

Original Article - Year 2014 - Volume 29 -
Breast reconstruction with pedicle fat dermal layer associated pectorallis muscle flap
Reconstrução mamária com retalho dermogorduroso de pedículo inferior associado ao músculo peitoral
ABSTRACT
INTRODUCTION: A mastectomy is the standard treatment for all types of breast cancer (CA). This disease, with the exception of non-melanoma skin cancers, ranks first cancers that affect women. Many are the possibilities for full mastectomy reconstruction, involving autologous flaps and implant placement. Advances in the use of these techniques have been refined over the years in order to provide excellent results. The aim of this study is to describe the technique of breast reconstruction with the fat dermal inferior pedicle flap associated with pectoral and analysis of postoperative results.
METHODS: Retrospective analysis of medical records of patients operated for treatment of breast cancer in the period 2008-2013, in the private practice of the author and all patients had tumors located in the upper quadrants were selected was performed.
RESULTS: Over this period, 210 patients underwent breast reconstruction. Of these, 17 (8.09%) underwent breast reconstruction by the proposed technique. Over this period, 210 patients underwent breast reconstruction. Of these, 17 (8.09%) underwent breast reconstruction by the proposed technique. Regarding postoperative complications, there was 1 case of skin necrosis and 1 case of asymmetry.
CONCLUSIONS: Apart from technically simple and acceptable cosmetic results, the proposed flap does not result in donor site morbidity, prolonged recovery, muscle weakness with the advantage that, in most cases, be accomplished in a single operation.
Keywords: Breast Reconstruction; myocutaneous flaps; Breast cancer.
RESUMO
INTRODUÇÃO: A mastectomia é o tratamento padrão para todos os tipos de câncer (CA) de mama. Essa doença, com exceção dos cânceres de pele não melanoma, ocupa o primeiro lugar dos cânceres que acometem as mulheres. Muitas são as possibilidades de reconstrução para mastectomia total, envolvendo retalhos autólogos e colocação de implantes. Os avanços na utilização dessas técnicas têm sido aprimorado ao longo dos anos de forma a proporcionar excelentes resultados. O objetivo deste trabalho é a descrição da técnica de reconstrução mamária com retalho dermogorduroso de pedículo inferior associado ao músculo peitoral e análise dos resultados.
MÉTODOS: Foi realizada análise retrospectiva de prontuários das pacientes operadas para tratamento de câncer de mama, no período de 2008 a 2013, na clínica privada do autor. Foram selecionadas todas as pacientes que apresentavam tumores localizados nos quadrantes superiores.
RESULTADOS: No período analisado, 210 pacientes foram submetidas à reconstrução mamária. Destas, 17 (8,09 %) foram submetidas à reconstrução de mama pela técnica proposta. Com relação às complicações pós-operatórias, observou-se 1 caso de necrose da pele e 1 caso de assimetria.
CONCLUSÃO: Além de tecnicamente simples e com resultados estéticos aceitáveis, o retalho proposto não acarreta em morbidade de sítio doador, recuperação prolongada, fraqueza muscular com a vantagem de, na maioria das vezes, ser realizado em um único tempo cirúrgico.
Palavras-chave: Reconstrução de Mama; Retalhos Miocutâneos; Neoplasias da mama.
Mastectomy is the standard treatment for all types of breast cancer. Among cancers affecting women, this disease is second only to non-melanoma skin cancers. In 2012, the expected number of new cases in Brazil was 52,680, with an estimated risk of 52 cases per 100,000 women1. However, this surgery entails a loss of femininity, making the patient feel mutilated and deformed. Anxiety, depression, and marital separation often occur, greatly affecting self-esteem and even the course of treatment.
Mastectomy followed by immediate breast reconstruction is now considered the gold standard in the management of breast cancer1. There are many possibilities for reconstruction after full mastectomy involving autologous flaps and implant placement. Advances in the use of these techniques over the years have led to excellent results.
Currently, with the rise in indications for low-risk mastectomies and partial mastectomies, surgeons face a new challenge of achieving good results with less invasive surgeries.
Young patients who work full-time and place high value on aesthetics demand results that are able to cover up a mastectomy.
Reconstructive mammoplasty techniques, as well as cosmetic surgery, are used to obtain symmetrical breasts with a good shape and lasting results, and have a low complication rate.
The most important aspect of the applicability of this technique for reconstructive purposes is respect for oncological principles. This requires joint work with the mastology team performing the surgery, whose task is to ensure the safety and effectiveness of the treatment2,3,4.
OBJECTIVES
The objective of this study is to describe a breast reconstruction technique with a dermal-fat flap using an inferior pedicle associated with the pectoral muscle and to analyze the results.
METHODS
We retrospectively analyzed medical records of breast cancer patients who underwent resection from 2008 to 2013 at the private practice of Dr. Meireles Cosac. All patients with tumors located in the upper quadrants and in whom breast volume allowed preservation of adipose tissue in the lower quadrants were selected. The technique employed an inferior dermal-fat pedicle associated with submuscular prosthesis placement. The flap was a thinner variation of the pedicle described by Ribeiro3 and occupied the entire lower breast pole in a belt conformation to maintain full coverage of the prosthesis by the local autologous tissue. Thus, the implant was placed in a submuscular pocket in the upper two-thirds of the breast, with the lower-third flap being covered by the aforementioned flap.
The upper part was covered with the pectoralis major, freeing it from the rib cage and creating a suture between the detached caudal pectoral muscle to the top edge of the inferior pedicle flap. This was followed by the removal of any excess skin to enable closure of the reconstructed breast. The procedures were performed on patients with the same cancer by a single team of surgeons following the same technical criteria. The patients were monitored for a period of at least 3 months and a maximum of 5 years.
RESULTS
Over the study period, 210 patients underwent breast reconstruction. Of these, 17 (8.09%) underwent breast reconstruction using an inferior pedicle associated with the pectoralis major. The mean patient age was 53.8 years (37-78 years). This surgery was performed on patients with an average to large breast volume. With regard to risk factors, 3 patients presented with comorbidities (hypertension, diabetes, and hypothyroidism), 3 patients were smokers, and 1 patient received postoperative radiotherapy. Regarding postoperative complications, we observed 1 case of skin necrosis and 1 case of asymmetry. There were no cases of local tumor recurrence during the study period. (Figure 1)
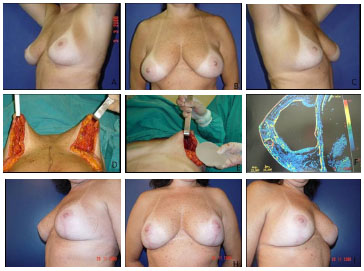
Figure 1 (A, B, C): Preoperative images. (D, E): Intraoperative images showing placement of the submuscular prosthesis and inferior pedicle, prepared in order to cover the prosthesis. (F): Magnetic resonance imaging after surgery showing the prosthesis completely covered at the upper pole by the pectoral muscle and at the lower pole by the dermal-fat pedicle. (G, H, I): Images 3 months post-surgery.
DISCUSSION
Advancement in breast cancer screening has enabled the early detection of tumors, making it possible to opt for conservative surgery followed by close monitoring. This is accompanied by greater insights into the role of genetic factors, such as mutations of the BRCA1 and BRCA2 genes, and the emergence of accessible genetic tests for risk stratification, which has led an increase in women seeking risk-reducing mastectomy.
Many young patients diagnosed with breast cancer have opted for a concomitant contralateral mastectomy4,5. In addition to genetic tests, other factors may influence the success of risk-reducing mastectomy: repeated changes in suspicious objects on mammography, precursor lesions such as atypical lesions or lobular carcinoma in situ, dense breasts that are difficult to screen, multiple lesions that require invasive investigation, and, often, patient anxiety6.
Thus, new reconstruction techniques have been tested to address these issues. There are several methods currently used for breast reconstruction, with conservative techniques, adjacent flaps, alloplastic materials, myocutaneous pedicles and microsurgical flaps, but none of them are free from limitations.
This procedure offers an adequate pocket for implant placement, does not result in excessive tension, allows amelioration of the projection in the upper and lower poles, and reduces the tendency for upward migration of the implant. Confirmation of the absence of tumor in the lower quadrants of the breast and discussion of the technique with a breast cancer specialist are essential in this type of reconstruction. Moreover, it presents minimal risk of extrusion of the prosthesis due to the interposition of viable tissue between the implant and the skin7.
The rate of complications found in this study (11.7%) is not consistent with that reported in the literature (15-45%); the rate of complications depends on the type of surgery performed, and increases with risk factors (obesity, smoking, comorbidities)7, which was also observed in this study. It is important to note that not all complications compromise the end result or require further intervention. As in the literature, smoking was associated with a significant increase in flap necrosis rates, as the only case of flap necrosis in this study occurred in a chronic smoker8. Over the study period, there was no need for surgical intervention.
Breast reconstruction plays an important role in the management of breast cancer patients. The decision on the necessity, method, and time for reconstruction requires a multidisciplinary approach between the patient, the plastic surgeon, the mastology team, and the oncology team8.
CONCLUSION
In addition to being technically simple and offering acceptable cosmetic results, the proposed flap technique does not cause morbidity in the donor site, prolonged recovery, muscle weakness, or the use of grafts. It is therefore a useful alternative in selected patients, particularly in risk-reducing adenomastectomy, and this procedure can, in most cases, be performed in a single surgical procedure.
REFERENCES
1. Instituto Nacional de Câncer (Brasil). Estimativa 2012: incidência de câncer no Brasil. Rio de Janeiro: INCA; 2011.
2. Melega, Cirurgia Plástica. Rio de Janeiro: Guanabara Koogan, 2011.
3. Ribeiro L, Accorsi A Jr, Buss A, Marcal-Pessoa M. Creation and evolution of 30 years of the inferior pedicle in reduction mammaplasties. Plast Reconstr Surg. 2002;110(3):960-70.
4. Tuttle TM, Jarosek S, Habermann EB, et al. Increasing rates of contralateral prophylactic mastectomy among patients with ductal carcinoma in situ. J Clin Oncol. 2009;27:1362-67.
5. Stucky CC, Gray RJ, Wasif N, Dueck AC, Pockaj BA. Increase in contralateral prophylactic mastectomy: echoes of a bygone era? Surgical trends for unilateral breast cancer. Ann Surg Oncol. 2010;17(Suppl 3):330-7.
6. Cosac OM, Costa LA, Barros APG. Reconstrução Mamária Bilateral com Retalhos Pediculados. In: Melega JM, Viterbo F, Mendes FH. Cirurgia Plástica: Os Princípios e a Atualidade. Rio de Janeiro: Guanabara Koogan; 2011:732-42.
7. Rozen WM, Ashton MW, Taylor GI. Defining the role for autologous breast reconstruction after mastectomy: social and oncologic implications. Clinical Breast Cancer. 2008;8(2):134-42.
8. Knobloch K, Gohritz A, Reuss E, Vogt PM. Nicotine in plastic surgery: a review. Chirurg. 2008;79(10):956-62.
1 - Plastic surgeon, member of the Brazilian Society of Plastic Surgery, Regent of the Plastic Surgery Service of the Armed Forces Hospital, Brasília, DF, Brazil
2 - Aspiring member of the Brazilian Society of Plastic Surgery, Resident of the Plastic Surgery Department of the Hospital Daher Lago Sul, Brasília, DF, Brazil
3 - Plastic surgeon, member of the Brazilian Society of Plastic Surgery, Preceptor of the Plastic Surgery Service of the Hospital Daher Lago Sul, Brasília, DF, Brazil
4 - Plastic surgeon, member of the Brazilian Society of Plastic Surgery, Regent of the Plastic Surgery Service of the Hospital Daher Lago Sul, Brasília, DF, Brazil
5 - Aspiring member of the Brazilian Society of Plastic Surgery, Resident of the Plastic Surgery Department of the Hospital Daher Lago Sul, Brasília, DF, Brazil
6 - Aspiring member of the Brazilian Society of Plastic Surgery, Resident of the Plastic Surgery Department of the Hospital Daher Lago Sul, Brasília, DF, Brazil
7 - Aspiring member of the Brazilian Society of Plastic Surgery, Resident of the Plastic Surgery Department of Hospital Daher Lago Sul, Brasília, DF, Brazil
8 - Aspiring member of the Brazilian Society of Plastic Surgery, Resident of the Plastic Surgery Department of Hospital Daher Lago Sul, Brasília, DF, Brazil
Institution: Study Center, Hospital Daher Lago Sul - DF, Brazil.
Corresponding author:
Ognev Meireles Cosac
Shtn Trecho 2, Lote 3, Condomínio Life Resorts Asa Norte Brasília- DF Bloco N, Apto. 355
E-mail: curadomed@gmail.com
Article received: January 25, 2014
Article accepted: February 16, 2014


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter