

Original Article - Year 2015 - Volume 30 -
Use of Bernard-Webster flap for lower lip reconstruction after excision of squamous cell carcinoma: analysis of functional results
Retalho de Bernard-Webster para reconstrução do lábio inferior após exérese de carcinoma espinocelular: uma análise dos resultados funcionais
ABSTRACT
INTRODUCTION Defects in the lower lips after the excision of squamous cell carcinoma (SCC) are usually repaired using several surgical techniques. However, the functional reconstruction of full-thickness defects in the lower lip remains a challenge. Therefore, the objectives of this study were to describe surgical strategies for the reconstruction of full-thickness defects of the lower lip after surgical excision of the SCC and evaluate the functional results.
METHODS: This was a retrospective study of all patients with full-thickness defects in the lower lip after excisions of SCC that were greater than one third of the lip that were repaired using the Bernard-Webster flap between 2011 and 2014. The functional results (sphincteric, motor and sensory function) were evaluated according to previously used criteria.
RESULTS: Six lip defects were reconstructed without complications using Bernard-Webster flaps. During the postoperative period, the patients reported liquid incontinence (16.67%), intermittent salivary incontinence (16.67%), and difficulty fully opening the mouth (33.33%). The tests revealed sensory deficits in the labiomental areas (100%) and lower lip (33.33%). There was full recovery of all functional changes an average of 3 months after surgery. The observed late functional results were considered satisfactory.
CONCLUSIONS: The Bernard-Webster flap was an excellent alternative to repairing the defects that affect more than one third of the lower lip since it allowed the use of similar local tissues, a single surgery could be performed, and the result was functionally efficient.
Keywords: Lower lip; Squamous cell carcinoma; Bernard-Webster flap.
RESUMO
INTRODUÇÃO Defeitos dos lábios inferiores após exéreses de carcinoma espinocelular (CEC) vêm sendo reparados com inúmeras técnicas cirúrgicas. No entanto, a reconstrução funcional de defeitos de espessura total do lábio inferior continua a ser um desafio. O objetivo deste estudo, portanto, foi descrever as estratégias cirúrgicas para a reconstrução de defeitos de espessura total do lábio inferior, subsequentes a exéreses cirúrgicas de CEC, bem como avaliar resultados funcionais.
MÉTODO: Trata-se de um estudo retrospectivo de todos os pacientes com defeitos de espessura total de lábio inferior após exérese de CEC maiores que um terço do lábio, reconstruídos com retalhos de Bernard-Webster, no período de 2011 a 2014. Os resultados funcionais (funções esfincteriana, motora e sensorial) foram avaliados de acordo com critérios previamente utilizados.
RESULTADOS: Seis defeitos labiais foram reconstruídos com retalhos de Bernard-Webster, sem complicações. No período pós-operatório, os pacientes relataram incontinência para líquidos (16,67%), incontinência salivar intermitente (16,67%) e dificuldade para abrir a boca completamente (33,33%). Os testes revelaram déficits sensoriais nas regiões mentoniana (100%) e de lábio inferior (33,33%). Houve recuperação completa de todas as alterações funcionais, em média, três meses após as intervenções cirúrgicas. Os resultados funcionais tardios foram considerados satisfatórios.
CCONCLUSÕES: O retalho de Bernard-Webster mostrou-se uma excelente alternativa para reparar defeitos que comprometem mais de um terço do lábio inferior, pois permitiu a utilização de tecidos vizinhos semelhantes, pôde ser realizado em tempo único e foi funcionalmente eficaz.
Palavras-chave: Lábio inferior; Carcinoma espinocelular; Retalho de Bernard-Webster.
The lips are the dynamic center of the lower third of the face and play an essential role in an individual's appearance, self-esteem, harmony, and facial expressions as well as in eating, drinking, swallowing, and speaking (phonation and pronunciation)1,2. Therefore, surgeons are challenged when facing congenital and acquired lip deformities (oncological excisions, traumatic avulsion, burns, or infections)1, with neoplasia excision being the main cause of lip defects3.
Squamous cell carcinoma (SCC) is the most common malignant neoplasia (95%) of the lips, and the lower lip is significantly more affected than the upper lip (90% and 10%, respectively)4. The first-line treatment for these tumors (excision with clear neoplasia margins) results in tissue deficits with variable thickness and extension4. Lesions that reach large dimensions may become infiltrative and destructive in a way that, to enable surgical excision, may require amputation of the important functional and/or aesthetical structures, resulting in complex defects that require adequate postoperative planning and meticulous selection of the surgical technique to reconstruct both an aesthetically pleasing lower lip (replacing the external skin adequately to maintain the aesthetical balance of the mucocutaneous junction and the lip aesthetic units) and a functional lower lip (preserving the intraoral lining, avoiding microstomy, and maintaining oral continence)1,4,5. Skin sensitivity must be preserved or re-established to provide a proprioceptive mechanism to movement, speech, and salivary continence1.
In this context, approximately 200 surgical techniques have been described to reach these objectives (aesthetical and functional lip reconstruction)6. All of the reconstruction processes of lower lip defects following oncological excision should be adapted to the individual2; as such, the specific surgical approach must be selected according to lip defect extension, location, and thickness2,5. For these reasons, lip defects have been divided into three main groups: defect only at the cutaneous part of the lip; defect only in the lip vermilion; and full-thickness defect, which varies according to the defect area (less than one third, between one third and two thirds, and near-total or total)2,3.
Full-thickness defects that compromise one third of the length of the lower lip can generally be repaired5. On the other hand, longer full-thickness defects require more laborious reconstruction procedures such as those described by Dieffenbach7, Burow8, Bernard9, Abbe10, Karapandzik11, Webster12, and others13. In 1845, Dieffenbach7 was the first to suggest reconstruction of the lower lip defects using the malar flap with medial advancement. In 1853, Bernard9 described a technique using a full-thickness triangular incision (Burow triangles) in the nasolabial sulcus to enable medial advancement of the malar flaps. This approach was modified by Webster12 in 1960: a triangular incision was then used for partial-thickness defects, while mucosal flaps and the guidelines by Schuchardt14 were applied in the reconstruction of the lip vermilion and advancement of the paranasal skin region, respectively. Since then, the Bernard-Webster flap12 has been used globally to reconstruct lower lip defects. There are various technical modifications15-19, preservation of the innervated muscle fibers of the mouth orbicular muscle through careful tissue dissection and manipulation in particular, without full muscle transection at the commissure level17.
In this context, the decision to perform reconstruction has been based on different algorithms described in the Brazilian20,21 and international2,6,22 literature. However, functional reconstruction of full-thickness defects of the lower lip remains a challenge since nearly none of the surgical techniques meet all of the requirements of ideal lip reconstruction6.
OBJECTIVE
The objective of this study was to describe the surgical strategies used for the reconstruction of full-thickness defects of the lower lip after surgical SCC excision through an analysis of the functional results.
METHOD
This is a retrospective observational study of all patients with full-thickness defects affecting a third of the length of the lower lip, following surgical excision of the SCC, reconstructed using Bernard-Webster flaps in the Institute of Craniofacial Plastic Surgery of the SOBRAPAR Hospital, from January 2011 to April 2014. This study was approved by the Human Research Ethics Committee of the SOBRAPAR Hospital, and is in agreement with the Declaration of Helsinki of 1975, which was improved in 1983.
Only patients presenting with full-thickness defects (excision of skin, muscle, and subjacent mucosa) affecting more than one third of the length of the lower lip subjected to surgical treatment by the same group of plastic surgeons who shared the same background training and philosophy and followed the patients postoperatively were included. We analyzed the time, clinical history, and anatomical locations (mostly involvement of the medial or lateral lip) of the lower lip lesions, the time used to monitor the patients after surgery, the emergence of new lesions in the perioral region, and locoregional or distant recurrences. In addition, aspects related to the surgical procedures - including excision, defects (classified according to the quantification method described by Jeng et al.23), reconstruction, functional results, and complications - were also evaluated and characterized.
Surgical strategies
All of the procedures conducted during the pre-, intra-, and postoperative periods were based on previous established recommendations1-5,22. According to the therapeutic algorithm adopted by our institution since 2011 (Figure 1), the full-thickness defects resulting from excision of SCC that compromises more than one third of the length of the lower lip have been reconstructed using Bernard-Webster flaps, preferably regardless of the defect location (mainly lateral or median) or involvement of the mouth commissure. Furthermore, the decision of which surgical procedure to use was performed individually based on previous confirmation data of SCC in the lower lip as well as patient and surgeon preference.
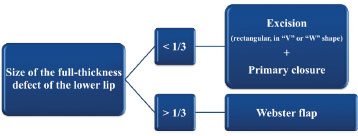
Figure 1. Simplified therapeutic algorithm used to assess the reconstruction of full-thickness defects of the lower lip after the surgical excision of squamous cell carcinoma.
Surgical technique
All surgical procedures were performed under local anesthesia. After marking of the flap, the labiomental and infraorbital nerves and all of the areas subjected to incision were infiltrated with 2% lidocaine luminescent solution, 0.5% bupivacaine, 0.9% physiological saline (1:1:2), and adrenaline (1:100,000). The surgery started with excision of the lip lesion in the full plane with safety margins of 1 cm in a quadrilateral shape with the lower border at the labiomental sulcus (Figures 2-4). Subsequently, the incisions were performed in the marked area to prepare the flaps with respect to the aesthetic units of the face (e.g., curved incisions along the nasogenian and labiomental sulcus). In the intraoral mucosa, the upper incisions were performed approximately 1 cm above the lip commissure to the superior bilateral molar region below the orifices of the parotid ducts. Thereafter, the mouth mucosal and submucosal tissues were separated from the remaining malar structures approximately 1 cm below the upper incisions to produce flaps from the mouth mucosa (used in reconstruction of the lip vermilion). The lower incisions were made near the alveolobuccal sulcus and performed deeper to the periosteum below the sulcus to allow the advancement of the lower borders of the flaps. Subsequently, the skin and fat tissue of the Burow compensation triangles were dried in the upper (nasolabial sulcus) and lower (labiomental sulcus) parts to preserve the underlying muscles (Figures 3 and 4). The length of each horizontal component (base) of the Burow triangles of the nasolabial sulcus should be from one half to one third of the horizontal lip defect. When performing the incisions and tissue manipulation, we were careful to preserve to the maximum vascular-nervous system (identification and isolation of the labiomental nerves) and muscle system (we did not transected the oral orbicular muscle at the lip commissure level) of the region (Figures 3 and 4). Finally, the flaps were advanced medially and sutured by planes, and we were careful to adequately place the skin-mucosal line (Figure 5): the mucosal plane and muscular girdle were approximated and aligned using simple separated polyglactin 4-0 stitches; the moist and dry mucosal tissues were approximated and aligned with polyglactin 4-0 and nylon 5-0 stitches, respectively; the procedure was then finished with inverted subdermal stitches of polyglactin 4-0 and simple separated nylon 5-0 or 6-0 stitches. This can be approached bilaterally or unilaterally (with defects predominantly at the median or lateral levels, respectively). Additional technical details have been reported elsewhere1,3,9,12,15-19,22.
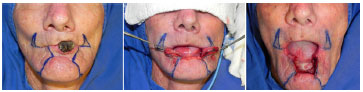
Figure 2. Patient with squamous cell carcinoma in the lower lip with marking of the bilateral Bernard-Webster flap (left). Full-thickness defect of the lip resulting from quadrangular excision with the lower border in the labiomental sulcus (center and right).

Figure 3. Patient with squamous cell carcinoma in the lower lip with marking of the bilateral Bernard-Webster flap (above, left). Full-thickness defect of the lip resulting from quadrangular excision with the lower border in the labiomental sulcus and incisions and resections of the skin and fat tissue of the upper (nasolabial sulcus) and lower (labiomental sulcus) portions of the Burow compensation triangle to preserve the underlying muscles (above, right). Elevation of the lower flaps (below) revealing isolation of the right (left) and left (right) labiomental nerves.
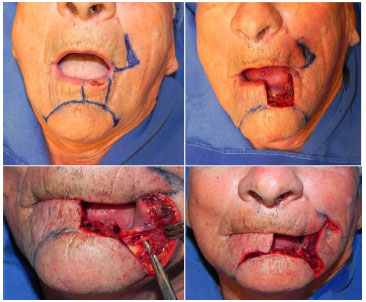
Figure 4. Patient with squamous cell carcinoma in the lower lip with marking of the unilateral Bernard-Webster flap on the left side (above, left). Full-thickness lip defect resulting from quadrangular excision with the lower border in the labiomental sulcus (above, right). Elevation of the lower flap revealing isolation of the left labiomental nerve (below, left). Incision and resection of the skin and fat tissue of the upper (left nasolabial sulcus) and lower (labiomental sulcus) portions of the Burow compensation triangle to preserve the underlying muscles (below, right).
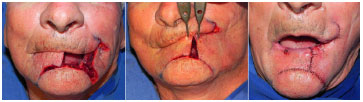
Figure 5. Patient with a full-thickness lip defect resulting from quadrangular excision of squamous cell carcinoma with the lower border in the labiomental sulcus and the incisions and resections of skin and fat tissue of the upper (left nasolabial sulcus) and lower (labiomental sulcus) portions of the Burow compensation triangle to preserve the underlying muscles (below, right). Elevation and advancement of the flaps (center). Final view of the surgical procedure revealing the reconstructed lower lip, location of the skin-mucosal line, and mouth opening (right).
Postoperative care and follow-up
All patients were discharged the first day after surgery. Postoperative care was performed similarly for all patients, and each was given directions about daily surgical wound care, revisiting the clinic between postsurgical days 5 and 7, eating liquid/paste meals for 2 weeks, and not conducting any open-mouthed activities for 4 weeks. In addition, since SCC carries a significant risk of recurrence and/or metastasis (lesions > 2 cm and periorificial lesions24), all patients were carefully evaluated before and after the surgical procedures according to previously established criteria1-5,24.
Postoperative functional results
Functional results25-27 (adequate mouth opening and continence for hygiene, meals, use of dental prosthesis, lip closure, phonation, and sensitivity) were assessed during the clinical visits of the postoperative follow-up period (postoperative days 7, 14, 21, 30, and 60, then every 3 months). Oral continence (incontinence, loss of saliva while resting, loss of saliva when ingesting liquids, or total continence), and lip mobility (symmetric or asymmetric in the observation of mouth opening and closing movements) were stratified according to a previous study26. Speaking was assessed during conversations in addition to interviewing patients about postoperative difficulties with oral communication27. The objective sensory evaluation of the malar regions, nasolabial sulcus, upper and lower lips, and labiomental region was performed with the aid of the Semmes-Weinstein test of tactile perception thresholds to pressure according to previously described standards28,29. Each side of the face was tested separately and the Semmes-Weinstein 3.22 monofilament was used as the upper limit of normality for the detection threshold of the assessed anatomical locations28,29. All patients were assessed during the pre- and postoperative periods. A sensory deficit was defined as an abnormal test result in the postoperative period, while a permanent sensory deficit was defined as an abnormal clinical test occurring at 12 or more months postoperative28,29. All patients were questioned about their satisfaction (pleased, partially pleased, or unsatisfied) of the late functional results27.
All data were recorded in the Excel program for Windows. For the descriptive analysis, the metric variables are summarized as averages and standard deviations, while the categorical variables are expressed as percentages.
RESULTS
Six male patients with SCC of the lower lip were evaluated. The average age at the time of the reconstruction surgeries was 69.67 ± 14.73 years (range, 44-88 years). All patients had a previous history of continuous occupational sun exposure. The individuals were all class I-III on the Fitzpatrick classification scale. Clinical exams of the skin for concomitant lesions and palpation of cervical lymph nodes did not reveal any changes for any patient. All of the lower lip lesions had an evolution > 3 months (range, 3 months to 5 years) and measured 2-5 cm in their highest diameter. Five lesions (83.33%) were predominantly located in the median portion of the lower lip, while one lesion (16.67%) was located in the lateral portion; none of the lesions compromised the lip commissure.
All patients underwent incisional biopsies (SCC was present in all samples) at different services and were then directed to our institution. The six lesions (100%) were excised with safe surgical margins. The defects created by the excision affected more than one third of the length of the lower lips and, according to the quantification method by Jeng et al.23, affected 63.33 ± 17.51% (range, 40-90%) of the lower lips. The six lip defects (100%) were reconstructed in a single surgical procedure using the Bernard-Webster flaps, with five (83.33%) being bilateral and one (16.67%) being unilateral on the left side. We did not observe a direct lesion of the mouth orbicular muscle or at the commissure or labiomental nerve level during the surgical procedures. There was no occurrence of hematoma, necrosis, infection, or orocutaneous fistula during the postoperative follow-up period. There was one case of partial dehiscence (16.67%) that was resolved with a new suture. No secondary surgical procedures were required.
The anatomopathological exam findings of the six surgical samples (100%) were compatible with SCC although moderately differentiated with surgical margins (laterally and deep) clear of neoplasia and lacking vascular or perineural invasion. All patients were classified as T2N0M0 according to the 7TH American Joint Committee on Cancer Staging Manual. There was no recurrence or new skin lesions suggestive of non-melanoma skin cancer in the perioral region during the average postoperative follow-up of 20.67 ± 9.29 months (range, 12-31 months).
Postoperative functionality
None of the patients showed deficits in the sensory tests conducted in the postoperative period. During this period, the patients did not report hypoesthesia or anesthesia in the perioral region. However, the six patients (100%) showed transitory bilateral sensory deficits to tactile pressure in the labiomental region; one patient (16.67%) showed a unilateral deficit on the left side after unilateral reconstruction (defect affected only the left half of the lower lip). Two patients (33.33%) also showed sensory deficits in the region of the lower lip, one (16.67%) bilaterally and the other (16.67%) unilaterally on the left side (after unilateral reconstruction). All patients showed normal results on sensitivity tests after an average postoperative period of 45.75 ± 30.73 days (range, 21-90 days). No permanent sensory deficit was observed during the analysis period.
One patient (16.67%) reported incontinence for liquid meals, another (16.67%) reported intermittent salivary loss, and two (33.33%) showed difficulty completely opening the mouth; total recovery of these functional changes occurred in an average of 3 months. All patients were able to restart their usual diet 30 days after the surgical interventions. None of the patients reported difficulty speaking, conducting their daily personal hygiene tasks, and/or using dental prostheses. Facial movements were normal in all assessments. The reconstructed lower lips had satisfactory volume and definition. The mouth opening circumference was maintained (none of the patients presented with microstomy) without distortion of the facial characteristics on the assessments performed in the late postoperative period.
The six patients (100%) were pleased with their late functional results. According to previous published classifications25,26, the functional results (100% lip contact, continence to liquids, adequate mouth opening for hygiene tasks, eating meals, use of dental prostheses, phonation, and normal facial movements) were considered satisfactory in the late postoperative period (Figures 6-10).
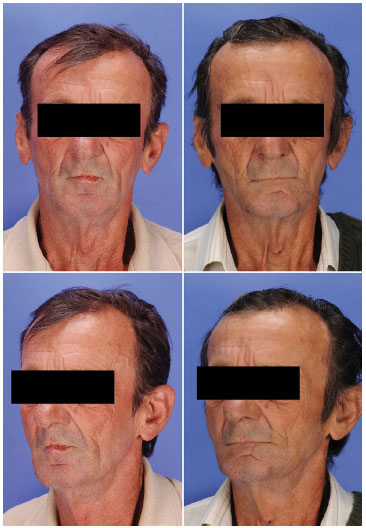
Figure 6. Frontal and semilateral views of a patient with squamous cell carcinoma of the lower lip before (left) and 18 months after (right) lip reconstruction using a bilateral Bernard-Webster flap.
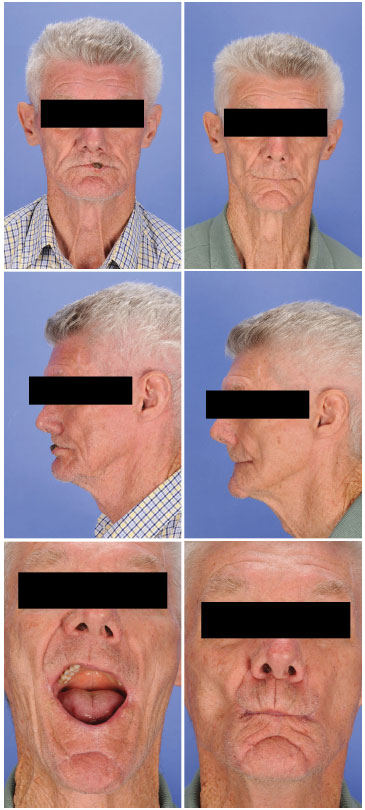
Figure 7. Frontal and lateral views of a patient with squamous cell carcinoma of the lower lip before (above and center, left) and 16 months after (above and center, right) lip reconstruction with the bilateral Bernard-Webster flap. Mouth function (mouth opening and kiss movements) 16 months after the surgical intervention (below).
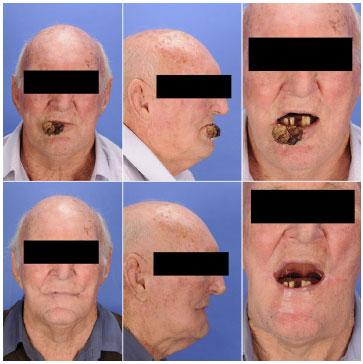
Figure 8. Frontal and lateral views as well as mouth opening of a patient with squamous cell carcinoma of the lower lip before (above) and 4 months after (below) lip reconstruction using a bilateral Bernard-Webster flap.
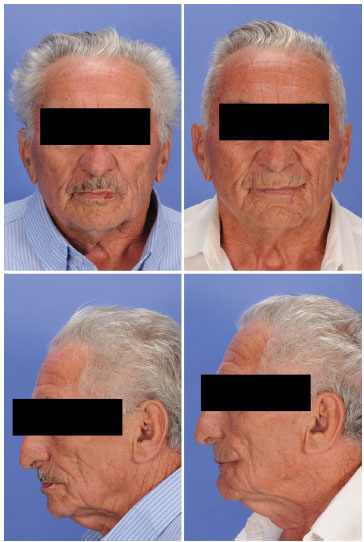
Figure 9. Frontal and lateral views of a patient with squamous cell carcinoma of the lower lip before (left) and 6 months after (right) lip reconstruction using a unilateral Bernard-Webster flap.
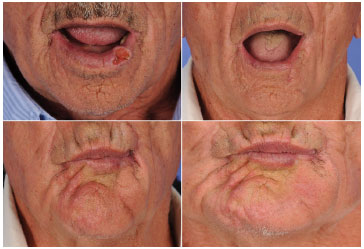
Figure 10. Mouth opening of a patient (above) with squamous cell carcinoma of the lower lip before (left) and 6 months after (right) lip reconstruction using a unilateral Bernard-Webster flap. Kiss movements (below) at 1 (left) and 2 months (right) after the surgical procedure
DISCUSSION
Radical excision surgery with clear microscopic margins of neoplasia should be the treatment of choice for SCC of the lower lip since this therapeutic modality is associated with satisfactory disease-free survival3,24. Such an approach invariably results in lip defects. The small full-thickness defects (less than one third of the length of the lower lip) can be excised in "W" or "V" shapes and the three layers of the lip repaired primarily without the need for local flaps1,3,5. On the other hand, the reconstruction of more extensive full-thickness defects (more than one third of the length of the lower lip), such as those reported in the present study, represents a more complex challenge3.
Among the various surgical techniques described to reconstruct defects in more than one third of the lower lip length, we can highlight the Abbe, Estlander, Gillies, Karapandzic, and Bernard-Webster flaps2,3,9-13. Although excellent results have been described with such techniques both in Brazil14,21,30-33 and internationally5,6,26,27, the selection of a specific procedure should consider the advantages and disadvantages of each approach6. The main disadvantages of the Abbe flap are the potential risk of lip vermilion misalignment, lip adhesion, and microstomy in high defect cases besides requiring two surgeries2,6. The Estlander flap is conducted in a single surgical procedure3; however, the patients frequently require commissuroplasty2. In addition, microstomy, misalignment of the lip vermilion, and round commissures are disadvantages associated with use of the bilateral Gillies flap2.
Therefore, the Karapandzic and Bernard-Webster flaps are the two most commonly used options for the reconstruction of great defects of the lower lip with the advantage of requiring only a single surgery6. Nevertheless, since the Karapandzic flap has the potential risks of microstomy as well as misalignment of the mouth commissure2, the Bernard-Webster flap is the first choice treatment in our service for the reconstruction of defects greater than one third of the length of the lower lip, similarly to what has been adopted in other institutions6.
We prefer the Bernard-Webster flap since it can be applied for extensive full-thickness defects (affecting more than one third of the lower lip)1-3, including defects with a limited residual lip since it does not depend on the reminiscent lip tissue for the reconstruction of a new lower lip as well as in defects in which only the skin is excised3 (not applied to our algorithm). Furthermore, the malar advancement flap considerably reduces the risk of microstomy1,2,6,19; as such, it is considered ideal for elders due to their skin flaccidity and their common use of dental prostheses26.
The potential disadvantages of the Bernard-Webster flap include the incision notch in the region of the lower lip and erasure of the alveolobuccal sulcus1. In addition, according to the surgical procedures described in the seminal manuscript by Webster12, the orbicular and buccinator muscles should be incised laterally to the mouth commissure; thus, few muscle fibers remain innervated. Therefore, the postoperative period of the patients who undergo reconstruction using this approach may be accompanied by functional deficits such as lip incontinence to liquids26. Since mouth continence depends on contraction of the mouth orbicular muscle as well as the function of the other muscles inserted in the modiolus, in 2002, Wechselberger et al.17 proposed technical modifications to preserve the muscles associated with the modiolus (the oral orbicular muscle in particular) for the flap described by Webster12 suggesting that the intervention performed in the lower lip would be completely preserved.
Under the scope of the reconstruction of full-thickness defects of the lower lip, the restoration of lip function (complete continence, maximum mouth opening, sensitivity) should be considered of the utmost importance so that the patients can maintain their daily activities without discomfort or incovenience6. Thus, we outlined the present study to carefully assess the functional results with the final aim of describing our simplified therapeutic protocol (Figure 1) in which defects greater than one third of the length of the lower lip have been reconstructed with the Bernard-Webster flap12 modified by others15-19, Wechselberger et al.17 in particular. For this purpose, we monitored patients continuously (for an average of 20 months) and analyzed the functionality of the surgical procedures according to the methods applied in similar studies25-27. In the literature, the types of techniques applied in the reconstruction of defects of the lower lips and the methodologies used (if any were adopted) to assess the surgical results vary widely5,6,18,25-27. Therefore, there are limitations in regard to the comparative discussion of the results obtained in different analyses. For this reason, we will only address the main findings of this study since a more detailed comparative analysis would be merely speculation.
In our study, four patients (66.67%) reported complaints related to lip function (salivary incontinence, liquid incontinence, and difficulty completely opening the mouth); an average of 3 months after the reconstruction procedures, no further functional alterations were detected or reported, a finding that is in agreement with previous studies22 about the use of different local flaps for the reconstruction of lower lip defects.
The literature27,34 has demonstrated no differences in postoperative perioral sensitivity in the comparison of patients who underwent reconstruction of lower lip defects of the lower lips with innervated flaps and patients subjected to interventions with non-innervated flaps. However, such studies27,34 did not evaluate the Bernard-Webster flap. Here we observed transitory sensory deficits in the perioral region (mainly in the labiomental region) in all patients. The relevant literature reported that sensitivity returns slowly in patients with reconstructed lower lips27. Such deficits were resolved an average of 40 days after the surgical interventions; therefore, no permanent sensory deficits were observed. Therefore, we believe that with adequate visualization and preservation of the local vascular nervous and muscular systems during tissue mobilization, the Bernard-Webster flap12 utilized with the modifications by Wechselberger et al.17 is safe at the sensorial level as demonstrated by other studies6,17.
It is also important to underline that, in addition to local flaps, the microsurgical free flap has been used in the total reconstruction of the lower lips3,23. Nevertheless, the free flap still has one limitation with regard to the functional and aesthetic features of the mouth since the transferred tissue is rather different from the lip tissue6,19. Similarly to Hamahata et al.19, our group believes that this reconstruction approach (free flaps) should be a complementary alternative, especially for total or near-total defects (>80% of the lower lip affected23) in which local flaps (the first option) cannot be used.
Similarly to Seo et al.6, our therapeutic algorithm is a simplified adaptation of the reconstructive approaches adopted in different services2,20-22. This simplification facilitates the approach of full-thickness defects greater than one third of the length of the lower lip since the Bernard-Webster flap is a reproducible surgical procedure as long as the technical procedures are rigorously followed. Therefore, we believe that since a large portion of the full-thickness defects of the lower lips can be reconstructed using this flap and the functional results were considered satisfactory in ours and other studies6,17, all surgeons correcting such defects should master the technical particularities to obtain the ideal ontological results without affecting function. However, although malar advancement flaps may be theoretically applied in the reconstruction of full-thickness defects of the lower lip that affect the mouth commissure35, we must be careful when extrapolating our results since none of the patients included in this study had involvement of the mouth commissure. Furthermore, although our functional results are satisfactory, we must admit that the absence of comparisons with other techniques is a limitation of the present study.
CONCLUSION
This study demonstrated that the Bernard-Webster flap is an excellent alternative to the reconstruction of full-thickness defects that are greater than one third of the length of the lower lip after surgical excision of SCC since it is functionally effective and can be conducted in a single surgery using similar local tissues.
REFERENCES
1. Baumann D, Robb G. Lip reconstruction. Semin Plast Surg. 2008;22(4):269-80. http://dx.doi.org/10.1055/s-0028-1095886. PMid:20567703.
2. Eskiizmir G, Baker S, Cingi C. Nonmelanoma skin cancer of the head and neck: reconstruction. Facial Plast Surg Clin North Am. 2012;20(4):493-513. http://dx.doi.org/10.1016/j.fsc.2012.08.003. PMid:23084301.
3. Anvar BA, Evans BC, Evans GR. Lip reconstruction. Plast Reconstr Surg. 2007;120(4):57e-64e. http://dx.doi.org/10.1097/01.prs.0000278056.41753.ce. PMid:17805106.
4. Vukadinovic M, Jezdic Z, Petrovic M, Medenica LM, Lens M. Surgical management of squamous cell carcinoma of the lip: analysis of a 10-year experience in 223 patients. J Oral Maxillofac Surg. 2007;65(4):675-9. http://dx.doi.org/10.1016/j.joms.2006.03.054. PMid:17368363.
5. Ebrahimi A, Maghsoudnia GR, Arshadi AA. Maghsoudnia GR, Arshadi AA. Prospective comparative study of lower lip defects reconstruction with different local flaps. J Craniofac Surg. 2011;22(6):2255-9. http://dx.doi.org/10.1097/SCS.0b013e318232786d. PMid:22075831.
6. Seo HJ, Bae SH, Nam SB, Choi SJ, Kim JH, Lee JW, et al. Lower lip reconstruction after wide excision of a malignancy with barrel-shaped excision or the Webster modification of the Bernard operation. Arch Plast Surg. 2013;40(1):36-43. http://dx.doi.org/10.5999/aps.2013.40.1.36. PMid:23362478.
7. Dieffenbach JF. Chirurgische erfahrungen, besonders ueber die wiederherstellung zerstoerter theile des menschlichen koerpers nach neuen methoden. Bedim: T.C.F. Enslin; 1829.
8. Burow A. Zur Blepharoplastik. Monatsschr Med Augenheilkd Chir. 1838;1:57-61.
9. Bernard C. Cancer de la levre inferieur opere par un procede nouveau. Bull Soc Chir Paris. 1853;3:357-60.
10. Abbe R. A new plastic operation for the relief of deformity due to double harelip. Plast Reconstr Surg. 1968;42(5):481-3. PMid:4880838.
11. Karapandzic M. Reconstruction of lip defects by local arterial flaps. Br J Plast Surg. 1974;27(1):93-7. http://dx.doi.org/10.1016/0007-1226(74)90068-X. PMid:4593704.
12. Webster RC, Coffey RJ, Kelleher RE. Total and partial reconstruction of the lower lip with innervated musclebearing flaps. Plast Reconstr Surg Transplant Bull. 1960;25(3):360-71. http://dx.doi.org/10.1097/00006534-196004000-00007. PMid:13843351.
13. Fujimori R. "Gate flap" for the total reconstruction of the lower lip. Br J Plast Surg. 1980;33(3):340-5. http://dx.doi.org/10.1016/0007-1226(80)90079-X. PMid:7426811.
14. Schuchardt K. Operationen im gesicht und im kieferbereich operationen an den lippen. In: Bier A, Braun H, Kummel H, editores. Chirurgishche operationslehre. Leipzig: JA Barth; 1954.
15. Konstantinović VS. Refinement of the Fries and Webster modifications of the Bernard repair of the lower lip. Br J Plast Surg. 1996;49(7):462-5. http://dx.doi.org/10.1016/S0007-1226(96)90031-4. PMid:8983548.
16. Zilinsky I, Winkler E, Weiss G, Haik J, Tamir J, Orenstein A. Total lower lip reconstruction with innervated muscle-bearing flaps: a modification of the Webster flap. Dermatol Surg. 2001;27(7):687-91. PMid:11442627.
17. Wechselberger G, Gurunluoglu R, Bauer T, Piza-Katzer H, Schoeller T. Functional lower lip reconstruction with bilateral cheek advancement flaps: revisitation of Webster method with a minor modification in the technique. Aesthetic Plast Surg. 2002;26(6):423-8. http://dx.doi.org/10.1007/s00266-002-2051-5. PMid:12621564.
18. Oliveira AC, Orsi V, Oliveira VS, Orige SC, Gus EI, Portinho CP, et al. Otimização da continência salivar na reconstrução labial inferior pela técnica de Webster-Bernard modificada. Rev Bras Cir Craniomaxilofac. 2009;12(2):41-6.
19. Hamahata A, Saitou T, Ishikawa M, Beppu T, Sakurai H. Lower lip reconstruction using a combined technique of the Webster and Johanson methods. Ann Plast Surg. 2013;70(6):654-6. http://dx.doi.org/10.1097/SAP.0b013e318243353f. PMid:23123609.
20. Siqueira EJ, Alvarez GS, Laitano FF, Martins PD, Oliveira MP. Estratégias em reconstrução do lábio inferior. Rev Bras Cir Plást. 2012;27(4):536-41. http://dx.doi.org/10.1590/S1983-51752012000400011.
21. Boisson VA, Muiniz LS, Leite AB, Jesus BM, Barbosa LC, Guimarães DR. Algoritmo para reconstrução dos lábios. Rev Bras Cir Plást. 2011;26(3 Supl 1):44.
22. Cupp CL, Larrabee WF JR. Reconstruction of the lips. Oper Tech Otolaryngol--Head Neck Surg. 1993;4(1):46-53. http://dx.doi.org/10.1016/S1043-1810(10)80106-X.
23. Jeng SF, Kuo YR, Wei FC, Su CY, Chien CY. Reconstruction of concomitant lip and cheek through-and-through defects with combined free flap and an advancement flap from the remaining lip. Plast Reconstr Surg. 2004;113(2):491-8. http://dx.doi.org/10.1097/01.PRS.0000100809.43453.C7. PMid:14758208.
24. Akcam TM, Gubisch W, Unlu H. Nonmelanoma skin cancer of the head and neck: surgical treatment. Facial Plast Surg Clin North Am. 2012;20(4):455-71. http://dx.doi.org/10.1016/j.fsc.2012.08.001. PMid:23084298.
25. Sbalchiero JC, Anlicoara R, Cammarota MC, Leal PR. Reconstrução labial: abordagem funcional e estética após ressecção tumoral. Rev Soc Bras Cir Plást. 2005;20(1):40-5.
26. Ünsal Tuna EE, Oksüzler O, Ozbek C, Ozdem C. Functional and aesthetic results obtained by modified Bernard reconstruction technique after tumour excision in lower lip cancers. J Plast Reconstr Aesthet Surg. 2010;63(6):981-7. http://dx.doi.org/10.1016/j.bjps.2009.02.073. PMid:19364684.
27. Civelek B, Celebioglu S, Unlu E, Civelek S, Inal I, Velidedeoglu HV. Denervated or innervated flaps for the lower lip reconstruction? Are they really different to get a good result? Otolaryngol Head Neck Surg. 2006;134(4):613-7. http://dx.doi.org/10.1016/j.otohns.2005.12.010. PMid:16564383.
28. Sarmento GS, Denadai R, Somensi RS, Giancolli AP, Junqueira JG NO, Buzzo CL, et al. Avaliação de déficit neurossensorial em pacientes com síndromes craniofaciais submetidos a avanço horizontal do mento. Rev Bras Cir Plást. 2013;28(2):205-11. http://dx.doi.org/10.1590/S1983-51752013000200006.
29. Essick GK. Comprehensive clinical evaluation of perioral sensory function. Oral Maxillofac Surg Clin North Am. 1992;4(2):503-26.
30. Oliveira MP, Martins PD, Cunha GL, Alvarez GS, Gazzalle A, Siqueira EJ. Use of the vermilion myomucosal flap with or without the mentolabial skin flap for lower lip reconstruction. Rev Bras Cir Plást. 2011;26(3):433-8.
31. Faveret P, Franco D, Boghossian LC, Medeiros J, Franco T. Carcinoma de lábios: análise de tratamento cirúrgico realizado em hospital universitário. Rev Bras Cir Craniomaxilofac. 2009;12(4):155-8.
32. Araújo BC NO, Duarte IS, Ferreira LM, Abrahao M. Reconstrução total do lábio inferior com retalhos de face. Rev Soc Bras Cir Plast. 2003;18(1):19-24.
33. Sabino M NO, Castilho HT, Ferreira LM, Hochberg J, Toledo SR. Utilization of the depressor anguli oris musculocutaneous flap for lip reconstruction. Ann Plast Surg. 2000;44(1):23-8. http://dx.doi.org/10.1097/00000637-200044010-00005. PMid:10651362.
34. Ayhan Oral M, Zeynep Sevim K, Görgü M, Yücel Öztan H. Sensory recovery with innervated and noninnervated flaps after total lower lip reconstruction: a comparative study. Plast Surg Int. 2013;1-7. http://dx.doi.org/10.1155/2013/643061. PMid:24381755.
35. Malard O, Corre P, Jégoux F, Durand N, Dréno B, Beauvillain C, et al. Surgical repair of labial defect. Eur Ann Otorhinolaryngol Head Neck Dis. 2010;127(2):49-62. http://dx.doi.org/10.1016/j.anorl.2010.04.001. PMid:20822758.
1. Instituto de Cirurgia Plástica Craniofacial, Hospital SOBRAPAR, Campinas, SP, Brazil
2. Universidade de São Paulo, São Paulo, SP, Brazil
Institution: Study performed at the Instituto de Cirurgia Plástica Craniofacial, Hospital SOBRAPAR, Campinas, SP, Brazil.
Corresponding author:
Cesar Augusto Raposo do Amaral
Hospital de Crânio e Face SOBRAPAR
Avenida Adolpho Lutz, 100 - Cidade Universitária
Campinas, SP, Brazil Zip Code 13083-880; P.O. Box 6028
E-mail: cesaraugustoraposo@hotmail.com
Article received: May 2, 2014.
Article accepted: August 31, 2014.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter