

Ideas and Innovation - Year 2015 - Volume 30 -
Z brachiothoracoplasty for body contouring after massive weight loss
Braquiotoracoplastia em Z no tratamento do contorno corporal após perda ponderal maciça
ABSTRACT
INTRODUCTION: Brachioplasty treats deformities of the upper limbs. Lateral thoracoplasty treats the upper torso. Brachioplasties, thoracoplasties, and brachiothoracoplasties have been performed with Z-plasty for deformities of the upper limbs and upper third of the chest, in the Sapopemba State Hospital. Objective: We describe modifications of surgical technique for the performance of Z brachiothoracoplasty, and evaluate the results of treatment of deformities of the lateral chest.
METHOD: Thirty-one Patients underwent brachiothoracoplasty and lateral thoracoplasty. The demarcation was made with the patient upright, and the upper limbs abducted at 90º. Marking for brachioplasty was performed using a double-ellipse, to lengthen the modified demarcation along the anterior axillary line toward the inframammary crease in a Z shape.
RESULTS: All patients reported an improvement in the contour of the region, and there were no complaints regarding the positioning of the scar.
DISCUSSION: Z brachiothoracoplasty consists of extending the incision line on the medial aspect of the arm, passing proximally to the axilla, and continuing through the midaxillary line to the inframammary crease. There was an improvement in the contour of the dorsal region and the skin folds of the lateral thoracic region.
CONCLUSION: Z brachiothoracoplasty and lateral thoracoplasty have the great advantage of eliminating a circumferential scar on the upper torso, thereby improving the contour of the region through skin resection in both the craniocaudal and anteroposterior directions.
Keywords: Obesity; Upper limbs/surgery; Thoracoplasty; Bariatric surgery.
RESUMO
INTRODUÇÃO: A braquioplastia trata as deformidades dos membros superiores. A toracoplastia lateral visa o tratamento do torso superior. As braquioplastias, toracoplastias e também as braquiotoracoplastias em Z têm sido utilizadas no Hospital Estadual de Sapopemba no tratamento das deformidades dos membros superiores e terço superior do tórax. Objetivo: Propõe-se descrever as modificações na técnica cirúrgica resultando na braquiotoracoplastia em Z e analisar a casuística e os resultados obtidos, no tratamento das deformidades da região lateral do tórax.
MÉTODO: Foram submetidos à braquiotoracoplastia e toracoplastia lateral 31 pacientes. A demarcação foi feita em posição ortostática, e os membros superiores abduzidos em 90o. Iniciou-se pela demarcação da braquioplastia, em duplo fuso, prolongando-se de maneira modificada a demarcação, seguindo pela linha axilar anterior em direção ao sulco inframamário em forma de Z.
RESULTADOS: Todos os pacientes referiram melhora do contorno da região e não houve queixas quanto ao posicionamento da cicatriz.
DISCUSSÃO: O procedimento da braquiotoracoplastia em Z atual consiste em estender a linha de incisão da face medial do braço, passando proximalmente à axila e continuando pela linha axilar média até o sulco mamário. Ocorreu a melhora do contorno da região dorsal e das dobras cutâneas da região torácica lateral.
CONCLUSÃO: A braquiotoracoplastia em Z e a toracoplastia lateral têm a grande vantagem de eliminar a cicatriz circunferencial no torso superior, promovendo a melhoria do contorno dessa região por meio da ressecção cutânea tanto no sentido craniocaudal, como anteroposterior.
Palavras-chave: Obesidade; Membros superiores/cirurgia; Toracoplastia; Cirurgia bariátrica.
Obesity is a growing problem, and is estimated to affect around one-third of the world's population; this is a concern in both developed and developing countries1. As a result, there is also an increase in surgical management of weight loss, specifically, bariatric surgery. Consequently, there is a high degree of lipodystrophy and flaccid skin in patients submitted to this surgery2.
The management of the sequelae of rapid weight loss involves the resection of surplus skin in a series of surgical stages3,4, and success depends upon proper patient selection and the technique used; evaluation of patient expectations, respect for their limits, the limits of the procedure, and the healing process must be considered.
Brachioplasty treats deformities of the upper limbs, and generally uses the suspension of the upper third of the torso. Frequently, the results of the procedures described for this region are underestimated, with resulting circumferential, extended, or poorly-positioned scars.
Lateral thoracoplasty aims to treat the upper torso, and has the great advantage of avoiding a scar extending to the dorsal region; the procedure extends the resulting curvilinear scar at the midaxillary line toward the inframammary crease, in a more discreet and less visible position5.
Brachioplasties, thoracoplasties, and Z brachiothoracoplasties have been routinely performed in the Sapopemba State Hospital-HESAP (affiliated with the Hospital das Clínicas, University of Sao Paulo, Brazil) since 2008, to treat deformities of the upper limbs and upper third of the chest.
OBJECTIVE
We describe the modifications of surgical technique for the performance of Z brachiothoracoplasty, and evaluate the results of treatment of deformities of the lateral region of the chest.
METHOD
Thirty-one patients (mean age, 44.2 years [29-68]; 27 women and 4 men) underwent brachiothoracoplasty and lateral thoracoplasty.
In 14 cases, combined brachioplasty and lateral thoracoplasty was performed, and in 17 patients, the surgeries were performed at different times.
Preoperative demarcation was performed with the patient upright, with the upper limbs abducted at 90º. Brachioplasty demarcation was performed using the technique described by Aly et al.6 in two stages; the demarcation was lengthened, following the anterior axillary line toward the inframammary fold. With bidigital pinching, the amount of tissue to be excised from the lateral thoracic region is delineated. Thus, the final positioning of the scar is on the midaxillary line. When the surgeries were performed at different times, brachioplasty always preceded lateral thoracoplasty.
With the patient supine and upper limbs abducted, surgical demarcation is repeated. The entire procedure was performed in the decubitus position, without the need to reposition the patient. All patients underwent the procedure under general anesthesia, with prophylaxis for deep vein thrombosis and pulmonary embolism using compression stockings and intermittent pneumatic compression. The patient was discharged on the first postoperative day, with scheduled appointments at 4, 7, 14 and 1 month after surgery.
The surgery on the upper limbs was performed with resection of the demarcated area, always starting with an anterior incision, and performing the detachment above the superficial fascia in the caudal or posterior direction, up to the preoperative demarcation. The procedure on the lateral thoracic region followed, beginning with an anterior incision up to the subcutaneous cellular tissue, releasing the flap, continuing to the superficial fascia, and up to the previously established demarcation.
To avoid excess resection or sutures under tension, the amount of tissue to be excised was confirmed by splitting the flaps in compensation triangles and repair points7 (Figures 1 and 2).
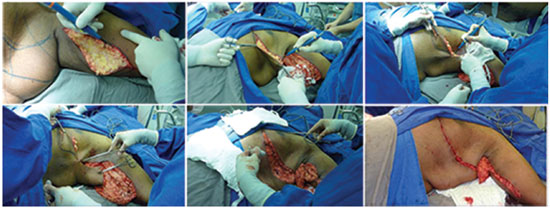
Figure 1. Steps of the Z brachiothoracoplasty operative technique (clockwise). 1A: Marking of brachiothoracoplasty. 1B: Anterior incision of brachiothoracoplasty. 1C: Detachment of the flap in the craniocaudal direction. 1D: Closure of deep planes and treatment of the axillary region.
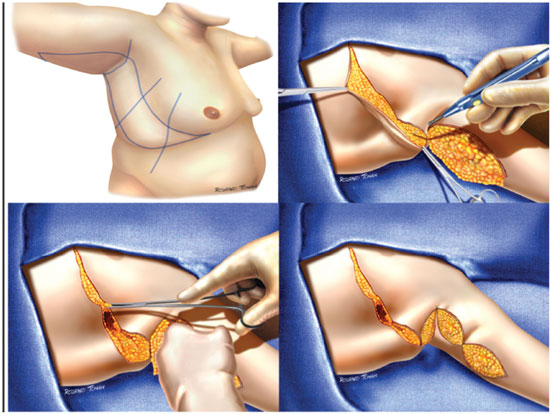
Figure 2. Demonstration of the surgical technique. 2A: Anterior incision of brachioplasty and detachment of the flap in the anteroposterior direction. 2B: Anterior incision of thoracoplasty and detachment of the flap in the craniocaudal direction. 2C, D: Splitting of the flaps and reference points to avoid overcorrection. 2E: Closing of deep planes. 2F: Treatment of axillary region.
After excision and hemostasis, closure was performed in layers, with Vicryl 3.0 sutures in the subcutaneous cellular tissue, subdermal sutures with Monocryl 3.0 and 4.0, and intradermal sutures using Monocryl 4.0. Drains were not used at the surgical site.
The axillary region was treated in the last step of the surgical procedure, changing orientation of the scar to avoid axillary adhesions. In this region, closure was performed with separated Mononylon 5.0 sutures.
RESULTS
Altogether 31 patients were operated, with a mean age of 44.2 years (29-68), 27 women and 4 men. The mean body mass index (BMI) before bariatric surgery was 43.59 kg/m2 (41.62-104.79), and the mean BMI before the current procedure was 23.64 kg/m2 (22.64-40.15).
Seromas developed in two patients, and were treated conservatively with serial punctures; one case of hematoma occurred, without the need for surgical intervention. There were no cases of infection, major dehiscence (i.e., larger than 1 cm2), or systemic complications.
All patients reported improvement in the contour of the region, and there were no complaints regarding the positioning of the scar (Figure 3).
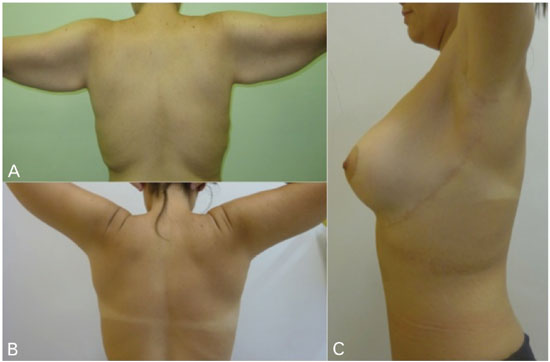
Figure 3. Posterior preoperative view, and posterior and lateral late postoperative period view, D, of a Z lateral brachiothoracoplasty.
DISCUSSION
Brachioplasty was first described in 1954 by Correa and Fernandes8, but there was a poor aesthetic result. Since then, several improvements have been made in the technique, such as the positioning of the scar in the brachial groove, and the longitudinal resection of excess fat, described by Baroudi in 19759; a quadrangular flap on the arm, with resection and closure of a T axillary scar, was described in 1979 by Juri et al.10.
The correction of lipodystrophy of the arms, elbows, and lateral chest wall in a single surgical procedure was described by Pitanguy5 in 1979.
The description of lateral excisions, however, is generally limited to vertical resections in the posterior axillary line. This type of procedure limits the treatment of patients with large amounts of flaccid skin, frequently found in patients undergoing bariatric surgery. In addition, the excess skin of the posterior region of the back is not accessed.
In cases of massive weight loss, the use of circumferential techniques, such as the suspension of the upper third of the torso, is common. These techniques, however, create generally extended or very visible scars11,12. In addition, the circumferential techniques promote the treatment of excess skin, with resection in the craniocaudal direction, at the expense of resection in the anteroposterior direction. Thus, however large the circumferential resection, it barely results in reduction of the perimeter of the area covered.
The current procedure of Z brachiothoracoplasty consists in extending the incision line on the medial aspect of the arm, passing proximally to the axilla, and stopping at this point, so that scar retraction does not occur, then continuing to the midaxillary line up to the inframammary crease. In this way, it is possible to improve the contour of the dorsal region and the skin folds of the lateral thoracic region, with skin resection both in the craniocaudal and anteroposterior direction.
This type of procedure may be combined with reverse abdominoplasty13, which complements the treatment of the epigastric region. According to our protocol, however, we prefer not to combine procedures in different anatomical regions, to avoid greater trauma and extended surgical time.
Recently, 30 cases of J torsoplasty were described by Clavijo-Alvarez and Hurwitz14, with a concept very similar to lateral thoracoplasty. The difference in the marking of brachioplasty, with positioning of the scar in the bicipital groove, and markings that extend inferiorly to the inframammary fold, should be noted. We believe that the position of the final scar, as an extension of the inframammary fold, allows better concealment with underwear or towels.
CONCLUSION
Z brachiothoracoplasty and lateral thoracoplasty are safe procedures with low morbidity, and satisfactorily manage excess skin of the lateral thoracic region, thereby eliminating skin folds and improving the contour of the dorsal region.
This approach has the great advantage of eliminating the circumferential scar on the upper torso, thus improving the contour of the region through skin resection, both in the craniocaudal and anteroposterior direction.
REFERENCES
1. Hurwitz DJ. Single-staged total body lift after massive weight loss. Ann Plast Surg. 2004;52(5):435-41.
2. Marcelino LF, Patrício ZM. A complexidade da obesidade e o processo de viver após a cirurgia bariátrica: uma questão de saúde coletiva. Ciênc Saúde Coletiva. 2011;16(12):4767-76.
3. Orpheu SC, Coltro PS, Scopel GP, Saito FL, Ferreira MC. Cirurgia do contorno corporal no paciente após perda ponderal maciça: experiência de três anos em hospital público secundário. Rev Assoc Med Bras. 2009,55(4):427-33.
4. Smaniotto PHS, Saito FL, Fortes F, Scople SO, Gemperli R, Ferreira MC. Comparative analysis of the evolution and postoperative complications of body contouring plastic surgeries after massive weight loss in young and elderly patients. Rev Bras Cir Plást. 2012;27(3):441-4.
5. Pitanguy I. Correction of lipodystrophy of the lateral thoracic aspect and inner side of the arm and elbow dermosenescence. Clin Plast Surg. 1975;2(3):477-83.
6. Aly A, Pace D, Cram A. Brachioplasty in the patient with massive weight loss. Aesthet Surg J. 2006;26(1):76-84.
7. Baroudi R. Dermolipectomy of the Upper Arm. Clin Plast Surg. 1975;2(3):485-94.
8. Correa Iturraspe M, Fernandez JC. Brachial dermolipectomy. Prensa Med Argent. 1954;41(34):2432-6.
9. Baroudi R. Umbilicaplasty. Clin Plast Surg. 1975;2(3):431-48.
10. Juri J, Juri C, Elías JC. Arm dermolipectomy with a quadrangular flap and "T" closure. Plast Reconstr Surg. 1979;64(4):521-5.
11. Hurwitz DJ, Holland SW. The L brachioplasty: an innovative approach to correct excess tissue of the upper arm, axilla, and lateral chest. Plast Reconstr Surg. 2006;117(2):403-11.
12. Strauch B, Rohde C, Patel MK, Patel S. Back contouring in weight loss patients. Plast Reconstr Surg. 2007;120(6):1692-6.
13. Schmitt GL, Rios MP, Scopel SO, Saito FL, Marques M, Ferreira MC. Abdominoplastia no paciente após perda ponderal maciça: experiência de cinco anos em hospital público secundário. Rev Bras Cir Plást. 2010;25(supl):1-102.
14. Clavijo-Alvarez JA, Hurwitz DJ. J torsoplasty: a novel approach to avoid circumferential scars of the upper body lift. Plast Reconstr Surg. 2012;130(2):382e-383e.
1. Sociedade Brasileira de Cirurgia Plástica, São Paulo, SP, Brazil
2. Universidade de São Paulo, São Paulo, SP, Brazil
Institution: Hospital Estadual de Sapopemba - HESAP, São Paulo, SP, Brazil.
Corresponding author:
Fabio Lopes Saito
Rua Al.Campinas, 977 - Jd. Paulista
São Paulo, SP, Brazil Zip code 01404-001
E-mail: fabio.saito@essere.med.br
Article received: October 15, 2013.
Article accepted: October 30, 2013.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter