surgery and Psychology (PSICOPLAST), Porto Alegre, RS, Brazil.
2. Physician graduated by Faculty of Medicine of the PUC-RS, Porto Alegre, RS, Brazil.
3. Physician graduated by Faculty of Medicine of the Federal University of Rio Grande do Sul, Porto Alegre, RS, Brazil.
Correspondence to:
Jones Martinho Copetti Praça Joaquim Leite, 39 - Chácara das Pedras
Porto Alegre, RS, Brazil - CEP 91330-070
E-mail: jonescopetti@psicoplast.com.br
Submitted to SGP (Sistema de Gestão de Publicações/Manager Publications System) of RBCP (Revista Brasileira de Cirurgia Plástica/Brazilian Journal of Plastic Surgery).
Article received: July 12, 2011
Article accepted: February 5, 2012
This study was performed at the Clínica Integrada de Cirurgia Plástica e Psicologia/Integrated Clinic of Plastic Surgery and Psychology (PSICOPLAST), Porto Alegre, RS, Brazil.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter