

Case Report - Year 2014 - Volume 29 -
Mondor's disease in aesthetic breast surgery
Doença de mondor em cirurgia estética de mama
ABSTRACT
INTRODUCTION: Mondor's disease is a rare, benign, and self-limiting inflammatory condition that affects the thoracoabdominal vasculature. Among the several predisposing factors of this disease, breast surgery is one of the most frequent.
CASE REPORT: The aim of this work was to describe a typical case of Mondor's disease and to discuss treatment options based on a succinct literature review, so that unnecessary procedures can be avoided in the future.
Keywords: Mondor's Disease; Superficial Thrombophlebitis; Aesthetic Mammoplasty.
RESUMO
INTRODUÇÃO: A doença de Mondor é descrita como um processo inflamatório raro, benigno e autolimitado que acomete os vasos tóraco-abdominais. São vários os fatores predisponentes e entre eles a cirurgia de mama é um dos mais frequentes.
RELADO DE CASO: O objetivo do trabalho é descrever um caso típico e tecer considerações quanto ao tratamento, após breve revisão bibliográfica, para que sejam evitados procedimentos desnecessários.
Palavras-chave: Doença de Mondor; Tromboflebite Superficial; Mamaplastia Estética.
Mondor's disease is a rare, benign, and self-limiting inflammatory process that affects the thoracoabdominal vasculature. Several predisposing factors are known, including breast surgery. This condition was first described by the French surgeon Henri Mondor in 1939 and has since been known as Mondor's disease or syndrome. To date, its physiopathological mechanism remains poorly understood. Postoperative diagnosis of Mondor's disease is important to ensure that the assistance and treatment provided to patients are adequate and reassuring.
CASE REPORT
A 54-year-old woman of average height and with a body mass index of 24.4 underwent mastopexy and breast augmentation with a 200mL textured prosthesis in October 2008.
The results of preoperative examinations were normal, including hemography, coagulography, urinalysis, and electrocardiography to evaluate the surgical risk, and chest radiography. Mammography showed both breasts classified as category 2 (BI-RADS®) with benign radiological findings. Breast ultrasonography was also performed and showed normal breasts with moderate adipose substitution.
According to the patient's medical records, she had undergone two caesarean sections and one hemorrhoid surgery, both successfully. It should be stressed that the patient smoked an average of 20 cigarettes per day.
Five weeks after surgery, the patient presented pain in the right anterior abdominal wall, running in a paramedian line on the right, below the surgical scar. A few days later, a thick fibrous cord had formed and mild skin hyperemia could be observed. The pain and cord were more evident when the patient raised the ipsilateral upper limb and/or the ipsilateral breast (Figure 1).
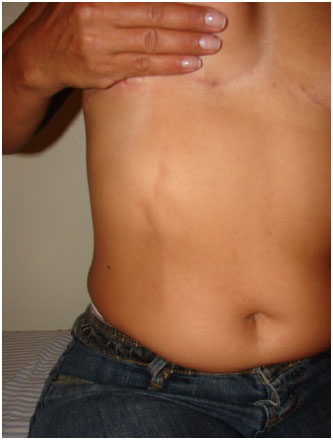
Figure 1. Appearance of the fibrous cord and superior epigastric vein during the postoperative period, after mastopexy and breast augmentation surgery.
The patient showed symptom regression and complete clinical remission within 3 weeks, with oral therapy consisting of the nonsteroid anti-inflammatory drug nimesulide at 200 mg/day. In addition, the patient was asked to rest and topically apply a wet warm compress. The patient was also encouraged to quit smoking.
DISCUSSION
The first description of compromised superficial vessels of the thorax and abdomen dates from 1869 and was performed by Fagge1-3. The French surgeon Henri Mondor further described this condition in 1939; since then, the pathology became known as Mondor's disease or syndrome. The physiopathological mechanism of this condition remains unclear, but it is currently known to involve the thrombosis of the superficial thoracoabdominal vasculature, with the thoracoepigastric, lateral thoracic, and superior epigastric veins being the most frequently involved4,5.
The causes of this disease include trauma1,2,4, surgery1,2, breast cancer2, tight clothes and compressive garments1,2, excessive physical activity1, vigorous sexual activity4, biopsy or resection of the axillary or sentinel lymph nodes3, and hepatitis C2. All of these causes are related in some way with Virchow's triad, that is, vasculature lesion, blood stasis, or hypercoagulability.
Despite compromising the vasculature, Mondor's disease can also affect the lymphatic system, and some immunohistochemical markers have been identified for differentiation, such as CD31 and D2406,7. However, any clinical application of these findings is scarce, as the treatment of the symptoms remains unchanged in both cases.
Mondor's disease has also been described in other body regions such as the penis7, neck8,9, upper limbs, and inguinal region10. Few reports indicated the development of this condition in the postoperative period of aesthetic surgery11.
Complementary examinations performed for the diagnosis of Mondor's disease include mammography and ultrasonography. Mammography can detect a limited number of findings with relevance to the diagnosis. In most cases, it only reveals superficial dilated tubular structures or alternatively, no alterations are reported9. However, it is extremely relevant for the diagnosis of concomitant breast cancer, which can be the cause of the disease. The reported frequency varies between 1% and 12.7%1,4. The ultrasonographic result can be normal or, alternatively, may reveal a superficial tubular hypoechoic structure that if associated with Doppler studies, can disclose interrupted blood flow9. Laboratory tests are not required.
Clinical examination is of crucial importance, and the most commonly reported symptom is pain1, followed by one or more superficial fibrous cords. The symptoms are aggravated when the patient performs movements of the affected region, which is characterized by hyperemia2,4,5.
Inflammation lasts from 2 weeks to 6 months, and the pain can persist from 2 to 6 weeks1,4,9.
Management of Mondor's disease focuses on the symptoms, with the use of non-steroid anti-inflammatory drugs as the only treatment option1-11. The use of corticosteroids, antibiotics, vaccines, anticoagulants2, and even manual distraction procedures was reported3, though all without any evidence of therapeutic benefits.
CONCLUSION
We can conclude that identification of Mondor's disease in affected patients is important, despite its being a rare condition. Mondor's disease is self-limiting and rarely requires any invasive approach for its remission, requiring only conservative procedures. Therefore, this report serves as a reassuring reminder for surgeons and patients that Mondor's disease usually progresses favorably toward remission in most cases.
REFERENCES
1. BauerfeindI, Himsl I, Ruehl I. Mondor's disease aftherbilateral axillary node biopsy. Arch Gynecol Obstet. 2006;27(6)3:374-7.
2. Santos JA, Santos KG, Nazário AC. Doença de Mondor. R BrasMastol. 2008;18(4):179-81.
3. Salmon RJ, Berry MG, Hamelin J P. A novel treatment for postoperative Mondor's disease: manual distraction. Breast J. 2009;15(4):381-84.
4. Schwartz R A, Trovato M J. MondorDisease. Available from: HTTP://emedicine.medscape.com/article/1087099-overview. Last accessed in 15/12/2010.
5. TIjerina AN, Saenz RA. Mondor's syndrome: a clinical finding on subfascial breast augmentation. Aesthetic Plast Surg. 2010;34(4):531-3.
6. IChinose A, Fukunaga A, Terashi H, Tanemura A, Nakajima T, Fukasawa Y A, et al. Objective recognition of vascular lesions in Mondor's disease by immunohistochemistry. J Eur Acad Dermatol Venereol. 2008;22(2):168-73.
7. Garrido HA, Muñoz CS, Fernandez L P, Ríos AA, Romero AM. Immunochemical clues to the diagnosis of Mondor's disease of the penis. Clin Exp Dermatol. 2009;34(8):e663-5.
8. Mera K, TerasakiK, Kawasaki T, KanekuraT. Mondor Disease on the neck. J Dermatol. 2009;36(3):179-80.
9. Faucz RA, Hidalgo R T, Faucz R S. Doença de Mondor: achados mamográficos e ultrasonográficos. Radiol Bras. 2005;38(2):153-5.
10. Losannoff MD, Basson MD, Salwen WA, Sochaki P. Mondor's Disease Mimicking a spigelian hernia. Hernia. 2008;12(4):425-7.
11. Bertolin SM, Martínez RG, Pastor MV, Mateo MD, Velayos J A. Mondor's disease and aesthetic breast surgery: report of case secondary to mastopexy with augmentation. Aesthetic Plast Surg. 1995;19(3):251-2.
Medical specialist of the Brazilian Society of Plastic Surgery (Sociedade Brasileira de Cirurgia Plástica, SBCP); professor of clinical surgery at the Faculty of Medicine of Barbacena
Institution: Work performed at the author's private clinic.
Corresponding author:
João Márcio Prazeres dos Santos
Street Catarina de Castro 75, Bairro Jardim Glória
Juiz de Fora, Minas Gerais, Brazil. CEP: 36036-060
E_mail: jmprazsantos@hotmail.com
Article received: February 21 , 2011
Article accepted: February 28 , 2011


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter