

Review Article - Year 2016 - Volume 31 -
Breast augmentation with autologous fat grafting: literature review and case report
Mamoplastia de aumento com lipoenxertia autóloga: revisão da literatura e relato de caso
ABSTRACT
INTRODUCTION: The technique and technology lipoaspirate autotransplantation to the breast with the aim of aesthetic appearance and reconstruction has strongly advanced; further, its acceptance by doctors and patients has also improved. The author reports cosmetic breast augmentation and performed a literature review, focusing on the efficacy, carcinogenic potential, and imaging diagnosis.
METHOD:A literature review was performed using English-language articles from the PubMed database and the Brazilian Journal of Plastic Surgery (RBCP); in addition, case series of the initial experience of the author has been described.
RESULTS: The volume remained stable from the second month, and there were no postoperative complications. Imaging did not show any pathological alterations. In all, 24-related articles were selected.
DISCUSSION: Among the 24 articles, only two prospective non-controlled studies were found, but overall, imaging diagnostic tests did not reveal problems, the carcinogenic potential was not increased, and case series had positive results.
CONCLUSION: The procedure is reproducible, safe and effective, and reinforces the use of this technique in breast reconstruction and as an option in cosmetic breast augmentation. However, it may require a longer learning curve to avoid complications and achieve good results.
Keywords: Grafts; Fat; Lipoaspiration; Mammoplasty; Breast.
RESUMO
INTRODUÇÃO: O autotransplante do lipoaspirado na mama para fins estéticos e reconstrutivas tem avançado intensamente na técnica e na tecnologia, assim como na aceitação dos médicos e dos pacientes. O autor relata um caso de aumento mamário estético e discute a revisão da literatura, interessando a eficácia, o potencial carcinogênico e o exame de imagem.
MÉTODO:Revisão da literatura no Pubmed na língua inglesa e na Revista Brasileira de Cirurgia Plástica, e relato de caso da experiência inicial do autor.
RESULTADO: O volume manteve-se estável a partir do segundo mês, e não houve complicações no pós-operatório. Os exames de imagem não apresentaram alterações patológicas. Foram selecionados 24 artigos relacionados.
DISCUSSÃO: Dos 24 artigos, só há dois artigos prospectivos não controlados, mas, de maneira geral, não há problemas no diagnóstico nos exames por imagem, não há aumento de potencial cancerígeno, e os resultados são bons nas séries de casos.
CONCLUSÃO: O procedimento é reprodutível, seguro e eficaz, consolidando-se como uma indicação no tratamento reparadora da mama e uma opção no aumento estético. Entretanto, uma curva de aprendizado mais longa pode ser necessária, para evitar complicações e atingir bons resultados.
Palavras-chave: Enxertos; Gordura; Lipoaspiração; Mamoplastia; Mama.
Fat grafting to the breast was condemned by the American Society of Plastic and Reconstructive Surgeons in 1987 owing to the possibility of calcifications that could interfere with the interpretation of breast cancer screening1-3. Recently, this scenario changed. Owing to the advancement of imaging diagnosis and improvement in fat grafting techniques, the lipoaspirate autotransplant was used in cosmetic breast augmentation and mammary reconstruction, and was relevant not only in the reposition of mammary volume but also in skin regeneration in postradiotherapy lesions4-20.
In 2009, the American Society of Plastic and Reconstructive Surgeons revised its position on this, and stated that the result obtained was dependent on the technique and surgeon experience21. Better insights into the actions of mesenchymal cells provided more predictable results in maintaining the graft volume and initiated a new phase in tissue regeneration and reconstructive surgery22-24.
Fat grafting to the breast is controversial as it is associated with interference with imaging diagnosis in breast cancer screening25-32 and the origin of transplanted mesenchymal cells from breast cancer or existing cancer enhancement33,34. Until currently, no case of breast cancer caused by fat grafting, as well as non-diagnosed breast cancer due to breast fat grafting have been reported in the literature, and thus, this procedure has become popular in Europe, USA, Japan, and China35. In the present work, the author performed a bibliographic review and reported the initial experience of the author.
METHODS
Bibliographic review
A search of bibliographic reviewsin the English language was performed in PubMed using the terms "breast augmentation fat" and in the Brazilian Journal of Plastic Surgery (RBCP), using the terms "lipoaspiration" and "breast". Articles on efficacy and safety of the technique, imaging studies in the postoperative period, research on the carcinogenic potential of the lipoaspirate autotransplant, and details on the positions that Societies and Public Health had in relation to the procedure were collected.
Case report
A CFA (age, 23 years) nulliparous woman, presenting hypomastia and discrete asymmetry, without a family history of mammary neoplasia, wished to undergo moderate augmentation of the breasts, however, she refused silicone implants. The patient underwent lipoaspiration under general anesthesia of the lumbar and abdominal regions, with infiltration using adrenaline solution 1:250,000, at the proportion 1:1 by using a 3-mm internal diameter cannula and catheter tip syringe 60 mL (Becton Dickinson do Brasil). The lipoaspirate was centrifuged for 3 min at 3,000 rpm.
From the four phases after centrifugation, the fat cell layer and the small stromal fraction were used. Fat grafting was performed with a 10 mL Luer-lock syringe and a 14G needle through a retro-injection at the retroglandular and subcutaneous planes, at the border or the base of the breast at 12, 2, 4, 6, 8, and 10 hours, and homogeneous distribution, avoiding bolus injection and mammary parenchyma injection (Figure 1).
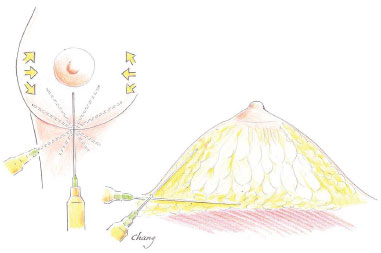
Figure 1. Fat grafting technique in the retromammary and subcutaneous planes.
In all, 190 mL of the centrifuged material was transplanted into the left breast and 240 mL in the right breast. Mammary ultrasonography at 6 months after surgery showed a nonspecific cyst. The second fat grafting session was performed 6 months later, with the same technique to remove material from the trochanteric regions of the knees and inside of the thigh, and 200 mL was injected in each breast (Figures 2, 3, and 4).
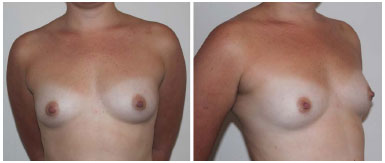
Figure 2. Preoperative.
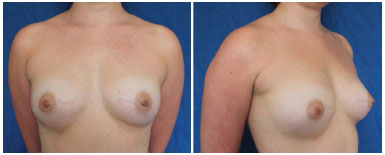
Figure 3. Six-month results after the first fat grafting session.
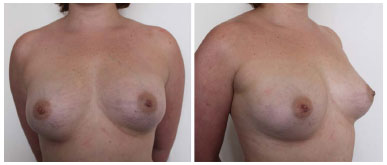
Figure 4. Results 7 months after the second fat grafting session and 13 months after the first fat grafting.
RESULTS
Edema and ecchymosis developed after 2 to 3 weeks, and there was a small to moderate loss of volume within 2 to 4 months, compared to the initial volume, and, later, a small increase in volume was noted, which stabilized subsequently. Volumes before and after the procedures were not measured, but apparently, there was a significant gain in volume.
Literature review
In all, 136 articles were found in PubMed and selected, of which 4 were review articles, 7 case series, 8 imaging studies, 2 carcinogenic potential analyses, and 3 were on complications. Among the case series reports, only 2 articles were prospective but uncontrolled. In the Brazilian Journal of Plastic Surgery (RBCP), we found a review article and one poster that cited fat grafting used to complement the post-breast reconstruction.
Imaging testing
In a blind test performed by Rubin et al.25, mammographic alterations after breast fat grafting in 27 patients were compared with those after breast reduction in 23 patients, and fewer radiological abnormalities, a lower BI-RADS index, and fewer calcifications in those with recommended biopsy were found in the fat grafting group that underwent breast augmentation. However, Wang et al.26 found microcalcifications in 8 patients from a total of 48 patients, in those who had undergone biopsies, and these were identified as steatonecrosis; the authors concluded that breast fat grafting should be "prohibited". When discussing the article, Del Vecchio27 underlines that this conclusion is not in agreement with the literature; that imaging techniques should be improved or adapted instead of "prohibiting" the procedure; and that if the recommendations by Dr. Wang should be followed, then reduction mammoplasty procedures should also be avoided. In a review of 20 patients in a study by Veber et al., there were no alterations in the breast radiological density and in the BI-RADS score, and the authors concluded that postoperative radiological imaging in breast fat grafting was not problematic, and should not constitute an impediment to the procedure28,29. Wang et al. investigated the characteristics of ultrasonography and follow-up of the evolution of nodules after breast fat grafting in 34 patients and concluded that ultrasonography is a simple and accurate procedure in the diagnosis and follow-up of such nodules, and may prevent unnecessary biopsies30,31. Carvajal & Patiño32 studied specific characteristics of steatonecrosis of breast fat grafting in 20 patients and described the re-classification of the most common alteration, the sparse microcalcification, followed by fat cysts, in 3 patients with BI-RADS score 3 into a score of 2, after performing digital mammography.
Carcinogenic potential
A retrospective multicenter study performed by Petit et al.33 involving three European institutions specialized in breast cancer and reconstruction: Milan, Paris and Lyon, analyzed immediate complications and the oncologic profiles of 646 fat grafting procedures after breast cancer treatment, and showed a complication rate of 2.8% (2% by liponecrosis, 0.5 by local infection, 0.2% by seroma, and 0.2% by pneumothorax), 2.07% of local or regional recurrence in the group that underwent conservative treatment, and 1.38% in the group treated with mastectomy. The study demonstrated that fat grafting presents a very low rate of complication and does not affect radiological control, but on the other hand, a control study was needed to provide evidence of its safety in regard to cancer recurrence33.
Rigotti et al.34 examined the rate of breast cancer recurrence after fat grafting at the resection site or near the site, by comparing the incidence of recurrence after mastectomy and before fat grafting with the incidence after fat grafting, and did not find a difference. Further, due to the regenerative capacity of the lipoaspirate graft, and apparently without any recurrence in cancer, this procedure was recommended by Rigotti for reconstructions after mastectomy.
Case series
Fulton published a series of 20 breast augmentation cases that underwent fat grafting in 1992, with the lipoaspirate washed with Ringer's lactate and obtained an initial average injection volume of 289.5 mL, with a retention rate of 71%. In this author's second series, published in 2003, a lipoaspirate "incubated" in platelet rich plasma (PRP) was used in 65 patients, a retention rate of 73% was obtained, and an average breast increase equivalent to a 200 to 250 mL implant was achieved4. Salgarello et al.5 did not observed any differences in a review that compared 17 patients who had undergone 10% fat grafting with the Coleman technique in PRP with 25 patients who had undergone breast fat grafting with the Coleman technique without PRP.
Coleman & Saboeiro6 described their technique as non-traumatic, with small volumes, good distribution, and limited intra-parenchymal injection, and reported a series of 17 patients, with fat grafting between 50 and 450 mL within one to three sessions, and found stabilization of the grafted volume within 4 to 6 months, with an excellent aesthetic result seven years after the procedure. Further, no relevant complications were reported. Two patients had cancer diagnosed by mammography, one in the site that did not received fat grafting, and the other, probably in the grafted area. Both patients were diagnosed and treated without delay.
Zocchi & Zuliani7 abandoned the intra-parenchymal injection technique due to the high rate of complications and graft resorption, and concluded that the result is dependent on the technique used. They used the breast pre-expansion with the BRAVA system, phase separation of the lipoaspirate using a shaking table, and performed an injection at the retromammary and subcutaneous planes. With this, an average retention rate of 55% of the transplanted volume and an average volume of 325 mL was achieved, with minimum complications.
In the series reported by Zheng et al.8, with 66 patients, the lipoaspirate was washed with saline solution and centrifuged at 600 rpm for 2 minutes, and the average volume injected was of 101 ml in the subcutaneous plane, and 73 ml in the subglandular. Seventeen patients were submitted to 3 sessions, 21 patients to 2 sessions, and 28 to one session of fat grafting. According to 3 independent plastic surgeons, there was a significant increase in 33%, increase in 58%, and absence of increase in 8%. Regarding patient level of satisfaction, 33% were very satisfied, 63% satisfied and 4% not satisfied.
In a series by Illouz & Sterodimas9 from 1983 to 2007, 820 patients underwent fat grafting; among which, cosmetic breast augmentation was performed in 385 patients. The lipoaspirate was decanted, with an average volume of 240 mL injected in the parenchyma and subcutaneous tissue and the retromammary plane was avoided, in 1 to 5 fat grafting sessions. It was necessary to complement this volume with that of the silicone implant in 36 cases, but the majority of patients was satisfied with the results.
Delay et al.10 published a retrospective series of 10 years on 880 lipoaspirate transplants centrifuged in 734 patients, of which 30 were used for aesthetic purposes. The mean volume injected was 140 mL, with a loss of 30% to 40%, and stabilization was achieved within 3 to 4 months. A high level of satisfaction was attained by patients and surgeons, and breast cancer recurrence was not observed, and a fat necrosis rate of 15% was initially observed and decreased when hyper-saturation of the volume transplanted was avoided.
Yoshimura et al.11 isolated the stromal vascular fraction containing cells of the mesenchymal trunk of half of the lipoaspirate and added these cells to the other half of the lipoaspirate, and described the technique as "cell assisted lipotransfer" (CAL), and in 40 patients, the final volume of 100 reached 200 mL after a mean injection volume of 270 mL was maintained. This volume did not change significantly after two months, and when compared to conventional fat grafting cases, an increase in the breast circumference was observed; however, this was not a controlled study.
Kamakura & Ito12 processed an adipose-derived regenerative cells (ADRCs)-enriched lipoaspirate by using the Celution 800 System® (a device that is still under revision by the Food and Drug Administration), and made a non-controlled analysis prospectively in 20 patients who had a mean increase of 3.3 cm in the mammary circumference, 9 months after fat grafting.
Khoury et al.13 (Khoury is the inventor of the Brava system) performed a prospective, multicenter study on 81 patients from 6 meta-analyses published recently, and compared their results of lipoaspirate transplants in pre-expanded breasts using negative pressure and breast fat grafting performed without pre-expansion. The expansion with negative pressure was performed 10 hours per day for 4 weeks, and continuously for 36 to 48 hours immediately before the fat grafting. The lipoaspirate was centrifuged at 15 g for 3 minutes, and the mean volume transplanted was 277 mL. From the third to the sixth month, the volume remained stable, and compared with the meta-analysis results, the mean volume increased at 12 months to 233 mL as against 134 mL per breast without pre-expansion, and the survival rate of the graft was 82 ± 18% as against 55 ± 18%.
DISCUSSION
Questions on the safety of fat grafting for cosmetic breast augmentation are associated with the interpretation of imaging diagnosis in cancer screening tests, and the possibility that the mesenchymal cell trunk may cause breast cancer. Regarding efficacy, relevance is given to graft survival, the lipoaspirate volume that the breast can take without resulting in necrosis, and the maintenance of that volume.
Necrosis in the center of the fat graft, when large, causes the formation of a fat cyst, and may develop into a nodule or calcification. The bolus injection technique is the main cause and has been discontinued7. Currently, there seems to be little disagreement between radiologists in regard differences between calcification after fat grafting and calcification with suspected malignancy.
The carcinogenic potential of the mesenchymal cell trunk is still not well known, and in vitro studies and animal models have demonstrated contrasting results for propensity and inhibition of the potential. There have been no reports in the literature about breast cancer caused by fat grafting; however, the complete safety of fat grafting is still inconclusive after conservative treatment of breast cancer.
On the other hand, there has been debate in regard to the efficacy, advantages and disadvantages of the procedure. The autologous transplant of the lipoaspirate prevents a scar, does not cause sensitivity alterations, is not related to problems with a foreign body in the site, the result is more natural, its application more versatile, and the donor area is also aesthetic. Meanwhile, the transplanted volume is limited due to recipient capacity and by graft survival rate, in addition to other specific or common complications in surgical procedures35-41.
The result, in general, is still not predictable, and several sessions of fat grafting may be necessary. Based on the reviewed series, it is possible to maintain 60% to 70% of the volume injected with the revised technique to obtain a moderate increase by only using lipoaspirate, and without adding growing factors or mesenchymal cell trunk. When larger augmentation is required and there is not enough breast skin, the external expansion system with negative pressure may be the solution.
In a reported case, the patient desired moderate increase and symmetry, and did not want a silicone breast implant. Although there was no evidence against this, there are still controversies regarding the safety of the addition of growth factors or mesenchymal stem cells in the transplanted lipoaspirate, which was not used in this case. A moderate increase in the content without an increase of continent may result in a more firm breast.
CONCLUSION
Fat grafting techniques, in general, and the breast, in particular, are already well established. Postoperative oncological treatment through imaging is not more problematic. There is no evidence of an increase in carcinogenic potential of the lipoaspirate transplant. The technique is reproducible, the results are more predictable, a greater volume can be transplanted in each session, and a greater maintenance rate of that volume has been noted; however, there may be a longer learning curve associated since the results are dependent on the techniques.
REFERENCES
1. Parrish JN, Metzinger SE. Autogenous fat grafting and breast augmentation: a review of the literature. Aesthet Surg J. 2010;30(4):549-56. DOI: http://dx.doi.org/10.1177/1090820X10380859
2. Rosing JH, Wong MS, Sahar D, Sevenson TR, Pu LL. Autologous fat grafting for primary breast augmentation: a systematic review. Aesthetic Plast Surg. 2011;35(5):882-90. DOI: http://dx.doi.org/10.1007/s00266-011-9691-2
3. Mizuno H, Hyakusoku H. Fat grafting to the breast and adipose-derived stem cells: recent scientific consensus and controversy. Aesthet Surg J. 2010;30(3):381-7. DOI: http://dx.doi.org/10.1177/1090820X10373063
4. Fulton JE. Breast countouring with "gelled" autologous fat: a 10 year update. Int J Cosmet Surg Aesthetic Dermatol. 2003;5(2):155-63. DOI: http://dx.doi.org/10.1089/153082003769591272
5. Sagarello M, Visconti G, Rusciano A. Breast fat grafting with platelet-rich plasma: a comparative clinical study and current state of the art. Plast Reconstr Surg. 2011;127(6):2176-85. DOI: http://dx.doi.org/10.1097/PRS.0b013e3182139fe7
6. Coleman SR, Saboeiro AP. Fat grafting to the breast revisited: safety and efficacy. Plast Reconstr Surg. 2007;119(3):775-85. DOI: http://dx.doi.org/10.1097/01.prs.0000252001.59162.c9
7. Zocchi ML, Zuliani F. Biocompartimental breast lipostructuring. Aesthetic Plast Surg. 2008;32(2):313-28. PMID: 18188638 DOI: http://dx.doi.org/10.1007/s00266-007-9089-3
8. Zheng DN, Li QF, Lei H, Zheng SW, Xie YZ, Xu QH, et al. Autologous fat grafting to the breast for cosmetic enhancement: experience in 66 patients with long-term follow up. J Plast Reconstr Aesthet Surg. 2008;61(7):792-8. PMID: 18321802 DOI: http://dx.doi.org/10.1016/j.bjps.2007.08.036
9. Illouz YG, Sterodimas A. Autologous fat transplantation to the breast: a personal technique with 25 years of experience. Aesthetic Plast Surg. 2009;33(5):706-15. PMID: 19495856 DOI: http://dx.doi.org/10.1007/s00266-009-9377-1
10. Delay E, Garson S, Tousson G, Sinna R. Fat injection to the breast: technique, results, and indications based on 880 procedures over 10 years. Aesthet Surg J. 2009;29(5):360-76. DOI: http://dx.doi.org/10.1016/j.asj.2009.08.010
11. Yoshimura K, Sato K, Aoi N, Kurita M, Hirohi T, Harii K. Cellassisted lipotransfer for cosmetic breast augmentation: supportive use of adipose-derived stem/stromal cells. Aesthetic Plast Surg. 2008;32(1):48-55. PMID: 17763894 DOI: http://dx.doi.org/10.1007/s00266-007-9019-4
12. Kamakura T, Ito K. Autologous cell-enriched fat grafting for breast augmentation. Aesthetic Plast Surg. 2011;35(6):1022-30. DOI: http://dx.doi.org/10.1007/s00266-011-9727-7
13. Khouri RK, Eisenmann-Klein M, Cardoso E, Cooley BC, Kacher D, Gombos E, et al. Brava and autologous fat transfer is a safe and effective breast augmentation alternative: results of a 6-year, 81-patient, prospective multicenter study. Plast Reconstr Surg. 2012;129(5):1173-87. PMID: 22261565 DOI: http://dx.doi.org/10.1097/PRS.0b013e31824a2db6
14. Serra-Renom JM, Muñoz-Olmo J, Serra-Mestre JM. Treatment of grade 3 tuberous breasts with Puckett's technique (modified) and fat grafting to correct the constricting ring. Aesthetic Plast Surg. 2011;35(5):773-81. DOI: http://dx.doi.org/10.1007/s00266-011-9686-z
15. Khouri R, Del Vecchio D. Breast reconstrution and augmentation using pré-expansion and autologous fat transplantation. Clin Plast Surg. 2009;36(2):269-80. DOI: http://dx.doi.org/10.1016/j.cps.2008.11.009
16. Del Vecchio DA, Bucky LP. Breast augmentation using preexpansion and autologous fat transplantation: a clinical radiographic study. Plast Reconstr Surg. 2011;127(6):2441-50. PMID: 21617476 DOI: http://dx.doi.org/10.1097/PRS.0b013e3182050a64
17. Hughes LM, Stephen C, Johnson AB, Wilson S. Breast augmentation in Familial Partial Lipodystrophy: a case report. J Plast Reconstr Aesthet Surg. 2011;64(5):e121-4. DOI: http://dx.doi.org/10.1016/j.bjps.2011.01.001
18. Rigotti G, Marchi A, Galiè M, Baroni G, Benati D, Krampera M, et al. Clinical treatment of radiotherapy tissue damage by lipoaspirate transplant: a healing process mediated by adipose-derived adult stem cells. Plast Reconstr Surg. 2007;119(5):1409-22. DOI: http://dx.doi.org/10.1097/01.prs.0000256047.47909.71
19. Penettiere P, Marchetti L, Accorsi D. The serial free fat transfer in irradiated prosthetic breast reconstructions. Aesthetic Plast Surg. 2009;33(5):695-700. DOI: http://dx.doi.org/10.1007/s00266-009-9366-4
20. Sultan SM, Stern CS, Allen RJ Jr, Thanik VD, Chang CC, Nguyen PD, et al. Human fat grafting alleviates radiation skin damage in a murine model. Plast Reconstr Surg. 2011;128(2):363-72. DOI: http://dx.doi.org/10.1097/PRS.0b013e31821e6e90
21. Gutowski KA; ASPS Fat Graft Task Force. Current applications and safety of autologous fat grafts: a report of the ASPS fat graft task force. Plast Reconstr Surg. 2009;124(1):272-80. PMID: 19346997 DOI: http://dx.doi.org/10.1097/PRS.0b013e3181a09506
22. Gir P, Oni G, Brown SA, Mojallal A, Rohrich RJ. Human adipose stem cells: current clinical applications. Plast Reconstr Surg. 2012;129(6):1277-90. PMID: 22634645 DOI: http://dx.doi.org/10.1097/PRS.0b013e31824ecae6
23. Hanson SE, Bentz ML, Hematti P. Mesenchymal stem cell therapy for nonhealing cutaneous wounds. Plast Reconstr Surg. 2010;125(2):510-6. PMID: 20124836 DOI: http://dx.doi.org/10.1097/PRS.0b013e3181c722bb
24. Li H, Zimmerlin L, Marra KG, Donnenberg VS, Donnenberg AD, Rubin JP. Adipogenic potential of adipose stem cell subpopulations. Plast Reconstr Surg. 2011;128(3):663-72. PMID: 21572381 DOI: http://dx.doi.org/10.1097/PRS.0b013e318221db33
25. Rubin JP, Coon D, Zuley M, Toy J, Asano Y, Kurita M, et al. Mammographic changes after fat transfer to the breast compared with changes after breast reduction: a blinded study. Plast Reconstr Surg. 2012;129(5):1029-38. PMID: 22261561 DOI: http://dx.doi.org/10.1097/PRS.0b013e31824a2a8e
26. Wang CF, Zhou Z, Yan YJ, Zhao DM, Chen F, Qiao Q. Clinical analyses of clustered microcalcifications after autologous fat injection for breast augmentation. Plast Reconstr Surg. 2011;127(4):1669-73. PMID: 21187809 DOI: http://dx.doi.org/10.1097/PRS.0b013e318208d1e4
27. Del Vecchio DA. Discussion: Clinical analyses of clustered microcalcifications after autologous fat injection for breast augmentation. Plast Recontr Surg. 2011;127(4):1674-6. PMID: 21460674 DOI: http://dx.doi.org/10.1097/PRS.0b013e3182100ddd
28. Veber M, Tourasse C, Toussoun G, Moutran M, Mojallal A, Delay E. Radiographic findings after breast augmentation by autologous fat transfer. Plast Reconstr Surg. 2011;127(3):1289-99. PMID: 21364429 DOI: http://dx.doi.org/10.1097/PRS.0b013e318205f38f
29. Veber M, Tourasse C, Moutran M, Mojallal A. Clinical analyses of clustered microcalcifications after autologous fat injection for breast augmentation. Plast Reconstr Surg. 2012;129(1):168e-9e. DOI: http://dx.doi.org/10.1097/PRS.0b013e3182362e2b
30. Wang H, Jiang Y, Meng H, Zhu Q, Dai Q, Qi K. Sonographic identification of complications of cosmetic augmentation with autologous fat obtained by liposuction. Ann Plast Surg. 2010;64(4):385-9. PMID: 20224341 DOI: http://dx.doi.org/10.1097/SAP.0b013e3181b14265
31. Wang H, Jiang Y, Meng H, Yu Y, Qi K. Sonographic assessment on breast augmentation after autologous fat graft. Plast Reconstr Surg. 2008;122(1):36e-8e. DOI: http://dx.doi.org/10.1097/PRS.0b013e3181774732
32. Carvajal J, Patiño JH. Mammographic findings after breast augmentation with autologous fat injection. Aesthet Surg J. 2008;28(2):153-62. DOI: http://dx.doi.org/10.1016/j.asj.2007.12.008
33. Petit JY, Lohsiriwat V, Clough KB, Sarfati I, Ihrai T, Rietjens M, et al. The oncologic outcome and immediate surgical complications of lipofilling in breast cancer patients: a multicenter study-Milan-Paris-Lyon experience of 646 lipofilling procedures. Plast Reconstr Surg. 2011;128(2):341-6. PMID: 21502905 DOI: http://dx.doi.org/10.1097/PRS.0b013e31821e713c
34. Rigotti G, Marchi A, Stringhini P, Baroni G, Galiè M, Molino AM, et al. Determining the oncological risk of autologous lipoaspirate grafting for post-mastectomy breast reconstruction. Aesthetic Plast Surg. 2010;34(4):475-80. PMID: 20333521 DOI: http://dx.doi.org/10.1007/s00266-010-9481-2
35. Mu DL, Luan J, Mu L, Xin MQ. Breast augmentation by autologous fat injection grafting menagement and clinical analysis of complications. Ann Plast Surg. 2009;63(2):124-7. DOI: http://dx.doi.org/10.1097/SAP.0b013e318189a98a
36. Blumenschein AR, Freitas-Júnior R, Tuffanin AT, Blumenschein DI. Lipoenxertia nas mamas: procedimento consagrado ou experimental? Rev Bras Cir Plást. 2012;27(4):616-22.
37. Kim H, Yang EJ, Bang SI. Bilateral liponecrotic pseudocysts after breast augmentation by fat injection: a case report. Aesthetic Plast Surg. 2012;36(2):359-62. DOI: http://dx.doi.org/10.1007/s00266-011-9790-0
38. Lazzaretti MG, Giovanardi G, Gibertoni F, Cagossi K, Artioli F. A late complication of fat autografting in breast augmentation. Plast Reconstr Surg. 2009;123(2):71e-2e. DOI: http://dx.doi.org/10.1097/PRS.0b013e3181959571
39. Hyakusoku H, Ogawa R, Ono S, Ishii N, Hirakawa K. Complications after autologous fat injection to the breast. Plast Reconstr Surg. 2009;123(1):360-70. DOI: http://dx.doi.org/10.1097/PRS.0b013e31819347ba
40. Lee KS, Seo SJ, Park MC, Park DH, Kim CS, Yoo YM, et al. Sepsis with multiple abscesses after massive autologous fat grafting for augmentation mammoplasty: a case report. Aesthetic Plast Surg. 2011;35(4):641-5. DOI: http://dx.doi.org/10.1007/s00266-010-9605-8
41. Bircoll M. Clinical analyses of clustered microcalcifications after autologous fat injection for breast augmentation. Plast Reconstr Surg. 2011;128(6):779e. PMID: 22094783 DOI: http://dx.doi.org/10.1097/PRS.0b013e318230bf6a
1. Sociedade Brasileira de Cirurgia Plástica, Rio de Janeiro, RJ, Brazil
2. Hospital Federal dos Servidores do Estado do Rio de Janeiro, Rio de Janeiro, RJ, Brazil
Institution: Chang Yung Chia Cirurgia Plástica, Rio de Janeiro, RJ, Brazil.
Corresponding author:
Chang Yung Chia
Rua Carlos Oswald, 140 bloco 1, apto. 206, Barra da Tijuca
Rio de Janeiro, RJ, Brazil Zip Code 22793-120
E-mail: changplastica@gmail.com
Article received: December 26, 2012.
Article accepted: September 1, 2013.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter