

Case Report - Year 2015 - Volume 30 -
Transplant of the greater omentum for reconstruction of a complex hand injury
Transplante de grande omento para reconstrução de lesão complexa na mão
ABSTRACT
The greater omentum, a large fold of the peritoneum, can be used as a free flap in numerous procedures due to the extensive network of its broad vascular pedicle and its versatility when manipulated. In this case report, we present a patient with a complex degloving injury, in which an omental flap was the best therapeutic option for reconstruction of the hand. The greater omental flap is a viable option for complex lesions of the hand, and provides good coverage of the lesion and good functional and aesthetic results.
Keywords: Hand injuries; Plastic surgery; Microsurgery.
RESUMO
O grande omento, uma larga prega de peritônio, pode ser usado como retalho livre em numerosos procedimentos devido à vasta e calibrosa rede de seu pedículo vascular e à sua versatilidade para ser manipulado. Neste relato de caso, nós apresentamos um paciente vítima de complexa lesão de desenluvamento, cujo retalho de grande omento se provou como a melhor opção para a reconstrução da mão dentre as outras opções terapêuticas. O retalho de grande omento é uma opção viável para lesões complexas da mão, oferecendo boa cobertura da lesão e bom resultado funcional e estético.
Palavras-chave: Traumatismos da mão; Cirurgia plástica; Microcirurgia.
The reconstruction of extensive skin losses in the hand is challenging for plastic surgeons, in view of the specific characteristics of the skin of the dorsum, which is mobile and has thin subcutaneous cellular tissue. The skin of the volar region also has peculiar characteristics: it is thick, with adipose pads and specific areas of skin folds that enable articulation and secure the structure, allowing stable prehension. Minor losses may be technically resolved using rotational forearm flaps, such as the Chinese flap or the posterior interosseous artery flap. Grafts satisfactorily resolve losses of the dorsum when subcutaneous cellular or paratendon tissue there is preserved; however, for the volar region, owing to the absence of melanin in this area, these grafts can be stigmatizing. In patients who sustain loss of a large mass of tissue, it becomes increasingly difficult to resolve such problems.
For these types of injuries, the use of the greater omental flap with partial-thickness skin grafts is indicated in the literature. The present case was reported because of the degree of severity of the lesion presented and the outcome obtained using the greater omentum1-4.
Surgical Anatomy
The greater omentum is a fold of the peritoneum attached to the greater curvature of the stomach and the proximal portion of the duodenum that descends on the abdominal viscera and, after folding in itself, is attached on the anterior surface of the transverse colon and its mesentery. Besides being rich in vascular and lymphatic structures, it has abundant lobular adipose tissue. It has a protective function against mechanical injury of intra-abdominal components that is usually exercised by wrapping around inflamed areas, and is also involved in the maintenance of body temperature. It receives blood supply via the right and left gastroepiploic arteries, from which the left, middle and right omental arteries originate2,3,5,6.
The characteristics described above make this flap an extremely versatile option for reconstructive surgery. The use of the omental flap has already been described for the coverage of thoracic injury, for the treatment of lymphedema, for the reduction of dead space, for the revascularization of the brain and spinal cord, and to restore loss of substance in surgeries of the face and the skull and repair of the lower limbs1-4.
Thus, we present the use of the greater omentum for reconstruction of a complex hand injury.
CASE REPORT
A 25-year-old male laborer with dark skin type, with no history of injury in the upper limb, experienced trauma in the hand during handling of a press at high temperatures in a cardboard factory.
In emergency primary care, the patient sustained the following injuries: total degloving of the hand, exposure of all the flexor and extensor tendons and all of the carpal and metacarpal bones, and phalangeal amputation by avulsion of all fingers. The radiological examination showed total avulsion of the third and fifth fingers, crushing with amputation of the first, second and fourth fingers, and carpometacarpal fracture dislocation of the second, third, fourth and fifth fingers. In primary care, surgical debridement was performed, and after this, the reconstruction of the limb was planned with the aim to cover the lesion by using a thin and flexible tissue enough to yield a compound grasp from the remainder of the proximal phalanx of the thumb and the stump of the proximal index phalanx (Figures 1 and 2).
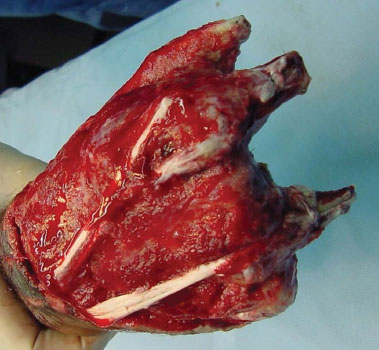
Figure 1. Pre-operative aspect of the dorsal surface. Note the degree of amputation and exposure of tendons.
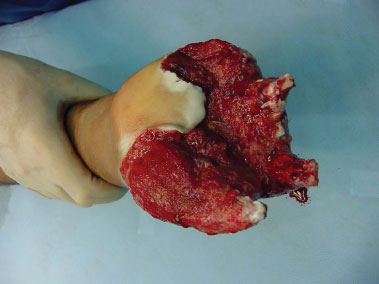
Figure 2. Pre-operative aspect of the volar surface. Note the degree of amputation.
As such, in the second operation, fractures were fixed using transmedullar Kirschner wires, and a flap derived from the greater omentum was transposed to the dorsum, volar area, and stumps of the proximal phalanges of the first and second fingers. Anastomosis of the gastroepiploic vessels with the radial artery and cephalic vein was performed (Figure 3).
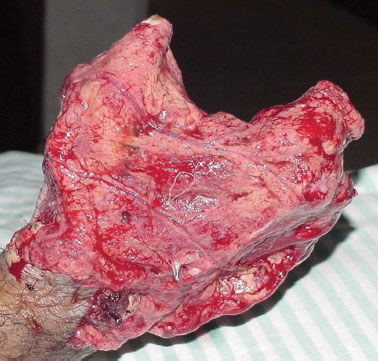
Figure 3. Transplanted omental flap. Detail of the free flap of greater omentum after the second surgical time.
In the third operation, after stabilization of the aforementioned flap in the desired areas and the restoration of adipose pads, partial skin grafting from the thigh was performed.
When the grafts were healed, the fourth operation was performed, which consisted of reducing the amount of fat and deepening the first interdigital space. The postoperative period was uneventful, and after surgery, the patient was referred for physical therapy and functional rehabilitation.
RESULTS
A successful outcome was achieved with the treatment reported in this case, as the deepening of the first interdigital groove was achieved, whilst maintaining adduction function and extension of first metacarpal joint, which enabled lateral pinching. This result and the maintenance of the length of the right upper limb allowed the patient to restart work (Figures 4 and 5).
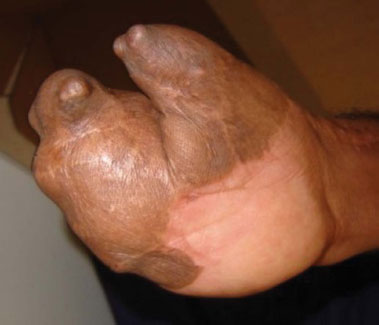
Figure 4. Post-operative period. Detail of the volar surface and lateral pinch after full integration of skin grafts.
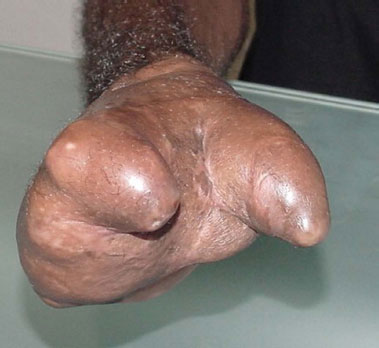
Figure 5. Late postoperative period. Full integration of skin grafts and oblique view of the pinch in the first interdigital space
DISCUSSION
For reconstruction of the hand, the surgeon should consider many aspects. The complex interactions between tendons, ligaments, bones and skin that promote refined movements of the hand should be taken into account when treating injuries such as the one presented herein.
There are few reported cases of degloving lesions with crushing and avulsion of all fingers as shown here. In the English literature, a review by Tutkus et al.7 showed no cases of avulsion as complex as the one reported here. The majority of lesions fully recovered with established flaps such as the large dorsal flap, but in lesions of greater complexity and extension, the few cases reported were satisfactorily reconstructed by using the greater omentum as a flap to recover volume lost in the injury1-3.
There are several types of flaps designed to cover injuries of the hand, such as the posterior interosseous flap, the Chinese antebrachial flap, the free muscle flap (latissimus dorsi flap), and the temporal fascia free flap. All of these flaps are extremely useful for covering injuries to the hand, but often provide a large volume that hinders finger movement. Even if procedures for the reduction of this volume are carried out, they are limited by local blood supply8.
The size of the lesion presented and the objective of recovering lateral pinching created the need for a large yet flexible flap. The latissimus dorsi muscle flap is an option, but this would be much more voluminous and impose technical complications for refinement, which could be easily avoided by using the greater omentum1,3. In addition, the lobular configuration of the omental fat could be used to rebuild the fat layer of the fingers, simulating the digital pulp and provided a sliding surface between the tendons and the skin graft.
The vascular pedicle of the greater omentum is also advantageous. Its versatility has been described in various types of procedures in which revascularization was required1-4,6,7,9. It has several large caliber secondary veins, which can serve as a source for venous grafts in complex lesions of the hand with vascular impairment and indications for revascularization6.
Nevertheless, there are disadvantages in harvesting this flap. The harvest of the flap through laparotomy presents complications inherent in this surgical procedure. Owing to the lower incidence of sequelae to the abdominal wall and the lower possibility of complications, some authors have suggested a laparoscopic procedure3,8,9. To prevent gastric volvulus, nasogastric intubation should be maintained for a week10.
For covering the greater omentum flap, using a skin autograft was the most viable option; however, synthetic skin substitutes are emerging, which may be economically viable alternatives in the future. Some of these serve as dressings to the injured area, and promote invasion of fibroblasts and keratinocytes. Ongoing studies are assessing the effectiveness of these methods and their main indications11.
As an option for covering injuries to the hand, the omentum should not be seen as a panacea and should be accurately indicated in order to obtain good results. Lesions caused by avulsion or crushing are the primary indications for these flaps.
REFERENCES
1. McLean DH, Buncke HJ Jr. Autotransplant of omentum to a large scalp defect, with microsurgical revascularization. Plast Reconstr Surg. 1972;49(3):268-74. PMID: 4551236 DOI: http://dx.doi.org/10.1097/00006534-197203000-00005
2. Erol OO, Spira M. Development and utilization of a composite island flap employing omentum: experimental investigation. Plast Reconstr Surg. 1980;65(4):405-18. DOI: http://dx.doi.org/10.1097/00006534-198004000-00003
3. Seitz IA, Williams CS, Wiedrich TA, Henry G, Seiler JG, Schechter LS. Omental free-tissue transfer for coverage of complex upper extremity and hand defects--the forgotten flap. Hand (N Y). 2009;4(4):397-405. DOI: http://dx.doi.org/10.1007/s11552-009-9187-6
4. Tavares FMO, Meneses CMGG, Moscozo MVA, Xavier GRS, Oliveira GM, Paiva MA, et al. Retalho de Omento: uma alternativa em cirurgia reparadora da parede torácica. Rev Bras Cir Plástica. 2011;26(2):360-5. DOI: http://dx.doi.org/10.1590/S1983-51752011000200028
5. Moore KL, Dalley AF. Anatomia orientada para a clínica. 5a ed. Rio de Janeiro: Guanabara Koogan; 2007. p.179-326.
6. Ferrigno CRA, Ito KC, Caquias DFI, Mariani TC, Della Nina MI, Ferraz VCM, et al. Retalho de omento maior para indução de vascularização e consolidação óssea em cão. Ciênc Rural. 2010;40(9):2033-6. DOI: http://dx.doi.org/10.1590/S0103-84782010000900029
7. Tutkus V, Vitkus K, Proskute D. Use of the omental free flap for reconstruction of degloving hand and foot injuries: two case reports. Cent Eur J Med. 2012;7(6):808-12. DOI: http://dx.doi.org/10.2478/s11536-012-0075-z
8. Rocha JR, Bijos P. Retalhos Microcirúrgicos para a Mão. In: Melega JM, Viterbo F, Mendes FH, Eds. Cirurgia Plástica: Os princípios e a atualidade. Rio de Janeiro: Guanabara Koogan; 2011. p.869-75
9. dos Santos Costa S, Blotta RM, Mariano MB, Meurer L, Edelweiss MI. Aesthetic improvements in Poland's syndrome treatment with omentum flap. Aesthetic Plast Surg. 2010;34(5):634-9. PMID: 20419302 DOI: http://dx.doi.org/10.1007/s00266-010-9513-y
10. Bento A, Baptista H, Pinheiro C, Pinho A, Lopes S, Martinho F. Volvo Gástrico: caso clínico. J Port Gastrenterol. 2010;17(5):223-6.
11. Ferreira MC, Paggiaro AO, Isaac C, Teixeira Neto N, Santos GB. Substitutos cutâneos: conceitos atuais e proposta de classificação. Rev Bras Cir Plást. 2011;26(4):696-702. DOI: http://dx.doi.org/10.1590/S1983-51752011000400028
1. Universidade Federal do Ceará, Fortaleza, CE, Brazil
2. Sociedade Brasileira de Cirurgia Plástica, Fortaleza, CE, Brazil
3. Comissões Estaduais de Residência Médica, Fortaleza, CE, Brazil
4. Instituto Dr. José Frota, Fortaleza, CE, Brazil
5. Universidade Estadual do Ceará, Fortaleza, CE, Brazil
Institution: Universidade Federal do Ceará, Fortaleza, CE, Brazil.
Corresponding author:
Salustiano Gomes de Pinho Pessoa
Rua Andrade Furtado, 1591, Cocó
Fortaleza, CE, Brazil Zip Code 60192-072
E-mail: salustianogomes@uol.com.br
Article received March 07, 2014.
Article accepted January 28, 2014.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter