

Original Article - Year 2016 - Volume 31 -
Forehead reduction in patients with precapillary incision: 10 years of experience
Redução frontal em pacientes submetidos à incisão pré-capilar: 10 anos de experiência
ABSTRACT
INTRODUCTION: The long forehead gives a less harmonious appearance, seems disproportionate and characterizes the aging face. Surgical procedures for frontal reduction with precapillary incision present insightful information and provide harmonious and pleasant restoration of the frontal region. This study evaluated results obtained in patients who underwent frontal reduction using precapillary incision at Daher Hospital plastic surgery service within the last ten years.
METHODS: This was a retrospective longitudinal study. The surgical technique entailed a careful dissection of the bilateral supraorbital ridge. The scalp was dissected in the parietoccipital region in order to easily move forward the flap. The vigorous hemostasis and resection of excessive flap were performed. In the end, synthesis of plans were performed.
RESULTS: The age of patients ranged from 48 to 76 years, the mean age was 58 years. Mean surgical time was 3 hours and 38 minutes. No complications were seen such as hematoma, flap necrosis, supratrochlear nerve injury, alopecia, infections, deep vein thrombosis, pulmonary embolism and/or dehiscence. Four patients (7%) had seroma that was drained. The symmetric of eyebrows and scars positioning was considered satisfactory in both assessment by patients and the technical evaluator.
CONCLUSION: The aesthetic results in patients who underwent frontal reduction by precapillary incision were satisfactory. The choice of the ideal patient was crucial for success of the surgery.
Keywords: Rhytidoplasty; Rejuvenation; Forehead.
RESUMO
INTRODUÇÃO: A testa longa confere uma aparência menos harmônica, desproporcional e caracteriza o envelhecimento. Procedimentos cirúrgicos para redução frontal com incisão pré-capilar apresentam indicações criteriosas e proporcionam a restauração harmônica da região frontal. O estudo avalia os resultados obtidos em pacientes submetidos à redução frontal por incisão pré-capilar no serviço de cirurgia plástica do Hospital Daher nos últimos dez anos.
MÉTODOS: Trata-se de um estudo observacional longitudinal retrospectivo. A técnica cirúrgica consiste em uma dissecção cuidadosa até o rebordo supraorbital bilateral. O couro cabeludo é dissecado até a região parietoccipital de forma a avançar com facilidade o retalho. Procede-se à hemostasia vigorosa e ressecção do retalho excedente. Por fim, realiza-se a síntese por planos.
RESULTADOS: A faixa etária das pacientes variou de 48 a 76 anos, com média de 58 anos. O tempo médio operatório foi de 3 horas e 38 minutos. Não foram observadas complicações como hematoma, necrose do retalho, lesão do nervo supratroclear, alopécia, infecções, trombose venosa profunda, embolia pulmonar e/ou deiscências. Quatro pacientes (7%) apresentaram seroma, os quais foram todos drenados. A simetrização das sobrancelhas e a posição das cicatrizes foram consideradas satisfatórias tanto pela avaliação feita pelos pacientes quanto pela avaliação técnica.
CONCLUSÃO: Os resultados estéticos obtidos em pacientes submetidos à redução frontal pela incisão pré-capilar foram satisfatórios. A escolha do paciente ideal foi fundamental para o bom sucesso operatório.
Palavras-chave: Ritidoplastia; Rejuvenescimento; Testa.
The long forehead gives a less harmonious appearance, seems disproportionate and characterize the aging face, factors that causes significant cosmetic concern in both sexes1,2. The proportions and facial aesthetic units are defined and used to evaluate the size of the forehead, which segment extends from the front to the glabella capillary implantation2,3.
Different surgical methods have been described in the literature to alleviate this condition by providing the rejuvenation of the frontal region (mainly in patients who have a high capillary line implantation)2,3. However, no technique reported so far present satisfactory final results4.
Some reports on front rhytidectomy for the treatment of long forehead describe the use of coronal incision with subgaleal or subcutaneously dissection, and endoscopic surgical techniques. However, such actions result in the rise of the previous line of the hair, and this the part of the reason that many surgeons do not routinely recommend these procedures 5,6.
To prevent the increase of the previous hairline, in certain situations and criterions surgical indications, the precapillary incision constitutes an option. Patients with brow ptosis, recession of the front line or frontal wrinkles patients are ideal for this surgical procedure7.
OBJECTIVE
To evaluate results obtained in selected patients for the last ten years by forehead reduction using precapillary incision.
METHODS
This was a retrospective longitudinal study from March 2006 to March 2016 carried out in the plastic surgery service at Daher Hospital in the city of Brasília, DF, Brazil.
The research project followed all legal procedures established by the National Health Council Resolution 196/96, and also guidelines of researches involving human subjects. This study is in accordance with the principles of the Declaration of Helsinki.
Our sample was intentional and included patients with long brow who underwent facial rhytidectomy with forehead reduction by precapillary incision.
We evaluated the following variables gender, age, duration of the surgery, complications after the surgery, treatment of forehead muscles, positioning of scar precapillary incision, size of the resection of the end of flap, length of hospital stay and satisfaction of medical staff and patient with scars and surgery.
Criteria used in this study for the surgery were:
1) Patients with ptosis of eyebrow and thin and scarce front hair;Surgical Technique
2) Patients with congenital long forehead;
3) Patients with accentuated forehead wrinkling.
Patients were initially examined in orthostatic position to assess the degree of ptosis of eyebrows and in order plan surgery of the intended reduction of the forehead. The broken type incision [I couldn't confirm this term, please check with authors] was selected in the previous line of hair immediately after hair junction with the forehead (Figure 1).
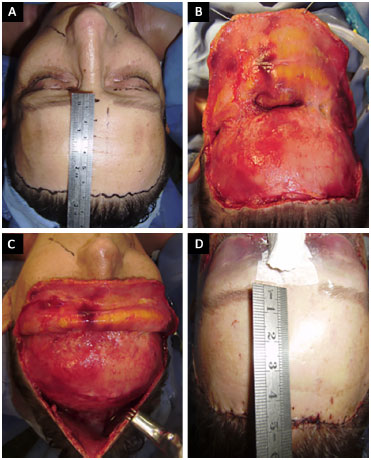
Figure 1. A: Marking of precapillary break type incision with initial measurement of front; B: Dissection of frontal region. C: Scalp; D: Final aspect with new measurement after creation of advancement flap.
All procedures were performed in the surgical room with patients under general anesthesia. The surgical team included a senior surgeon and two assistants.
Local infiltration was performed using 0.9% saline and epinephrine in a 1: 200.000 in the incision site and in areas to be dissected. A subgaleal incision was then performed following the marking of the skin and arrangement of the hair follicles.
A careful dissection with Metzenbaum scissors was performed to separate the skin from strongly adhered septal of the frontal muscle. The atraumatic tissue handling was required to prevent vascular compromise. Dissection was extended to the bilateral supraorbital ridge and could be extended until the nasal dorsum if necessary. The scalp was dissected up to the parietooccipital area to allow the easily advance of the flap.
Treatment of frontal muscles, corrugators and procerus was performed when needed. Surgical team gave special attention to the supratrochlear nerve and vessels of the region to avoid unintentional injury.
A vigorous hemostasis was performed for subsequent repositioning of the flap. The excessive skin was removed gradually to avoid excessive tension on the scar. We used 4-0 and 5-0 nylon for suture.
After the surgery we used compressive dressing cushion. Surgical drains were not used, and suture was removed between 7 and 10 days after the surgery.
Assessment of Satisfaction Level
The assessment of the degree of patients' satisfaction with the result of the surgery was obtained 3 months after the procedure.
The evaluation of technical result was done by a plastic surgeon member of the Brazilian Society of Plastic Surgery (who did not participate in surgical procedures). This evaluation used a comparative analysis of preoperative images with postoperatively images 3 months later.
Statistical Analysis
Results were organized in a Microsoft Excel 2008 spreadsheet and analyzed using the Epi Info program, version 3.5.1. A descriptive analysis of the data was carried out, and frequencies are presented.
RESULTS
From March 2006 to March 2016, 60 patients underwent surgical procedure of the forehead reduction. Of these, two were men and 58 were women (Table 1).

The age of patients ranged from 48 to 76 years, with an average of 58 years.
The mean time of surgery was 3 hours and 38 minutes. Hospital stay was 24 hours for all patients. The size of the resection edge of flap ranged from 2 to 3 cm.
Treatment of frontal muscles, corrugators and procerus was necessary in 46 cases. Four cases had seroma formation after the surgery that was treated with punctures and local drainage.
Temporary paresthesia was seen in 80% of cases, of these 68.75% had sensory recovery within 6 months and 31.25% 1 year after the surgery.
Two cases presented scar enlargement (one man and one woman), three cases of unpigmented scar (women). No cases of hypertrophic scars and/or keloids were seen.
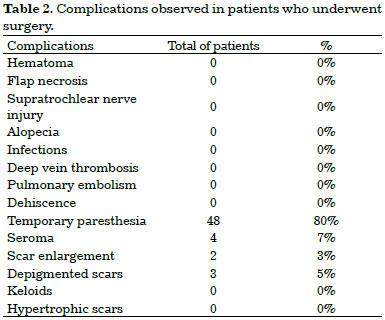
No surgical complications were seen such as hematoma, flap necrosis, supratrochlear nerve injury, alopecia, infections, deep vein thrombosis (DVT), pulmonary embolism and/or dehiscence (Table 2).
Results immediate after the surgery were satisfactory regarding the positioning and symmetrization of eyebrows in front rhytidectomies.
Patients were followed-up after the surgery for a period ranging from 3 months to 8 years, mean follow-up of 3.5 years.
In outpatient follow-up, 88.3% of patients showed to be satisfied with the final result and without complaints regarding the size and placement of the scars. No case was observed related to raising of the anterior hairline. The technical evaluation achieved 90% of satisfaction with the final result in terms of positioning of the scars and symmetrization of the eyebrows.
Figures 2 to 5 illustrate some cases included in this study.
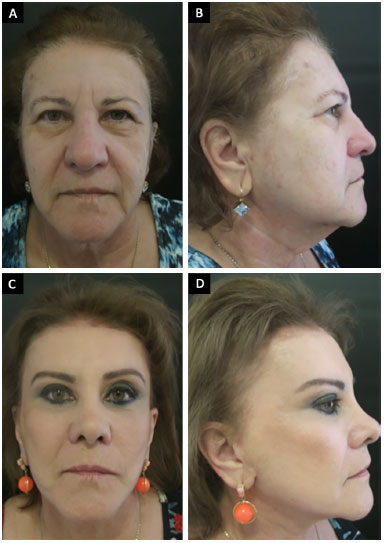
Figure 2. A 62-year-old patient who underwent frontal reduction with precapillary incision and treatment of frontal muscles, corrugators and procerus. A and B: Preoperative; C and D: 3 years after the surgery.
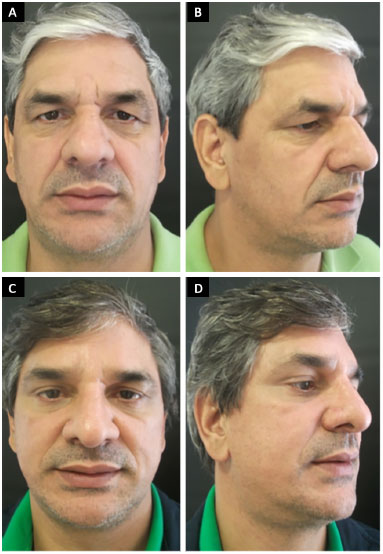
Figure 3. A 53-year-old patient who underwent fronta reduction with precapillary incision and treatment of fronta muscles, corrugators and procerus. A and B: Preoperative; C and D: 2 years after surgery.
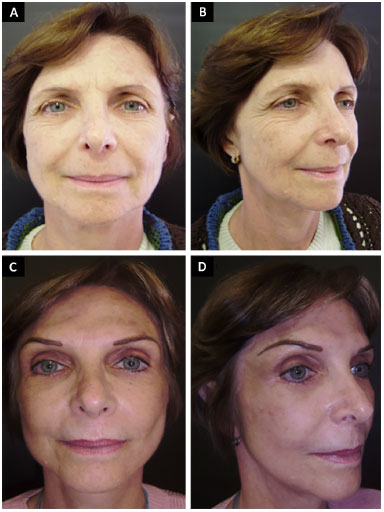
Figure 4. A 50-year-old patient who underwent frontal reduction with preccapillary incision. A and B: Preoperative; C and D: 4 years after surgery the symmetric eyebrows are evident.
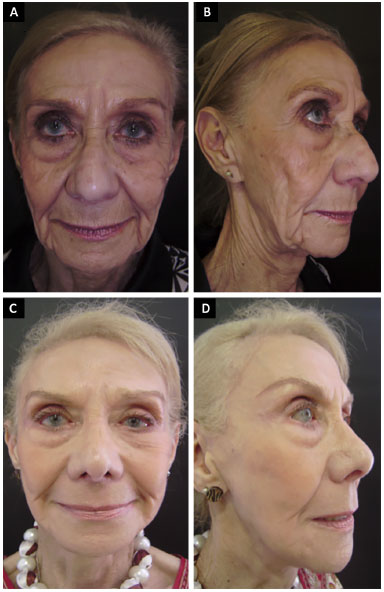
Figure 5. A 76-year-old patient who underwent frontal reduction with precapillary incision and treatment of frontal muscles, corrugators and procerus. A and B: Preoperative; C and D: 2 years after surgery.
DISCUSSION
Men and women have aesthetic concerns with their image because this interferes with their social life and constitutes an important factor for integration and maintenance in the job market8. For this reason, progress has been seen in the surgical procedures on the face, especially in the ancillary procedures as first reported by Hunt in 19269.
These data corroborate with results obtained in our study, because from 60 surgical procedures performed, 2 were performed in male patients and 58 female patients; patients mean age was 58 years.
A high capillary implantation line may cause both facial disproportion and contribute to the appearance of aging in patients. Surgical repositioning with local muscle treatment, when necessary, restores the harmonious of the face and promotes a pleasant facial appearance2,3.
Some cases require the combined treatment of the muscle groups of the front area because with aging some dynamic wrinkles may appear. The dynamic wrinkles are properly treated and softened with the use of botulinum toxin, but static wrinkles require other therapies such as fillers and surgical procedure, either endoscopic or open (conventional) surgery2.
In our study, 46 patients underwent forehead reduction procedure associated with treatment of forehead muscles for better matching the results.
In many institutions, the endoscopic technique has become the most performed procedure, for this reason, the conventional technique is taking the role of unknown, which creates certain stereotypes that could not replace knowledge and experience6.
The conventional surgery can be done by various incisions. The use of broken incision in the anterior frontal line is a good way of approaching since it allows a better scar appearance, preserve hair follicles in the distal flap and promote the growth of new targeted hair through proximal and anterior flange to the scar7.
We emphasize that the procedure described in our study requires an individualized approach that is needed to improve the results. In patients with normal pattern of hair and previous low hair insertion line, the literature shows that endoscopic technique or bicoronal incision provide satisfactory cosmetic result. However, patients with previous high hairline insertion (long forehead), very thin extensive wrinkling or skin, the best indication is the precapillary incision10.
In our experience with this procedure, we conducted extensive subgaleal detachment to the advancement of the forehead flaps and scalp, which does not need rigid fixation (screws) of the flap.
No surgical complications were observed in our study such as hematoma, flap necrosis, facial nerve injury, alopecia, infection, deep vein thrombosis (DVT), pulmonary embolism and / or dehiscence. Four cases had formation of seroma and they were properly treated with punctures and drainages without compromising the final aesthetic result. In 80% of cases temporary paresthesia were reported, but all reversed within 1 year. We believe that a vigorous hemostasis associated with surgical technique care were key factors to prevent complications.
In terms of satisfaction and scar positioning, we obtained similar results as described by Marten11, which highlight that complications that may perhaps occur in conventional procedures, such as hematoma, seroma, paresthesia, hair loss, flap necrosis, poor scar quality and excessive elevation of eyebrows.
All patients in our study who underwent surgical procedure were informed about the position and the size of the scar along the capillary implantation line, and 88.3% of them were satisfied with the scar placement, which confirms the feasibility of using this technique based on the satisfactory results obtained.
Although we did not use objective means to measure results, our study achieved high percentage of satisfaction both from patients (88.3% of cases) and from the plastic surgeon who evaluated final results (90% of cases), which are similar to other studies in the literature that used the same techniques11.
These findings corroborate the fact that, when properly indicated, the precapillary incision reestablishes a pleasant and harmonious appearance of the front segment, prevents flap displacement, provides symmetry in the positioning of eyebrows and maintains the line of hair implantation in the same place, as observed in cases of evaluted 6 years after the surgery.
The statement that the open techniques implies a number of "difficulties", low patient acceptance and high morbidity, as frequently reported in the literature, should not be taken as an absolute truth, mainly because of the satisfactory results obtained in this study showing that in experienced hand, the conventional technique provides results with low rates of complications6,12,13.
CONCLUSION
The forehead reduction procedure with precapillary incision is indicated for patients with brow ptosis, thin and scarce frontal hair, those who had long congenital forehead and patients with broad forehead wrinkling.
The satisfactory results report in our study clarify the safety and feasibility of the technique that allows the symmetrically raising of eyebrows, tension-free closure, reasonable scars, and good access for treatment of underlying muscles.
We emphasize the importance of correct identification of patients to perform the procedure in order to achieve success in surgery.
COLLABORATIONS
JNRN Contributed with activities and/or experiments of the study.
DASS Statistical analyses, conception and design of the study, drafting the manuscript or critical review of the content.
DBP Analyses and/or interpretation of data.
BPE Drafting the manuscript or critical review of the content.
IRJ Conception and study of the study.
LGM Conception and study of the study.
LMCD Conception and study of the study.
JCD Approval of final manuscript.
REFERENCES
1. Guyuron B, Gatherwright J, Totonchi A, Ahmadian R, Farajipour N. Cessation of hairline recession following open forehead rejuvenation. Plast Reconstr Surg. 2014;133(1):1e-6e.
2. Rodrigues Neto JN, Pedroso DB, Vasconcelos FRP, Cintra Júnior R, Borgatto MS, Câmara Filho JPP. Redução da região frontal com incisão pré-capilar: relato de experiência e indicações. Rev Bras Cir Plást. 2012;27(2):238-42.
3. Marten TJ. Hairline lowering during foreheadplasty. Plast Reconstr Surg. 1999;103(1):224-36.
4. Price VH. Androgenetic alopecia in women. J Investig Dermatol Symp Proc. 2003;8(1):24-7.
5. Connell BF, Lambros VS, Neurohr GH. The forehead lift: techniques to avoid complications and produce optimal results. Aesthetic Plast Surg. 1989;13(4):217-37.
6. Puig CM, LaFerriere KA. A retrospective comparison of open and endoscopic brow-lifts. Arch Facial Plast Surg. 2002;4(4):221-5.
7. Guyuron B, Davies B. Subcutaneous anterior hairline forehead rhytidectomy. Aesthetic Plast Surg. 1988;12(2):77-83.
8. Rees TD, Wood-Smith D. Cosmetic facial surgery. Philadelphia: Saunders; 1973.
9. Hunt HL. Plastic surgery of the head, face and neck. Philadelphia: Lea & Febiger; 1926.
10. Dayan SH, Perkins SW, Vartanian AJ, Wiesman IM. The forehead lift: endoscopic versus coronal approaches. Aesthetic Plast Surg. 2001;25(1):35-9.
11. Marten TJ. Hairline lowering during foreheadplasty. Plast Reconstr Surg. 1999;103(1):224-36.
12. Farkas LG, Kolar JC. Anthropometrics and art in the aesthetics of women's faces. Clin Plast Surg. 1987;14(4):599-616.
13. De Cordier BC, de la Torre JI, Al-Hakeem MS, Rosenberg LZ, Gardner PM, Costa-Ferreira A, et al. Endoscopic forehead lift: review of technique, cases, and complications. Plast Reconstr Surg. 2002;110(6):1558-68.
1. Sociedade Brasileira de Cirurgia Plástica, São Paulo, SP, Brazil
2. Hospital Daher Lago Sul, Brasília, DF, Brazil
Institution: Hospital Daher Lago Sul, Brasília, DF, Brazil.
Corresponding author:
Daniel Augusto dos Santos Soares
CCSW 02, Lote 03, Edifício Unique Duplex, Apt 105 - Sudoeste
Brasília, DF, Brazil Zip Code 70680-250
E-mail: daniel.soares@globo.com
Article received: September 17, 2016.
Article accepted: October 30, 2016.
Conflicts of interest: none.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter