

Original Article - Year 2015 - Volume 30 -
Complex reconstruction of the upper and lower limbs by using reverse-flow flaps: a series of 32 cases
Reconstruções complexas de membros superiores e inferiores com retalhos de fluxo reverso: uma série de 32 casos
ABSTRACT
INTRODUCTION: Reconstruction of the soft tissues after loss of substance in the distal third of the upper and lower limbs, in particular when associated with the exposure of noble structures (bone, tendon, nerves, or blood vessels), remains a challenge in plastic surgery. Fasciocutaneous reverse flow flaps are an efficient surgical option for covering small and medium lesions in this location.
METHOD: A retrospective clinical study was performed on a series of 32 cases of complex trauma of the upper and lower limbs treated between January 2013 and December 2014.
RESULTS: A total of 24 reverse-flow flaps were performed in the lower limbs and eight in the upper limbs, resulting in efficient coverage of the defects.
CONCLUSION: Reverse-flow flaps are reliable and present rotation arcs that allow coverage of a variety of lesions in the distal third of the upper and lower limbs.
Keywords: Surgical flaps; Reconstructive surgical procedures; Hand trauma; Lesion of the soft tissues; Leg trauma/surgery.
RESUMO
INTRODUÇÃO: A reconstrução de partes moles após perdas de substância do terço distal dos membros superiores e inferiores, principalmente quando associada à exposição de estruturas nobres (osso, tendão, nervos ou vasos sanguíneos), continua a desafiar a cirurgia plástica. Os retalhos fasciocutâneos de fluxo reverso são uma eficiente opção cirúrgica na cobertura de lesões pequenas e médias nesta localização.
MÉTODO: Foi realizado um estudo clínico retrospectivo, no período de janeiro de 2013 a dezembro de 2014, de uma série de 32 casos de traumas complexos em membros superiores e inferiores.
RESULTADOS: Foram realizados 24 retalhos de fluxo reverso nos membros inferiores e 8 nos membros superiores, observando-se uma cobertura eficaz dos defeitos.
CONCLUSÃO: Os retalhos de fluxo reverso são confiáveis e apresentam arcos de rotação que permitem a cobertura de lesões diversas no terço distal de membros superiores e inferiores.
Palavras-chave: Retalhos cirúrgicos; Procedimentos cirúrgicos reconstrutivos; Traumatismos da mão; Lesões dos tecidos moles; Traumatismos da perna/cirurgia.
The reconstruction of soft tissues after loss of substance in the distal third of the upper and lower limbs, with exposure of noble structures (bone, tendon, nerves, or blood vessels), remains a challenge in plastic surgery. Few options are available for treating these regions with flaps; in most cases, microsurgical flaps are used1-3.
Since the work of Pontén in 1981, fasciocutaneous flaps have become an alternative to microsurgical flaps, since the latter require the use of a specialized team and a long surgery time. The distal position of some lesions in the upper and lower limbs hinders or makes the application of direct-flow flaps impossible. Reverse arterial flow is maintained via arterial anastomosis at the fist and ankle level. However, another type of flow to consider is the venous flow, which is obtained through the pressure gradient of valvular insufficiency itself, by the communicating capillaries and collateral veins and by valve denervation during the release of a vascular pedicle4-9.
Fasciocutaneous reverse-flow flaps are useful for covering small and medium-sized lesions in the distal third of the limbs, with mild functional and aesthetic sequelae and less surgical time. These are an efficient surgical option because of the ease of execution, safety, and versatility4.
OBJECTIVE
The objective of the study was to demonstrate the technical viability and results of a series of complex reconstructions of the soft tissues in the distal third of the upper and lower limbs by using reverse-flow flaps.
METHOD
A retrospective clinical study was performed on a consecutive case series of complex trauma in the upper and lower limbs treated between January 2013 and December 2014. Thirty-two reverse-flow flaps were performed for limb reconstruction.
The inclusion criteria were patients presenting with skin loss after trauma leading to the exposure of noble structures (bone, tendon, nerves, or vessels) in the distal upper and lower limbs. The following parameters were studied: sex, age, etiology, location of the lesion, repair procedure, and complications. The choice of flaps was based on the study of defect, location, and quantity and quality of the required tissues. This study was approved by the Ethics Committee of the Walter Cantídio University Hospital, under protocol nº 043.04.15°.
RESULTS
In this case study, 81.2% of patients were men aged 18 to 52 years (mean age of 26 years). Most trauma cases (87.5%) were caused by motorcycle accidents.
Twenty-four reverse-flow flaps were performed in the lower limbs, including 14 sural flaps, 8 lateral supramalleolar flaps, and two reverse soleus flaps. Eight reconstructions were performed in the upper limbs, including 5 antebrachial reverse flaps and 3 posterior reverse-flow interosseous artery flaps.
We observed efficient coverage of the defects in upper and lower limbs. Additionally, we observed one case each of total necrosis of a sural flap due to venous thrombosis, total necrosis of a lateral supramalleolar flap, partial necrosis of a reverse sural flap, and partial necrosis of a lateral supramalleolar flap. The surgical time ranged between 60 and 120 minutes with low morbidity in the donor area.
DISCUSSION
Loss of substance in the lower third of the leg due to trauma caused by crushing, with the exposure of noble structures, is difficult to treat.
The reverse-flow sural fasciocutaneous flap is important for use in the reconstruction of loss of substance in the distal third of leg, calcaneus, and proximal plantar region. It comprises of a versatile flap with a wide rotation arc, and ranges from 90º-180º. Moreover, it has an axial pattern based on the reverse flow of the fibular branch of the superficial sural artery and primary venous drainage via the sural tributaries of the small saphenous vein. The reverse-flow sural flap is a good option for covering important structures, such as bones or tendons in the distal region of leg, and is one of the few alternatives available for local flaps in this region. This flap is utilized as a viable option even with a microsurgical technique since it involves a simple and quick surgical procedure when compared to microsurgery3,7,8,10-12. In the present case series, one sural flap showed total necrosis due to venous thrombosis (7.14% of reverse sural flaps) and one flap showed partial necrosis (7.14% of sural flaps). The literature report a rate of 3.3-19% for total necrosis of flaps, with 11-17% for partial necrosis12 (Figure 1).
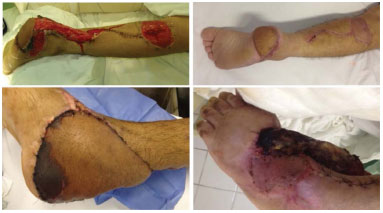
Figure 1. A patient with skin loss in the calcaneus who underwent reconstruction with a sural reverse-flow flap. The patient with partial necrosis of the sural flap. The patient with total necrosis of the flap.
The lateral supramalleolar flap is used to cover skin loss on the dorsal region of the foot and the distal third of the leg. It is based on an arterial arc anastomosis around the ankle with the perforating branches of the fibular artery, which emerge from the interosseous membrane at approximately 5 cm of the lateral malleolus. These anastomoses branch out into the skin at this level and anastomose with the plexus that follows the superficial fibular nerve, in turn involving the septocutaneous territory of the anterior tibial artery. The advantage of this type of flap is the preservation of arteries and muscles, in addition to the simulation of thickness, texture, pigmentation, and flexibility of skin in the recipient area4. In this study, we performed eight (25% of flaps) lateral supramalleolar flaps with one total loss (12.5% of supramalleolar flaps) and one partial loss; the cause of loss of the flap was not determined (Figure 2).
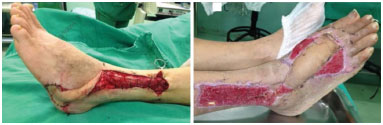
Figure 2. Two patients with skin loss in the lateral plantar surface and dorsal foot who underwent reconstruction using the reverse-flow supramalleolar flap.
The soleus muscle is located in the posterior region of the leg, deep to the gastrocnemius muscle, and classified as Type II according to the Mathes and Nahai classification. The reverse soleus muscle flap has irrigation based in the secondary pedicles with perforating branches of the posterior tibial artery, and it has been used for the reconstruction of defects in the lower third of leg5. In the present case study, we performed two reverse-flow soleus flaps with good coverage of the defect, and skin grafting was subsequently performed over the muscle without complications (Figure 3).
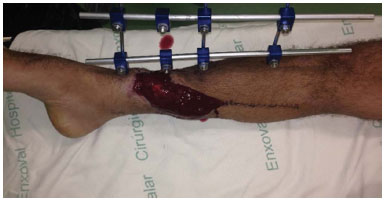
Figure 3. Reconstruction of skin loss with exposure of the tibia using the reverse soleus muscle flap.
Skin covering for complex distal lesions of the upper limbs is a challenge in reconstructive plastic surgery. The antebrachial reverse flap is based on the perforating branches of radial artery. This flap was shown to be very useful for tegumentary covering of the upper limb, in particular of the hands; the retrograde flow flap is most widely used for the repair of distal lesions6,13. It has the disadvantage of sacrificing one of the hand arteries, in addition to a poor aesthetic result at the donor area13. In the present case series, we performed five (15.6% of the studied cases) antebrachial reverse-flow flaps used for covering the skin losses in the dorsal hand with the exposed bone and tendon; No complications were associated with the use of this flap, and the donor area was grafted (Figure 4).
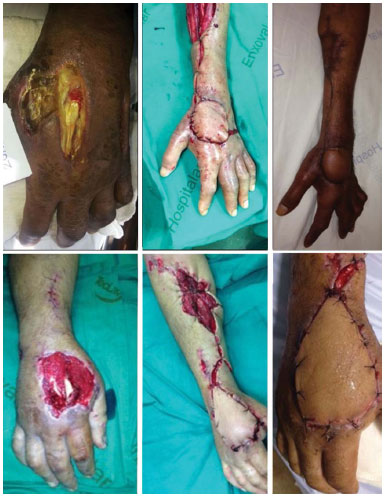
Figure 4. Two patients with skin loss in the dorsal hand who underwent reconstruction using the antebrachial reverse-flow flaps.
The fasciocutaneous island flap is based on the posterior interosseous artery. This artery is usually a branch of the common interosseous artery, the reverse flow being based on anastomosis with the anterior interosseous artery and venous drainage via the concomitant and superficial veins contained in the pedicle. This flap is a safe and efficient choice, and is recommended for lesions of the distal third of forearm, dorsum of the wrist and hand, and the first commissure of the thenar region, and it provides a stable cover without sacrificing the main arteries of hand irrigation. The donor area demonstrates minimal morbidity, and is closed with a primary suture or a skin graft7,9,14. In the present study, we had three cases (9.3% of total) of posterior interosseous reverse-flow flap for lesions in the distal region of the forearm and hand, and found no complications (Figure 5).
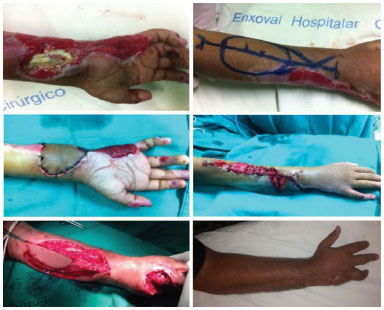
Figure 5. Two patients with skin loss in the proximal third of forearm and dorsal hand who underwent reconstruction using the posterior interosseous reverse-flow flap.
CONCLUSION
Reverse-flow flaps are reliable and safe, and present rotation arcs that allow coverage of various lesions in the distal third of the upper and lower limbs. Therefore, their application is an alternative to microsurgical flaps, even for complex lesions, since they can be performed at centers without technical and laboratory resources required for the microsurgery.
REFERENCES
1. Belém LFMM, Lima JCSA, Ferreira FPM, Ferreira EM, Penna FV, Alves MB. Retalho sural de fluxo reverso em ilha. Rev Soc Bras Cir Plást. 2007;22(4):195-201.
2. Souza FI, Saito M, Torres LR, Wei TH, Mattar Júnior R, Zumiotti AV. Estudo anatômico do retalho lateral do braço de fluxo reverso. Acta Ortop Bras. 2010;18(1):39-43. DOI: http://dx.doi.org/10.1590/S1413-78522010000100008
3. Vendramin FS. Retalho sural de fluxo reverso: 10 anos de experiência clínica e modificações. Rev Bras Cir Plást. 2012;27(2):309-15. DOI: http://dx.doi.org/10.1590/S1983-51752012000200023
4. Batista JC. Retalho supramaleolar de fluxo reverso: aplicações clínicas. Rev Bras Cir Plást. 2011;26(1):140-6. DOI: http://dx.doi.org/10.1590/S1983-51752011000100025
5. Souza Filho MVP, Teixeira JCEO, Castro OC. Retalho hemissolear reverso na reconstrução de defeito do terço distal da perna. Rev Bras Cir Plást. 2011;26(4):710-3. DOI: http://dx.doi.org/10.1590/S1983-51752011000400031
6. Scozzafave GAE, Abel JL, Bloch RJ, Andreoni WR, Pastro DA, Miranda FBS, et al. Aplicações clínico-cirúrgicas do retalho antebraquial: análise de 89 casos. Rev Bras Cir Plást. 2010;25(2):361-6.
7. Lima SJ, Costa RPD, Oliveira E, Prudente FG, Mendonça MP, Camargo CS. Retalho da artéria interóssea posterior na cobertura das lesões graves do antebraço, punho e mão. Rev Bras Ortop. 2009;44(1):40-5. DOI: http://dx.doi.org/10.1590/S0102-36162009000100006
8. Almeida MF, da Costa PR, Okawa RY. Reverse-flow island sural flap. Plast Reconstr Surg. 2002;109(2):583-91. DOI: http://dx.doi.org/10.1097/00006534-200202000-00027
9. Cheema TA, Lakshman S, Cheema MA, Durrani SF. Reverse-flow posterior interosseous flap-a review of 68 cases. Hand (N Y). 2007;2(3):112-6. DOI: http://dx.doi.org/10.1007/s11552-007-9031-9
10. Ip KC, Lee KB, Shen WY. The use of a reverse flow sural fasciocutaneous flap in a patient with multiple trauma: a case report. J Orthop Surg (Hong Kong). 2008;16(3):373-7.
11. Mahboub T, Gad M. Increasing versality of reverse-flow sural flap in distal leg and foot reconstruction. Egypt J Plast Reconstr Surg. 2004;28(2):99-112.
12. Ajmal S, Khan MA, Khan RA, Shadman M, Yousof K, Iqbal T. Distally based sural fasciocutaneous flap for soft tissue reconstruction of the distal leg, ankle and foot defects. J Ayub Med Coll Abbottabad. 2009;21(4):19-23.
13. Maamoun MI, Rizk IN, Minawi HME, Moharram AN. Adipofascial Perforator Based Reversed Flow Radial Forearm Flap for the Reconstruction of Hand Defects. Kasr El Aini J Surg. 2007;8(1):55-62.
14. Shahzad MN, Ahmed N, Qureshi KH. Reverse flow posterior interosseous flap: experience with 53 flaps at Nishtar Hospital, Multan. J Pak Med Assoc. 2012;62(9):950-4.
1. Sociedade Brasileira de Cirurgia Plástica, São Paulo, SP, Brazil
2. Hospital Universitário Walter Cantídio da Universidade Federal do Ceará, Fortaleza, CE, Brazil
3. Instituto Dr. José Frota, Fortaleza, CE, Brazil
Institution: Universidade Federal do Ceará, Fortaleza, CE, Brazil.
Corresponding author:
Caio Alcobaça Marcondes
Rua Luiza Amelia Brandão, 916, São Cristovão
Teresina, PI, Brazil Zip Code 64056-170
E-mail: caio_alcobaca@hotmail.com
Article received: April 17, 2015.
Article accepted: October 8, 2015.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter