

Original Article - Year 2016 - Volume 31 -
Transconjunctival lower blepharoplasty with skin resection and preservation of the orbicularis muscle
Blefaroplastia inferior transconjuntival associada à ressecção cutânea com preservação do músculo orbicular
ABSTRACT
INTRODUCTION: Transconjunctival lower blepharoplasty is increasingly used by surgeons, since it is reproducible and has a low rate of complications compared to transcutaneous technique. The advantage of the transconjunctival technique is the preservation of the orbital septum, middle lamella, and orbicularis muscle innervation. This study aims to assess the results and complications of transconjunctival blepharoplasty with skin resection in the lower eyelid without detachment.
METHOD: Eighteen patients who underwent this surgery with or without lateral canthopexy were analyzed. The surgical technique is described in detail.
RESULTS: A total of 16 female and 2 male patients were assessed, with an average age of 52.7 years. There was improvement in all cases in the appearance of increased volume in the lower eyelid, and a decrease in skin and lateral ligament laxity. Late complications such as eyelid retraction, ectropion, unaesthetic scars, diplopia, or remnant fat bags were not observed. Surgical reintervention was not required in any cases.
CONCLUSION: Transconjunctival lower blepharoplasty with skin resection without detachment and with preservation of the orbicularis muscle, with or without canthopexy, is an excellent technique, and is easily reproducible, reliable, and safe, with few postoperative complications in treatment of age-related changes in the lower eyelids.
Keywords: Blepharoplasty; Eyelids; Eyelids/Pathology; Lacrimal apparatus; Reconstructive surgical procedures.
RESUMO
INTRODUÇÃO: A blefaroplastia inferior transconjuntival está cada vez sendo mais utilizada pelos cirurgiões por ser uma técnica reprodutível e com baixo índice de complicações quando comparada à via transcutânea. Esta técnica tem como vantagens em relação à transcutânea a preservação do septo orbital, da lamela média e a manutenção da inervação do músculo orbicular. Este estudo tem o objetivo de analisar os resultados e as complicações da blefaroplastia transconjuntival com ressecção de pele na pálpebra inferior sem descolamento em uma amostra de pacientes.
MÉTODO: Foram avaliados 18 pacientes submetidos a esta cirurgia, associada ou não à cantopexia lateral. A técnica cirúrgica é descrita detalhadamente.
RESULTADOS: Um total de 16 pacientes femininos e 2 masculinos foram avaliados, com idade média de 52,7 anos. Houve melhora do aspecto do aumento de volume da pálpebra inferior, da flacidez de pele e da flacidez ligamentar lateral em todos os casos. Não foram registradas complicações tardias como retrações palpebrais, ectrópio, cicatrizes inestéticas, diplopia ou bolsas gordurosas remanescentes. Em nenhum caso foi necessária reintervenção cirúrgica.
CONCLUSÃO: A blefaroplastia inferior transconjuntival com ressecção cutânea sem descolamento e preservação do músculo orbicular, associada ou não à cantopexia, se mostrou uma excelente técnica, facilmente reprodutível, confiável, segura e com poucas complicações pós-operatórias para o tratamento das alterações senis das pálpebras inferiores.
Palavras-chave: Blefaroplastia; Pálpebras; Pálpebras/Patologia. Aparelho lacrimal; Procedimentos cirúrgicos reconstrutivos.
Transcutaneous blepharoplasty has long been the most common technique used by surgeons in the approach to fat bags and lower eyelid skin, despite the fact that several authors reported high rates of eyelid malposition and functional deficits using this technique1-3. Transconjunctival lower blepharoplasty was first described by Bourget in 19244 and popularized by Tessier, who conducted work associated with genetic malformations5. This technique has been improved over the years and gained greater popularity when authors such as Zarem and Resnick reported that transconjunctival blepharoplasty showed lower rates of postoperative complications than the classic transcutaneous technique6,7.
Isolated transconjunctival lower blepharoplasty is highly recommended for young patients with herniated fat bags without skin redundancy, or for revision in secondary blepharoplasty in cases with residual eye bags8,9. In patients with excess skin in the lower eyelids, in addition to fat bags, the skin can be treated separately through a skin pinch and resection without skin detachment, (skin-pinch), maintaining the integrity of the orbicularis muscle, its innervation, and the middle lamella10.
Several authors describe a combined transconjunctival approach for fat bags with the skin pinch technique for the lower eyelid and call this the "no-touch" or "no-flap" technique11-13. If required, this surgery can also be complemented with treatments for lateral ligament laxity and adequate palpebral support, such as canthopexy and canthoplasty14-18. This combination of techniques is becoming more popular among surgeons, who have observed lower morbidity through the preservation of the middle lamella and innervation of the orbicularis muscle and lower risk of complications related to eyelid surgery as compared to those in the transcutaneous technique19.
The aim of this study was to analyze the results and complications of transconjunctival blepharoplasty with skin pinch and resection in the lower eyelid, without skin detachment, and with preservation of the orbicularis muscle ("no-touch technique") in a series of patients with 2 years of postoperative follow-up.
METHOD
Eighteen patients who underwent transconjunctival lower blepharoplasty with skin pinch and resection of the lower eyelid, with or without lateral canthopexy, were assessed. The technique used is described in detail. The patients underwent surgery by the same surgeon at the Hospital da Plástica de Santa Catarina in Florianópolis from April 2012 to April 2014. The inclusion criterion was surgical indication for the technique; there were no exclusion criteria. The study was conducted according to the Helsinki Declaration and the patients provided signed informed consent.
The detailed preoperative evaluation included an interview to collect information about past clinical and ophthalmological history, and a physical examination. Patients with a history of dry eyes or laser-assisted in situ keratomileusis (LASIK) surgery underwent a Schirmer test. Lower eyelid tone was also examined by using the snap test, comprised of lifting the eyelid from the eyeball and observing its position. In cases where the distance is greater than 5 mm, with horizontal tarsal laxity and/ or a negative vector, lateral canthopexy is indicated to minimize the risk of postoperative malposition of the lower eyelid (this technique was used, and is also described below). Relevant findings noted in preoperative records included the presence of scleral show, malar hypoplasia, festoons, entropion, ectropion, etc. The amount and extent of herniated periorbital fat bags and skin excess were also assessed during physical examination for adequate surgical planning. Pre- and postoperative pictures were taken at various angles to document the cases, and informed consent was obtained from all patients before the procedures.
Surgical technique
The procedures were performed in a hospital environment under general or local anesthesia and sedation. Corneal protectors were positioned with ophthalmic ointment. Infiltration was performed in the lower conjunctiva, in the medial, median and lateral fat bags, and the lower eyelid skin using a 2% lidocaine and epinephrine 1:100,000 solution (Figure 1).
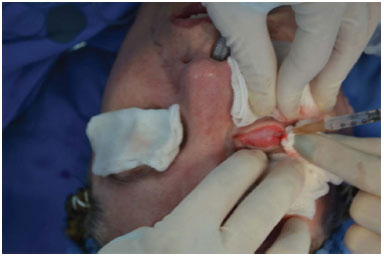
Figure 1. Infiltration of the lower conjunctiva, fat bags, and lower palpebral skin with a 2% lidocaine and epinephrine 1:100,000 solution.
A horizontal 3-4-mm conjunctival incision with retroseptal access was made in the lower tarsal plate, at the level of the second vascular arcade with a delicate electrocoagulation tip. This approach allows access to the fat bags without breaching the orbital septum. The dissection continued through Müller's muscle and the capsulopalpebral fascia (lower eyelid retractors), with the middle lamella kept intact. A Desmarres lid retractor was placed and gentle downward pressure was applied to the eyeball by the assistant, exposing the herniated periorbital fat in the following order: medial, median, and lateral (Figure 2).
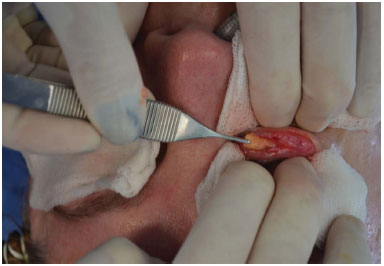
Figure 2. A horizontal conjunctival incision and access to the fat bags without injury to the orbital septum.
These were independent and previously contained by the orbital septum. The bags were identified, gently grasped with hemostatic forceps, and resected with electrocoagulation, making sure that there was no subjacent bleeding. It is important to exercise care in order to avoid damaging the lower oblique muscle located between the medial and median fat bags, which would cause diplopia. The lateral bag is generally less easily herniated and more difficult to resect because it is attached by adjacent fascia to Lockwood's ligament20. Hemostasis was then performed and the conjunctiva was brought together without suturing.
The lower eyelid skin was raised using an Adson-Brown forceps. The skin was pinched to create a thin strip of skin alone, close to the ciliary margin (Figure 3). The skin was excised with a delicate iris scissors, extending up to 2 to 3 mm laterally to the lateral corner (Figure 4). During the resection, it is important to maintain lateral and not anterior tension, in order to avoid excessive skin resection or damage to the orbicularis muscle. Continuous suturing was performed with a 6.0 mono-nylon thread in the lower eyelid skin.
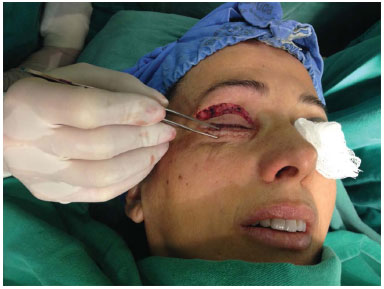
Figure 3. The skin is pinched to create a thin strip of skin alone, very close to the ciliary margin.
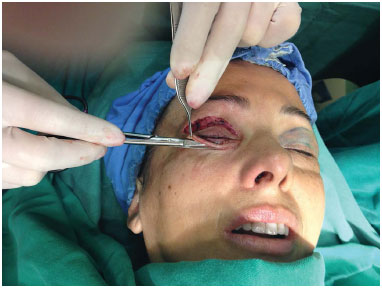
Figure 4. The skin is excised with a delicate iris scissors, extending up to 2 to 3 mm laterally to the lateral corner.
In patients with an indication for canthal support because of lateral tarsal ligament laxity, canthopexy of the lateral retinaculum with muscle suspension was performed without cantholysis. This procedure was performed with a 5.0 mono-nylon suture that passed through the inferolateral portion of the preseptal orbicularis muscle and lateral retinaculum, suspending these structures to a fixed shield, which is the periosteum of the superolateral orbital rim. The needle exits through the incision in the upper eyelid, where it grasps the periosteum and travels in the direction of the skin incision of the lower eyelid. When returned in the direction of the periosteum, the suture grasps the lower branch of the lateral canthal ligament, and then a knot is made with overcorrection of the lower eyelid 1 to 2 mm past the limbus16 (Figure 5). This technique is useful for cases of mild to moderate laxity.
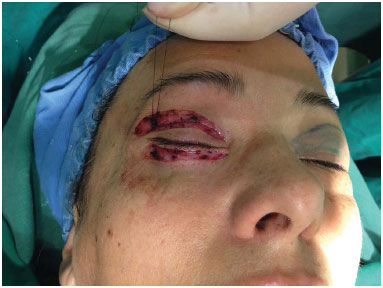
Figure 5. Canthopexy of the lateral retinaculum with muscle suspension without cantholysis.
Other types of canthopexy or canthoplasty may be performed depending on the eyelid laxity grading; however, in this study, all patients who required ligament reinforcement presented mild to moderate laxity and only underwent this canthopexy technique.
After the surgical procedure, the patient was treated with cold compresses, raised head support, eye drops and lubricant gel, prophylactic oral antibiotics, and painkillers.
RESULTS
A total of 18 patients were assessed in this study (16 females and 2 males), with age ranging from 32 to 78 years (average 52.7). All patients were discharged from the hospital within 24 hours, and the postoperative follow-up ranged from 1 to 24 months, with an average of 12.4 months. In all cases, surgery was performed in association with other procedures, such as upper blepharoplasty (UB) (94.4%), cervical lifting (CL) (44.4%), frontal and middle-third video-surgery (VFTM) (16.6%), rhinoplasty (R) (5.5%), and mini-abdominoplasty (MA) with liposuction (L) (5.5%) (Table 1).
In one case, secondary surgery was performed due to remnant fat bags (primary surgery was performed by a different surgeon). Primary surgery was performed in the remaining 17 patients.
The most common clinical comorbidity was systemic arterial hypertension (SAH) in 4 patients. One was an active smoker and another was seropositive. Preexisting palpebral changes such as ectropion, entropion, and scleral show were not observed in any of the patients. There were no cases of previous LASIK surgery and no history of dry eyes. Mild to moderate eyelid laxity was observed in 15 patients (83.3%), and canthopexy was performed in these cases (technique as described above) to prevent postoperative eyelid malposition. Severe eyelid laxity cases were not observed.
Pre- and postoperative aesthetic evaluation was performed using anteroposterior and profile photos, which revealed satisfactory results in all cases. There was improvement in the appearance of increased volume in the lower eyelid due to herniated fat bags, improvement in skin laxity in the lower eyelid, and improvement in lateral ligament laxity in all cases.
In the early postoperative period, common findings were the presence of corneal abrasion (foreign body sensation), lacrimation, and chemosis (33.3%) that resolved in a few days with the use of lubricants. Temporary periorbital edema and ecchymoses were also observed in 83.3% of cases.
In one case, presence of a conjunctival pedicle was observed (due to malposition of the conjunctival scar), but was easily excised at the outpatient stage using an anesthetic collyrium. In two cases (11.1%), a transient scleral show was observed (both with a duration of 2 months), which resolved with local massage and muscle exercises. Late complications such as eyelid retractions, ectropion, hematoma, infection, rounding of the lateral corner, lacrimal pump dysfunction, conjunctival granuloma, unaesthetic scars, infraorbital emptying (tearthrough deformity), diplopia, or remnant fat bags, were not observed. No surgical reintervention was required in any case.
Some of the pre- and postoperative results are seen in Figures 6 and 7.
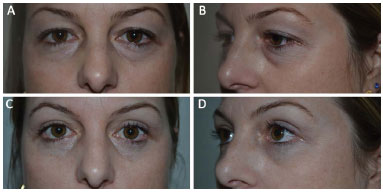
Figure 6. A e B: Preoperative. C e D: 60 days postoperative.
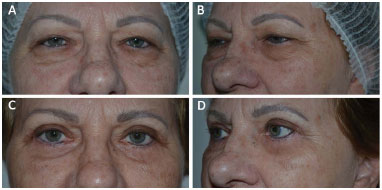
Figure 7. A e B: Preoperative. C e D: 60 days postoperative.
DISCUSSION
Transcutaneous lower blepharoplasty, despite offering excellent intraoperative exposure to structures, causes damage to the orbital septum and increases the chances of eyelid malposition in up to 20% of cases, including retraction with scleral show, ectropion, rounding of the lateral canthal angle, and changes in the dimensions of the palpebral fissure with functional consequences1-3,8.
The transconjunctival approach associated with skin resection with preservation of the orbicularis muscle, also called the "no touch" technique, has been gaining popularity among surgeons since it also allows access to the fat bags, but with a much lower rate of complications than that in the transcutaneous approach7,8,19,20. This is due to the preservation of the orbital septum, middle lamella, and the innervation of the orbicularis muscle10.
The motor innervation of the orbicularis muscle of the lower eyelid is through nerve fibers from the zygomatic branch of the facial nerve. There is no single dominant branch, and adjacent branches have the capacity for collateral reinnervation in the case of partial injury. Studies performed with cadavers indicate that there are 5 to 7 terminal branches that reach the muscle transversely to their parallel course21, or from 3 to 5 branches that reach the muscle perpendicularly22.
Regardless of the anatomy controversy, authors agree that when there is transection or removal of the muscle fibers, there is a partial or complete denervation of the preseptal portion of the muscle above the level of the incision. This is the main cause of the most common long-term problem in transcutaneous blepharoplasties, i.e., a decrease in muscle tone is observed in the long term due to denervation and acceleration of senile palpebral alterations23. This is prevented by using the "no touch" technique. Therefore, the majority of authors now strongly recommend the preservation of the integrity of the orbicularis muscle of the lower eyelid, to prevent complications related to its denervation9-11,19,21,24. Our study is in agreement with this idea, since in all patients from our sample, no muscle or nerve injury of the lower eyelid was observed, and related postoperative complications were not detected.
Some authors suggest that transconjunctival lower blepharoplasty presents several advantages over the transcutaneous approach, such as lower risk of retraction and ectropion, ease in accessing the middle third of the face (if required), decreased surgical duration, and the possibility of combining it with other facial surgeries and skin treatments such as resurfacing with a CO2 laser19.
In our study, the treatment performed on the lower eyelid was exclusively the skin pinch with resection and muscle preservation. This technique without skin detachment grasps a smaller skin area, decreasing the chances of occurrence of hematomas and scar contracture10. Furthermore, it minimizes the risks of eyelid malposition since it avoids breaching the orbital septum and middle lamella8. Some studies point out the increased risks of skin necrosis and damage to local lymphatic drainage23 when this technique is used. However, this was not observed in our sample.
In all patients, the skin strip resected was sufficient to obtain a satisfactory aesthetic result. There was no need for reintervention and there were no complaints from patients. Nevertheless, we believe that in cases of greater excess of skin, this technique may not be adequate, and may require a different approach, with either skin or musculocutaneous grafts, and with greater detachment and resection of skin.
In regard to the resected fat bags in the lower eyelid, it is important to avoid overcorrection. Otherwise, there will be risks of causing a tear-through deformity, which is the unaesthetic sinking of the nasojugal sulcus region. However, too little resection of bags, in particular the lateral bag, may also result in deformities in lower eyelid shape and require surgical reintervention19. In our sample, there were no complaints from patients or the need for reintervention due to the extent of fat bag resection.
Temporary periorbital edema, ecchymoses, chemosis, and corneal abrasions are common complaints in this type of intervention, and are also reported in the literature, with a rate of occurrence very similar to that observed in our study9,13,19,20,24.
The reinforcement of the lateral canthal ligament with canthopexy in patients with mild to moderate laxity may treat this preexisting condition and also prevent postoperative eyelid malposition. Several authors favor using this technique to complement lower blepharoplasty14-18. In this study, patients who presented with mild to moderate laxity were submitted to canthopexy of the lateral retinaculum with muscle suspension without cantholysis, with good results in all cases. We did not observe severe ligament laxity in any patients, and other surgical techniques such as canthoplasty, cantholysis, or tarsal stripping were not required.
CONCLUSION
Transconjunctival blepharoplasty is an excellent method for accessing herniated fat bags in the lower eyelid and offers the surgeon a good view for the excision of the bags, while maintaining the orbital septum and middle lamella intact. The association of this technique with skin pinch and resection without detachment has the added advantage of preserving the orbicularis muscle and its innervation, considerably decreasing postoperative complications and sequelae when compared with transcutaneous blepharoplasty. In addition, in selected cases, the need for lateral ligament support with simple canthopexy has been shown to be an efficient method for correction of mild to moderate laxity of the lower eyelid and prevention of postoperative eyelid malposition.
Transconjunctival lower blepharoplasty with skin resection without detachment and with preservation of the orbicularis muscle, with or without canthopexy, is an excellent technique, and is easily reproducible, reliable, and safe, with few postoperative complications in the treatment of age-related changes in the lower eyelids.
REFERENCES
1. Mathes SJ, Hentz VR. Plastic Surgery. Philadelphia: Saunders, Elsevier; 2006. DOI: http://dx.doi.org/10.1016/S1551-7977(08)70117-1
2. DiFrancesco LM, Anjema CM, Codner MA, McCord CD, English J. Evaluation of conventional subciliary incision used in blepharoplasty: preoperative and postoperative videography and electromyography findings. Plast Reconstr Surg. 2005;116(2):632-9. PMID: 16079702 DOI: http://dx.doi.org/10.1097/01.prs.0000173446.21513.47
3. Lessa SF, Elena LH, Araújo MRC, Pitanguy I. Modificação anatômica da fenda palpebral pós blefaroplastia. Rev Bras Cir. 1997;87(4):179-88.
4. Bourguet J. Les lernies graissenses de l'orbite: Notre traitement chirugical. Bull Acad Med (Paris). 1924;92:1270.
5. Tessier P. The conjunctival approach to the orbital floor and maxilla in congenital malformation and trauma. J Maxillofac Surg. 1973;1(1):3-8. DOI: http://dx.doi.org/10.1016/S0301-0503(73)80005-0
6. Zarem HA, Resnick JI. Expanded applications for transconjunctival lower lid blepharoplasty. Plast Reconstr Surg. 1991;88(2):215-20. DOI: http://dx.doi.org/10.1097/00006534-199108000-00006
7. McCord CD Jr, Shore JW. Avoidance of complications in lower lid blepharoplasty. Ophthalmology. 1983;90(9):1039-46. DOI: http://dx.doi.org/10.1016/S0161-6420(83)80044-X
8. Taban M, Taban M, Perry JD. Lower eyelid position after transconjunctival lower blepharoplasty with versus without a skin pinch. Ophthal Plast Reconstr Surg. 2008;24(1):7-9. DOI: http://dx.doi.org/10.1097/IOP.0b013e318160f3a0
9. Pacella SJ, Nahai FR, Nahai F. Transconjunctival blepharoplasty for upper and lower eyelids. Plast Reconstr Surg. 2010;125(1):384-92. PMID: 20048630 DOI: http://dx.doi.org/10.1097/PRS.0b013e3181c2a534
10. Kim EM, Bucky LP. Power of the pinch: pinch lower lid blepharoplasty. Ann Plast Surg. 2008;60(5):532-7. PMID: 18434828 DOI: http://dx.doi.org/10.1097/SAP.0b013e318172f60e
11. Dinner MI, Glassman H, Artz JS. The "no flap" technique for lower-lid blepharoplasty. Aesthetic Plast Surg. 1992;16(2):155-8. PMID: 1570778 DOI: http://dx.doi.org/10.1007/BF00450607
12. Glat PM, Jelks GW, Jelks EB, Wood M, Gadangi P, Longaker MT. Evolution of the lateral canthoplasty: techniques and indications. Plast Reconstr Surg. 1997;100(6):1396-405. DOI: http://dx.doi.org/10.1097/00006534-199711000-00003
13. de Castro CC. A critical analysis of the current surgical concepts for lower blepharoplasty. Plast Reconstr Surg. 2004;114(3):785-93. DOI: http://dx.doi.org/10.1097/01.PRS.0000131238.55620.9F
14. Mladick RA. The muscle-suspension lower blepharoplasty. Plast Reconstr Surg. 1979;64(2):171-5. PMID: 451075 DOI: http://dx.doi.org/10.1097/00006534-197908000-00006
15. Fagien S. Lower-eyelid rejuvenation via transconjunctival blepharoplasty and lateral retinacular suspension: a simplified suture canthopexy and algorithm for treatment of the anterior lower-eyelid lamella. Op Tech Plast Reconstr Surg. 1998;5(2):121-8. DOI: http://dx.doi.org/10.1016/S1071-0949(98)80005-X
16. Jelks GW, Glat PM, Jelks EB, Longaker MT. The inferior retinacular lateral canthoplasty: a new technique. Plast Reconstr Surg. 1997;100(5):1262-70. DOI: http://dx.doi.org/10.1097/00006534-199710000-00030
17. Lessa S, Nanci M. Simple canthopexy used in transconjunctival blepharoplasty. Ophthal Plast Reconstr Surg. 2009;25(4):284-8. DOI: http://dx.doi.org/10.1097/IOP.0b013e3181aa9426
18. Flowers RS. Canthopexy as a routine blepharoplasty component. Clin Plast Surg. 1993;20(2):351-65.
19. Kashkouli MB, Pakdel F, Kiavash V, Ghiasian L, Heirati A, Jamshidian-Tehrani M. Transconjunctival lower blepharoplasty: a 2-sided assessment of results and subjects' satisfaction. Ophthal Plast Reconstr Surg. 2013;29(4):249-55. DOI: http://dx.doi.org/10.1097/IOP.0b013e31828ecfb9
20. Carreirão S, ed. Cirurgia plástica: para a formação do especialista. São Paulo: Atheneu; 2011.
21. Hwang K, Lee DK, Lee EJ, Chung IH, Lee SI. Innervation of the lower eyelid in relation to blepharoplasty and midface lift: clinical observation and cadaveric study. Ann Plast Surg. 2001;47(1):1-5. PMID: 11756795 DOI: http://dx.doi.org/10.1097/00000637-200107000-00001
22. Ramirez OM, Santamarina R. Spatial orientation of motor innervation to the lower orbicularis oculi muscle. Aesthetic Surg. 2000;20:107-13. DOI: http://dx.doi.org/10.1067/maj.2000.106712
23. Lowe JB 3rd, Cohen M, Hunter DA, Mackinnon SE. Analysis of the nerve branches to the orbicularis oculi muscle of the lower eyelid in fresh cadavers. Plast Reconstr Surg. 2005;116(6):1743-9. DOI: http://dx.doi.org/10.1097/01.prs.0000186532.29557.96
24. Mélega JM. Cirurgia Plástica - Fundamentos e Arte: princípios gerais. Cirurgia Estética. Rio de Janeiro: Guanabara; 2003.
Sociedade Brasileira de Cirurgia Plástica, Florianópolis, SC, Brazil
Institution: Hospital da Plástica de Santa Catarina, Florianópolis SC, Brazil.
Corresponding author:
Ingrid Paula Lückmann Bernardino
Rua Dom Joaquim, 885, Centro
Florianópolis, SC, Brazil Zip Code 88015-310
E-mail: ingridplb@hotmail.com
Article received: August 6, 2014.
Article accepted: November 17, 2014.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter