

Case Report - Year 2015 - Volume 30 -
Use of the microsurgical anterolateral thigh flap to correct esophagocutaneous fistula
Uso do retalho microcirúrgico anterolateral da coxa na correção de fístula esôfago-cutânea
ABSTRACT
INTRODUCTION: The anterolateral thigh (ALT) flap has become an important tool in the microsurgical reconstruction of cutaneous and subcutaneous defects. Since the ALT flap can be up to 35 cm long, it can be used in both, esophageal reconstruction and cervical skin defects.
CASE REPORT: Patient C. S. M., a 57-year-old woman, presented with squamous cell carcinoma of the larynx and underwent radiotherapy and a total laryngectomy followed by reconstruction by primary closure. However, she developed a postoperative complication due to the formation of a cervical esophagocutaneous fistula that required four surgical procedures to ensure permanent closure. The latter procedure consisted of the creation of a microsurgical ALT flap to correct the esophagocutaneous fistula, the subject of this report.
CONCLUSIONS: The microsurgical ALT flap has extensive applications in various fields based on the following characteristics: reliable vascularization, long and broad vascular pedicle (at least 8 cm long), an extensive and easily delimited flap region, the possibility of reducing the primary flap thickness to 3-5 mm without compromising its vascularization, the possibility of a simultaneously dual approach because of the distance between the donor and recipient site, and the possibility of primary closure without the need for skin grafting. The case report presented in this study emphasizes the possibility of the use of a microsurgical ALT sandwich flap to correct a high output esophagocutaneous fistula.
Keywords: Reconstruction; Microsurgery; Fistula; Esophagus.
RESUMO
INTRODUÇÃO: O retalho anterolateral da coxa (RALC) vem se tornando uma ferramenta importante na reconstrução microcirúrgica de defeitos cutâneos e subcutâneos. Tendo em vista que o RALC pode se estender por até 35 cm, ele pode ser utilizado tanto na reconstrução esofágica como em defeitos cutâneos cervicais.
RELATO DO CASO: Paciente C.S.M., sexo feminino, 57 anos, apresentando um carcinoma espinocelular de laringe foi submetida à radioterapia e tratamento cirúrgico de laringectomia total seguido de reconstrução por fechamento primário. Porém, a paciente evoluiu com uma complicação pósoperatória devido à formação de uma fístula esôfago-cutânea cervical, sendo necessária a realização de 4 procedimentos cirúrgicos para fechamento definitivo da fístula. O último procedimento consistiu na realização de retalho microcirúrgico da região anterolateral da coxa para correção da fístula esôfago-cutânea, objeto desse relato.
CONCLUSÕES: O retalho microcirúrgico anterolateral da coxa possui extensa aplicação em diversos campos, baseada nas seguintes características: vascularização confiável, pedículo vascular longo e largo de no mínimo 8 cm, região do retalho extensa e de fácil delimitação, possibilidade de diminuir a espessura primária do retalho em 3 a 5 mm sem risco de comprometer sua vascularização, possibilidade de abordagem dupla simultânea devido à distância entre sítio doador e receptor, possibilidade de fechamento primário sem a necessidade de enxerto de pele. O relato do caso apresentado neste estudo justifica-se com o intuito de ressaltar
a possibilidade da utilização microcirúrgica do RALC em sanduíche na correção de fístula esôfago-cutânea de alto débito.
Palavras-chave: Reconstrução; Microcirurgia; Fístula; Esôfago.
The role of reconstructive microvascular surgery of the head and neck is well established1,2. These surgeries have evolved to focus not only on the functional and aesthetic aspects but also on donor area morbidity3. In this context, the microsurgical anterolateral thigh (ALT) flap has become the main tool for the reconstruction of cutaneous and subcutaneous defects, replacing various other flaps used in the past few decades1,3,4.
The major advantages of this flap are the possibility of lifting the flap while resecting the tumor, long vascular pedicle, moderately thick to thin flap thickness, simpler implementation than other flaps based on the musculocutaneous perforator vessels, lower donor area morbidity, and the possibility of reconstructing complex defects1-4.
The ALT flap can be constructed as a fasciocutaneous or myofasciocutaneous flap depending on the course of the perforating vessels of the lateral femoral circumflex artery and may still be elevated with multiple components (of the ALT cutaneous flap, vastus lateralis muscle, rectus femoris muscle, or tensor fasciae latae) to form a chimeric flap3.
The flap dimensions depend on the defect to be corrected and the donor area. It has been described to vary up to 8 inches wide by 15 cm long with primary closure of the donor area5. In the presence of major defects, grafting from the donor area may become necessary1,3,4,6. Another possibility is pre-expansion of the donor area with skin expanders aimed to create primary synthesis of the area after flap removal4.
Although the best choice for total esophageal reconstruction is the transfer of a free intestinal segment, a cutaneous flap can be used when there are contraindications for laparotomy (elderly patient, previous laparotomies with intestinal adhesions, surgeon inexperience with intestinal transfers, risk of prolonged ischemia during intestinal transfer)3.
Taking into account that the ALT flap can extend up to 35 cm, it can be used in the reconstruction of the cervical esophagus and long thoracic defects of the esophagus. The swallowing function of the esophagus prepared with a skin flap is lower than that achieved with the small or large intestine, making it necessary for the patient to manipulate the food with their hands. Another possible complication is stenosis of the mucocutaneous junction, which may appear years after the surgical procedure. The disadvantages of the ALT include anatomical variations as well as hairiness in some male patients3.
The reconstruction of the cervical region remains a challenging issue with regard to restoring function and aesthetics. Free flaps have the advantages of providing tissue with similar texture and color to the skin of the cervical region as well as offering good anatomical contour with minimal donor site morbidity. In addition, flap adaptability results in excellent neck mobility after postoperative recovery5,6.
CASE REPORT
Patient C. S. M., a 57-year-old woman, presented to the Head and Neck Surgery service at Faculdade de Medicina do ABC 4 years previously, complaining of dysphagia, odynophagia, and vocal alteration and was diagnosed with squamous cell carcinoma of the larynx T1N0M0. She reported smoking 10 cigarettes/day for 40 years and social drinking. She did not report any other comorbidities.
The patient underwent neoadjuvant radiotherapy followed by salvage total laryngectomy to resect the tumor as well as primary synthesis. In the postoperative period, she presented with a high output cervical esophagocutaneous fistula. After 2 months of unsuccessful clinical observation, nasogastric tube feeding, and curative measures, primary synthesis of the defect was attempted.
She developed early dehiscence and relapse of the fistula, being subjected to the new suturing attempt, presenting new early relapse. At that moment, she presented with an esophagocutaneous fistula approximately 1 cm in diameter with high output (Figure 1). To improve her nutritional intake, the patient underwent gastrostomy tube placement. After 6 months of expectant management, a new attempt to close the esophagocutaneous fistula was made by the Head and Neck Surgery team, using a Bakamjian deltopectoral flap. She presented with new early recurrence and requested an evaluation by the microsurgery team of the Hospital Estadual Mário Covas Plastic Surgery service of the Faculty of Medicine of ABC.
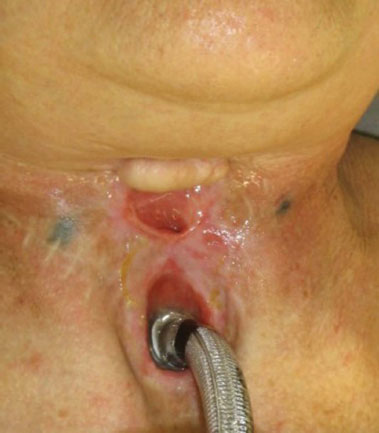
Figure 1. Initial clinical aspect of the esophagocutaneous fistula.
The team opted to implement a microsurgical ALT fasciocutaneous sandwich flap with half of the de-epidermized part used to reconstruct the anterior esophageal wall and the other half for reconstruction of the cervical skin portion (Figure 2). The patient progressed without complications and her oral diet was released after the 30th postoperative day. She has had no further recurrence of the fistula till 18 months (Figure 3). She underwent upper endoscopy, which revealed no signs of esophageal stenosis.
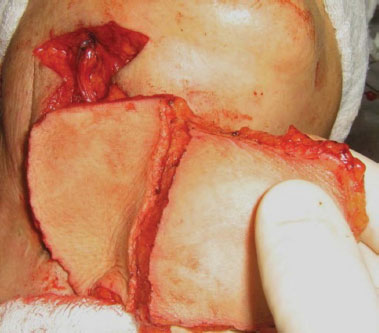
Figure 2. Extension of the microsurgical anterolateral thigh flap after thickness standardization.
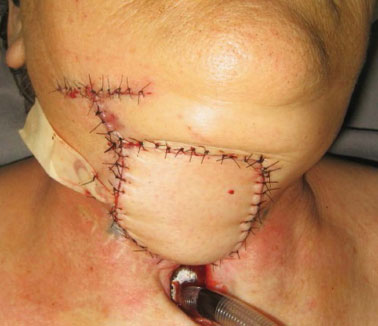
Figure 3. Final intraoperative aspect of the microsurgical reconstruction of the esophagocutaneous fistula.
DISCUSSION
With the development of microsurgical reconstructions, surgical flap success rates are approaching 100%. Hence, the refinement of aesthetic and functional results as well as the reduction of donor site morbidity, have become the major concerns5,7. A microsurgical ALT flap meets these requirements; its extensive application in various fields is based on the following: its reliable vascularization, long and broad vascular pedicle (at least 8 cm long); an extensive and easily delimited flap region; possibility of reducing the primary flap thickness to 3-5 mm without the risk of compromising its vascularization; the possibility of extracting combined flaps that can include the muscle, fascia, and bone; possibility of a simultaneous dual approach because of the distance between donor and recipient sites; and the possibility of primary closure without the need for skin grafting when the width is < 8 cm. Moreover, the donor site is located in a covered area and its motor function is minimally affected1,3,6.
The contraindications for an ALT flap include obesity, arteriosclerosis, and infection8. When there is a risk of infection, one should opt for a myocutaneous flap instead of a skin flap, which is based on septocutaneous or musculocutaneous perforator vessels7. Previous injuries or surgeries with incisions in the lateral thigh region are also a contraindication for the use of the ALT flap1,3,8.
The versatility of the ALT flap makes it especially useful for a heterogeneous group of extensive defects in the soft tissues of the head and neck. This versatility is a consequence of the adaptability and ability to independently remove the muscular component and moderate skin thickness1.
The ALT flap has specific advantages for the reconstruction of the cervical region: it is relatively thin and hairless, the flap pedicle can exceed 10 cm in length and 2 mm in width, and patient repositioning is not required to harvest the flap9.
The case report presented in this study emphasizes the importance of the sandwich ALT flap for correcting high output esophagocutaneous fistula.
REFERENCES
1. Lueg EA. The anterolateral thigh flap: radial forearm's "big brother" for extensive soft tissue head and neck defects. Arch Otolaryngol Head Neck Surg. 2004;130(7):813-8. DOI: http://dx.doi.org/10.1001/archotol.130.7.813
2. Chen HC, Tang YB. Anterolateral thigh flap: an ideal soft tissue flap. Clin Plast Surg. 2003;30(3):383-401. DOI: http://dx.doi.org/10.1016/S0094-1298(03)00040-3
3. Hallock GG. The preexpanded anterolateral thigh free flap. Ann Plast Surg. 2004;53(2):170-3. DOI: http://dx.doi.org/10.1097/01.sap.0000112288.25696.fb
4. Yang JY, Tsai FC, Chana JS, Chuang SS, Chang SY, Huang WC. Use of free thin anterolateral thigh flaps combined with cervicoplasty for reconstruction of postburn anterior cervical contractures. Plast Reconstr Surg. 2002;110(1):39-46. PMID: 12087229 DOI: http://dx.doi.org/10.1097/00006534-200207000-00009
5. Wei FC, Demirkan F, Chen HC, Chuang DC, Chen SH, Lin CH, et al. The outcome of failed free flaps in head and neck and extremity reconstruction: what is next in the reconstructive ladder? Plast Reconstr Surg. 2001;108(5):1154-60.
6. Groth AK, Silva ABD. Reconstrução oromandibular complexa com dois retalhos microcirúrgicos. Rev Bras Cir Plast. 2009;24(1):11-21.
7. Nuara MJ, Sauder CL, Alam DS. Prospective analysis of outcomes and complications of 300 consecutive microvascular reconstructions. Arch Facial Plast Surg. 2009;11(4):235-9. DOI: http://dx.doi.org/10.1001/archfacial.2009.46
8. Kroll SS, Schusterman MA, Reece GP, Miller MJ, Evans GR, Robb GL, et al. Choice of flap and incidence of free flap success. Plast Recontr Surg. 1996;98(3):459-63. DOI: http://dx.doi.org/10.1097/00006534-199609000-00015
9. Aki FE, Besteiro JM, Pinto FR, Durazzo MD, Cunha AS, S Filho GB, et al. Emprego do retalho microcirúrgico antebraquial na reconstrução em cabeça e pescoço: experiência de 11 casos. Rev Assoc Med Bras. 2000;46(2):182-5. DOI: http://dx.doi.org/10.1590/S0104-42302000000200014
1. Faculdade de Medicina do ABC, Santo André, SP, Brazil
2. Sociedade Brasileira de Cirurgia Plástica, São Paulo, SP, Brazil
3. Hospital Estadual Mário Covas, Santo André, SP, Brazil
4. Hospital de Ensino Anchieta, Santo André, SP, Brazil
Institution: Faculdade de Medicina do ABC, Santo André, SP, Brazil.
Corresponding author:
Roberta França Spener
Av. Príncipe de Gales, 821
Santo André, SP, Brazil Zip Code 09061-260
E-mail: robertaspener@hotmail.com
Article received January 22, 2012.
Article accepted March 04, 2012.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter