

Original Article - Year 2014 - Volume 29 -
Onphaloplasty: comparative study of techniques
Onfaloplastia: estudo comparativo de técnicas
ABSTRACT
INTRODUCTION: The navel is central to the appearance of the abdomen, and it is important for the umbilical scar to have a natural aspect following abdominoplasty. The objective of this study was to compare three omphaloplasty techniques.
METHOD: Forty-two patients undergoing abdominoplasty were grouped according to the technique used: in group O (n=19), the navel was resected in an oval shape and the abdominal flap incised in a vertical ellipse; in group U (n=11), the navel was resected in a short oval shape and the flap incised with an upper concavity; and in group Y (n=12), the navel was resected in a triangular shape and the flap incised in a "Y" shape. The groups were compared regarding complications and satisfaction of patients and the surgeon.
RESULTS: Three patients in group O had stenoses associated with pathological scars. A wide navel was more prevalent in the upper concave curve technique used in group U (36.36%), although the differences in prevalence rates were not statistically significantly. Pearson linear correlation test showed an association between patient dissatisfaction and navel enlargement (p = 0.0003). Patient satisfaction was evaluated using the Kruskal-Wallis test. The triangular scar group showed statistically better patient satisfaction than the upper concave curve technique (p <0.05). There was no statistical significance in patient satisfaction between oval scarring and the other methods. We found no significant difference in physician satisfaction with the three techniques.
CONCLUSION: Patients who underwent the triangular technique experienced greater satisfaction than those who underwent the upper concave curve technique. Navel enlargement was the factor most related to patient dissatisfaction.
Keywords: Abdominoplasty; Omphaloplasty; Satisfaction.
RESUMO
INTRODUÇÃO: O umbigo tem importância central na harmonia do abdome, sendo importante uma cicatriz umbilical de aspecto natural na abdominoplastia. O objetivo deste trabalho foi comparar três técnicas de onfaloplastia.
MÉTODO: Quarenta e duas pacientes submetidas à abdominoplastia foram agrupadas conforme a técnica utilizada: grupo O (n=19), o umbigo ressecado de forma oval e o retalho abdominal incisado em elipse vertical; no grupo U (n=11), o umbigo ressecado em forma pouco oval e o retalho recebeu incisão curva de concavidade superior; e no Grupo Y (n=12), o umbigo ressecado em forma triangular e o retalho incisado em forma de "Y". Os grupos foram comparados quanto a complicações e satisfações das pacientes e do cirurgião.
RESULTADOS: Ocorreram estenoses em três pacientes com cicatriz oval, associadas a cicatrizes patológicas. O umbigo largo foi mais prevalente na técnica curva de concavidade superior (36,36%), embora sem significância estatística. O teste de correlação linear de Person mostrou associação da insatisfação da paciente com o alargamento do umbigo (p=0,0003). Quanto à satisfação das pacientes, avaliada pelo Teste de Kruskal-Wallis, a cicatriz triangular foi estatisticamente melhor que a curva de concavidade superior (p<0,05). Não houve significância estatística na comparação da satisfação das pacientes da cicatriz oval com as outras, assim como não foi constatada diferença significante da satisfação do médico com as três técnicas.
CONCLUSÃO: A técnica triangular proporcionou maior satisfação às pacientes, em relação à incisão curva de concavidade superior. O alargamento do umbigo foi o fator mais relacionado à insatisfação das pacientes, nesta casuística.
Palavras-chave: Abdominoplastia; Onfaloplastia; Satisfação.
The navel is the only scar considered normal in the human body. It is present from the first days of life and is an essential component of the esthetics of the abdomen. In abdominoplasty, the shape and position of the naval are very important for a successful outcome.
The umbilicus has a rounded look, deeper at the top, limited by skin tension. Its central portion is the vestige of the umbilical cord scar. Surrounding the central portion, there is a circular depression called the umbilical groove1.
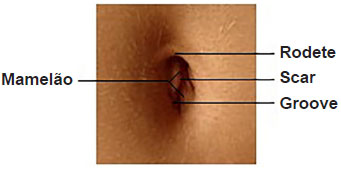
Figure 1. Navel Anatomy.
Initially, for abdominoplasties, little or no attention was given to the navel, which, in many cases, was excised with the excess adipose tissue. Noting aesthetic reasons, some surgeons began to preserve the navel, maintaining its original position2.
In 1921, Frist made the first navel transposition in abdominoplasty, using circular shapes. Flesch, Thebesius, and Weisheimer, in 1931, retained a distal skin triangle in the navel. Vernon, 1957, returned to circular shapes, but in many cases, this resulted in stenosis. Pitanguy, in 1967, performed an incision with a concave cranial curve for navel reconstruction following abdominoplasty. In 1976, Avelar published the three-pointed star technique to avoid scar retraction, with a triangular-shaped navel resection and the abdominal flap incision in the form of "Y"2, 3.
Currently, in most abdominal plastic surgeries, the umbilicus is transposed, and is kept adhered to a pedicle at the abdominal wall. The pedicle can be shortened, if necessary, by fixing, bending, or anchoring it at the aponeurosis by stitches that hold the navel in the new position in the abdominal flap2.
Several authors use various geometric shapes to treat the umbilicus scar: three-pointed star, diamonds, ellipses, crosses, shamrocks, rectangles, shields, infinity symbol, double "V", etc.3-6 In addition, some authors recommend neo-omphaloplasty in abdominal plastic surgery, especially when performed after major weight loss3,4,7,8.
OBJECTIVE
Despite being one of the most commonly performed plastic surgery procedures in Brazil, abdominoplasty does not include an ideal technique for treating the umbilicus. The aim of this study was to compare three widely known omphaloplasty techniques to evaluate complications and patient and physician satisfaction with the outcome.
METHOD
This study was characterized as an observational, cross-sectional, comparative study, based on retrospective viewing of the medical records and survey responses from female patients who had undergone classic abdominoplasty during 2011-2013, and the results were compared according to the technique used for the treatment of navel scarring.
Patients with weight variation of greater than 5 kg between the pre- and postoperative period were excluded at the time of interview.
After analysis of medical records, patients were allocated to three groups according to the omphaloplasty technique used: In group O, the navel was resected in an oval shape and a vertical ellipse incision was made in the abdominal flap. In group U, the navel was resected in a short oval shape and the flap incised with an upper concave curve. In group Y, the navel was resected in a triangular shape and the abdominal flap had a Y-shaped incision (Figure 2).
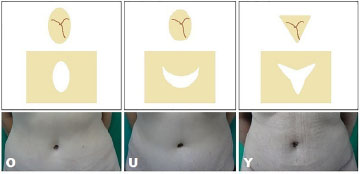
Figure 2. The omphaloplasty techniques used in this study.
During abdominoplasty, regardless of the omphaloplasty technique used, the incision sites were first marked on the abdominal flap, followed by skin incision to ensure that the umbilicus remained attached to the abdominal wall of the patient. The umbilicus was fixed with non-absorbable sutures to the aponeurosis of the rectus abdominis muscle at its edge points. The abdominal flap was incised according to the omphaloplasty technique and the peri-incisional area subjected to frustoconical-shaped lipectomy using Metzenbaum scissors. After re-assembly of the abdomen, the navel was sutured in two planes to the abdominal flap, concluding the omphaloplasty.
In post-operative care of the umbilicus, a collagenase-based ointment and restraining plasters with a surgical belt were used. Sometimes, prostheses have been used to maintain the shape of the umbilicus and/or assist in the treatment of hypertrophic scars.
Demographic data were recorded in a questionnaire and were used to confirm the homogeneity of the groups. The questionnaire also contained the ratings of patient and physician satisfaction with the navel in 4 scores: very dissatisfied, dissatisfied, satisfied, and very satisfied. These scores were used in the statistical analysis as 1, 2, 3, and 4, respectively.
Statistical tests were performed to evaluate and compare the three groups in terms of complications, patient satisfaction, and physician satisfaction, which were performed using the BioEstat 5.0 software, available for download on the internet. The level of significance was p<0.05.
The homogeneity of the groups was confirmed by the Bartlett test that enabled comparisons of three or more multivariate samples to obtain a "maximum-likelihood ratio" symbolized by φ, which can be used with equal or unequal sample sizes10.
Satisfaction was assessed using the Kruskal-Wallis test, which is a non-parametric test, also known as the H Test, used to compare three or more independent ordinal samples of equal or unequal sizes10.
The complications were compared using the Chi-Square test. The association between patient satisfaction (index 1-4, depending on the degree) and umbilicus enlargement (presence=1, no=0) was evaluated using the Person linear correlation test, which associates two variables measured at the interval level, and measures the degree and the direction of the linear correlation coefficient r, ranging from -1 to 1. The closer these values are, the stronger the association of variables10.
RESULTS
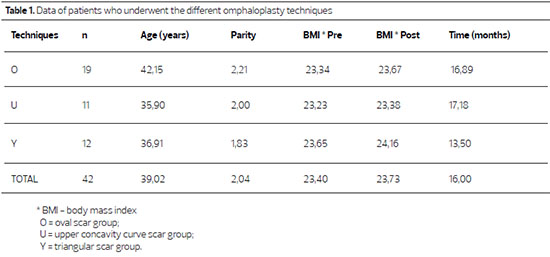
Forty-two patients who had undergone classic abdominoplasty were evaluated. The data are shown in Table 1. The groups were statistically homogeneous (φ=25.3362 p = 0.0047) in age, parity, follow-up duration, and pre- and post-operative body mass indexes.
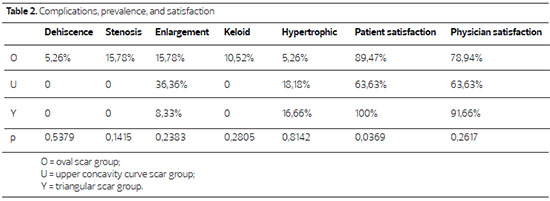
Complications are shown in Table 2. In the x2 partition test analysis, there were no statistically significant differences between the groups. There were no occurrences of infection, necrosis, or flattening of the navel.
Three patients from group O had stenosis associated with pathological scarring: keloid scars (2) and hypertrophic scars (1) were also present in horizontal scar abdominoplasty.
Navel enlargement was more prevalent in the upper concave curve incision technique (36.36%), but the prevalence rates were not statistically significant. The main cause of dissatisfaction with the navel identified by the patients was enlargement that was reported in three patients in group O, four patients in group U, and one patients in group Y (Figure 3). The Pearson linear correlation test showed an association between patient dissatisfaction and navel enlargement (p = 0.0003, r = - 0.5351).
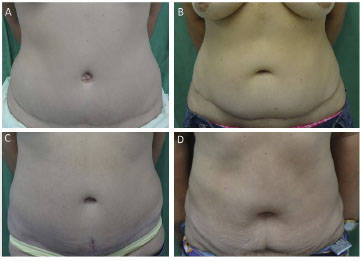
Figure 3. Patients with large navels: A - patient from group U, 27 years old, 13 months postoperatively (PO), not satisfied. B - patient from group U, 39 years old, 32 months PO, not satisfied. C - patient from group U, 43 years old, 16 months PO, not satisfied. D - patient from group O, 50 years old, 13 months PO, satisfied, dissatisfied doctor, an increase of 5 kg.
Patients in whom the triangular scar was used had statistically greater satisfaction, as evaluated by the Kruskal-Wallis test, than patients who underwent the upper concave curve technique (p <0.05). However, there was no statistical significance in patient satisfaction in the oval scarring group compared to the other group (Figure 4). There were also no statistically significant differences in physician satisfaction between the three groups (Figure 5).
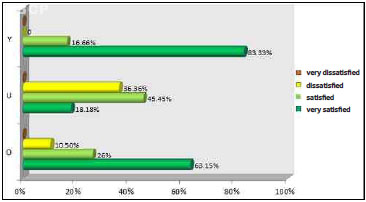
Figure 4. Patient satisfaction with outcomes for the navel.
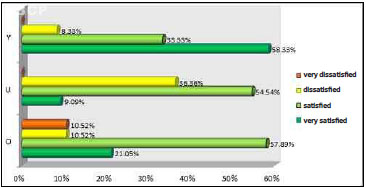
Figure 5. Physician satisfaction with the navel.
Figure 6 shows preoperative and 8-month postoperative photographs of a patient from group O who was very satisfied with the navel. The medical examiner also rated the result as very satisfactory for a good navel contour and the obvious absence of scars.
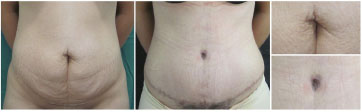
Figure 6. Preoperative and postoperative outcomes of a patient from group O who was delighted with the results.
Figure 7 illustrates preoperative and 7-month postoperative photographs of a patient from group U who was satisfied with the outcome. The doctor described the result as satisfactory due to the obvious absence of scars.
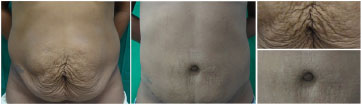
Figure 7. Preoperative and postoperative outcomes of a patient from group U who was satisfied with the outcome.
Figure 8 shows preoperative and 7-month postoperative photographs of a patient from group Y who was satisfied with the navel. The doctor described the result as satisfactory, although there was a hypertrophic scar on the upper rim.
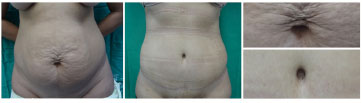
Figure 8. Preoperative and postoperative outcomes of a patient from group Y who was satisfied with the outcome.
DISCUSSION
In abdominoplasty, the shape and position of the navel is of great importance for a successful outcome. Several techniques have been proposed to achieve a natural-looking scar.
As previously well established in the literature3,5,6,7,9,11, stenosis was observed with the circular techniques used in this sample, although this included patients with pathological scars in the navel.
Navel enlargement was more prevalent in patients who underwent the upper concave curve technique (36.36%), although this was not statistically significant. From the 6 dissatisfied patients in the study, a statistically significant majority (5) were dissatisfied because of naval enlargement.
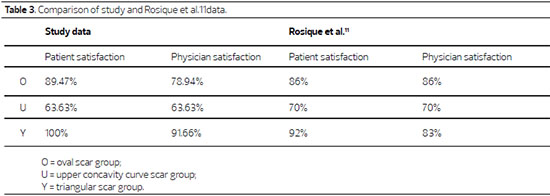
The triangular technique was assessed as being significantly better than the upper concave curve technique. Satisfaction of patients and surgeons were very similar to those found by Rosique and colleagues11, published in the Journal of Plastic Surgery in 2009. (Table 3)
The difference in satisfaction between patient and surgeon may be due to an increased tolerance for scarring and consequent subjective satisfaction by patients, because they are satisfied with the overall aesthetic improvement of the abdomen after abdominoplasty.
Plastic surgeon dissatisfaction with umbilical scarring in abdominoplasty generates a constant search for the ideal omphaloplasty technique, with many different publications concentrating on the quality of results depending on different geometric shapes, with respect to both the navel resection and the flap incision.
CONCLUSION
The triangular technique provided greater satisfaction to patients compared to the upper concave curve technique. Navel enlargement was the most common complication related to dissatisfaction of patients in the present series.
REFERENCES
1. Jaimovich CA, Mazzarone F, Parra JF, Pitanguy I. Semiologia da parede abdominal: seu valor no planejamento das abdominoplastias. Rev Bras Cir Plast. 1999;14(3):21-50.
2. Sinder R. Abdominoplastias. In: ed. Carreirão S, Cardim V, Goldenberg D. Cirurgia Plástica. São Paulo: Atheneu, 2005.
3. Tavares Filho JM, Oliveira DF, Franco TR. Umbilico e Neoumbilicoplastias. In: ed. Lima Júnior EM. Tratado de Cirurgia Plástica após Grandes Perdas Ponderais. São Paulo: Atheneu, 2010.
4. Bozola AR. Abdominoplastia: novos conceitos e tratamentos na mesma classificação de 25 anos. In: ed. Mélega JM, Viterbo F, Mendes FH. Cirurgia plástica: princípios e atualidades. Rio de Janeiro: Guanabara Koogan, 2011.
5. Freitas JO, Guerreiro V, Sperli AE. Neo-onfaloplastia na dermolipectomia abdominal: técnica do duplo "V". Rev Bras Cir Plást. 2010;25(3):504-8.
6. Furtado IR. Onfaloplastia: técnica do infinito. Rev Bras Cir Plást. 2011;26(2):298-301.
7. Nogueira DS. Neo-onfaloplastia de rotina em abdominoplastias. Rev Bras Cir Plást. 2008;23(3):207-13.
8. Abreu JA. Abdominoplastias: neo-onfaloplastia sem cicatriz e sem excisão de gordura. Rev Bras Cir Plást. 2010;25(3):499-503.
9. Avelar JM. Abdominoplasty: systematization of a technique without external umbilical scar. Aesthetic Plast Surg. 1978;2:141-51.
10. Ayres M, Ayres JM, Ayres DL, Santos AA. BioEstat: aplicações estatísticas nas áreas das ciências biomédicas. Belém, PA, 1997.
11. Rosique MJ, Rosique RG, Lee FD, Kawakam H, Glattsteins N, Mélega JM. Estudo comparativo entre técnicas de onfaloplastia. Rev Bras Cir Plást. 2009;24(1):47-51.
1 - Specialist Member of SBCP. Hospital Plastic Surgeon. University President Dutra (HU-UFMA), São Luís, Brazil. Former Plastic Surgery Resident at Fortaleza General Hospital
2 - Plastic Surgery resident at Fortaleza General Hospital
3 - Plastic Surgery resident at Fortaleza General Hospital
4 - Titular Member of SBCP. Preceptor of Plastic Surgery Department of Fortaleza General Hospital. Plastic surgeon Ceará Cancer Institute
Institution: Study conducted at the Plastic Surgery Department of Fortaleza General Hospital (FGH), Fortaleza, CE, Brazil.
Corresponding author:
Antonio Vieira Dias Filho
Rua do Aririzal, Condomínio Ville, Bloco 8, Apto 1303, COHAMA
São Luís, MA, Brasil, CEP: 65067-190
Email: vieiradias@gmail.com
Article Submitted: February 3, 2014
Article Accepted: June 1, 2014


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter