

Articles - Year 2004 - Volume 19 -
The Effects of Pentoxifylline and Buflomedil Hydrochloride in Random Flaps in Rats under the Influence of Nicotine
Efeitos da Pentoxifilina e o Cloridrato de Buflomedil em Retalhos Randomizados em Ratos sob Influência da Nicotina
ABSTRACT
Many reports in the literature show the harmful effects of nicotine on microcirculation, leading to increased risk of skin flap ischemia. In an attempt to reverse these effects, an experimental trial was carried out to test two drugs: pentoxifylline, whose action changes blood viscosity, and buflomedil, which is a vasoactive substance that acts on microcirculation. After a 6-week treatment with nicotine, 40 rats were subdivided into 4 groups and operated on to prepare a random dorsal skin flap. Group A was not treated with any of the drugs. Groups B and C were treated for 7 postoperative days with pentoxifylline and buflomedil, respectively. Group D, the control group, received only saline solution. VVhen compared, there was a significant difference between groups A and D (p< 0.05). We concluded that these drugs showed some effectiveness in the reversal of the effects caused by nicotine, but it would be necessary to have larger samples to achieve statistically significant results.
Keywords: Ischemia; necrosis; nicotine; flaps; smoking
RESUMO
São abundantes na literatura trabalhos que demonstraram os efeitos nocivos da nicotina na microcirculação, resultando em maior risco de isquemia de retalhos cutâneos. Na tentativa de reverter esses efeitos, foi desenvolvido um estudo experimental no qual foram testadas duas drogas: a pentoxifilina, que atua alterando a viscosidade sangüínea, e o buflomedil, que é uma substância vasoativa com ação na microcirculação. Após tratamento com nicotina durante 6 semanas, 40 ratos foram subdivididos em 4 grupos e operados para confecção de um retalho cutâneo dorsal randomizado. O grupo A não recebeu tratamento com as drogas. Os grupos B e C foram tratados no pós-operatório durante 7 dias com pentoxifilina e buflomedil, respectivamente. O grupo D, controle, recebeu apenas soro. Quando comparados, houve uma diferença significativa entre os grupos A e D (p< 0,05), mostrando uma participação efetiva da nicotina na ocorrência de necrose. Os grupos tratados com as drogas mostraram uma resposta clínica importante na melhora da sobrevida dos retalhos, entretanto esses valores não foram estatisticamente significantes (p>0,05). Concluímos que essas drogas mostram alguma efetividade na reversão dos efeitos causados pela nicotina, mas se faz necessário ampliar as amostras para obtermos resultados com significado estatístico.
Palavras-chave: Isquemia; necrose; nicotina; retalhos; tabagismo
Clinical and experimental evidence shows an increased risk of skin flap necrosis in smokers. The increase in morbidity due to vascular hypoperfusion implies that nicotine metabolites significantly affect microcirculation(1). Mosley and Finseth were me first to report me negative effects on healing, observing me reduction in blood flow in distal regions in me fingers, and changes in healing in me hands of smokers(2). Another study, by Rees et al., showed that smoking patients are twice more likely to develop skin necrosis after rhytidectomy when compared to non-smoking patients(3).
Cigarette smoke has more than 3,800 components, but only carbon monoxide, nitric acid, hydrogen, cyanide, and nicotine have been widely identified as leading causes of adverse effects, bom in me cardiovascular system and in skin microcirculation (1). Nicotine reduces skin blood flow by 30 to 40%, because it stimulates me release of catecholamines and norepinephrine, which cause vasoconstriction. It also reduces me synthesis of vasodilating prostacyclin and increases me release of thromboxane, a vasoconstritor. In microcirculation it induces platelet activation and aggregation, producing microthromboses(2). Moreover, it changes me healing process of wounds by reducing proliferation fibroblasts and macrophages and stimulating catecholamines, which are co-factors in me formation of chalones, which, in turn, inhibit me epithelialization process.
There have been some studies with vasodilating drugs, like nifedipine and nitroglicerine in rats exposed to cigarette smoke, with significant clinical results in me survival of random flaps(4).
Pentoxifylline is a byproduct of methylxanthines that is used in me treatment of intermittent claudication. It improves blood viscosity, as it increases me capacity of deformation of erythrocytes and granulocyres, reduces fibrinogen levels and thromboxane release, inhibits platelet aggregation, and increases prostacyclin levels. These effects were not seen in people with normal blood coagulation, only changes in blood viscosity(2).
Buflomedil hydrochloride is a vasoactive substance that acts on cerebral and peripheral microcirculation, working by blocking me passage of calcium to vascular smooth muscles. Ir does not have an adrenergic blocking action not does it change hemodynamic constants (5). Due to these effects, it has been used empirically in plastic surgery to improve flap perfusion, although no studies yet show its effectiveness.
OBJECTIVE
The first objective was to establish me negative effects of nicotine in the survival of random flaps in rats. The second objective was to check me influence of pentoxifylline (TrentalÒ or PentoxÒ) and buflomedil hydrochloride (BufedilÒ) in me survival of random flaps in rats exposed to nicotine at doses that produce levels comparable to human smoking.
MATERIALS AND METHODS
Forty female rats of the race LOU/M, weighing between 250g and 350g and aged berween 6 and 8 months were used in this study. This group was randomly divided into 4 groups, with 10 animais each:
A: rats exposed to nicotine
B and C: rats exposed to nicotine and drugs
D: control group
GROUP A: NICOTINE + SALINE SOLUTION
Nicotine: 0.5 mg/kg in 0.1 ml of saline solution injected subcutaneously, twice a day, for 6 weeks in me preoperative and 1 week in me postoperative.
Saline solution: 1 ml of saline solution, intraperitoneally, for 1 week in me postoperative.
GROUP B: NICOTINE + PENTOXIFYLLINE
Nicotine: 0.5 mg/kg in 0.1 ml of saline solution injected subcutaneously, twice a day, for 6 weeks in me preoperative and 1 week in me postoperative.
Pentoxifylline: 20 mg/kg in 1.0 ml of saline solution, intraperitoneally, twice a day, for 1 week in me postoperative.
GROUP C: NICOTINE + BUFLOMEDIL
Nicotine: 0.5 mg/kg in 0.1 ml of saline solution, injected subcutaneously, twice a day, for 6 weeks in me preoperative and 1 week in me postoperative.
Buflomedil: 34.2 mg/kg in 1.0 ml of saline solution, intraperitoneally, twice a day, for 1 week in me postoperative.
GROUP D: CONTROL GROUP: SALINE SOLUTION + SALINE SOLUTION
Saline solution: 0.1 ml of saline solution, subcutaneously, twice a day, for 6 weeks, and 1.0 ml, intraperitoneally, twice a day, for 1 week in the postoperative.
TECHNIQUE
We initially conducted a pilot test to adjust the dose of nicotine. For one week, the 30 rats were submitted to the application of intradermal nicotine at the initial dose of 2 mg/kg, which was slowly reduced until it reached a non-convulsant dose. The standard dose was established at 0.5 mg/kg, compatible with many reports in the literature(1,2).
After 6 weeks of treatment with nicotine for groups A, B, and C, and saline solution for group D, the rats underwent a surgical procedure. Ketamine + Clorpromazine were used for anesthesia at the intramuscular doses of 2.5 ml/kg and 0.5 ml/kg, respectively. Dorsal flaps were obtained according to McFarlane's caudal base technique(6) modified by Hammond(7), based on the level of the posterior iliac crest, formed by skin and the panniculus carnosus (Figs. 1 and 2).
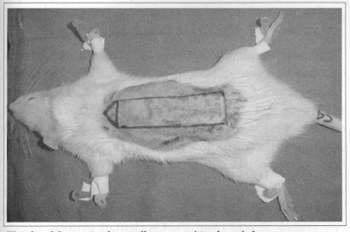
Fig. 1 - Marking of flap on the dorsal region of the rat.
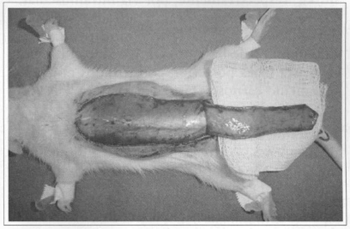
Fig. 2 - Construction of dorsal flap.
2 x 7 cm molds were used to design these flaps, with a compensation triangle on their distal end (2 x 1.5 x 1.5), and they were used as total skin grafts (Fig. 1).
After dissection and elevation of the flap, first the danar site was closed with continuou:" suture (Fig. 3). Then the graft was surured to the base of the lifted flap to prevent any contact with the vascularized bed where attachment of the danar site is not normally possible. The flap was attached over the dorsal skin and sutured with 4 equidistant lateral stitches, and one on each angle (Fig. 4). After the procedure, the dorsal region of the rats was covered with a BioclusiveÒ dressing and they were put in separate cages, receiving water and food ad libitum.
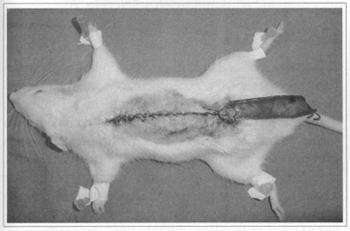
Fig. 3 - Primary synthesis of donor site with fixation of graft at the base of the flap.
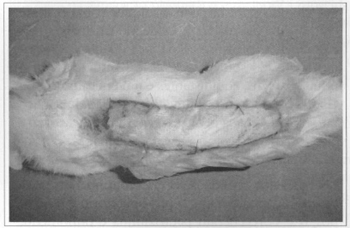
Fig. 4 - Fixation of flap on the dorsal region after suture of the donor site.
The rats of groups A, B and C continued receiving nicotine during the postoperative, and groups B and C received pentoxifylline and buflomedil, respectively. Group D continued receiving intramuscular and intraperitoneal saline solution.
The percentage of skin necrosis in the flaps was assessed on the 5th and 7th postoperative day and observed for another day to confirm these data. Measures were taken in millimeters and the area of viable tissue was calculated in square centimeters (Fig. 5).
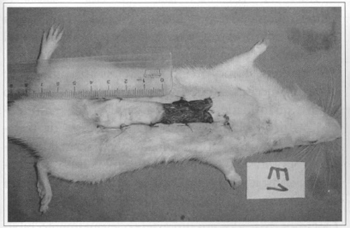
Fig. 5 - Measurement of viable areas in centimeters.
STATISTICAL ANALYSIS
The Anova F Test was used in this study to analyze the four groups and the T Test was applied to for the paired analysis of groups A x B, A x C, A x D, B x D and C x D. Averages and standard deviations were calculated. The level of significance adopted was "p" smaller than or equal to 0.05.
RESULTS
The results of each group are shown in Table I. In the entire experiment there were a total of 4 dcaths without an identifiable cause. These deaths occurred either during the anesthetic procedure or in the immediate postoperative. Some rats were excluded from the study because, despire care to isolate the operated area with an occlusive dressing, amophagia of the flap occurred, hindering appropriate evaluation.
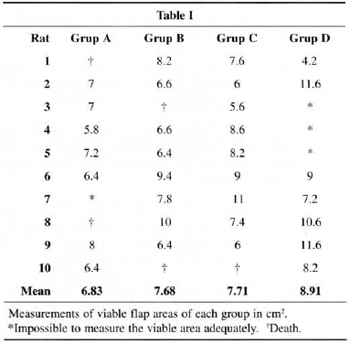
Averages and standard deviations were calculated for each group for these results. They were respectively: group A = 6.83 ± 0.70; group B = 7.71 ± 1.73; group C = 7.68 ± 1.42; and group D = 8.91 ± 2.67 (Fig. 8). The group with the smallest standard deviation was group A, and the one with the largest deviation was D.
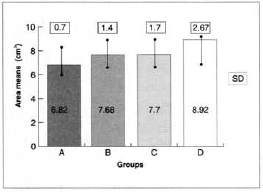
Fig. 8 - Area means of each group and standard deviations.
The result of the F Test was 1.65, with p>0.05, therefore, not significant. The T Test paired analyses resulted in p< 0.05 when comparing groups A and D (Fig. 7). The other groups, in spite of the considerable clinical difference, did not have a significant "p" at 5% (Fig. 6).
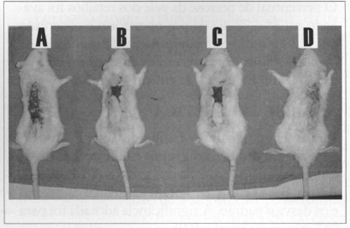
Fig. 6 - Comparison of groups: A= nearly total necrosis of flap, B and C = partial necrosis and O = minimum necrosis.
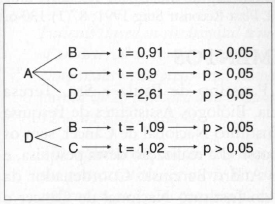
Fig. 7 - Results of T test for each pair and sequencee.
DISCUSSION
The pharmacokinetics of nicotine has been widely studied and there are many experimental models that attempt to simulate the effects of smoking in human beings. Studies comparing the action of nicotine as a base with the action of tartarate salt showed that the first has greater and longer plasmatic levels. In this manner, when one chooses using the base, it is necessary to titrate the previously defined dose to administer the tartarate. For this reason, we conducted a weeklong pilot test, to study the clinical effects of the drug and define the non-lethal dose for the chosen rat strain.
Another difficulty in studying the effects of nicotine in experimental models is to reach plasma levels that effectively simulate that of smoking adults. There are many variables, such as type of exposure (cigarette smoke, subdermal injections, slow-release capsules), amount of exposure/day for keeping a constant plasma level, time of treatment, type of nicotine, strain of the animals used, and ali of them influence results considerably. Therefore, these variables need other studies to be better defined.
Based on extensive research of the literature, we decided to define the time of treatment with nicotine at 6 weeks. During surgical procedures, we drew and stored blood samples of the animals, so that we could continue the studies with the plasmatic leveis of cotinine, a metabolite of nicotine. However, we may regard the treatment as effective, considering that when comparing groups A (nicotine) and D (saline solution), we found a significant difference (p< 0,05)in the survival of flaps of non-smoking rats.
The action of pentoxifylline on the survival of random flaps has been fairly well explored. lts hematological effects include increased deformation capacity of erythrocytes and increased capillary blood flow(10). Other results have been described nonetheless. Pentoxifylline increases hypercoagulability, decreases platelet aggregation, by increasing plasmin, plasminogen activating factor, antithrombin III, and by decreasing fibrinogen, alpha-2-antiplasrnin, alpha-1-antitrypsin and alpha-2-rnacroglobulin(11).
Despire all the effects described, the drug's clinical applicability is still controversial. Experimental studies have shown conflicting results. Some authors such as Karacaoglan et al. have demonstrated an increase in flap survival with pentoxifylline(12,16). Others(13) have not correlated microscopic changes with increased flap survival. Another major aspect is the initial time of treatment. For Williams et al. (14) preoperative treatment of at least 14 days is necessary in order to reach desired results. On the other hand, the work carried out by Hayden(15), that tested 3 different utilization regimens including preoperative administration, did not confirm previous findings.
In the present study we began using the drug on the same day of surgery, based on studies performed previously (15>, and maintained its use for 7 days. Results showed an improvement in flap survival, as shown in Table I and Fig. 8, although values were not significant (p>0.05).
Buflomedil hydrochloride has an inhibitory effect on platelet aggregation and improves the deformation capaciry of red blood cells with abnormal flowability.In vitro studies suggest that the drug has an unspecific antagonist effect on the calcium ion and an unspecific alpha receptor blocking effect(5).
Experimental studies have shown adequate results in reverting flap ischemia. Uhl et al.(18) showed that the drug can be used therapeutically in skin flaps and that preoperative treatment for an additional 5 days did not change previous results. Another srudy, in which treatment was given 4 hours before the operarion and 5 minutes after, attained significant values for both groups(l9).
In our study, buflomedil and pentoxifylline were used in the same way. Results were also very similar. There was no significant result in the group treated with buflomedil in comparison to the remaining groups, despire marked clinical improvement. This finding, like the results found for the pentoxifylline group, may be due to the smali sample size, although it is an experimental study Contrasting results would probably be diluted in a higher number of events, as with rat D1, whose results are completely different from those in the remainder of the group.
CONCLUSION
Various drugs have been tested for reverting the deleterious effects of nicotine, although findings are still unclear. No definitive results have been found, but there is clinical evidence that some drugs exert favorable effects, and improve the survival of skin flaps. The present study has confirmed the effects of nicotine described elsewhere, by showing greater damage to flaps constructed in rats exposed to the drug. Although buflomedil and pentoxifylline improve vascularization of flaps, no statistically significant results have been recorded. We therefore need to expand our research, by increasing the number of cases in each group to create significant data.
REFERENCES
1. Forrest CR, Oang CY,Lindsay WK. Pathogenesis of ischemic necrosis in random-Pattern skin flaps induced by long-term low dose nicotine treatment in the rato Plast Reconstr Surg 1991; 87(3):518-28.
2. Aker JS, Mancoll J, Lewis B, Collen LB. The effect of Pentoxifylline on randorn-pattern skin-flap necrosis induced by nicotine treatrnent in the rat.Plast Reconstr Surg 1997; 100(1):66-71.
3. Rees TD, Liverett DM, Guy CL. The effect of cigarette smoking on skin-flap survival in the face lift patient. Plast Reconstr Surg 1984; 73(6 ): 911- 5.
4. Davis BW,Lewis RD, Pennington G. The impact of vasodilators on random-pattem skin flap survival in the rat following mainstream smoke exposure. Ann Plast Surg 1998; 40(6 ):630-6.
5. Thomas JG, MD, Rainer KES, Hammersen F, MD, Messmer K, MD. Increase in skin-flap survival by the vasoactive drug buflomedil. Plast Reconstr Surg 1991; 87(1):130-41.
6. Mcfarlane RM, De Young G, Henry RA. The design of a pedicle flap in the rat to study necrosis and its prevention. Plast Reconstr Surg 1965; 35:177.
7. Hanunond DC, Brooksher RD, Mann RI, et al. The dorsal skin flap model in the rat: factors influencing survival. Plast Reconstr Surg 1993; 91(2) :316-21.
8. Nolan I, Jenkins RA, Kurihara K, Schultz R. The acutte effecta of cigarette smoke exposure on experimental skin flaps. Plast Reconstr Surg 1985; 75(4):544 -51.
9. Forrest CR, Pang CY, Lindsay WK. Dose and time effects of nicotine treatment on the capillary blood flow and viability of random pattem skin flaps in the rat. Br J Plast Surg 1987; 40(3):295-9.
10. Freedman AM, Hyde GL, Luce EA. Failure of pentoxifylline to enhance skin flap survival in the rat.Ann Plast Surg 1989; 23(1):31-4.
11. Samlaska CP, Winfield EA. Pentoxifylline. J Am Acad Dermatol. 1994; 30(4):603-21.
12. Karacaoglan N, Akbas H. Effect of parenteral pentoxifylline and topical nitroglycerin on skin flap survival. Otolaryngol Head Neck Surg 1999; 120(2):272-4.
13. Pratt MF, Williams PB. Pentoxifylline and acerylsalicylic acid in a pig random skin-flap model. J Otolaryngol 1996; 25(6):393-8.
14. Williams PB, Hankins DB, Layton CT, Phan T, Pratt MP. Long-term pretreatment with pentoxifylline increases random skin flap survival. Arch Otolaryngol Head Neck Surg. 1994 Jan;120(1) :65-71
15. Hayden RE, Snyder BJ. Pharmacologic manipulation of random skin flaps with pentoxifylline. Laryngoscope 1993; 103(2):185-8.
16. Monteiro DT, Santamore WP, Nemir PJR. The influence of pentoxifylline on skin-flap survival. Plast Reconstr Surg 1986; 77(2):277-81.
17. Quirinia A, Gottrup F, Viidik A. Failure of buflomedil to improve healing in ischaemic kin flaps. Scand J Plast Reconstr Surg Hand Surg 1996; 30(2):81-7.
18. Uhl E, Rosken F, Curri SB, Menger MD. Reduction of skin flap necrosis by transdermal application of buflomedil bound to liposomes. Plast Reconstr Surg 1998; 102(5):1598-1604.
19. Galla TJ, Saetzler RK, Hanunersen F, Messmer K. Increase in skin-flap survival by the vasoactive drug buflomedil. Plast Reconstr Surg 1991; 87(1): 130-6.
ACKNOWLEDGEMENTS
To Mr. Emílio Faustino de Paula and Ms. Teresa Gonçalves Correia, Assistant Research Biologists of the Animal Center of the Instituto Nacional de Câncer, without whom this study would not have been possible, and to Dr. Marcello André Barcinsk, Basic Research Coordinator of Instituto Nacional de Câncer and tutor of the present work.
I - Head of the Plastic Surgery and Microsurgery Clinic of INCA.
II - Resident Physician of the Plastic Surgery and Microsurgery Clinic ofthe Instituto Nacional de Câncer-INCA.
III - Staff of the Plastic Surgery and Microsurgery Clinic of INCA.
Instituto Nacional de Câncer - INCA - Plastic Surgery and Microsurgery Clinic
Address for correspondence:
Paulo Roberto Leal, MD
Pça. da Cruz Vermelha, 23 - 8º andar
20230-130 - Rio de Janeiro - RJ Brazil
Phone: (55 21) 2506-6087
e-mail prleal@inca.gov.br


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter