

Original Article - Year 2016 - Volume 31 -
Continuous absorbable suture versus interrupted permanent suture in the treatment of diastasis of the rectus abdominis muscle
Sutura contínua com fio absorvível versus interrompida com fio permanente no tratamento da diástase do músculo reto abdominal
ABSTRACT
INTRODUCTION: Plication of the rectus abdominis muscle is an important step in remodeling the abdomen in abdominoplasties. It can be performed using several types of threads with interrupted or continuous sutures, according to the surgeon's preferences. Few studies in the literature compared the different plication techniques in abdominoplasties. The present study aimed to compare continuous anchored suture with polydioxanone (PDS) with interrupted nylon suture regarding surgical time, relapse, and costs and discuss the advantages and disadvantages of each method.
METHODS: A randomized clinical trial in which 30 patients were enrolled for each of the two groups, 15 with continuous suture and 15 with interrupted suture, was conducted. The plication time was compared between the groups using the Student's t-test. Between 10 and 12 months postoperatively, all patients underwent ultrasonography for investigating diastasis recurrence.
RESULTS: Continuous suture decreased the plication time by almost 40% when compared to the interrupted suture (p < 0.001), without affecting the esthetic outcome. The PDS used in the continuous suture implied higher costs than those with the nylon threads used in the interrupted suture. No recurrence was found on the postoperative control ultrasonography results.
CONCLUSION: Continuous suture reduced the plication time by almost 40% (p < 0.001) when compared to interrupted suture. Despite being associated with higher costs, PDS seems to be a good alternative to non-absorbable sutures, such as nylon threads, in plications of the rectus abdominis, since it is a more biocompatible material.
Keywords: Abdominoplasty; Suture techniques; Biocompatible Materials; Polydioxanone; Nylons.
RESUMO
INTRODUÇÃO: A plicatura do músculo reto abdominal é um passo importante no remodelamento do abdômen nas abdominoplastias. Ela pode ser realizada com vários tipos de fios e com suturas interrompidas ou contínuas, de acordo com as preferências do cirurgião. Poucos estudos na literatura compararam diferentes técnicas de plicatura nas abdominoplastias. O objetivo do estudo é comparar a sutura contínua ancorada com polidioxanona (PDS) com a sutura interrompida com náilon quanto ao tempo cirúrgico, recidiva, custos e discutir vantagens de desvantagens de cada método.
MÉTODOS: Ensaio clínico randomizado no qual 30 pacientes foram arroladas para cada um dos grupos, 15 sutura contínua e 15 sutura interrompida. O tempo de plicatura foi comparado entre os grupos utilizando-se o teste t de Student. Entre 10 a 12 meses de pós-operatório, todas as pacientes foram submetidas à ecografia em busca de recidivas da diástase.
RESULTADOS: A sutura contínua diminuiu em quase 40% o tempo de plicatura quando comparada à sutura interrompida (p < 0,001), sem prejuízo no resultado estético. O PDS utilizado na sutura contínua implicou maiores custos que os fios de náilon utilizados na sutura interrompida. Nenhuma recidiva foi encontrada na ecografia de controle no pós-operatório.
CONCLUSÃO: A sutura contínua quando comparada à sutura interrompida foi capaz de reduzir o tempo de plicatura em quase 40% (p < 0,001). A utilização do PDS, apesar dos maiores custos, parece ser uma boa alternativa às suturas com fios não absorvíveis como o náilon nas plicaturas do músculo reto abdominal, uma vez que se trata de um fio de maior biocompatibilidade.
Palavras-chave: Abdominoplastia; Técnicas de sutura; Materiais biocompatíveis; Polidioxanona; Nylons.
Abdominoplasty has an important impact on the well-being and quality of life of operated patients1. The goals of surgery include the remodeling of the abdomen and reduction of the waist, and the plication of the rectus abdominis muscle is an important step within this procedure to obtain good results. Plication can be carried out in several ways with various types of sutures.
For a long time, there was a controversy among many authors regarding the use of absorbable sutures in the treatment of diastasis of the rectus abdominis muscle for the fear of possible deformity recurrence after absorption of the suture. Reinforcing this idea, authors who compared the use of polyglactin (Vicryl) tended to find high rates of relapse2, compared to the good results with the use of definitive sutures3.
However, after the comparative studies on slow absorption and non-absorbable sutures4, especially those conducted by Nahas5,6, there is evidence that prolonged absorption sutures are a good alternative to non-absorbable sutures for the treatment of diastasis of the rectus abdominis muscle, without impairing the results or increasing the number of recurrences of the deformity.
Among the long-term absorbable sutures, polydioxanone (PDS) is a good pliable suture to use in abdominoplasty. This suture has been tested in previous studies to demonstrate good results compared to those with nylon (polyamide) suture not only in abdominoplasty but also in the synthesis of abdominal aponeurosis in median laparotomies7 and sutures of the cartilages8 among other procedures.
No comparative studies have evaluated which between the use of a continuous or interrupted suture in the plication of the rectus abdominis muscle is the best approach. However, it seems clear that continuous sutures tend to be performed faster, which reduces the surgical time. Some surgeons, however, may be resistant to use this method because of the risk of opening all sutures in case a continuous suture is disrupted.
Nevertheless, partial disruption may also occur with interrupted sutures, which can sometimes cause even larger deformities than the complete opening of the suture; such method can lead to localized abdominal bulging, which can be more esthetically unpleasant than the recurrence of diastasis.
Considering the potential advantages and disadvantages of the different types of sutures, with recent interest in PDS and in continuous versus simple plication, the author decided to compare the results of the use of continuous suture with double-laced PDS with the use of interrupted X suture with nylon threads.
OBJECTIVE
The objectives of the study were to compare the two techniques regarding surgical time, relapse, and costs and discuss the advantages and disadvantages of both methods.
METHODS
From December 2013 to April 2014, the author performed 30 abdominoplasties, 15 with interrupted X suture and 15 with continuous suture. The method of allocation of the patients was random, by means of a draw, which was done pre-operatively (randomized clinical trials). A dark container with 30 lots was used for randomization, 15 of which were labeled group 1 (continuous suture) and 15 were labeled group 2 (interrupted sutures).
Before the surgery of each patient, a lot was removed from the container to determine the allocation group of each patient. Thereafter, this lot was discarded to create equal groups. The number 30 was estimated through the observation of the author, who had already been using the two techniques routinely on his patients, that the plication time was reduced by approximately 50% with the use of continuous suture.
The number of patients to be included in the study was estimated using the program "Power and Sample Size," considering a power of 80%. All patients signed an informed consent form pre-operatively agreeing to participate in the study. The present study was conducted at Hospital Ernesto Dornelles, Porto Alegre, RS, following the ethical principles according to the Declaration of Helsinki.
Classical dermolipectomy with or without liposuction was performed in all patients enrolled for this comparison. The patients had excess skin above and below the navel, with high or low implantation of the umbilicus, and with or without excess abdominal fat; further, all patients had some degree of diastasis of the rectus abdominis muscle, which would classify them as grades III and IV, as proposed by Bozola9,10, or A and B according to the abdominal aponeurosis classification proposed by Nahas11.
Exclusion criteria included having undergone mini-abdominoplasty, absence of abdominal diastasis, and presence of marked oblique flaccidity, requiring plication of the oblique muscles.
Age, time of the plication, and length of the plication (measured from the xiphoid to the pubis) were compared between the groups. Continuous variables were tested for normality using the Shapiro-Wilk test, presented as mean and standard deviation, and compared using the Student's t-test. The data were analyzed using the SPSS software, version 19.0.
Between 10 and 12 months after surgery, all patients underwent ultrasonography of the abdominal wall for investigation of recurrences of diastasis.
Technique
The same abdominoplasty technique was used in all patients: arciforme incision and detachment in the tunnel on the midline up to the xiphoid appendix, exposing the entire abdominal diastasis and limited lateral detachment.
Before plication began, the craniocaudal distances (from the xiphoid to the pubis) with complete flap detachment were measured to estimate the length of the plicature to be performed (Figure 1). In all patients, simple supraumbilical and infraumbilical sutures were made (Figure 2). Only after these initial sutures were the suture times timed for the two groups.
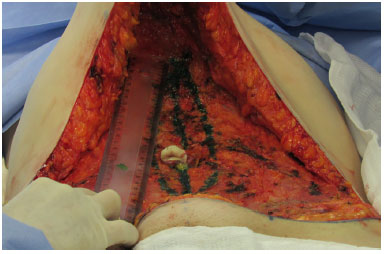
Figure 1. Craniocaudal measurement of the xiphoid appendix to the pubis.
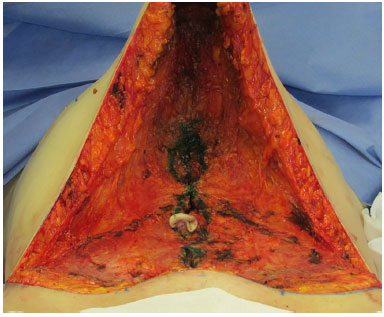
Figure 2. Initial upper and lower sutures performed before timing of the plication.
The material used for the simple sutures was nylon 0.0 (polyamide) and that for the continuous sutures was double-laced PDS 1. Continuous PDS suturing was anchored followed by Alferich knots (one above and one below the umbilicus) to ensure that the suture was adequately tensioned, reducing the risk of loosening. Interrupted sutures with 0.0 nylon were performed in X with inverted (downward) knots.
After plication, the procedure was followed equally in all patients. All patients remained with a Portovac drain postoperatively, which was the author's preferred method to avoid the formation of seroma.
RESULTS
The variables that were compared between the two groups are presented in Table 1.
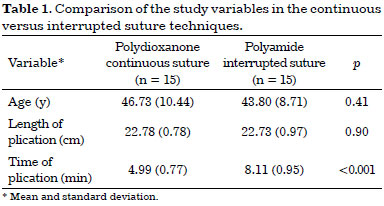
There were no differences regarding age and length of the xiphoid to the pubis among all patients included in the groups, demonstrating that all of them had similar initial parameters; such finding confirms the effectiveness of the randomization. All patients included were women.
For the time of plication, there was a reduction of almost 40% in the time of completion of the suture using the continuous suture compared to the interrupted suture (p < 0.001) (Figure 3).
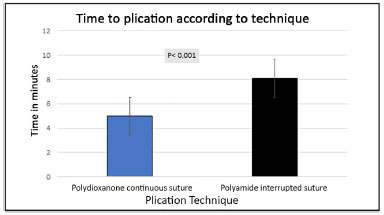
Figure 3. Graph of the average plication time according to the technique used.
Among the patients enrolled in the continuous PDS suture group, only one thread was used, whereas among the patients in the separate nylon suture group, three to four threads were used.
Regarding the costs of the sutures used, the PDS 1 costed R$ 49.42 each, while the nylon thread 0.0 costed R$ 3.60 per unit at the time of this study. Given that three to four nylon threads were used in the interrupted suture group, the total cost in this group was around R$ 10.80 to 14.40 per patient.
With regard to complications, seroma was reported in five cases, epidermolysis < 1 cm thick in four cases, and dehiscence of the suture in the central region of the incision in two cases. All the complications reported were found in patients with a body mass index (BMI) greater than 35 kg/m2, i.e., obesity grade II. However, there were no complications directly related to the type of technique or the type of suture used in the plication, which was the objective of this study. Figure 4 show the pre- and post-operative view results of one patient in the continuous suture group.
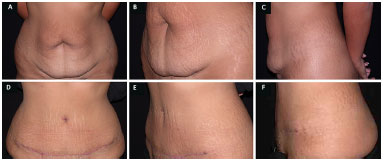
Figure 4. A: Pre-operative frontal view; B: Pre-operative oblique view; C: Pre-operative side view; D: Post-operative frontal view; E: Post- operative oblique view; F: Post-operative side view.
In the control ultrasound scans carried out between 10 and 12 months after surgery, no case of suture rupture with recurrence of diastasis was found in any of the groups.
DISCUSSION
According to the data from this study, the continuous suture significantly reduced the time of plication around 40% when compared to the separate sutures. Moreover, there was no recurrence of diastasis in any of the cases studied, even in the control ultrasound scans after 1 year, or any differences in the esthetic results.
In this study, we used the PDS 1 in the continuous suture group and nylon in the separate suture group. PDS is a more expensive thread, but more biocompatible and with less risk of foreign-body type reactions and local inflammation on a long-term basis. A recent study comparing local erythema in surgical skin sutures showed that PDS resulted in less local reactions when compared to other threads, including absorbable and non-absorbable sutures12 if removed within 10 days.
A possible criticism of this study, however, is that it did not perform a long-term evaluation. Although non-absorbable sutures are considered of low reactivity, there is no doubt that some degree of cellular reaction occurs, with consequent inflammatory reactions and erythema12,13. Although not a common event, granulomas can occur when using permanent sutures.
In addition, permanent sutures can be uncomfortable and palpable in very thin patients, while absorbable sutures can avoid this type of complication. However, this type of complication is not common when permanent suture knots are positioned downward, as performed in this study in the interrupted suture group.
For these reasons regarding the lower reaction and greater biocompatibility, interest in PDS has been increasing considerably since its launch in the market. PDS is close to an ideal material; besides being absorbable, it is a monofilament thread, implying a lower risk of infection compared to multifilament threads, such as polyglactin. The PDS thread used in this study was double-laced, adding safety and resistance to the suture.
As to the type of suture, no studies have compared the different techniques in suturing the abdominal fascia, except for the study of Weissman et al14. They compared continuous simple suture and continuous horizontal suture (in continuous U) with nylon in an experimental model simulating the abdominal wall, concluding that the continuous horizontal suture was performed faster and caused less damage to the tissues.
Continuous anchored suture (continuous horizontal suture) was used in the present study, which, in the opinion of the author, also distributes the tension better than the simple continuous suture, besides maintaining more consistent tension on the suture, preventing the thread to run easily.
Although different suture materials were compared in this study, mainly because of the worldwide trend in using PDS in place of nylon in numerous procedures, the aim of this study to compare the plication time between the continuous and separate suture techniques was not impaired.
If we used a double-laced nylon thread in the continuous suture performed in this study to compare it with the interrupted suture with nylon thread, for example, the reduction in the time of plication would be maintained. Thus, even when comparing different threads, the results of this study regarding the shorter surgical time associated with continuous sutures are not invalid.
The findings of this study validate the decision of the author to change his standard technique of plication of the fascia of the rectus abdominis muscle from separated X sutures with 0-0 nylon to continuous sutures using double-laced PDS 1, despite increased costs. Previous cases in the personal series of the author, not included in this study, regarding partial rupture of interrupted sutures with unpleasant results also reinforced this change.
CONCLUSION
The continuous suture technique in the plication of the rectus abdominis muscle in abdominoplasties reduces the time of plication by around 40% when compared to interrupted sutures (p < 0.001), without negatively affecting the outcome. The use of absorbable long-term materials, such as PDS did not imply a higher risk of diastasis recurrence when compared to the use of polyamide thread, as observed in the control ultrasound results. However, the use of PDS implies higher costs. The use of continuous suture with nylon (polyamide) would benefit from the reduction in surgical time while keeping the costs low; however, this is a material with a lower biocompatibility.
COLLABORATIONS
LF Study design; implementation of the operations and experiments; review of the literature; analysis and interpretation of the data; drafting and critical review of the data; and final approval of the manuscript.
DWD Study design; statistical analysis; analysis and interpretation of the data; review of the literature; drafting of the manuscript; and final approval of the manuscript.
VG Collaboration in the execution of the operations and experiments; review of the literature; drafting of the manuscript; and final approval of the manuscript.
REFERENCES
1. de Brito MJ, Nahas FX, Barbosa MV, Dini GM, Kimura AK, Farah AB, et al. Abdominoplasty and its effect on body image, self-esteem, and mental health. Ann Plast Surg. 2010;65(1):5-10.
2. van Uchelen JH, Kon M, Werker PM. The long-term durability of plication of the anterior rectus sheath assessed by ultrasonography. Plast Reconstr Surg. 2001;107(6):1578-84.
3. Tadiparthi S, Shokrollahi K, Doyle GS, Fahmy FS. Rectus sheath plication in abdominoplasty: assessment of its longevity and a review of the literature. J Plast Reconstr Aesthet Surg. 2012;65(3):328-32.
4. Mestak O, Kullac R, Mestak J, Nosek A, Krajcova A, Sukop A. Evaluation of the long-term stability of sheath plication using absorbable sutures in 51 patients with diastasis of the recti muscles: an ultrasonographic study. Plast Reconstr Surg. 2012;130(5):714e-719e.
5. Nahas FX, Ferreira LM, Ely PB, Ghelfond C. Rectus diastasis corrected with absorbable suture: a long-term evaluation. Aesthetic Plast Surg. 2011;35(1):43-8.
6. Nahas FX, Augusto SM, Ghelfond C. Nylon versus polydioxanone in the correction of rectus diastasis. Plast Reconstr Surg. 2001;107(3):700-6.
7. Sajid MS, Parampalli U, Baig MK, McFall MR. A systematic review on the effectiveness of slowly-absorbable versus non-absorbable sutures for abdominal fascial closure following laparotomy. Int J Surg. 2011;9(8):615-25.
8. Iamphongsai S, Eshraghi Y, Totonchi A, Midler J, Abdul-Karim FW, Guyuron B. Effect of different suture materials on cartilage reshaping. Aesthet Surg J. 2009;29(2):93-7.
9. Bozola AR. Abdominoplasty: same classification and a new treatment concept 20 years later. Aesthetic Plast Surg. 2010;34(2):181-92.
10. Bozola AR, Bozola A. Abdominoplastias. In: Mélega JM, Baroudi R, eds. Cirurgia plástica fundamentos e arte: cirurgia estética. Rio de Janeiro: Medsi; 2003. p. 609-23.
11. Nahas FX. An aesthetic classification of the abdomen based on the myoaponeurotic layer. Plast Reconstr Surg. 2001;108(6):1787-95.
12. Parara SM, Manios A, de Bree E, Tosca A, Tsiftsis DD. Significant differences in skin irritation by common suture materials assessed by a comparative computerized objective method. Plast Reconstr Surg. 2011;127(3):1191-8.
13. Greenwald D, Shumway S, Albear P, Gottlieb L. Mechanical comparison of 10 suture materials before and after in vivo incubation. J Surg Res. 1994;56(4):372-7.
14. Weissman O, Zmora N, Rozenblatt SM, Tessone A, Nardini GG, Zilinsky I, et al. Simple continuous suture versus continuous horizontal mattress suture for plication of abdominal fascia: which is better? Aesthetic Plast Surg. 2012;36(5):1015-8.
1. Sociedade Brasileira de Cirurgia Plástica, São Paulo, SP, Brazil
2. Hospital Ernesto Dornelles, Porto Alegre, RS, Brazil
3. Associação Brasileira de Cirurgia Crânio-Maxilo-Facial, São Paulo, SP, Brazil
4. Universidade Federal do Rio Grande do Sul, Porto Alegre, RS, Brazil
Institution: Hospital Ernesto Dornelles, Porto Alegre, RS, Brazil.
Corresponding author:
Leandro Fuchs
Rua Quintino Bocaiuva, 984
Porto Alegre, RS, Brazil Zip Code 90440-050
E-mail: lndfuchs@terra.com.br
Article received: July 11, 2015.
Article accepted: November 12, 2015.
Conflicts of interest: none.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter