

Review Article - Year 2016 - Volume 31 -
Depressive disorders in patients who seek cosmetic surgery: a broad and updated view
Transtornos depressivos em pacientes que buscam cirurgia plástica estética: uma visão ampla e atualizada
ABSTRACT
INTRODUCTION: Aesthetic surgery can improve the quality of life of patients, but some candidates for the procedure have depressive disorders (DDs) that may develop, in the postoperative period, in a disastrous manner from a psychological point of view and even progress to suicide. The prevalence of DDs in cosmetic surgery patients is 20% on average and reaches 70%. This article aims to review depression and aesthetic surgery as well as to alert and educate plastic surgeons on the growing number of these patients in clinical settings. It also aims to guide surgeons to the appropriate approach and specific behaviors with these patients.
METHODS: A search was performed in MEDLINE/PubMed and Embase, and key words were entered, including "cosmetic surgery," "depression," "mood disorders," "depressive disorder," "depressive symptoms," and "suicide and plastic surgery."
RESULTS: The success of plastic surgery depends a great deal on the selection of patients for the procedure. Suspect patients, patients with elevated depressive symptoms in questionnaires (such as the BDI), and patients with psychopathology "markers" should be forwarded to a psychiatrist for proper evaluation.
CONCLUSION: Due to the high prevalence of DDs in aesthetic plastic surgery patients, every plastic surgery patient should be evaluated properly to identify those with possible DDs in the preoperative period, and those should be forwarded to a psychiatrist, thus avoiding an unfavorable postoperative psychological evolution.
Keywords: Depression; Depressive Disorder; Psychopathology; Aesthetic Surgery.
RESUMO
INTRODUÇÃO: A cirurgia estética pode melhorar a qualidade de vida de pacientes, porém alguns que se apresentam para o procedimento são portadores de transtornos depressivos (TD) e podem evoluir, no pós-operatório, de forma desastrosa do ponto de vista psicológico e até mesmo evoluir para o suicídio. A prevalência de TD em pacientes de cirurgia plásticaestética é em média de 20%, podendo chegar até 70%. Este artigo tem por objetivo fazer uma revisão sobre depressão e cirurgia estética bem como alertar e conscientizar os cirurgiões plásticos sobre o crescente aumento destes pacientes nos consultórios. Objetiva, ainda, orientar os cirurgiões quanto a abordagem adequada e condutas específicas perante estes.
MÉTODOS: Realizou-se busca nos bancos de dados MEDLINE/PubMed e Embase e cruzamento de palavras chaves, incluindo "cirurgia plástica estética", "depressão"; "transtornos de humor", "transtorno depressivo", "sintomas depressivos", "suicídio e cirurgia plástica".
RESULTADOS: O sucesso de uma cirurgia plástica depende em muito da seleção dos pacientes para o procedimento. Pacientes suspeitos, pacientes com sintomas depressivos elevados nos questionários (como o BDI) e pacientes com "marcadores" de psicopatologia deverão ser encaminhados ao psiquiatra para avaliação adequada.
CONCLUSÃO: Pela elevada prevalência de TD em cirurgia plástica estética, todo paciente de cirurgia plástica deverá ser avaliado adequadamente para identificação daqueles com possíveis TD no pré-operatório e encaminhado ao psiquiatra, para assim tentar se evitar evolução psicológica desfavorável pós-operatória.
Palavras-chave: Depressão; Transtorno depressivo; Psicopatologia; Cirurgia estética
Body image is one of the constructors of self-esteem, which is influenced by a variety of historical, temporal, cultural, social, individual, biological, and religious factors that operate at variable intervals1. Dissatisfaction with this body image is the most relevant factor and the main motivator of demand for cosmetic surgery procedures2. Thus, aesthetic surgery is an essential component of plastic surgery due to its capacity not only to restore function at the physical level but, equally important, to stimulate positive changes in the personality and behavior of an individual as well as several favorable postoperative psychological reactions, including individual/social well-being and self-confidence2-8.
Nevertheless, it is difficult to quantify the exact benefit that plastic surgery may have for the patient's psyche3. Of the patients who seek a consultation for an aesthetic procedure, up to 47.7% fit the criteria for a mental disorder8. They seek in surgery the illusion of achieving an ideal body image with the purpose of decreasing their anguish and feelings of constant dissatisfaction9,10. Several studies have demonstrated that patients who seek cosmetic surgery present larger psychological alterations when compared to the general population2-4,11,12, and the most common disorder found was depression11-13. Depression is a generic term and can encompass depressive symptoms, depressive episodes, and/or depressive disorders (DDs).
This article aims to review DDs and plastic surgery and to alert and educate plastic surgeons on the growing number in these patients during a medical consultation. It also aims to guide surgeons regarding the appropriate approach and practices for these patients and thus avoid possible unfavorable developments in terms of postoperative function and psychological adaptation, regardless of a technically satisfactory result.
SEARCH STRATEGY: DEPRESSIVE DISORDERS
A search was performed in Medline and Embase (on studies from the last 20 years) using key words (in Portuguese and English) including "cosmetic surgery," "mood disorders," "depression," "depressive disorders," "depressive symptoms," and "suicide and plastic surgery."
RESULTS
History
Mood disorders (which include depression) have been known for approximately 2,500 years and were long called melancholy. In the 19th century, the term "depression" found a place in the medical literature with the use of the translation of "melancholy" from the Latin word "deprimere" meaning to lower or depress14.
One of the first descriptions of psychological changes related to a surgical procedure was observed in a patient of the psychiatrist Sigmund Freud who underwent an aesthetic surgical procedure in 1918. His obsession, related to a trivial scar left by removing a cyst, became a focus of one of the most famous cases in the annals of psychiatry14.
Surgical advances obtained in the First World War (1914-1918) and reports of emotional relief observed in scarred individuals served as fuel for the growth of aesthetic surgery15.
Some surgeons performed the first psychiatric evaluations of patients who sought aesthetic surgery in the '40s, '50s, and '60s and described these patients as having highly psychopathological profiles, becoming cautious with insatiable and male patients15. However, these first evaluations did not use adequate methodology, analysis, and standardization, affecting the quality of results and benchmarking of the relationship between DDs and plastic surgery15.
Epidemiology
Depression is a highly lethal disease that often initiates in individuals between 20 and 40 years old with a ratio of up to 2:1 between women and men2,16.
Its annual prevalence varies between 3 and 13% in the general population3-5,8,9,13. Approximately 12% of women and 8% of men are affected at some point in their lives by depressive episodes9,16.
In Brazil, approximately 10% of the adult population presents depressive symptoms. In this group, only 28.1% received a diagnosis for the syndrome (DDs), and an even smaller portion (15.6%) used medications prescribed by specialists for their clinical control16.
According to the World Health Organization (WHO), DDs currently affect more than 350 million people in the world and are already the second cause of Disability Adjusted Life Years in the age range of 15 to 44 years old in both genders. It is estimated that, in 2020, DDs will occupy the first position in developing countries and the second in developed countries and will be the most important cause of disability in both genders, in any age group, followed by coronary diseases. In 2030, DD is calculated to be the most common disease in the world16.
Depression is already the most common disease in children and adolescents between 10 and 19 years old and is the main cause of disability in both genders. Suicide is one of the three main causes of death in that age range16.
More than 90% of patients who use psychotropic medication use antidepressants with a predominance of women3,11,13.
The association between DDs and suicide is consistent and significant, and the average risk of suicide observed among patients with depression is around 30 times higher than in the general population8,17. It is possible to establish a diagnosis of depression among 20.8% to 35.8% of completed suicides (WHO), and a 60% increase in the rates of suicide in the last decades was observed, considering global data. It is estimated that 90% of the suicides in older adults are associated with some type of mental disease, and the most frequent is depression2,13,16,17.
Etiology
Depression is a mental disorder due to internal conflict and a biochemical alteration in neurons responsible for controlling the mood state and can be triggered by heritable genetic, psychological, environmental, and biochemical factors4.
Associated factors such as urban life; unemployment; physical diseases; prior affective changes; stressful events; loss of loved ones; and use of medication, alcohol, and other drugs may be factors triggering or aggravating DDs11.
In spite of all efforts, the etiology and pathophysiology of DDs are not yet well defined. Imaging studies related to the analysis of the neurobiological and genetic mechanisms of depression have shown promising results.
Diagnosis
Depression is a difficult affective condition to assess. As a clinical entity, it is classified in the ICD-10 and DSM-V in the mood disorder categories18. Its diagnosis should be done clinically by a psychiatrist during an accurate and consistent clinical examination of the patient1,4,9,13,15.
However, in the day-to-day routine, the plastic surgeon, as well as the entire medical class, should be attentive, trained, and prepared to identify not only the physical complaints but also possible psychological symptoms presented by the patient during the consultation.
There are several signs and symptoms (organic and psychological) of depression (Chart 1)1,4,5,8,11-13. The depressed individual, in some cases, may present only with vague and unspecific symptoms, thus hampering diagnosis.
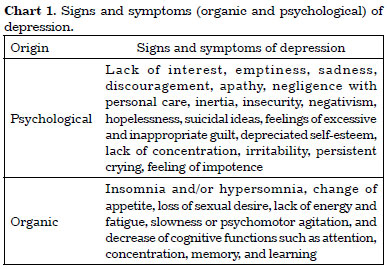
One must observe the nature of the symptoms, use of some type of substance, personal and family history of depression, history of psychiatric hospitalization, use of psychotropic drugs (and who prescribed them), psychotherapy, or even apathetic behavior alternating with euphoria1,4,5,8,9,11-13.
Scales, questionnaires, and inventories contribute substantially in the medical office towards the screening of possible mental diseases including DDs19.
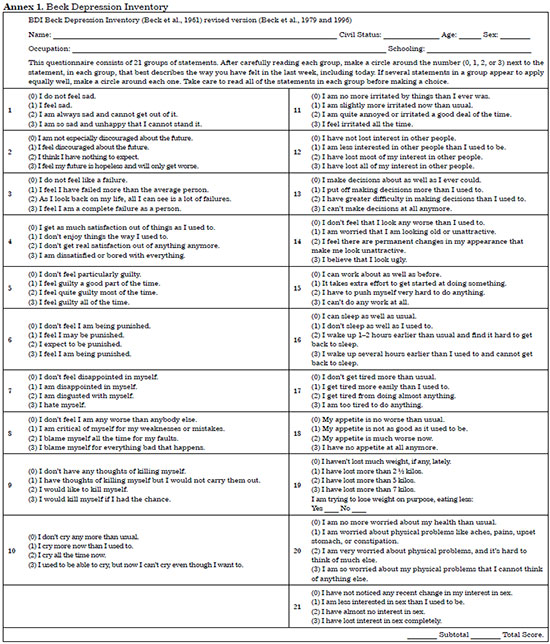
Beck et al.19 developed a questionnaire, the Beck Depression Inventory (BDI), to evaluate the intensity of depression symptoms; the questionnaire presented internal consistency and reliability. It is a practical instrument with a high rate of acceptance, credibility, and accuracy and was translated, adapted, and validated for use in Brazil20.
This is a self-reporting scale containing 21 groups of statements, each item showing symptoms and attitudes at varying intensities from 0 to 3, suggesting increased degrees of depressive symptom severity (Annex 1)20.
The total score is the result of the sum of all item scores and allows the classification of symptomatic intensity levels of depression with a minimum score of 0 and a maximum of 63 points. The operating manual of the BDI proposes a stratification in which the presence of 1 to 9 positive points corresponds to the symptoms of minimal depression (from 10 to 16: mild symptoms of depression, from 17 to 29: symptoms of moderate depression, and 30 or more: symptoms of severe depression). The limit between symptoms of mild and moderate depression (> 17 positive responses) is used as the cut-off point among negative and positive cases as significant risk of depression; however, the manual itself guides that "the cutoff points may vary according to the sample and the purpose of the examiner"19,20.
Correlation of depressive disorder and plastic surgery
When correlating DDs and plastic surgery in the first studies, some authors found extreme values, ranging from 3 to 90%1,2,4,5,8,9. More recent studies have demonstrated less heterogeneity; however, there was a high prevalence of DDs in this population, ranging from 13 to 32% compared to the general population8,10,12,21-25. Approximately 20% of the cosmetic surgery patients reported psychiatric treatment, and 18% used antidepressants2,5,23,24.
PSYCHOPATHOLOGY OF DEPRESSIVE DISORDER AND PLASTIC SURGERY
Currently, DD is considered one of the great challenges of medicine due to its high and growing prevalence, chronicity, and therapeutic implications in the world population16,19-21,23,24,26. Until the advent of AIDS, depression held the incontestable title of "Evil of the Century." However, even devoid now of this pointless honor, it continues to increase without hindrance throughout the world, along with several other mental illnesses.
Some authors have demonstrated that improvements related to cosmetic surgery are confined solely to the physical domain, providing little or no change in psychological functions5,15,25,26. However, a large number of articles have shown that aesthetic surgery can provide benefits to people not only in the relief of physical symptoms but also in the degree of satisfaction with body image, quality of life, self-esteem, social confidence, sexual function, behavior, and reduction of depressive symptoms5-9,10-13,15,21-23.
From a philosophical point of view, the result and level of satisfaction (often subjective) regarding surgery are more directly related to cultural factors and temporal patterns of beauty than an appreciation of the beauty of patients' own body results.
A strong correlation is observed in the day-to-day between the preoperative psychological history and postoperative psychological complications. There is a belief that aesthetic surgery is psychologically safe, and it is not. Psychological complications may occur at rates equal to or greater than physical complications in daily practice. Patients who present physical complications are prone to undergo psychological complications simultaneously22,23.
Patients can progress improperly or even disastrously in the postoperative period, even with an adequate surgical result. Altered psychological states or negative body image can irreparably affect perceptions of satisfaction with a surgical intervention. Postoperative dissatisfaction is generally caused by emotional disappointment through breakage or violation of their expectations or through a psychopathologic façade unnoticed by the surgeon and (usually) not through technical failure3,5.
Patients with lower preoperative psychological alterations seem to obtain better postoperative satisfaction with aesthetic surgery. On the other hand, patients identified with signs of depression in the preoperative period may present up to five times more dissatisfaction with their surgical results in the postoperative period3,4,11,13,15,21,24,25.
Depressive patients may have simple psychosomatic complaints, claims, general dissatisfactions, slight or larger depressive clinical pictures, anger, aggressiveness, and medical processes27,28 and, in extreme cases, may progress to suicide based on the high correlation of depression and suicide16,27-30.
Moved by constant dissatisfaction, some patients request repeated procedures, generating problems for the surgeon such as anguish and burnout. More extreme situations can occur against the professional such as exposure, risk of persecution, body threat, physical violence, and legal actions. The literature even reports cases of surgeons who were murdered by patients who presented symptoms consistent with psychosomatics alterations27,31.
Correlation of implant breast augmentation with depression and suicide
A series of important studies from different countries has been published with the goal of increasing the awareness of the possible mental health problems related to breast implants. Intriguing and alarming data have demonstrated potential risks of increase of suicide in patients submitted to breast augmentation compared to the general population. These findings demonstrated relative risk for suicide in all these studies and may reach up to 4 times higher risk32-38.
However, a cause and effect relationship could not be identified, and nor could the presence of potential preoperative risk factors or psychopathological profiles that could put these women at greatest risk of suicide. It is suggested that this probably occurs due to the sociodemographic traits, psychopathologic history, and specific lifestyles of these patients rather than the presence of the implant itself. Among them, smoking, excessive alcohol consumption, drug dependencies, civil status/divorce, and parity are the main risk factors associated with depression and, consequently, a greater risk for suicide2,3,5,21,23,27,30,32.
Candidates for breast augmentation surgery with implants feature striking personal characteristics with a higher number of depressive symptoms13,23,33,38, psychiatric history39, psychotherapy2,11, psychiatric hospitalization32,39, suicide32-39, and greater use of psychotropic drugs - in particular, antidepressants which are used up to seven times more, when compared with other plastic surgery patients or women in the general population11,22,35. Underlying risk factors and complementary psychopathological characteristics are also observed in this population, including low educational level24,36, behavior disorders, and higher prevalence of eating disorders5,11,22,23.
Patient selection
It is known that the key to success with plastic surgery lies in the preoperative selection of patients, and the key is prevention instead of treatment.
Some authors defend that the psychiatric evaluation should always be performed routinely in all aesthetic surgery patients13.
However, the request for a psychiatric evaluation can, for some individuals, cause distance and malaise in the doctor-patient relationship, creating an embarrassing situation with increased time for preoperative preparation and costs and may seem like an insult or even an aggression8,23.
Not all candidates for aesthetic surgeries have a high probability of psychiatric problems. On the contrary, the great majority presents a high degree of postoperative satisfaction11. The difficulty, then, is to recognize which patients who seek these surgeries have psychological stability, have an established psychiatric disorder (controlled or not), or are even close to being triggered and if these individuals are more prone to experience an exacerbation of psychiatric symptoms in the postoperative period. Recognition and awareness of these profiles (preoperative) constitute the first line of defense of the surgeon in the prevention of postoperative psychological complications11.
Plastic surgeons must be alert to the possible patients who present for the different surgical procedures by means of a well-clarified consultation about their symptoms and their (real) motivations and clinical history, including mental health and some investigative method (questionnaire) in all patients.
The BDI as a self-evaluation measure of depressive symptoms is a useful instrument for the non-specialist, taking an average time of 5 minutes to be answered. Although without diagnostic accuracy (reserved for the psychiatrist), its use may assist in screening and identifying possible patients with DDs and the appropriate forwarding for mental health evaluation by a qualified professional4,13,19,20.
Indicators of patients who have a chance of poor psychosocial development (called "markers" of psychopathology and evaluators of possible negative postoperative evolution) are high degree of demands and expectations about the procedure, constant dissatisfaction or dissatisfaction with their prior aesthetic surgery (with good result), (suspected) candidacy for surgeries with use of breast implants, minimal deformities, failure to understand postoperative evolution and limitations of the technique (primarily adolescents), vague motivations of third parties or based on relationship issues, extreme low self-esteem, history of depression, psychiatric hospitalization, use of antidepressants, higher score on the questionnaire (> 17), personality disorder, lack of companion, and low schooling and income2-15,21,26-39.
It is suggested that all patients with the above characteristics be forwarded to the psychiatrist (preferably with the surgeon's confidence) for a more detailed and enlightening assessment, and a psychiatric opinion should be added to the patient's record, releasing him or her for the surgical act from the point of view of mental health, along with the signed Free and Informed Consent Form. Patients dissatisfied with their postoperative results can use their psychiatric history as part of their judicial action against the surgeon, claiming that their psychiatric framework prevented them from understanding the surgery, limitations, complications, and potential results2,5,11,23,31.
The presence of a history of psychiatric hospitalization represents a strong and important predictive factor of postoperative complications and suicide when compared with the general population30,39.
The impact of surgical procedures in the areas of psychological function remains poorly known, and the relationship between the treatment of DDs and postoperative evolution is unknown5,21. Thus, as long as there are sufficient data for the triage of these patients with well-defined risk factors for psychopathology and suicide, it is prudent to assess each case and forward for psychiatric evaluation patients identified as high risk before the surgical procedure for a more consistent and rigorous evaluation. The psychiatrist shall decide if the patient can undergo the procedure or not and at what moment or if they need specific treatment (psychotherapy and/or drug therapy). The success of the surgery in this population depends on a successful treatment of depression.
For patients who develop DDs in the postoperative period, it is imperative that they be referred immediately to a psychiatrist to limit or control this adverse experience and, thus, promote their well-being.
Contraindicating or postponing a cosmetic surgery in a patient with a possible DD does not mean insecurity or lack of skills or lack of respect for the patient. It means caution, concern, and well-being for the patient and especially wisdom and professional maturity.
CONCLUSION
Cosmetic surgery patients should be evaluated properly for the identification of those with possible DDs preoperatively, thus avoiding an unfavorable postoperative evolution.
COLLABORATIONS
PRP Writing of the manuscript and critical review of its contents.
RFJ Final approval of the study.
MP Conception and design of the study.
CGLN Analysis and interpretation of the data.
FCFA Statistical analysis.
VEBV Critical review of contents.
FSF Bibliographical survey.
REFERENCES
1. Slade PD. What is body image? Behav Res Ther. 1994;32(5):497-502. PMID: 8042960 DOI: http://dx.doi.org/10.1016/0005-7967(94)90136-8
2. Sarwer DB, LaRossa D, Bartlett SP, Low DW, Bucky LP, Whitaker LA. Body image concerns of breast augmentation patients. Plast Reconstr Surg. 2003;112(1):83-90. PMID: 12832880 DOI: http://dx.doi.org/10.1097/01.PRS.0000066005.07796.51
3. McGrath MH, Mukerji S. Plastic surgery and the teenage patient. J Pediatr Adolesc Gynecol. 2000;13(3):105-18. DOI: http://dx.doi.org/10.1016/S1083-3188(00)00042-5
4. Honigman RJ, Phillips KA, Castle DJ. A review of psychosocial outcomes for patients seeking cosmetic surgery. Plast Reconstr Surg. 2004;113(4):1229-37. PMID: 15083026 DOI: http://dx.doi.org/10.1097/01.PRS.0000110214.88868.CA
5. Rohrich RJ. Silicone breast implants: Outcomes and safety update. Plast Reconstr Surg. 2007;120(7):1S-3S. DOI: http://dx.doi.org/10.1097/01.prs.0000286668.18934.37
6. de Brito MJ, Nahas FX, Barbosa MV, Dini GM, Kimura AK, Farah AB, et al. Abdominoplasty and its effect on body image, self-esteem, and mental health. Ann Plast Surg. 2010;65(1):5-10. PMID: 20467297 DOI: http://dx.doi.org/10.1097/SAP.0b013e3181bc30f7
7. Zojaji R, Arshadi HR, Keshavarz M, Mazloum Farsibaf M, Golzari F, Khorashadizadeh M. Personality characteristics of patients seeking cosmetic rhinoplasty. Aesthetic Plast Surg. 2014;38(6):1090-3. PMID: 25270095 DOI: http://dx.doi.org/10.1007/s00266-014-0402-7
8. Shridharani SM, Magarakis M, Manson PN, Rodriguez ED. Psychology of plastic and reconstructive surgery: a systematic clinical review. Plast Reconstr Surg. 2010;126(6):2243-51. DOI: http://dx.doi.org/10.1097/PRS.0b013e3181f445ae
9. Bhugra D, Mastrogianni A. Globalisation and mental disorders. Overview with relation to depression. Br J Psychiatry. 2004;184:10-20. PMID: 14702222
10. Naraghi M, Atari M. A comparison of depression scores between aesthetic and functional rhinoplasty patients. Asian J Psychiatr. 2015;14:28-30. DOI: http://dx.doi.org/10.1016/j.ajp.2015.01.009
11. Sarwer DB, Gibbons LM, Magee L, Baker JL, Casas LA, Glat PM, et al. A prospective, multi-site investigation of patient satisfaction and psychosocial status following cosmetic surgery. Aesthet Surg J. 2005;25(3):263-9. DOI: http://dx.doi.org/10.1016/j.asj.2005.03.009
12. Klassen AF, Pusic AL, Scott A, Klok J, Cano SJ. Satisfaction and quality of life in women who undergo breast surgery: a qualitative study. BMC Womens Health. 2009;9:11. DOI: http://dx.doi.org/10.1186/1472-6874-9-11
13. Vargel S, Uluşahin A. Psychopathology and body image in cosmetic surgery patients. Aesthetic Plast Surg. 2001;25(6):474-8. DOI: http://dx.doi.org/10.1007/s00266-001-0009-7
14. Stone MH. A cura da mente: a história da antiguidade até o presente. Porto Alegre: Artmed; 1999.
15. Saariniemi KM, Kuokkanen HO, Tukiainen EJ. The outcome of reduction mammaplasty remains stable at 2-5 years' follow-up: a prospective study. J Plast Reconstr Aesthet Surg. 2011;64(5):573-6. DOI: http://dx.doi.org/10.1016/j.bjps.2010.09.010
16. World Health Organization. Depression. Geneva: World Health Organization); 2012. [Acesso 2 Fev 2015]. Disponível em: http://www.who.int/topics/depression/en/
17. Gibbons RD, Hur K, Bhaumik DK, Mann JJ. The relationship between antidepressant medication use and rate of suicide. Arch Gen Psychiatry. 2005;62(2):165-72. DOI: http://dx.doi.org/10.1001/archpsyc.62.2.165
18. American Psychiatric Association. DSM-V Diagnostic and Statistical Manual of Mental Disorders. 5ª ed.; 2014 [Acesso 8 Abr 2016]. Disponível em: http://www.dsm5.org/about/Pages/faq.aspx
19. Beck AT, Ward CH, Mendelson M, Mock J, Erbaugh J. An inventory for measuring depression. Arch Gen Psychiatry. 1961;4:561-71. DOI: http://dx.doi.org/10.1001/archpsyc.1961.01710120031004
20. Cunha JA. Manual da versão em português das escalas Beck. 1 ed. São Paulo: Casa do Psicólogo; 2001. p.171.
21. Chahraoui K, Danino A, Frachebois C, Clerc AS, Malka G. Aesthetic surgery and quality of life before and four months postoperatively. Ann Chir Plast Esthet. 2006;51(3):207-10. PMID: 16181718
22. Alagöz MS, Başterzi AD, Uysal AC, Tüzer V, Unlü RE, Sensöz O, et al. The psychiatric view of patients of aesthetic surgery: self-esteem, body image, and eating attitude. Aesthetic Plast Surg. 2003;27:345-8.
23. McGrath MH. The psychological safety of breast implant surgery. Plast Reconstr Surg. 2007;120(7 Suppl 1):103S-109S.
24. Javo IM, Sørlie T. Psychosocial predictors of an interest in cosmetic surgery among young Norwegian women: a population-based study. Plast Reconstr Surg. 2010;126(2):687-8.
25. Von Soest T, Kvalem IL, Skolleborg KC, Roald HE. The effects of cosmetic surgery on body image, self-esteem, and psychological problems. J Plastic Reconstr Aesth Surg. 2009;62(10):1238-44.
26. O'Blenes CA, Delbridge CL, Miller BJ, Pantelis A, Morris SF. Prospective study of outcomes after reduction mammaplasty: long-term follow-up. Plast Reconstr Surg. 2006;117(2):351-8. PMID: 16462312
27. Goin MK, Rees TD. A prospective study of patients' psychological reactions to rhinoplasty. Ann Plast Surg. 1991;27(3):210-5. PMID: 1952747
28. Leonardo J. New York's highest court dismisses BDD case. Plast Surg News. 2001;1-9.
29. Sher L, Oquendo MA, Mann JJ. Risk of suicide in mood disorders. Clin Neurosci Res. 2001;1(5):337-344.
30. Bertolote JM, Fleischmann A. Suicide and psychiatric diagnosis: a worldwide perspective. World Psychiatry. 2002;1(3):181-5.
31. Gorney M. Ten years' experience in aesthetic surgery malpractice claims. Aesthet Surg J. 2001;21(6):569-71. DOI: http://dx.doi.org/10.1067/maj.2001.121244
32. Joiner TE Jr. Does breast augmentation confer risk of or protection from suicide? Aesthet Surg J. 2003;23(5):370-5. PMID: 19336102 DOI: http://dx.doi.org/10.1016/S1090-820X(03)00213-9
33. Koot VC, Peeters PH, Granath F, Grobbee DE, Nyren O. Total and cause specific mortality among Swedish women with cosmetic breast implants: prospective study. BMJ. 2003;326(7388):527-8. DOI: http://dx.doi.org/10.1136/bmj.326.7388.527
34. Pukkala E, Kulmala I, Hovi SL, Hemminki E, Keskimäki I, Pakkanen M, et al. Causes of death among Finnish women with cosmetic breast implants, 1971-2001. Ann Plast Surg. 2003;51(4):339-42. DOI: http://dx.doi.org/10.1097/01.sap.0000080407.97677.A
35. Breiting VB, Hölmich LR, Brandt B, Fryzek JP, Wolthers MS, Kjøller K, et al. Long-term health status of Danish women with silicone breast implants. Plast Reconst Surg. 2004;114(1):217-26; discussion 227-8. DOI: http://dx.doi.org/10.1097/01.PRS.0000128823.77637.8
36. Brinton LA, Lubin JH, Murray MC, Colton T, Hoover RN. Mortality rates among augmentation mammoplasty patients: an update. Epidemiology. 2006;17(2):162-9. DOI: http://dx.doi.org/10.1097/01.ede.0000197056.84629.1
37. Villeneuve PJ, Holowaty EJ, Brisson J, Xie L, Ugnat AM, Latulippe L, et al. Mortality among Canadian women with cosmetic breast implants. Am J Epidemiol. 2006;164(4):334-41. PMID: 16777929 DOI: http://dx.doi.org/10.1093/aje/kwj214
38. Lipworth L, Kjøller K, Hölmich LR, Friis S, Olsen JH, McLaughlin JK. Psychological characteristics of Danish women with cosmetic breast implants. Ann Plast Surg. 2009;63(1):11-4. DOI: http://dx.doi.org/10.1097/SAP.0b013e318185731
39. Appleby L, Shaw J, Amos T, McDonnell R, Harris C, McCann K, et al. Suicide within 12 months of contact with mental health services: national clinical survey. BMJ. 1999;318(7193):1235-9. PMID: 10231250 DOI: http://dx.doi.org/10.1136/bmj.318.7193.1235
1. Universidade Federal de Goiás, Goiânia, GO, Brazil
2. Hospital das Clínicas, Universidade Federal de Goiás, Goiânia, GO, Brazil
3. Sociedade Brasileira de Cirurgia Plástica, São Paulo, SP, Brazil
Institution: Faculdade de Medicina, Universidade Federal de Goiás, Goiânia, GO, Brazil.
Corresponding author:
Paulo Renato de Paula
Rua T-50, 540 - Setor Bueno
Goiânia, GO, Brazil Zip Code 74215-200
E-mail: p-renato@uol.com.br
Article received: July 12, 2015.
Article accepted: October 22, 2015.
Conflicts of interest: none.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter