

Original Article - Year 2013 - Volume 28 -
Complex nasal reconstruction: surgical options in a series of cases
Reconstrução nasal complexa: opções cirúrgicas numa série de casos
ABSTRACT
BACKGROUND: Complex nasal reconstruction has reached a high level of sophistication, emphasizing the need to replace nasal tissues with other similar tissues. We aimed to describe a series of patients who underwent complex nasal reconstruction secondary to oncologic resection or trauma.
METHODS: Patients simultaneously presenting with mucosa, cartilaginous support, and nasal skin defects were considered to have complex nasal defects and were eligible for reconstruction. The type of reconstruction was established according to the location and size of the defect; however, the procedure always included simultaneous reconstruction of the mucosa, cartilaginous support, and nasal skin.
RESULTS: Ten patients underwent complex reconstruction of the nose, including 8 men with a mean age of 53 years. Mucosal reconstruction was performed using a contralateral chondromucosal septal flap, ipsilateral mucosa, or cutaneous malar somersault flap. Cartilaginous support was performed with septal and conchal cartilage grafts and cutaneous coverage with a frontal paramedian flap. There were no cases of hematoma, necrosis, or infection. Patients who underwent mucosa reconstruction with mucosal flaps reported normal breathing, unlike those who underwent reconstruction with a dermal-fat somersault flap and reported air flow obstruction.
CONCLUSIONS: Reconstruction of complex nasal defects is challenging for plastic surgeons. Replacing the nasal tissue with similar tissue promotes the best possible aesthetic and functional results and is associated with a low incidence of complications.
Keywords: Skin neoplasms. Nose/surgery. Surgical flaps.
RESUMO
INTRODUÇÃO: As reconstruções nasais complexas têm alcançado alto nível de sofisticação, enfatizando-se a necessidade de substituir os tecidos nasais por outros similares. O objetivo deste estudo é descrever uma série de casos de pacientes submetidos a reconstrução nasal complexa secundária a ressecções oncológicas ou trauma.
MÉTODO: Foi considerado defeito nasal complexo, e, consequentemente, sua reconstrução, aquele que acometia mucosa, suporte cartilaginoso e pele nasal, simultaneamente. O tipo de reconstrução foi definido de acordo com a localização e o tamanho do defeito, mas sempre incluiu reconstrução da mucosa, suporte cartilaginoso e pele nasal simultaneamente.
RESULTADOS: Dez pacientes foram submetidos a reconstrução complexa do nariz, sendo 8 do sexo masculino, com média de idade de 53 anos. A reconstrução da mucosa foi feita com retalho septal condromucoso contralateral, mucoso ipsilateral ou retalho cutâneo malar em cambalhota. O suporte cartilaginoso foi realizado com enxerto de cartilagem septal e conchal e a cobertura cutânea, com retalho paramediano frontal. Não foi observado nenhum caso de hematoma, necrose ou infecção. Os pacientes que tiveram a reconstrução da mucosa realizada com retalhos mucosos referiam que respiravam normalmente, ao contrário dos pacientes submetidos a reconstrução com retalho dermogorduroso em cambalhota, que referiam obstrução ao fluxo aéreo.
CONCLUSÕES: A reconstrução de defeitos nasais complexos se constitui num desafio para o cirurgião plástico. A substituição dos tecidos nasais por outros similares promove melhor resultado tanto estético como funcional possível e está associado a baixa incidência de complicações.
Palavras-chave: Neoplasias cutâneas. Nariz/cirurgia. Retalhos cirúrgicos.
The nose is a central facial structure of great aesthetic and functional importance. It is particularly exposed to traumas and skin neoplasms, making its reconstruction challenging for plastic surgeons1.
In recent decades, complex nasal reconstruction has reached a high level of sophistication, emphasizing the need to replace the nasal tissue with similar tissue. Thus, whenever possible, the skin should be replaced with skin of similar color and texture such as that from frontal flaps, mucosa, septal flaps, and cartilaginous support with septal, conchal, or costal flaps or grafts2.
In the present study, we aimed to describe a series of patients who underwent complex nasal reconstruction secondary to oncologic resection or trauma.
METHODS
Patients simultaneously presenting with mucosa, cartilaginous support, and nasal skin defects were considered to have complex nasal defects and were eligible for reconstruction.
Patients who had complex defects in one or more aesthetic nose subunits, secondary to oncologic resection - either simultaneously or preceding - or due to trauma were included in the study.
All patients underwent complex nasal reconstruction in the Plastic Surgery Service of the Oswaldo Cruz University Hospital at Pernambuco University between May 2010 and April 2012.
All patients received general anesthesia and local infusion with 0.5% lidocaine and 1:200,000 adrenaline. In all cases, patients received antibiotic prophylaxis with 2 g of intravenous cefazolin during anesthetic induction.
The type of reconstruction was established according to the location and size of the defect; however, it always included mucosa, cartilaginous support, and nasal skin reconstruction, either performed separately or simultaneously.
The release of the frontal paramedian flap base was planned at 21 days after surgery.
This study was approved by the Research Ethics Committee of Pernambuco University (CAAE 00744712.0. 0000.5207).
RESULTS
Ten patients underwent complex reconstruction of the nose, including eight men with a mean age of 53 years (range, 27−82 years). Nine patients underwent cutaneous malignant tumor resection, and one was a victim of trauma caused by a non-firearm weapon.
All defects were located in one of the wings and lower portion of side walls, or on the nasal tip, i.e., in the lower third of the nose involving the mucosa, lower lateral cartilage, and/or higher and overlying skin segment.
In two patients undergoing oncologic resection, the mucosa was rebuilt with a dermal-fat somersault flap in the medial basic malar region because these patients underwent resection of the entire cartilaginous septum. Cartilaginous support was performed with conchal cartilage grafting (Figure 1).
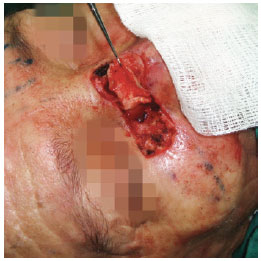
Figure 1 - A malar dermal-fat somersault flap of the medial base was used for reconstruction of the lateral wall mucosa of the nose after basal cell carcinoma resection.
In the trauma patient, nasal mucosa reconstruction was performed using a contralateral chondromucosal septal flap in the hinge of an anterosuperior base. The ipsilateral mucosa was pushed back, returned, and sutured to prevent septal fistulas. The cartilaginous support was reconstituted with a conchal cartilage graft for nasal wing support, and with the abovementioned septal cartilage flap segment for internal nasal valve construction (Figure 2).
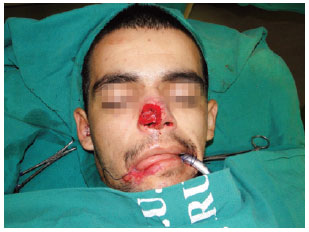
Figure 2 - A contralateral chondromucosal septal flap in the hinge of the anterosuperior base with a conchal cartilage graft in the nostril margin was used for reconstruction of the mucosa membrane and cartilaginous support of the wing and right side wall of the nose after post-traumatic substance loss caused by a non-firearm weapon. The flap was elevated and fixed previously.
In the other seven patients, the mucosal lining was reconstructed using a ipsilateral mucoperichondrial flap based on the caudal septum. The contralateral mucosa was kept intact. The cartilaginous skeleton was reconstructed with conchal and septal cartilage grafts for wing support and internal nasal valve construction, respectively (Figure 3).
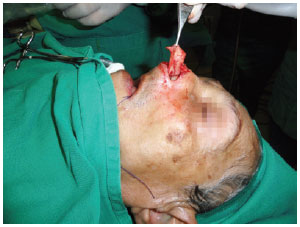
Figure 3 - An ipsilateral mucoperichondrial flap based on the caudal septum was used for reconstruction of the nasal mucosa of the wing and lateral left wall of the nose after basal cell carcinoma resection. The septal cartilage is exposed, which was used as the graft for construction of the internal nasal valve.
Cutaneous coverage was achieved with a frontal paramedian flap in all patients, and elevated in the supraperiosteal plane, while the supratrochlear artery pedicle was kept intact. Flap distal thinning was performed in the portion corresponding to the cutaneous defect, through myectomy of the frontal prominence (Figure 4).
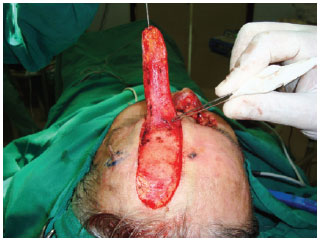
Figure 4 - A frontal paramedian flap, elevated in the supraperiosteal plane with distal thinning on the portion corresponding to the cutaneous defect, through myectomy on the frontal prominence, was used for nasal tip skin coverage.
In 9 patients, primary closure of the frontal donor area was performed, including the portion corresponding to the distal end of the flap. In a young trauma patient, owing to the lack of frontal skin sagging, the area corresponding to the end of the flap was left to heal.
Division of the frontal paramedian flap pedicle was performed on postoperative day 21, and included the base of the ipsilateral mucoperichondrial flap, if it was used.
All patients presented with epistaxis or bleeding of the bloody cutaneous flap area; however, none of the patients required surgical revision. No cases of hematoma, necrosis, or infection were observed. Patients who underwent mucosa reconstruction with mucosal flaps reported normal breathing, unlike patients who underwent reconstruction with dermal-fat somersault flaps and reported air flow obstruction.
Figures 5 and 6 depict the results obtained 12 months after complex nasal reconstruction in 2 patients.
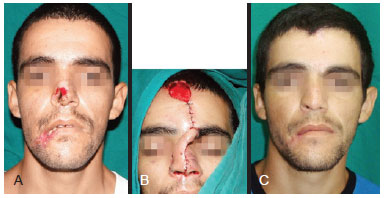
Figure 5 - Male 27-year-old patient. In A, preoperative appearance, showing extensive nasal substance loss following trauma caused by a non-firearm weapon. In B, intraoperative appearance. In C, appearance 12 months after complex nasal reconstruction using a contralateral chondromucosal septal flap in the hinge of the anterosuperior base, and conchal and septal cartilage grafts for wing support and construction of the internal nasal valve, respectively; a frontal paramedian flap was used for cutaneous coverage.
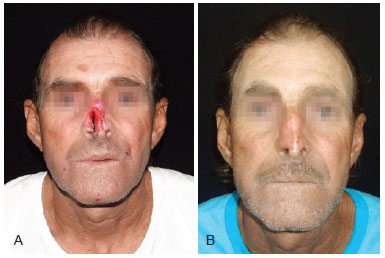
Figure 6 - Male 55-year-old patient. In A, preoperative appearance. In B, appearance 12 months after complex nasal reconstruction using an ipsilateral mucoperichondrial flap based on the caudal septum, and conchal and septal cartilage grafts for wing support and construction of the internal nasal valve, respectively; a frontal paramedian flap was used for cutaneous coverage.
DISCUSSION
Reconstruction of complex nose defects requires the reconstitution of the nasal mucosa, cartilaginous support, and cutaneous coverage with color, texture, and contour similar to the original nose skin, in addition to the restoration of normal nasal breathing function2,3.
Nasal reconstruction must be based on nasal subunits, which form the nasal aesthetic unit. The incisions must be planned within the limits of subunits where scars will be less visible. Thus, removal of additional tissue with reconstruction of the entire subunit ensures optimal results in cases where more than 50% of the subunit is lost, and simulates the normal nasal contour4.
Skin flaps in hinges are too thick and poorly vascularized for reconstruction of the nasal mucosa; they cause distortion and decreased permeability of the nostril cavity5, unlike mucous flaps, which are thin and well vascularized, and provide ideal blood supply for the cartilaginous graft without any obstructions to nasal air flow6.
Restoration of the nasal support is crucial for excellent aesthetic and functional results. Autogenous materials such as septal, auricular, and costal cartilage are the most widely used constituents for this purpose, either with free or compound grafts, or as part of chondromucosal septal flaps, each with its advantages and disadvantages7,8.
The conchal cartilage free graft is usually used to support the nasal wing because it possesses natural convexity, which enhances support to the nostril margin. However, grafts or chondromucosal septal flaps are the most widely used materials for reconstruction of the internal nasal valve2,8.
Cutaneous coverage in complex nasal reconstruction is performed in most cases with a frontal paramedian flap because it provides skin texture and color that are similar to those of the original nose9,10. Important strategies led to aesthetic improvements in nasal reconstruction when using this flap. The concept of nasal aesthetic units emerged, with the emphasis on replacing the skin of an entire unit in cases with more than 50% unit loss8, in addition to making incisions along the edges of the unit and attempting to avoid exceeding its limits2.
Moreover, owing to its rich vascularization11, the frontal paramedian flap is quite versatile and its rotation arc can be extended and its end can be thinned through frontal myectomy, which enables molding of the recesses and projections that are normal in the nose because of its relatively thin cutaneous coverage8.
Most surgeons perform nasal reconstruction in two or three stages, including flap thinning, repositioning of the eyebrow head, and other alterations. In general, flap release is performed between postoperative day 15 and 21, at which time the flap is autonomized2,8. Others perform nasal reconstruction in a single procedure using free flaps12.
Despite not achieving an objective method to verify nasal respiratory function in our study, most authors suggest that reconstruction of the lining with nasal mucosa and use of cartilaginous grafts for support are the best options to maintain air flow permeability, which was verified subjectively in the present research2,5,8.
CONCLUSIONS
Reconstruction of complex nasal defects is challenging to plastic surgeons. Replacement of nasal tissues with similar tissues promotes the best aesthetic and functional results and is associated with fewer complications. With regard to the functional results, further objective assessments should be performed to confirm the present findings.
REFERENCES
1. Anbar RA, Arruda AM, Reis GC, Santos L. Reconstrução nasal com emprego de retalho médio-frontal. Rev Bras Cir Plást. 2010;25(1):208-10.
2. Menick FJ. A 10-year experience in nasal reconstruction with the three-stage forehead flap. Plast Reconstr Surg. 2002;109(6):1839-55.
3. Bhrany AD. Complex nasal reconstruction: a case study: reconstruction of full-thickness nasal defect. Facial Plast Surg Clin North Am. 2011;19(1):183-95.
4. Burget GC, Menick FJ. The subunit principle in nasal reconstruction. Plast Reconstr Surg. 1985;76(2):239-47.
5. Burget GC, Menick FJ. Nasal reconstruction: seeking a fourth dimension. Plast Reconstr Surg. 1986;78(2):145-57.
6. Weber SM, Wang TD. Options for internal lining in nasal reconstruction. Facial Plast Surg Clin North Am. 2011;19(1):163-73.
7. Immerman S, White WM, Constantinides M. Cartilage grafting in nasal reconstruction. Facial Plast Surg Clin North Am. 2011;19(1):175-82.
8. Menick FJ. Nasal reconstruction. Plast Reconstr Surg. 2010;125(4): 138e-150e.
9. Angobaldo J, Marks M. Refinements in nasal reconstruction: the crossparamedian forehead flap. Plast Reconstr Surg. 2009;123(1):87-93.
10. Belmar P, Eusebio E, Sánchez C, Vergara A, Martín A, Juanes A, et al. Paramedian forehead flap for the reconstruction of extensive nasal defects. Actas Dermosifiliogr. 2011;102(3):187-92.
11. Reece EM, Schaverien M, Rohrich RJ. The paramedian forehead flap: a dynamic anatomical vascular study verifying safety and clinical implications. Plast Reconstr Surg. 2008;121(6):1956-63.
12. Cinpolat A, Bektas G, Coskunfirat OK. Complex partial nasal reconstruction using free prelaminated temporoparietal fascial flap. Microsurgery. 2013;33(2):156-9.
1. Master's degree, full member of the Sociedade Brasileira de Cirurgia Plástica (Brazilian Society of Plastic Surgery - SBCP), plastic surgeon at the Hospital Universitário Oswaldo Cruz da Universidade de Pernambuco (Oswaldo Cruz University Hospital at Pernambuco University), Recife, PE, Brazil
2. Specialist member at the SBCP, plastic surgeon at the Hospital Universitário Oswaldo Cruz da Universidade de Pernambuco (Oswaldo Cruz University Hospital at Pernambuco University), Recife, PE, Brazil
3. Medical Clinic resident specialized in Dermatology by the CEDER in the Santa Casa de Misericórdia in Recife - Santo Amaro Hospital, Recife, PE, Brazil
4. Specialist member at the SBCP, plastic surgeon at the Instituto Materno-Infantil de Pernambuco Professor Fernando Figueira (Professor Fernando Figueira Mother-Child Institute of Pernambuco - IMIP), Recife, PE, Brazil
5. Full member at the SBCP, plastic surgeon at the IMIP, Recife, PE, Brazil
6. Medical School student at the Universidade Federal de Pernambuco (Federal University of Pernambuco), Recife, PE, Brazil
7. Adjunct Professor at Universidade de Pernambuco (Pernambuco University), chief of the Plastic Surgery Service at the Hospital Universitário Oswaldo Cruz da Universidade de Pernambuco (Oswaldo Cruz University Hospital at Pernambuco University), Recife, PE, Brazil
Correspondence to:
Rodrigo Campos Soares Quintas
Serviço de Cirurgia Plástica do Hospital Universitário Oswaldo Cruz da Universidade de Pernambuco
Rua Arnóbio Marques, 310 - Santo Amaro - Campus Universitário
Recife, PE, Brazil - CEP: 50100-130
E-mail: rodrigo-quintas@hotmail.com
Submitted to SGP (Sistema de Gestão de Publicações/Manager Publications System) of RBCP (Revista Brasileira de Cirurgia Plástica/Brazilian Journal of Plastic Surgery).
Article received: February 17, 2013
Article accepted: April 11, 2013
This study was performed at the Hospital Universitário Oswaldo Cruz da Universidade de Pernambuco (Oswaldo Cruz University Hospital at Pernambuco University), Recife, PE, Brazil.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter