

Original Article - Year 2016 - Volume 31 -
Abdominoplasty with corset plication
Abdominolipoplastia com plicatura em espartilho
ABSTRACT
INTRODUCTION: Abdominoplasty is one of the most common plastic surgery procedures used worldwide. It covers the esthetic appearance and reconstruction of the abdominal wall. Many variations of the incisions, musculofascial repair, and remodeling of the navel have been described. In 1965, Callia performed an incision on the pubis with lateral extensions. In 1967, Pitanguy performed a low horizontal incision with the extremities out and down, and promoted the plication of the rectus abdominis muscles without opening the aponeurosis. Besides demonstrating the ease of implementation and safety of the procedure, the objective of this study was to perform classical abdominoplasty in combination with median and external pararectal plications, also referred to as a corset technique, to recover abdominal wall tension and then liposuction at the end of the procedure to improve abdominal body contour.
METHODS: Sixty-two women with a mean age of 37 years underwent operation between 2011 and 2013.
RESULTS: None of the women in the present study had hematoma, infection, necrosis, or epidermolysis. Late encapsulated seroma was observed in one patient. Five patients had a "dog ear," and eight had unsightly scars but no keloid. All the patients were satisfied with the surgical outcome.
CONCLUSION: The technique described in this study adds two more plications to the classic abdominoplasty, which lead to higher tension in the abdominal wall and more satisfactory esthetic results. Besides being easy to implement, the technique enables lower positioning of the suprapubic transverse incision, which can be easily hidden even with short clothing.
Keywords: Lipectomy; Abdominal muscles/surgery; Abdominal wall/surgery; Abdominoplasty.
RESUMO
INTRODUÇÃO: Abdominoplastia é um dos procedimentos mais realizados na Cirurgia Plástica mundial. Abrange o aspecto estético e reconstrutor da parede abdominal. Muitas variações das incisões, do reparo musculofascial e da remodelagem do umbigo têm sido descritas. Em 1965, Callia realizou incisão sobre o púbis com prolongamentos laterais. Em 1967, Pitanguy fez incisão horizontal baixa com as extremidades para fora e para baixo e promoveu a plicatura dos músculos retos abdominais sem a abertura da aponeurose. O objetivo deste estudo foi realizar abdominoplastia clássica associada às plicaturas mediana e pararretais externas para recuperar a tensão da parede abdominal - técnica em espartilho - e também à lipoaspiração ao final do procedimento, no intuito de melhorar o contorno corporal abdominal, além de mostrar a facilidade de execução e a segurança do procedimento.
MÉTODOS: Foram operadas 62 mulheres no período de 2011 a 2013, com idade média de 37 anos.
RESULTADOS: Não houve hematoma, infecção, necrose ou epidermólise no presente estudo. Observou-se a presença de seroma encapsulado tardio em uma paciente. Houve cinco casos de "dog ear", oito de cicatrizes inestéticas, mas nenhuma queloideana. Todas as pacientes sentiramse satisfeitas.
CONCLUSÃO: Esta técnica agregou mais duas plicaturas musculares à abdominoplastia clássica, levando a uma maior tensão na parede abdominal, com resultado estético mais satisfatório. Conseguiu-se um posicionamento mais baixo da incisão transversal suprapúbica, que pode ser facilmente oculta por roupas menores, além da facilidade de execução.
Palavras-chave: Lipectomia; Músculos abdominais/cirurgia; Parede abdominal/cirurgia; Abdominoplastia.
Abdominoplasty is one of the most frequently performed plastic surgery procedures worldwide. It covers not only the esthetic aspect but also reconstruction of the abdominal wall. Esthetic aspects include abdominal body contour, natural appearance of the navel, and proper location of the scars. The reconstructive component includes recreating the anatomical position of the fascia and musculature, and restoring other deformities that may be present1.
In addition to umbilical repositioning, the surgery consists of low abdominal dermolipectomy, associated with repair or musculofascial plastic surgery, which is achieved with the plication of the aponeuroses of the rectus abdominis muscles. Many variations of the incisions, musculofascial repair, and navel remodeling have been described2,3.
Since 1899, several authors have described abdominoplasty techniques, with tactical variants that require collaboration with specialists. In 1965, Callia4,5 performed an incision of the pubis with lateral extensions; this procedure was then used by other surgeons. Pitanguy6,7 performed a low horizontal incision with the ends out and down. In addition, he promoted the plication of the rectus abdominis muscles without opening the aponeurosis, contributing to the improvement of the result of abdominoplasty.
Franco and Rebello8,9 performed dermolipectomy in combination with a submammary incision called an inverted abdomen. Sinder10,11 reported anterior marking of the abdomen with a triangle, only removing the inferior flap after the detachment of the upper flap and positioning the scar thereafter. Planas12 described a technique similar to that of Sinder10, 11, called "vest over pants."
Psillakis13 described the treatment of muscleaponeurotic flaccidity where the oblique muscle is sutured to the fascia of the rectus abdominis muscle. Illouz14,15 presented for the first time in Brazil, at the Brazilian Congress of Plastic Surgery, in Fortaleza, a liposuction technique that then became part of abdominal dermolipectomy in order to obtain a more satisfactory esthetic result.
Hakme16 performed liposuction with partial abdominoplasty, denominating it as mini lipoabdominoplasty and abdominoplasty. Avelar17-19 described liposuction with abdominoplasty for patients with a protruding abdomen, supraumbilical and infraumbilical localized fat, and muscle flaccidity. Baroudi et al.20,21 proposed the use of quilting sutures by attaching the flap to the abdominal wall, from the xiphoid process to the inferior border of the pubis incision, to prevent seroma.
Matarasso22 described liposuction with abdominoplasty performed to preserve the blood supply of the abdominal flap. Avelar17,18 published his work on liposuction with abdominoplasty without detachment. Nahas23,24 presented a plication of the external oblique muscles in the region of the semilunar line and later presented a study to determine effective techniques for correction of abdominal wall defects and deformities.
Saldanha et al. and Avelar17,18,25,26 in parallel studies presented abdominoplasty techniques without detachment, introducing lipoabdominoplasty techniques in the clinical setting. Bozola and Psillakis, in 1988,27 and Rosa and Bozola, in 2010,28 emphasized the classification of esthetic changes attained with their specific treatments for the abdomen. Nahas and Ferreira29 showed the long-term efficacy of correction of diastasis of the rectus abdominis muscles. In 2010, the same authors30 called attention to factors related to flaccidity of the abdominal wall.
In this study, we performed classic abdominoplasty in combination with medial and external pararectal plications, a technique we call "corset abdominoplasty," to recover the abdominal wall tension and then liposuction at the end of the procedure to improve abdominal body contour13. In addition, we demonstrate the ease of execution and safety of the procedure. The name of the technique arose from the similarity of the plications to a corset, a female fashion piece used to highlight the abdominal contour (Figure 1).
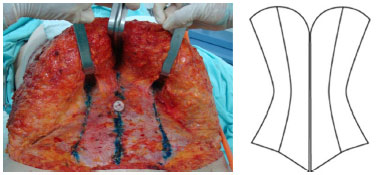
Figure 1. Similarity between a corset and abdominal plicatures.
The main vascularization of the abdominal flap occurs through the perforating arteries of the rectus abdominis muscles17,25,31. The tunnels required for lateral plications are performed at the confluence of the aponeuroses of the external, internal, and transverse oblique muscles, lateral to the fibers of the rectus abdominis muscle and its perforating arteries, avoiding impairment of the vascularization of the flap. This area is also called the semilunar line or Spigelian line32 (Figure 2).
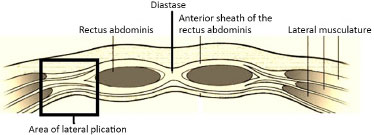
Figure 2. Confluence of the external, internal, and transverse oblique muscles, lateral to the fibers of the rectus abdominis muscles.
OBJECTIVE
The objectives of this study were to present a technique of classic abdominoplasty with medial and external medial plications in combination with liposuction at the end of the procedure and to evaluate the esthetic results of the technique and the associated complications.
METHODS
Between February 2011 and December 2013, 62 cases of abdominolipoplasty with corset plication were performed either in combination with other surgeries or as a single procedure. All the patients were female, aged between 21 and 53 years (mean, 37 years). The procedures were performed by the same surgical team. All the patients were referred for preoperative clinical evaluation of surgical-cardiac risk and pre-anesthetic evaluation. Their weights were measured, and photographic documentation was accomplished.
All the patients provided written informed consent after resolving all doubts in relation to the procedure, being deemed suitable for surgery. The study followed the principles of the Declaration of Helsinki.
Surgical markings were made with the patient in the supine position, and the surgeries were performed under neuraxial block (spinal or epidural) and sedation and/or general anesthesia, with prophylactic antibiotic therapy during anesthetic induction and every 3 h during the procedure.
Compression stockings (¾) and a venous compression device at 60 mm Hg were routinely used. Antithrombotic prophylaxis therapy (enoxaparin 40 mg) was administered in accordance with the modified protocol of Sandri33-35 (Annex 133) and maintained daily until normal ambulation of the patient.
With the patient in the lateral decubitus position, infiltration of a vasoconstrictor solution (saline solution at 0.9% with epinephrine 1:500,000 IU) was initiated. Then, liposuction of the flanks or back, depending on the need, was performed.
In the dorsal decubitus position, the patient underwent incision of the marked area (periumbilical and low abdominal) with a no. 15 scalpel blade. With electrocautery, pre-aponeurotic detachment was attained in a semicircle up to approximately 2 cm above the navel. Selective detachment of the supraumbilical flap was started in a tunnel with a width necessary to correct diastasis (Figure 3).
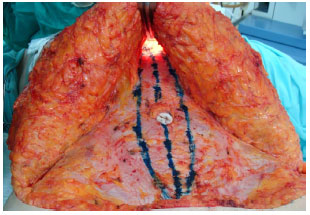
Figure 3. Area of detachment and the median tunnel usually performed in abdominoplasty.
Medial plication of the rectus abdominis muscles in the upper and lower limbs was initiated by using 0 polypropylene wires (Prolene-). After the medial plication, the lateral tunnels were detached from the edges of the rectus abdominis muscles (Spigelian line). This maneuver keeps intact the perforating vessels of the rectus abdominis muscles that supply the flap.
Next, lateral plications were started with 0 polypropylene wires, which originate at the costal borders and terminate approximately at the height of an imaginary line joining the anterior superior iliac spines (Figure 4). A dermal fat flap resection was performed with lower traction of the flap.
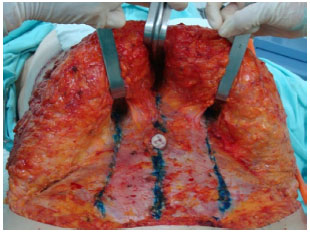
Figure 4. Complete plications (corset appearance). Note the preservation of the area on the rectus abdominis muscles where the perforating vessels exit to supply the flap.
Next, the new position of the navel on the flap was marked. Closure was performed on four planes, the first two with Vicryl- 2.0 covering the fascia of Scarpa, lamellar fat, and areolar fat. Subdermal suture was accomplished with Monocryl-3.0; and intradermal suture, with Monocryl-4.0.
A diamond-shaped incision was made for the new positioning of the navel and pubic incision in the midline between the commissure and the newly formed horizontal scar. Subsequently, infiltration with 0.9% saline solution with adrenaline 1:500,000 IU and liposuction of the flap and pubis were performed by using the two incisions (umbilical and pubic) for the entry of the 4- and/or 5-mm cannulas (Figure 5).
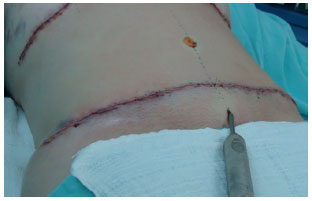
Figure 5. Pubic orifice for liposuction where the continuous suction drain will be placed.
A suction drain was placed with a closed system through the pubic incision, which remained with the patient for approximately 7 days (Figure 6).
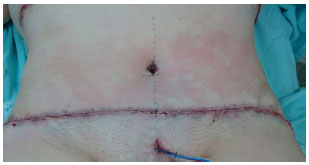
Figure 6. Positioning of the drain through the pubic incision and final aspect of the surgery.
Still in the surgical block, a dressing was laced on the scars and the modeling corset was placed. Surgeries lasted approximately 4 h. The patients were encouraged to walk on the same day of surgery and discharged the next morning.
RESULTS
Among the 62 patients who underwent operation, none had hematoma, infection, necrosis, or epidermolysis. Despite the use of the drain for approximately 7 days after surgery, the presence of late encapsulated seroma (Morel-Lavallée cyst) was observed in one patient, requiring a new surgical procedure for its removal. Five cases of "dog ear" were observed in the side edges of the scar, and eight cases of unsightly scars were observed by the physician and/or patient. For these cases, surgical revisions were performed under local anesthesia. None of the patients developed a keloid scar (Figure 7).
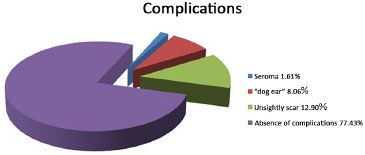
Figure 7. Complication rate.
In the subsequent consultations, the patients were greatly satisfied with the results obtained, although this satisfaction was not reported in response to individual and confidential questionnaires but only through an interview between the physician and the patient during the postoperative follow-up. Even in the cases where unsightly scars were corrected, the level of satisfaction was high, considering the final results (Figures 8-13).
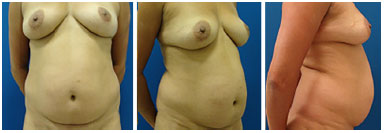
Figure 8. Preoperative front, profile, and side views.
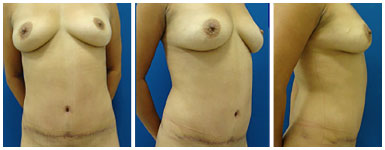
Figure 9. Three-month postoperative period: front, profile, and side views.
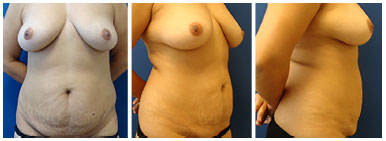
Figure 10. Preoperative front, profile, and side views.
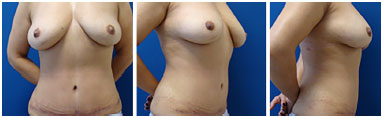
Figure 11. Three-month postoperative period: front, profile, and side views.
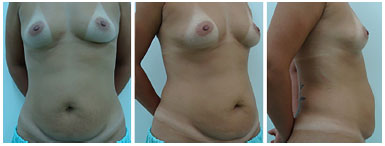
Figure 12. Three-month preoperative period: front, profile, and side views.
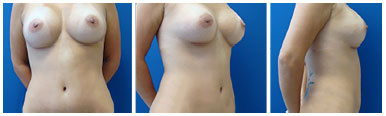
Figure 13. Three-month postoperative period: front, profile, and side views. Purposely showing the low position of the scar, which can be naturally hidden with a short garment.
The technique reported in this study added two more muscle plications to the classic abdominoplasty, which leads to a higher tension in the abdominal wall and a more satisfactory esthetic result. With the technique, the suprapubic transverse incision could be positioned lower, allowing the coverage of the scar even with small garments (Figures 8-13).
DISCUSSION
In this study, the following two good indications for the application of lateral plications to the median plicature were reinforced:
1. Multiparous patients with great flaccidity of the abdominal wall showing residual sagging even after performing medial plication, and
2. Patients with great flaccidity of the abdominal wall without excess of adipose tissue, who when only medial plication is performed, show a projection of the skin and adipose tissue above the navel (epigastrium and mesogastrium), which alters the harmony and esthetics of the abdominal relief pad, being a frequent complaint of patients in the postoperative period27,28. Medial plication performed in combination with external pararectal plications results in better skin and fat distributions, in addition to achieving greater abdominal wall tension with optimal esthetic results (Figures 14 and 15).
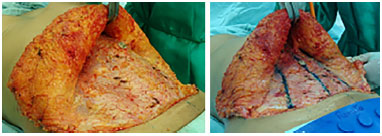
Figure 14. Before and after the plications. Improvement of the bulging of the abdominal wall can be observed.
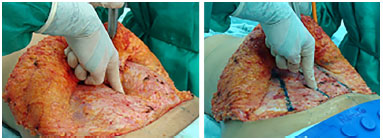
Figure 15. Application of force on the abdominal wall, demonstrating improvement in tension.
In addition to plications, liposuction of the flap is performed at the end of the procedure, which decreases the tension with probable improvement of circulation28. Another issue raised is that possible hernias can be visualized and corrected during abdominoplasty, before liposuction, without the risk of cannula entry through the hernia.
As the plication area lies laterally to the perforating vessels of the rectus abdominis muscles, the vascularization of the flap is not impaired, which makes the technique quite safe17,25,31.
Recall that classic abdominoplasty is a technique widely used by plastic surgeons for a long time. The technique proposed by Callia4,5 marked a new era of abdominoplasties, placing the incision over the pubis and its lateral extensions parallel to the inguinal folds, positioning the scar in a hidden area.
Pitanguy6,7 suggested a plication of the rectus abdominis muscles without opening the aponeurosis, contributing to the improvement of the result of abdominoplasty. Psillakis13 described the treatment of muscle-aponeurotic flaccidity where the oblique muscle is sutured to the fascia of the rectus abdominis muscle. Performing liposuction at the same surgical time provided better results in abdominal contour15,17.
Liposuction at the end of abdominoplasty promotes uniformization of the upper flap with the pubis. In addition, it probably allows preservation of several musculocutaneous perforating vessels, maintaining sufficient blood supply, and venous and lymphatic drainage of the detachment flap to avoid impairment to the final vascularization28.
The removal of a large number of adipose cells via liposuction can contribute to decreased tension and the metabolic need of the flap, and allows the relaxation of vascular plexuses in the flap, improving blood flow and venous return28, which can be evidenced by the absence of complications such as epidermolysis and necrosis of the abdominal flap in the cases studied. On the contrary, it seems to increase postoperative drainage, requiring aspiration drainage.
To better validate our observations, a larger sample size with a longer follow-up (>3 years) is needed.
CONCLUSION
The technique described herein is effective in the esthetic treatment of the abdominal region. Candidate patients for classic abdominoplasty who have excess adipose tissue in the upper abdomen and/ or large muscle-aponeurotic flaccidity may benefit from the technique. Liposuction performed at the end of abdominoplasty maintains the natural results, as it promotes a uniformity of adipose tissue throughout the abdominal and pubic regions. It also facilitates lower positioning of the suprapubic transverse incision, which allows covering of the scar even with short garments. It is easy, safe, and fast to execute, with low complication
COLLABORATIONS
RFPG Analysis and/or interpretation of data; statistical analysis; final approval of the manuscript; conception and design of the study; completion of operations and/or experiments; and drafting of the manuscript or critical review of its contents.
IRG Analysis and/or interpretation, and drafting of the manuscript or critical review of its contents.
JGT Analysis and/or interpretation of data, and drafting of the manuscript or critical review of its contents.
REFERENCES
1. Richter DF, Stoff A. Abdominoplasty procedures. In: Neligan PC, ed. Plastic Surgery. 3rd ed. London: Elsevier; 2013. p. 530-58.
2. Pontes R. Plástica abdominal: importância de sua associação a hérnias incisionais. Rev Bras Cir. 1965;52(2):85-91.
3. Pitanguy I. Abdominoplastias. Hospital. 1967;71(6):1541-56.
4. Callia WEP. Contribuição para o estudo da correção cirúrgica do abdome em pêndulo e globoso: técnica original [Tese de doutorado]. São Paulo: Faculdade de Medicina, Universidade de São Paulo; 1965.
5. Callia W. Uma plástica para a cirurgia geral. Méd Hosp (São Paulo). 1967;1:40-1.
6. Pitanguy I. Abdominoplastias. Hospital. 1967;71(1):541-56.
7. Pitanguy I. Surgical reduction of the abdomen, thigh, and buttocks. Surg Clin North Am. 1971;51(2):479-89.
8. Franco T, Rebello C. Abdominoplastia - Nem sempre uma cirurgia simples. Medicina de Hoje. 1977;638-44.
9. Rebello C, Franco T. Abdominoplastia por incisão submamária. Rev Bras Cir. 1972;62:249-52.
10. Sinder R. Plastic surgery of the abdômen: técnica pessoal de abdominoplastia, com prévio descolamento de retalho supraumbilical e uso de retalho dermoadiposo, VI International Congress of Plastic and Reconstrutive Surgery, Paris, França, 25 de agosto de 1975. Rev Bras Cir Plást. 2009;24(3):336-44 MonAteleirxoa nCdGreZ W et al.
11. Sinder R. Detalhe da técnica citada no livro de Cirurgia Estética de Talita Franco e Cláudio Rebello (Abdominoplastia). Capítulo 9. Rio de Janeiro, São Paulo: Atheneu; 1977. p.277.
12. Planas J. The "vest over pants" abdominoplasty. Plast Reconstr Surg. 1978;61(5):694-700.
13. Psillakis JM. Abdominoplasty: Some ideas to improve results. Aesthetic Plast Surg. 1978;2(1):205-15.
14. Illouz YG. Une nouvelle technique pour leslipodystrophies localeseés. Rev Chir Esther. 1980;4:19.
15. Illouz YG. A new safe and aesthetic approach to suction abdominoplasty. Aesthetic Plast Surg. 1992;16(3):237-45.
16. Hakme F. Technical details in the lipoaspiration associate with liposuction. Rev Bras Cir. 1985;75(5):331-7.
17. Avelar JM. Abdominoplastia - uma nova técnica sem deslocamento e sem ressecçäo do panículo abdominal. Arq Catarin Med. 2000;29(Supl 1):147-9.
18. Avelar JM. Abdominoplasty combined with lipoplasty without panniculus undermining: abdominolipoplasty--a safe technique. Clin Plast Surg. 2006;33(1):79-90.
19. Avelar JM. Abdominoplasty without panniculus underming and resection. São Paulo: Hipócrates; 2002.
20. Baroudi R, Keppke EM, Netto FT. Abdominoplasty. Plast Reconstr Surg. 1974;54(2):161-8.
21. Baroudi R. Management of the umbilicus in abdominoplasty. In: American Society of Aesthetic Plastic Surgery Meeting; 1973 Mar; Newport Beach, USA.
22. Matarasso A. Abdominolipoplasty: a system of classification and treatment for combined abdominoplasty and suction-assisted lipectomy. Aesthetic Plast Surg. 1991;15(2):111-21.
23. Nahas FX. Advancement of the external oblique muscle flap to improve the waistline: a study in cadavers. Plast Reconstr Surg. 2001;108(2):550-5.
24. Nahas FX. An aesthetic classification of the abdomen based on the myoaponeurotic layer. Plast Reconstr Surg. 2001;108(6):1787-95.
25. Saldanha OR, Pinto EB, Matos WN Jr, Lucon RL, Magalhães F, Bello EM. Lipoabdominoplasty without undermining. Aesthet Surg J. 2001;21(6):518-26.
26. Saldanha OR, De Souza Pinto EB, Mattos WN Jr, Pazetti CE, Lopes Bello EM, Rojas Y, et al. Lipoabdominoplasty with selective and safe undermining. Aesthetic Plast Surg. 2003;27(4):322-7.
27. Bozola AR, Psillakis JM. Abdominoplasty: a new concept and classification for treatment. Plast Reconstr Surg. 1988;82(6):983-93.
28. Rosa MP, Bozola AR. Abdominoplastia clássica associada à vibrolipoaspiração setorial. Rev Bras Cir Plást. 2010;25(2):337-43.
29. Nahas FX, Ferreira LM, Augusto SM, Ghelfond C. Long-term follow-up of correction of rectus diastasis. Plast Reconstr Surg. 2005;115(6):1736-41.
30. Nahas FX, Ferreira LM. Concepts on correction of the musculoaponeurotic layer in abdominoplasty. Clin Plast Surg. 2010;37(3):527-38.
31. Graf R, Freitas R, Fisher M, Bark A, Loureiro A, Pianowski R, et al. Estudo de fluxometria Doppler. In: Saldanha O, ed. Lipoabdominoplastia. Rio de Janeiro: Di-Livros; 2004. p. 87-92.
32. Guimarães VHM, Andrade CFI, Magalhães GMC, Guerra SNE. Hérnia de Spiegel após Abdominoplastia. Rev Bras Cir Plást. 1997;12(1):57-64.
33. Moulim JL, Sobreira ML, Malgor RD, Abreu CR, Araújo ESF, Palhares Neto AA. Estudo comparativo entre protocolos para profilaxia da trombose venosa profunda: uma nova proposta. Rev Bras Cir Plást. 2010;25(3):415-22.
34. Sandri JL. Profilaxia do tromboembolismo em cirurgia plástica. In: Carreirão S, Cardim V, Goldenberg D, eds. Cirurgia Plástica - Sociedade Brasileira de Cirurgia Plástica. São Paulo: Atheneu; 2005. p.119-25.
35. Hatef DA, Trussler AP, Kenkel JM. Procedural risk for venous thromboembolism in abdominal contouring surgery: a systematic review of the literature. Plast Reconstr Surg. 2010;125(1):352-62.
Hospital Vaz Monteiro, Lavras, MG, Brazil
Institution: Hospital Vaz Monteiro e Santa Casa de Misericórdia de Lavras, MG, Brazil.
Corresponding author:
Renato Fonseca de Pádua Gonçalves
Rua Dr. Antonio Gonçalves de Faria, 1540, sala 14 - Jardim Eldorado
Lavras, MG, Brazil Zip Code 37200-000
E-mail: rf_padua@yahoo.com.br
Article received: July 27, 2014.
Article accepted: January 6, 2015.
Conflicts of interest: none.



 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter