

Case Report - Year 2014 - Volume 29 -
Surgical treatment of relapsed Marcus Gunn syndrome: a case report and literature review
Fenômeno de Marcus Gunn recidivado: relato de caso e revisão bibliográfica
ABSTRACT
INTRODUCTION: Marcus Gunn syndrome is a rare and little known congenital ptosis of neurogenic origin. Its physiopathological mechanism has not been clarified. The authors report a case of pronounced ptosis that relapsed after four surgical corrections, along with a brief literature review.
CASE REPORT: A 19-year-old young adult underwent four surgical corrections of the right palpebral ptosis in other services, without a definite diagnosis of the origin of the congenital ptosis. The patient showed eyelid opening in the right eye on opening the mouth, when the eye is lateralized to the ipsilateral side, and with contralateral eye closure. The last surgery was performed 2 years prior, during which silicone bands were placed and fixated. The patient did not present any visual or neurological deficit. He underwent surgery in order to remove the silicone bands that were previously placed, to prepare the strip grafts made of fibrous connective tissue from the fascia lata of the right inferior limb, and to perform myectomy of the levator muscle of the palpebral ptosis, fixation of the fascia lata grafts at the upper edge of the tarsus with traction and fixation to the ipsilateral frontal muscle. The patient progressed with synchronic movements of the eyelids bilaterally, and without relapse of the ptosis until the present date.
Keywords: Marcus-Gunn; Palpebral ptosis; Frontal fixation.
RESUMO
INTRODUÇÃO: O fenômeno de Marcus Gunn é uma ptose congênita rara e pouco conhecida, de origem neurogênica, de fisiopatogenia ainda não esclarecida. Os autores relatam um caso de ptose acentuada e recidivada após quatro correções cirúrgicas, e fazem uma breve revisão bibliográfica.
RELATO DE CASO: Adulto jovem de 19 anos, sexo masculino, foi submetido a quatro tentativas de correção de ptose palpebral a direita em outros serviços, sem diagnóstico da origem da ptose congênita. O paciente apresentava abertura palpebral do olho direito ao abrir a boca, ao lateralizar o olhar para o lado ipse-lateral, e ao fechamento do olho contra-lateral. A última cirurgia foi realizada 2 anos antes, com posicionamento e fixação de fitas de silicone. O paciente não apresentava nenhum déficit neurológico ou visual. Foi submetido à cirurgia para remoção das fitas de silicone anteriormente posicionadas, confecção de enxertos em fita de técido fibroconectivo da fáscia lata do membro inferior direito, miectomia do musculo elevador da pálpebra ptosada, fixação dos enxertos da fáscia lata na borda superior do tarso com tração e fixação ao musculo frontal ipsilateral. Evoluiu com movimentos sincrônicos das pálpebras bilateralmente, e sem recidiva do ptose até o presente momento.
Palavras-chave: Marcus-Gunn; Ptose palpebral; Fixação frontal.
The Marcus Gunn syndrome is a synkinesia that progresses into congenital palpebral ptosis associated with jaw movement. It was first described by Marcus Gunn in 1883. The Marcus Gunn syndrome (or jaw-winking phenomenon) is characterized by palpebral ptosis of varying severity, usually unilateral, which decreases or even progresses into eyelid retraction in response to jaw movement1-3. Generally, it sporadically occurs, although cases of irregular autosomal dominant inheritance have been described5. The syndrome is responsible for 2% to 13% of congenital ptosis. Recent studies reported a prevalence rate of 5%4-5. No clinical treatment exists; however, some patients may learn to control synkinesia and show improvement of the condition1. Surgical treatment is reserved for pronounced cases of ptosis or moderate ptosis associated with amblyopia or vertical strabismus1. Only few articles on this subject are available in the literature. Thus, the authors report a severe case of Marcus Gunn syndrome that relapsed after the fourth surgery, along with a brief literature review.
CASE REPORT
A.L.C.M, a 19-year-old man from Rio de Janeiro, presented at the Plastic Surgery Service of the Hospital Federal do Andaraí and reported a history of ptosis in the right eyelid since birth, with improvement of the ptosis on opening the mouth or contralaterally closing the eye. He reported having undergone four previous surgical corrections of the ptosis in other services. The last procedure comprised placement of silicone suspender bands (Silastic), with a relapse occurring after 2 years. On examination, the patient showed isocoric pupils, which were reactive to light, and severe right eyelid ptosis, which improved on opening the mouth, when he lateralized the eye to the ipsilateral side, and with the contralateral eye closure (Figure 1).
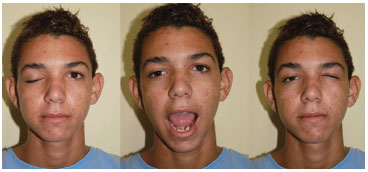
Figure 1. The Marcus Gunn syndrome. Patient at rest (left). Eyelid opening on opening the mouth (center). Eyelid opening on contralateral eye closure (right).
The patient was referred to the neurology service. No other neurological disorder was identified. Therefore, Marcus Gunn syndrome was definitively diagnosed.
After explaining the procedure to the patient, he signed the consent form and underwent the procedure. The surgery was performed in a surgical center, under local anesthesia and without sedation, in order to determine the degree of ptosis correction required through voluntary movements of the patient. After infiltration with 1% lidocaine solution with adrenaline diluted at 1:200,000, an incision was performed in the upper eyelid sulcus, at the upper edge of the tarsus, approximately 10 mm from the ciliary edge. Dissection was performed below the orbicular muscle and septum, until identification of the silicone suspender band, which was found intact and fixated in the tarsal plate, and the aponeurosis of the eyelid levator muscle. We removed the suspender band and the myotomy of the tarsal plate levator muscle (Figure 2).
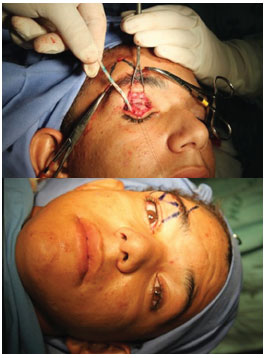
Figure 2. Removal of the silicone suspender band and preparation of the fascia lata strips.
Under local anesthesia, a fragment of the fascia lata of approximately 5cm2 was removed in the lateral side of the right thigh. The fragment was cut into various strips and used for autografting. One end of the fascia lata strips were fixated in the upper edge of the tarsus, in the lateral, median, and medial aspects, and the other end of the strips were placed in the cranial direction, through a tunnel in the subcutaneous plane, converging to form two triangles until reaching the more mobile part of the frontal muscle. The patient was asked to open the eye, and the opening of the healthy eyelid was used as reference for the correction. We determined the fixation points and the length of the fascia lata strips, with a small degree of overcorrection (Figure 3).

Figure 3. Placement and fixation of the fascia lata suspender strips, with a slight overcorrection.
After ensuring hemostasis, we performed simple skin suturing of the orifices by using monofilament nylon 5-0 and continuous suturing of the eyelid incision by using monofilament nylon 6-0. The patient recovered without relapse until the time of this writing (Figure 4).

Figure 4. Result after 3 postoperative weeks.
DISCUSSION
The upper eyelid levator muscle, which is innervated by the third cranial and oculomotor nerves, is responsible for eyelid opening, with the frontalis and Müller muscles supporting its function. The orbicularis muscle, which is innervated by the facial nerve, is responsible for eye closure2.
Eyelid ptosis is defined when the upper eyelid covers more than 2mm of the corneal limbus when the patient is in orthostasis and primary gaze position. Eyelid ptosis may be classified as follows: mild, when the upper eyelid margin covers 2 to 4 mm of the corneal limbus; moderate, when it covers 4 to 6 mm of the corneal limbus; and severe, when it covers more than 6mm of the corneal limbus. By assessing levator muscle function according to the aforementioned classification and determining whether the ptosis is congenital or acquired, the appropriate treatment can be determined.
Congenital ptosis occurs due to impairment of striated fibers of the eyelid levator muscle. Acquired ptosis can be classified as mechanical, aponeurotic, or neurogenic. Eyelid ptosis of mechanical origin results from mechanisms that increase the weight of the upper eyelid, such as tumors, orbitopalpebral neurofibromatosis, and scars. Myogenic ptosis occurs due to dystrophic structural failure or myoneural plaque dysfunction in the striated fibers of the eyelid levator muscle, such as miastenia gravis and family chronic progressive ophthalmoplegia (oculopharyngeal syndrome). Aponeurotic ptosis includes senile ptosis, ptosis associated with eye surgery, blepharochalasis, Graves' disease, and pregnancy. They are caused by dehiscence, elongation, or release of the eyelid levator muscle. Finally, neurogenic ptosis due to third cranial nerve lesion alters eyelid function. The most common type of neurogenic ptosis is observed in the Horner syndrome, in third cranial nerve paralysis (ophthalmoplegia), and in synkinetic ptosis3,4.
In the Marcus Gunn syndrome, the elevation, or even retraction, of the ptotic eyelid is triggered by chewing, suction, lateral jaw movement, smiling, sternocleidomastoid contraction, tongue protrusion, Valsalva maneuver, and even just by inhalation. The present case was also associated to the spontaneous closure of the contralateral eyelid.
The etiopathological mechanism of the Marcus Gunn syndrome remains unclear and has been considered as the result of an anomalous connection between the nerves of the external pterygoid muscle and the eyelid levator muscle. The eyelid levator muscle is innervated by the motor ramifications of the trigeminal nerve and by the oculomotor nerve4. Recently, a case was reported of a child with Marcus Gunn syndrome associated with synkinesia of the trigeminal and abducens extraocular muscles6,7. Some authors described cases where oculomotor nerve lesion occurred with subsequent innervations of the eyelid through ramification of the fifth cranial nerve, including rare cases of acquired forms of the syndrome. The detection of the syndrome in children, even in infants, by relatives or pediatricians should be reason for an immediate ophthalmologic examination. Examination at an early stage is aimed at preventing amblyopia, anisometry, strabismus, eyelid levator muscles paralysis, superior rectus muscle paralysis, congenital nystagmus, and congenital fibrosis syndrome.
Some authors stated that the Marcus Gunn syndrome improves with age; however, some claim that what actually happens is that patients learn the mechanism of synkinesia and apply methods to avoid or control it8. Other changes associated with synkinesia are the inverse Marcus Gunn syndrome and Marin-Amat syndrome. Both conditions progress with ptosis, which becomes more evident with jaw movement9,10. The difference between them is that the former is a congenital condition, in which the eyelid levator muscle is impaired, whereas the latter is acquired, occurring after facial paralysis. In addition, in the latter, the orbicular and levator muscle contractions are not affected9,10.
For the Marcus Gunn syndrome, surgery is performed in order to correct moderate eyelid ptosis associated to vertical strabismus or amblyopia, or severe ptosis. In severe ptosis, when levator muscle dysfunction is present, the ptosis is improved with myectomy of the elevator muscle and fixation of the tarsal plate influenced by the frontalis muscle movement1. However, if the patient shows good function of the levator muscle, even in severe cases of ptosis, only shortening of the aponeurosis procedure is required2. Khwarg et al.11 reported a series of 24 patients (unilateral in 21 and bilateral in 3) who underwent surgery between 1978 and 1997, for a section of the levator muscle of the upper eyelid, unilaterally or bilaterally, followed by frontalis muscle suspension. Of the eyelids, 37% were completely resolved and 48.2% (13 eyelids) showed elevation of 1 mm or less during jaw movements, without any perceptible functional or aesthetic impairment. In addition, another surgical technique used to eliminate eyelid elevation related to chewing is the mandibular nerve section, with the removal of the site in the external pterygoid muscle associated to the section of the molar root of the trigeminal nerve12. According to Torres et al, conventional ophthalmological examination may underestimate the severity of ptosis and result in surgical undercorrection. Thus, better results were obtained when the preoperative evaluation of ptosis severity was performed with the jaw immobilization technique and temporary ipsilateral eye closure1.
In the present case, the patient showed pronounced ptosis and a weak levator muscle function. Therefore, we chose to disconnect the levator muscle to avoid synkinesia and static fixation of the frontalis muscle, and used an autologous tissue graft from fascia lata strips to prevent another relapse.
REFERENCES
1. Torres MR, Calixto NJ, Oliveira LR, Steiner SA, Iscold AM. Fenômeno de Marcus Gunn: diagnóstico diferencial das ptoses palpebrais na criança. J Pediatr. 2004;80(3):249-52.
2. Moribe I, Cruz AA, Habib JT. Anomalias palpebrais. In: Rodrigues MLV, editor. Oftalmologia Clínica. Rio de Janeiro: Cultura Médica; 1992. p. 306-07.
3. Disorders of the eyelids. In: Kanski JJ, editor. Clinical Ophthalmology. 3rd ed. Butterworth-Heinemann Medical; 1997. p. 1-26.
4. Chaves PS, Hoyt, WF. Neuro-oftalmologia. In: Vanghan DG, Asbury T, Riordan P, editor. Oftalmologia Geral. 4a ed. São Paulo: Atheneu; 1998. p. 84.
5. Pratt SP, Beyer CK, Johnson CC. The Marcus Gunn phenomenon. Ophthalmol. 1984;91:27-30.
6. Freedman HL, Kushner BJ. Congenital ocular aberrant innervation:. new concepts. J Pediatr Ophtalmol Strabismus. 1997;34(1):10-6.
7. Kodsi S. Marcus Gunn jaw winking with trigemino-abducens synkinesis. AAPOS. 2000;4(5):316-7.
8. Odehnal M, Malec J. New views on aberrant innervation of oculomotor muscles. Cesk Slov Oftalmol. 2002;58(5):307-14.
9. Wong JF, Theriault JF, Bouzouaya C, Codere F. Marcus Gunn jaw-winking phenomenon: a new supplemental test in the preoperative evaluation. Ophthal Plast Reconstr Surg. 2001;17(6):412-8.
10. Rana PS. The Marin-Amat syndrome: an unusual facial synkinesia. J Neurosurg Psychiatry. 1985;48:939-41.
11. Khawrg SI, et al. Management of moderate-to-severe Marcus Gunn jaw-winking ptosis, Ophthalmol. 1999;106(6):1191-6.
12. Ramos SM, Soardi D, Carli E. Marcus Gunn Sindrome; Rev. Cient. AMECS. 2001;10(1):80-82.
1. Associate member of the Brazilian Society of Plastic Surgery (SBCP); Staff of the Plastic Surgery Service at the Hospital Servidor of the State of Pernambuco; Preceptor of the Plastic Surgery Service at the Hospital Alcides Carneiro (UFCG); Professor of Surgery at the Faculty of Medical Sciences of Campina Grande
2. Associate member of the Brazilian Society of Plastic Surgery
3. Full member of the Brazilian Society of Plastic Surgery; Head of the Reconstructive Microsurgery Service of the Hospital Federal dos Servidores of the State of Rio de Janeiro; Associate professor at the Ivo Pitanguy Institute
Institution: Plastic Surgery Service of Hospital Federal do Andaraí.
Corresponding author:
José Daniel de Albuquerque Lins Rolim
Rua Pedro II, 407 - Sala 301 - Bairro da Prata
Campina Grande, PB, Brazil Zip code: 58400-565
E-mail: drdanielrolim@gmail.com
Article submitted: August 8, 2011.
Article accepted: December 1, 2011.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter