

Original Article - Year 2014 - Volume 29 -
Mini-invasive facelift, an effective procedure through small incisions
Ritidoplastia mini-invasiva, um procedimento efetivo através de pequenas incisões
ABSTRACT
INTRODUCTION: A restoring procedure of the ageing process of the face should consider the conditions of the soft tissues and the relationship between them and the existing skeletal volume. This could be done through different approaches: open, endoscopic or mini-invasive. To present our concept of mini-invasive facelift, a full facelift through minimal incisions, product of eighteen years of experience.
METHODS: The mini-invasive facelift is done through minimal incisions located on the frontal hairline, temporal area, triangular fossae of the auricle, submentalis sulcus and eyelids. A wide dissection is performed to liberate the parieto-temporal fascia from the zigomatic arch, to pull it up in continuity with the SMAS and the platysma as one continuous layer or composite flap. These structures are selectively fixed to a higher position restoring the location of the soft tissues and the contour of the face.
RESULTS: We have done this procedure to 672 patients, along 19 years, with minimal complications (described also), and avoiding the pre-auricular incisions in 89% of our patients. In this paper details and tips to perform this procedure in a safer way and to get the most natural results are presented.
CONCLUSIONS: Different approaches are described to perform a face lift with specific mini access views according to the regions to be treated , without periauricular scar round 89% of the operated cases.
Keywords: Rhytidoplasty; Facial Surgery; Incisions; Surgical Procedures; Minimally Invasive
RESUMO
INTRODUÇÃO: Os procedimentos aplicados nos problemas de envelhecimento facial devem ficar restritos aos tecidos brandos e às relações com o volume prévio do esqueleto. Eles podem ser realizados mediante diversas técnicas: dissecção ampla e aberta, endoscópica e mini-invasiva. O objetivo é apresentar nossa concepção de ritidoplastias mini-invasivas e ritidoplastias completas através de mini-incisões, após 18 anos de experiência.
MÉTODOS: A ritidoplastia mini-invasiva é realizada através de mini-incisões localizadas na linha do cabelo da região frontal, região temporal, na fossa triangular da orelha, no sulco submentoniano e nas pálpebras. Ampla dissecção é realizada para liberar a fáscia parietal do arco zigomático para elevar em continuidade com o SMAS e o platisma num único plano. Essas estruturas são seletivamente fixadas em posições mais elevadas, restaurando a posição dos tecidos brandos e o contorno da face.
RESULTADOS: Nossa experiência se apoia em 672 pacientes, operados durante 19 anos, com mínimo de complicações a serem registradas, tendo sido evitadas as incisões pré-auriculares em 89% dos pacientes. Estão registrados os detalhes e táticas de como realizar cirurgias com segurança e a qualidade dos resultados.
CONCLUSÕES: Diferentes procedimentos são descritos para mostrar como realizamos as ritidoplastias com minivias de acesso, de acordo com as regiões tratadas e sem cicatrizes pré-auriculares em 89% dos casos operados.
Palavras-chave: ritidoplastia; cirurgia facial; incisões; técnicas minimamente invasivas
Through the ageing process all the tissues of the face are affected in different ways, the skin loses elasticity, fat reabsorbs, muscles lose tone and volume, and the bone loses volume also, which leads to descent and increasing laxity of the overlying soft tissues that rely on it for support. The skin is not a supporting structure and it is displaced by falling subcutaneous soft tissues. With age it loses elasticity, so applying direct traction to the skin will cause further deterioration, transforming the skin in an inert layer, hypotonic and unnatural. Fornatural results, the skin should be redistributed indirectly by relocating deep soft tissues.
Based on this principle, an effective method of facial rejuvenation should also include restoring lost bony volume. While there is not yet one satisfactory method of achieving this, a good alternative is to restore the conditions of the soft tissues and the relationship between them and the existing skeletal volume. To achieve this effectively, a deep plane approach is required.
The subperiosteal dissection has the advantages of a relative avascular plane dissection away from nerves and that allows displacement of the soft tissues of the face in block, as one continuous layer or composite flap, without disturbing the original relationship between the skin and the deep soft tissues. By preserving the anatomical relationship between the periosteum, muscles and the skin, a cushion effect is provided that allows the traction applied to the deep soft tissues indirectly tense the skin, but in a smooth and natural way1-5 .
A deep plane facelift sub or supraperiosteal , could be done open, through a coronal approach or by using small incisions with a endoscopic method6-8. As we gained experience with the endoscopic approach, we found it possible to carry out most of the maneuvers of the endoscopic facelift, through small incisions but without endoscopic assistance9-12.
This paper presents my experience of almost 20 years performing "Minimally Invasive Facelift", and I describe in it the procedure, and useful details which have helped me to get better results.
METHODS
Preoperative clinical assessment
The patient is assessed at rest without contracting the frontalis muscle and looking straight ahead. In most cases the horizontal forehead lines have been produced by chronic contraction of the frontalis muscle that the patient activates out of habit, during expression or to elevate the eyebrows in an attempt to eliminate the weight and shadow caused by the agglomerated skin at the upper eyelid ( blepharochalasia ). Limiting the frontalis muscle action during the evaluation confirms the actual position of the eyebrows and excess upper eyelid skin, and helps to plan with more precision a possible brow lift. The displacement and redundancy of the soft tissues of the cheeks are also evaluated. The neck is evaluated considering amount of fat, muscle laxity, elasticity and skin redundancy.
We have classified the severity of ageing changes into 4 groups:
Grade I: Flabbiness and incipient fall off the mid-face and the neck skin good turgor.
Grade II: Flabbiness and evident mid-facial fall and incipient neck flabbiness
Grade III: Incipient flabbiness of the mid-face and evident neck flabbiness.
Grade IV: Evident mid-face and neck flabbiness.
The "Minimally Invasive Facelift" procedure described here has been designed to restore the aging face, antagonizing the gravity that affects the soft tissues, by using vertical displacements and selective suspensions. Variations of the procedure are done in each patient depending on its degree of aging.
Surgical Technique
The procedure can be done under general or local anesthesia with sedation. For local anesthesia, bilateral block are done of the supraorbital, infraorbital, mandibular, and mental nerves and the superficial cervical plexus. The area is infiltrated with a vasoconstrictor solution (1ml of 1:1000 epinephrine, 25ml of 2% lidocaine and 8ml of Bupivacaina in 175ml of normal saline). For those cases under general anesthesia the same solution but without lidocaine, is infiltrated.
Frontal and Eyelid Region
In this area the goals are to eliminate the horizontal lines, to raise the eyebrows to an aesthetically appealing height with the desired contour, and to balance the function of the muscles of facial expression.
Two access are used. A bilateral 2cm. Incision just above the lateral eyebrow at the hairline. To site these incisions two lines are drawn both starting at the lateral margin of the nasal ala, one continuing up through the lateral corneal margin while the other passes through the pupil and both meet the hairline.The incision is placed at the hairline between these two lines, parallel to the eyebrow (Figure 1). In cases with grade I rhytidosis where there is usually minimal redundancy of the upper lid skin, only a conservative brow lift is required without the need for an upper lid blepharoplasty. Those patients with evident upper lid redundancy (grades II-IV rhytidosis), superior orbicularis hypertrophy or fat bags herniation, require also a transpalpebral approach through a conventional blepharoplasty incision.Through the hairline incisions a subperiosteal dissection is done and carried down to the superior orbital rim, surrounding the emergency of the troclear an supraorbital nerves, protected by applying a finger tip on them (Figure 1).
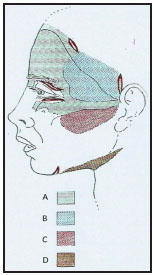
Figura 1. Dissection areas. (A) Subperiosteal. (B) Under the temporo-parietal fascia. (C) Sub- superficial musculoaponeurotic system (SMAS). (D) Subcutaneous. Incisions for the approach to these regions.
Subperiosteal dissection above the hairline incisions (fronto-parietal area) is performed only in those cases where hairline elevation is indicated. The attachment of the temporo-parietal fascia where it blends with the frontalis must free off the superior temporal line on both sides.
The subperiosteal dissection plane has less bleeding and be able to move and redrape the soft tissues on block. In order to do so and to treat the depressor muscles it is necessary open the periosteum 2cm. above the nerves, so it is cut side to side horizontally. In this way the eyebrows are liberated from the deep soft tissues and the vertical traction acts directly on them. Partial excision or disfunctioning of procerus and depressor supercilii is indicated in those patients who need elevation of the medial third of the brow, or to correct the vertical lines in the glabelar area.
A conventional blepharoplasty incision is made, resecting redundant skin and orbicularis muscle present. Usually more muscle than skin is resected to reduce its redundancy but caring to leave enough skin to drape the supratarsal concavity of the upper lid. Dissection is done bluntly with scissors, between orbicularis and the orbital septum, taking care to not let retroseptal fat extrude by inadvertently opening the septum. The supraorbital rim is reached and the periosteum is incised horizontally. Through this incision, subperiosteal dissection of the superior orbital rim is carried out upwards to connect with the previous dissection performed from above. Orbicularis is weakened and separated from the frontalis muscle by resecting an arcus marginalis strip, 4 to 5mm. wide (Figure 2).
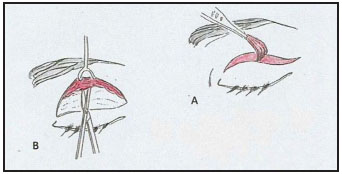
Figure 2. Transpalpebral frontoplasty. (A) Skin-muscle resection. (B) Dissection behind the orbicularis oculi muscle, to the superior orbital rim. (C) Arcus marginalis strip resection. (D) Subperiosteal dissection of the superior orbital rim, and exposure of the neurovascular bundles. (E) Subperiosteal dissection of the frontal region.
The blunt dissection behind the orbicularis muscle in the supero-medial angle of the orbit leads to the depressor supercilii muscle, characterized by its vertical fibers and its deep red color. Continuing up medially to the glabella area the dissection is performed in two planes, one subcutaneous and the other subperiosteal. The procerus muscle lies between these two planes and is sectioned at different levels to dysfunction it. Bleeding from this maneuver can be controlled by local pressure. If indicated, partial or total resection of the depressor supercilii is performed. Corrugator muscle could be also treated, by reaching it in between its medial insertion and the supra-orbital nerve taking care not to dysfunction it totally in order to avoid causing excessive separation of the medial brow13,14. In those patients on who a blepharoplasty is not indicated the treatment of the muscles could be performed endoscopically from above.
Generally, the eyebrow lift caused by improvement in frontal muscle action significantly reduces the presence of the fat pads of the upper eyelid,but if they still obvious, are grasped gently with fine forceps and cauterized, causing contraction of the orbital septum and intrusion of the fat pads. In those cases where the upper lid bags are extremely obvious, the orbital septum could be also plicated with absorbable 6-0 sutures to reduce fat herniation. The upper lid incision is closed with an intradermal running suture using 5/0 nylon and suturing the upper skin border to the lower border including the tarsal plate to give good definition to the supratarsal fold.
Because frontalis muscle is acting only on the medial brow its action elevates the two medial thirds of the brows, any procedure that improves its function will result in elevation of the medial part of the eyebrow but the lateral part will remain descended, giving a facial expression of surprise or sadness, at less the lateral part will be elevated also by its selective traction and fixation to obtain an adequate brow contour. Once homeostasis is achieved in this region, suspension of the lateral third of the brow is carried out by using 4/0 polyglactin sutures. A retractor is used in the frontal hairline incision to aid passage of the suture needle to place "backward and forward sutures", the needle is introduced downwards through this tunnel in a subperiosteal plane to the upper edge of the horizontal incision previously performed to the frontal periosteum and partially going through the skin (Figure 3).

Figure 3. Ciliary suspension, anchored with a "Backward and forward suture" to a monocortical tunnel.
Once the posterior end of the needle is found at the subcutaneous level, it is returned 1cm along this plane, grasping there a thick bite of subcutaneous tissue, and then back to the subperiosteal plane where the two extremes of the suture are joined. Bringing them back out through the hairline incision allows putting moderate traction on the brow without dimpling or marking the skin. The suspension could be fixed to the periosteum and subcutaneous tissues located above this incision or to a monocortical tunnel if by any reason the local soft tissues are not strong enough. A monocortical tunnel is a easy procedure, that provides excellent suspension without the need to place screws or any other foreign material that could be palpated or that will need to be removed later on.
When there are asymmetric upper lids, different tension is applied to correct it. Sometimes the brow elevation with this method causes bunching of skin around the hairline incision, in these cases a short incision perpendicular to the center of the lower edge of the hairline incision is done, creating two small skin triangles to be resected without increase the original length of the incision. Wounds are closed subcutaneously with long term absorbing sutures. In order to have stable fixation of the frontal soft tissues to its new position, the remnant action of the muscles in this region is controlled with Botulin toxin applied to the depressor muscles one week before to the surgery.
Cheeks
For practical purposes we divide the cheeks into two areas, medial or centro-facial and latero facial ( pré-auricular ).
Centrofacial area
This area extends from the naso-labial fold, to the lateral limit of the malar /cheek prominence. Attention here is focused on correcting the naso-labial fold, the malar bags and the laxity of the soft tissues in this zone. This area can be addressed as an isolated procedure or combined with a blepharoplasty, is the case of patients with rhytidosis grades I and II, or combined with a full face-lift in grades III and IV15,16.
The approach for this procedure is a conventional inferior blepharoplasty skin incision. Subcutaneous dissection one centimeter wide along the lower eyelid and near to its lateral end, and a horizontal opening of the orbicularis muscle, one centimeter long, and one centimeter below the eyelid margin.
Through this approach blunt dissection is continued behind orbicularis until the inferior orbital rim is reached and from there down in a supraperiosteal plane over all the surface of the maxilla. This is a small area, so a sub-periosteal dissection is no necessary. Using the same "back and forward" suture (Figure 4), described for suspension of the brow, two sutures (4/0 polyglactin) are placed lifting the deep soft tissues. The medial is fixed to the infraorbital rim periosteum or arcus marginalis, and the lateral one to the periosteum of the lateral orbital rim or the temporal fascia. In cases where this structure is not strong enough, a drill hole is made in the inferior orbital rim. If the suspension sutures cause obvious dimples in the skin they should be relocated at a deeper level. This vertical suspension of the cheek soft tissues corrects the naso-labial crest, the tear through deformity, and the herniating lower lid fat pads. This procedure produces obvious elevation and redundancy of skin and orbicularis muscle of the lower lid, that may encourage generous resections of these tissues, but because we have observed this skin retracts a lot, it is important to be very conservative and to resect no more than half of the apparent excess, in order to avoid an ectropion. The excess orbicularis muscle can either be resected, used as a flap to fix it laterally as a cantopexy or rolled over it to act as a filler of the infraorbital rim area, maneuver that is very useful in patients with evident ageing of the orbital area or to correct excessive fat resection of a previous blepharoplasty.
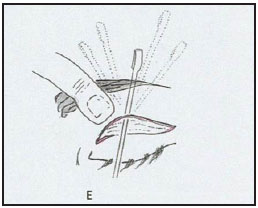
Figure 4. Backward and forward' suture to take the deep subcutaneous tissues of the nasolabial crest as composite flap and suspend them to the arcus marginalis or periosteum of the infraorbital rim.
To improve the "crows feet" the area lateral to the lower lid incision and its surroundings is detached sub-periosteally, and its periosteum is incised with scalpel in a radial way allowing the orbicularis muscle to spread out and redrape . To correct malar bags, the orbicularis muscle is freed detaching its posterior surface and low insertion, pulling them up in direction of the lateral canthus. A horizontal ellipse of skin is resected from its edge at the outer third of the lower eyelid incision. The muscle defect is closed and anchored by two sutures (polyglactin 4/0) to the periosteum in this region at the level of the lateral canthal ligament or even higher, depending on the desired effect. This technique has proven very useful for correcting this deformity that is due to the redundancy of the inferior orbicularis muscle resulting of the loss of projection of the malar bone. This gives also support to the tarsal component of the orbicularis muscle and prevents post-operative ectropion that can result from temporary palsy of the orbicularis due to edema or surgical handling17-20 (Figure 5).
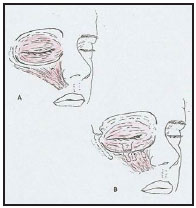
Figure 5. Vertical and lateral traction of the orbicular orbis muscle, to correct the malar fat bag.
These lateral sutures can be placed under direct vision if an upper blepharoplasty is being done at the same time or, if not, can be placed blind using the "back and forward" technique.
Latero-facial area
We use two approaches to correct this area, temporal and trans-auricular. The temporal is usually a vertical incision, 3 to 4cm long running vertically above the ear. Thetemporal area is dissected between the parieto-temporal fascia and the deep temporal fascia to the superior temporal line, where it communicates with subperiosteal dissection previously made on the forehead. Dissection continues downward until it reaches the upper edge of the zygomatic arch.
The parieto-temporal fascia, SMAS and platysma are different structures but connected in between as one continual anatomical layer. The best way to detach and move them as one structure only, is freeing their insertion to the zygomatic arch. This could be done through the supra-auricular incision, the lower blepharoplasty incision, a vestibular approach or by a trans-auricular approach, depending of the surgeon preferences. The dissection is directed to reach the zygomatic arch where the periosteum is opened using a sharp curved elevator. Dissection of the zygomatic arch is continued, firstly over its anterior surface as far as the malar, which is partially dissected taking care not to damage the infraorbital nerve by protecting it applying a finger tip of the other hand percutaneously, on top. At this point the dissection could be communicated with the supraperiosteal dissection performed on the centro-facial area. Following along the lower edge of the arch to reach the rear surface of the SMAS and continue down dissecting between the SMAS and the masseter muscle, using anoval blunt dissector (Figure 6). The SMAS is freed from the deep tissues of the cheek although the degree of dissection is tailored according to what each patient requires.
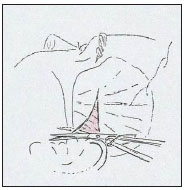
Figure 6. Blunt dissection between the SMAS and the masseter muscle, performed with a blunt, oval-ended dissector.
The subperiosteal dissection of the arch is completed by directing along the superior edge of the arch where this dissection communicates with the previous dissection done from above in the temporal region. Given the proximity of the front-temporal branch of the facial nerve, this dissection should be done upwards carefully controlled by percutaneous palpation or with a finger tip through the temporal incision.
Once the periosteum has been freed off the zygomatic arch it is easy to displace the SMAS upwards across the cheek by pulling up the parieto-temporal fascia.
To achieve the maximum mobilization of SMAS and indirectly of the overlying cheek skin, which is required for patients with severe age changes (grade III and IV rhytidosis), the pre-auricular SMAS should be dissected from above through the temporal incision in two different planes, making a subcutaneous and a sub-SMAS tunnel taking care not to damage the temporal vessels. Holding the scissors with one blade under and one blade above the SMAS this is cut vertically, about one centimeter in front of the ear, stopping at the level of the tragus to avoid injury to the facial nerve (Figure 7). This frees up the lateral attachments of the SMAS and allows a larger displacement of this structure. Dissection and traction to this layer must be symmetrical on both sides of the face.
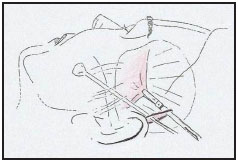
Figure 7. Pre-auricular SMAS vertical section through the extended temporal approach.
In some cases of extreme rhytidosis we carry out the subperiosteal dissection in the medial third of the face and malar area through an additional intraoral incision made in the vestibular upper sulcus. In those cases in which it is necessary to apply some tension to the lateral canthal area to correct the "crows feet", the temporal incision is extended from back to front from its superior end with an incision directed diagonally from above to below in direction of the eyebrow tail, but keeping it within the hair of the temple area.
The suspension starts with two or three suspension sutures for the SMAS, placed in the pre-auricular area in oblique direction forward and upwards, to be anchored to the deep temporal fascia, allowing the pre-auricular skin to be redistributed without agglomerate in the pre-auricular area which would require of pre-auricular excision.
The parieto-temporal fascia is pulled and suspended vertically, suturing it to the deep temporal fascia in a stepwise fashion with 2 or 3 sutures at 3 different levels in order to disperse the tension and prevent ischaemia causing dehiscence of the supported tissues (Figure 8). It is necessary to take care to place these sutures either side of the path of the frontal branch of the facial nerve to avoid catching the nerve with a suture. Some stitches are applied to pull and fix the temporal skin flap to the temporal aponeurosis, taking the segments of parieto-temporal fascia included in it.
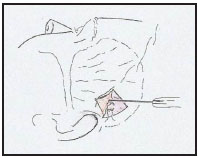
Figure 8. Temporo-parietalis fascia attached to the temporal skin flap is pulled up and fixed to the temporal aponeurosis also.
There is usually no skin excess in the temporal region and the incision is simply closed directly without tension.
Adjuvant Procedures
In many of our patients we perform other procedures at the same time such as platysmoplasty, autologous fat injection, lateral cantopexy, senile ptosis correction, ear lobule reduction, chemical or laser peels, dermabrasion, rhinoplasty, genioplasty, lip augmentation and in patients with a previous rhytidectomy the revision of scars or even hair transplants to alopecic areas.
Postoperative Treatment
The ends of the sutures are fixed with micropore tape and all the sutured incisions are covered with it. The forehead, the cheeks and the neck are covered with strips of micropore also.
The strips are placed horizontally in the forehead, on the cheeks directed diagonally, and on the neck transversely on the sub-mandibular region, from one side to the other, passing through the sub-mental area. The intention is to constrain with this tape the possible distention of the soft tissues due to edema or hematoma, and accordingly the possible detachment of the sutures. We have observed that, in those areas where the micropore is used, the bruising is substantially reduced.
In some cases where we consider the possibility of a post-op bleeding, a suction drain is placed in the cheek areas to prevent hematoma, and the area is protected with gauzes, cotton and a soft bandage around the head. In contrast, in those patients where drains are not necessary the areas are left unbandaged, prescribe the frequent use of cold compresses in order to encourage local vasoconstriction, the control the swelling, and reduce a possible bleeding.
For suturing we use resorbable material placed in sub-cuticular fashion, so much of the times it is not necessary to remove the stitches. The knots are cut at 4-5 days and the wounds covered with narrow strips of micropore for 8 more days. About 15 to 20 days later, in which most of the edema has gone, any prominent or no absorbable suture ends will be removed.
The use of absorbable sutures reduces the possible pain caused by removing the stitches and particularly for those foreign patient or with busy schedules which find it difficult to attend to frequent checks (Figure 9).
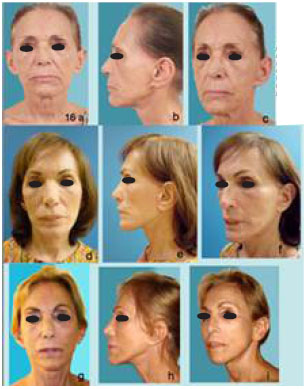
Figure 9 (A - B ) 48 year old female patient with Rhitidosis grade I - II. ( C - D ) 14 months after mini invasive endo-forehead , mini-invasive facelift , centro-facial lifting through lower blepharoplasty approach, lateral facial trough temporal approach .( No peri-auricular incision ).
RESULTS
We have been doing mini-invasive face lift procedures with some variations since 1993, for a almost fifteen years experience. During the last 9 years we have carried out the procedures described in this paper or combinations of them, depending on individual patient requirements, on a total of 539 patients, 436 women and 103 men.
We have been able to avoid the pre-auricular incision in all the patients with rhytidosis grade I and II, virtually in most with grade III, but it have been necessary in all the grade IV cases, so 83 % of our cases do not have pre-auricular scars.
There are almost no ecchymosis . The swelling is discreet to medium and disappears in about 15 days to one month. Two months later the patients shows very natural results. The complications have been relatively minimum, such as temporary hypoesthesia of the forehead (15%), or of the cheeks (5%), as well as an occasional temporary palsy of the front-temporal branch of the facial nerve lasting between three to four weeks. All these manifestations were solved spontaneously.
We apply Botulin toxin to the occipito-frontalis muscle, and to the depressors muscles, ten days before the surgery, in this way we will not observed manifestations of post-operative facial palsy, if during the surgery by accident a nerve is stretched, affecting their function it will recover before the effect of the Botulin toxin disappears.
This is a useful resource to keep a good relationship with our patient, avoiding any possible conflict due to a temporary palsy, by the effect of the Botulin toxin in the mean time that the temporary palsy disappears.
Given that the areas where skin is undermined are minimal, and limited to specific cases we have had very few problems with hematomas (3%). In only one case it was necessary to take the patient back to the operating room to check the homoeostasis, but the others did not required any operative intervention, only its simple drainage in the office.
In this mini-invasive facelift the deep soft tissues are pulled upwards and are relocated, but the skin is not dissected subcutaneously, neither stretched, respecting its consistency and remnant elasticity, factors that helps to get more natural results (Figure 10). Because the skin do not charge any more the deep soft tissues spontaneous and progressively retracts itself, improving its quality and in general the result day by day. The patients express their satisfaction because they realize that they looks better "every day", even two or three years after the surgery.
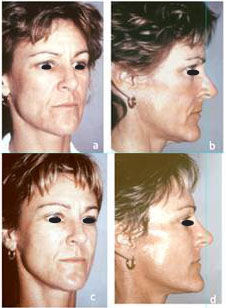
Figure 10 ( A - B ) 57 year old female patient with Rhitidosis grade IV. ( C - D ) 17 months after mini-invasive facelift ( Trans-palpebral endo-forehead , upper and lower blepharoplasty centro facial endo-lifting through lower blepharoplasty approach , antero-facial correction through temporal approach and hammock platismoplasty. ( No pre-auricular incision ). ( E ) detail of the peri-auricular scar.
DISCUSSION
The vertical suspension of the deep soft tissues is an important factor of the contemporary facelift. In the centro-facial area the vertical suspension corrects the naso-labial crest and the tear through, gives excellent definition to the lower lid contour and eliminates the effect of downward pull exerted by soft tissue to the orbital septum. Elevation of these tissues allows the fat pads to return to their original position within the orbit, restoring the volume of the orbital contents, and moves the eyeball forwards that slightly raises the upper eyelid, getting a more open eyelid fissure where the light gives to the eye a youthful shine 21-24.
The dissection of the centro-facial area could be done in a sub-periosteal or supra-periosteal plane depending of the surgeon's preference, but both approaches will produce the same effect in most of the cases.
Just in some cases of extreme rhytidosis the sub-periosteal dissection in the medial third of the face and malar area is carried out through an additional incision on the vestibular upper sulcus, which allows quick, direct and safe access, but adds considerable postoperative edema.
The aging process affects the volume, structure and consistency of the tissues, the neck platysma and skin are displaced inferiorly, giving the neck a convex profile. The vertical displacement of the parieto-temporal fascia in continuity with the SMAS and platysma muscle, improve in good proportion aging alterations of the neck, so we treat the neck at the end of the facelift and rarely we do neck corrections in isolation. The eyelids also are rarely addressed in isolation because the upper lid is intimately related to the eyebrows and the forehead, and this whole area should be treated as one unit. The lower lid is usually treated as part of the midface region (Figure 11).Occasionally we treat the eyelids in isolation although, but try to broaden our focus to offer the patients the maximal possible benefits. This concept gave origin to our term " centro-facial lifting13,which consists of correcting brow position, improve cheek, the nasolabial crest, and blepharoplasty all through a conventional blepharoplasty approach. We do not use permanent sutures, only long term reabsorbable ones, because in our experience mechanically speaking, there are not needed of the sutures beyond 3 weeks, and permanent sutures may be palpable later on.

Figure 11 (A) 49-year-old male patient, rhytidosis grade III. (B) 12 months after mini-invasive endo-forehead, mini-invasive facelift (upper blepharoplasty, centro-facial lifting, latero-facial correction through temporal approach and hammock platysmaplasty), deep and superficial lipoinjection (no preauricular incisions).
So far these minimally invasive techniques, have given excellent very natural results in our hands. In the cases with grade IV deformity and some grade III with obvious skin redundancy, it is necessary to combine these procedure with a traditional subcutaneous facelift in the lateral cheek region, via pre-auricular incisions. In these cases the incision is done at the edge of the tragus and the subcutaneous dissection is no more than 3 to5 cm wide, to allow remove the redundant skin, which is trimmed conservatively in order to allow its redistribution over the pre-auricular area without tension. With age, the skin loses its elasticity and its remaining must be preserved by avoiding subcutaneous dissection and skin tension. In these cases we have observed that by trying to dissect and tighten the SMAS backwards, having previously tightened the parieto-temporal fascia vertically from above, obtained minimal changes that not justify even its dissection.
The elevation of the deep soft tissues of the face gives a volume augmentation of key facial prominences, giving a natural, youthful effect.
These procedures are simple and easy to carry out, producing notable changes but needs a short learning curve to achieve the best results.
One of the great benefits of this method is to restore the structure of the face, augment cheekbone prominence, redistribute the lax skin and tighten the skin indirectly, in a more natural manner than it is done with traditional methods (Figure 12).
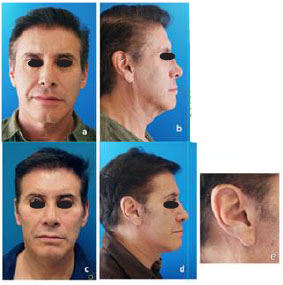
Figure12 (A, B, C, D) 54-year-old female patient, rhytidosis grades III- IV. (E, F, G, H ) 2 years after mini-invasive endo-forehead and mini-invasive facelift ( upper and lower blepharoplasty, centro-facial lifting, latero-facial correction through temporal approach, and hammock platysmaplasty), deep and superficial lipoinjection, and limited pre-auricular skin resection.
We have observed that results are more durable because this technique removes all the weight that the descent of the deep tissues exerts from behind against the skin, allowing it to recover some of its diminished elasticity. These procedures are very safe, and safer than other deep plane facelift procedures.
The Botulin Toxin applied before surgery to the frontalis, corrugator and orbicularis muscles, allows to work with relaxed muscles and will not counteract the displacement of the soft tissues we want to do. Also if a transitory palsy of the frontal nerve occurre, it will give us 6 months of break allowing in the mean time, the nerve recovery, without the pressure of an anxious patient.
The minimally invasive facelift permits to avoid long incisions and the alopecia associated with traditional coronal scars, entails minimal blood loss, causes less altered sensation in hair-bearing skin, allows to not elevate the hairline if it is not necessary, and causes less edema due to preservation of veins and lymphatic drainage pathways, accelerating the recovery period. The minimally invasive facelift that we describe here is a technique that is applicable to virtually all cases and has radically changed our conventional approach to the restoration of the soft tissue contours of the face, it has reduced the morbidity of the procedures restorers of facial aging, giving longer lasting results and greater satisfaction to our patients.
REFERENCES
1. Tessie, P Lifting facial sus periosté, Ann Chir Plast Esthéc. 1989;34:193-197.
2. Psillakis, JM ; Rumley,TO, Camargo A. Subperiosteal approach as an improved concept for correction of aging face. Plast Reconstr Surg. 1988;82:383-392
3. Ramírez OM, Maillard GF, Musolas A. The extended sub-periosteal facelift: a definitive soft-tissue remodeling for facial rejuvenation. Plast Reconstr Surg 1991;88:227-232.
4. Fuente del Campo A. Face lift without pre-auricular scars. Plast Reconstr Surg 1993;92:642-653.
5. Fuente del Campo A. Subperiosteal face-lift with staged suspension: a facial restoration method without pre-auricular scars. IN: Psillakis JM , ed. Deep-lifting techniques. New York: Thieme Medical, 1994:76-89.
6. Fuente del Campo A. Technique and auxiliary maneuvers for a face-lift without pre-auricular scars. Oper Tech Plast Reconstr Surg 1995;2:116-126.
7. Isse N. Endoscopic facial rejuvenation: endo-forehead, the functional lift. Aesthetic Plast Surg 1994;18:21-29.
8. Ramírez OM. Endoscopic subperiosteal browlift and facelift. Clin Plast Surg 1995,22:639-660.
9. Fuente del Campo A. Facial rejuvenation (endoscopic): technique and rationale. In: Fodor PB, Isse NG, eds. Endocopically assisted aesthetic plastic surgery. St Louis: Mosby, 1996:63-77.
10. Fuente del Campo A. The endo-facelift, basic and options. Rev Clin Plast Surg 1997;24:309-327.
11. Fuente del Campo A. Mini-invasive facial rejuvenation without endoscopy. Aesthetic Surg Q 1996;16(2):129-137.
12. Fuente del Campo AB, Gordon C, Kiesler Bergman O. Evolution from endoscopic to mini-invasive facelift: a logical progression. Aesthetic Plast Surg 1998;22:267-275.
13. Knize DM : Limited incision forehead lift for eyebrow elevation to enhance upper blepharoplasty. Plast Reconstr Surg 1990;86:682-694.
14. Knize DM. Transpalpebral approach to the corrugator supercilii and procerus muscles. Plast Reconstr Surg 1995;95:52-60.
15. Fuente del Campo A. Centro facial lifting. Perspect Plast Surg 1993;7:87-99.
16. Hagerty RC. Central suspension technique of the midface. Plast Reconstr Surg 1995;96:728-730.
17. Fuente del Campo A. The subperiosteal Rhytidectomy and the lower lid incision approach to the nasolabial fold. In: Bernard BW, ed. Surgical restoration of the face. Butterworth-Heinemann, 1996:169-194.
18. McCord CD. Redraping the inferior orbicularis arc. Plast Reconstr Surg 1998;102:2471-2479.
19. Hobar PC, Flood J. Subperiosteal rejuvenation of the midface and periorbital area: a simplified approach. Plast Reconstr Surg 1999;104:842-851.
20. Moelleken B. the superficial subciliary check lift, a technique for rejuvenating the infraorbital region and nasojugal groove: a clinical series of 71 patients. Plast Reconstr Surg 1999;104:1863-1874.
21. Hester RT, Vodner MA, McCord CD. The centrofacial approach for correction of facial aging using the transblepharoplasty subperiosteal cheek lift. Aesthetic Surg Q 1999;16:51-58.
22. Gunter JR. A simplified transblepharoplasty subperiosteal cheek lift. Plast Reconstr Surg 2000;103:2029-2036.
23. Fuente del Campo, A. Ritidectomia Mini-invasiva". Coiffman, Cirugía Plástica, Reconstructiva y Estética. 3ª Edic. , Amolca, Caracas, Ven., 2007,1131-1146.
24. Fuente del Campo A. Update on Minimally Invasive facelift technique. Aesth Surg Jour, 2008,28:51-61.
Member of the American Society for Aesthetic Plastic Surgery - Professor of Plastic, Aesthetic and Reconstructive Surgery, Universidad Nacional Autónoma de México
Institution: Universidad Nacional Autónoma de México.
Corresponding Author:
CAP Interlomas, 26
Ciudad del México - Méximo - Zip Code: 52786
Article received: November 5, 2013
Article accepted: January 5, 2014


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter