

Ideas and Innovation - Year 2016 - Volume 31 -
Flap and abdominal wall washing and debridement using dressings to prevent seromas and hematomas in abdominoplasty
Lavagem e desbridamento do retalho e da parede abdominal com compressas como prevenção de seromas e hematomas em abdominoplastia
ABSTRACT
Seroma formation remains a common complication of abdominoplasty. The use of drain, flap fixation points, and fibrin glue has been described to reduce the incidence of seroma formation. The authors present herein an easy-to-reproduce technique to decrease the risk of bleeding and eliminate the devitalized tissue caused by the detachment. The proposed strategy consists of washing and debridement, which was conducted with mechanical friction using moist flap and abdominal wall dressings.
Keywords: Abdominoplasty; Postoperative complications; Seroma.
RESUMO
A formação de seroma após uma abdominoplastia continua sendo uma complicação frequente. O uso de dreno, os pontos de fixação do retalho e o uso da cola de fibrina foram descritos com a finalidade de diminuir a sua incidência. Os autores apresentam uma técnica de fácil reprodução para reduzir o risco de sangramento, bem como para eliminar o tecido desvitalizado decorrente do descolamento. A tática proposta constitui-se de lavagem e desbridamento por meio da fricção mecânica com compressas umedecidas do retalho e da parede abdominal.
Palavras-chave: Abdominoplastia; Complicações pós-operatórias; Seroma.
Abdominoplasty is one of the most commonly performed surgical procedures in plastic surgery. According to statistics from the American Society of Plastic Surgeons, the frequency of the use of abdominoplasty has increased to 71% since 2000 and 537% since 19921,2.
The British Association of Aesthetic Plastic Surgeons reported that >3,000 abdominoplasties were performed in the year 20103. Abdominoplasty was the fourth most performed aesthetic procedure in the world in 2011 and the first procedure to be performed to correct body contour in 2013. Overall, >129,000 procedures have been conducted in Brazil (ISAPS International Survey, 2011 and 2013).
The most frequent postoperative complication is seroma, with an incidence of 10-15%4-7. On the other hand, pulmonary embolism is the most feared complication8. The formation of seroma depends on the experience of the surgeon, body mass index (BMI) of the patient, or liposuction performed along with this procedure9.
The use of drains, flap sutures to the abdominal wall, and fibrin glue were described to decrease the incidence of seroma8-10. Apparently, when cases where drains, sutures, and fibrin glue were used were compared, the use of adhesion points significantly reduced the incidence of seroma formation in the patients11. In relation to the drain placement, several output locations have already been described12. Seroma formation often occurs in the hypogastrium region and starts to be noticed from the second postoperative week13.
The mechanisms that were proposed to clarify seroma formation are disruption of the lymphatic and vascular circulations, formation of a dead space, extensive detachment of the flap, and production and release of inflammatory mediators in the traumatized tissue1,7,14. Smoking, diabetes, obesity, male sex, and the association with suction-assisted lipectomy are risk factors15.
The recommendations of the authors to prevent these complications are as follows: prolonged use of a closed vacuum drainage, application of abdominal dressing, avoidance of performing liposuction simultaneously with abdominoplasty, limitation of the detachment, restriction of early ambulation, and use of fibrin glue13,16.
Beer and Wallner4 described that immobilizing the patient in the first 48 hours after abdominoplasty would reduce the risk of seroma while performing an appropriate pharmacological prophylaxis for thromboembolism. Scarpa's fascia preservation method was described to decrease abdominoplasty complications such as seroma17.
For other authors, the prevention of seroma relies on a restricted and suprafascial detachment, and on the preservation of good arterial and lymphatic irrigations18. Fang et al.19 described the detachment in a more superficial plane than in a suprafascial one to reduce the time of drain use in the postoperative period, thus improving patient comfort and recovery.
Costa-Ferreira et al.17, in a randomized trial with evidence level I, described that Scarpa's fascia preservation in abdominoplasty has a beneficial effect on patient recovery, reducing the total volume of drain output by 65.5%, decreasing the time of drain use up to 3 days, and diminishing the incidence of seroma by 86.7%.
Di Martino et al.14 described that the combination of lipoabdominoplasty and the use of flap adhesion sutures decreases the risk of seroma. More recently, in 2014, Skillman et al.3 reported that the use of clips or suture ligation rather than diathermic ablation of large abdominal perforators reduces the incidence of seroma.
The use of progressive tension suture is a relatively simple technique and can be used to prevent the formation of seroma in abdominoplasties1. Matarasso commented on the study published by Chaouat et al.6, emphasizing the need to reduce the dead space behind the abdominal flap. Mladick20 briefly discussed the importance of fixing the flap with internal sutures to reduce the dead space.
Baroudi and Ferreira13 reported the use of up to 40 separate stitches on four suture lines. Hamra21 described points of parallel continuous suture in abdominoplasty, while Pollock and Pollock22 described progressive tension sutures.
Despite all these procedures, prevention remains the best form of treatment7. Similarly, ultrasonography is the most appropriate diagnostic method for seroma formation after abdominoplasty14.
OBJECTIVE
The authors present a simple, fast, and effective technique that may reduce the risk of seroma and hematoma formations after abdominoplasty. This relies on washing and mechanical debridement by using flap and abdominal wall dressings.
METHODS
Surgical procedure
During conventional abdominoplasty, the removal of the dermal-adipose flap and plication of the rectus abdominis are followed by washing with 1 liter of 0.9% saline solution, using dressings to mechanically debride the surface of the flap and abdominal wall fat tissue (Figures 1 and 2).
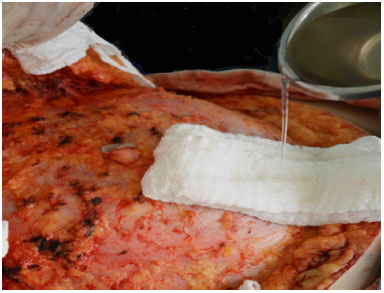
Figure 1. Washing with saline solution.
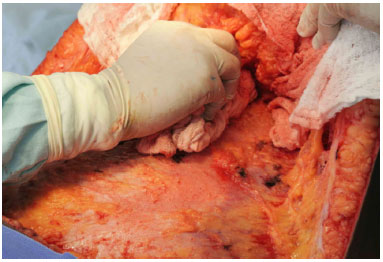
Figure 2. Mechanical debridement with a moist dressing.
In this way, the blood vessels lose their weak and superficial clots, while a more meticulous hemostasis is performed (Figure 3).
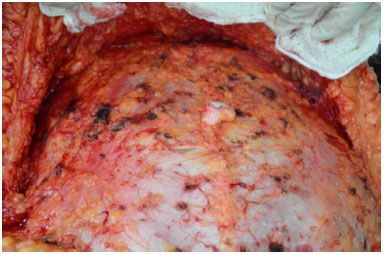
Figure 3. Bleeding points that could cause postoperative hematomas.
The fat from the flap can be cleaned by removing the superficial fatty tissue, which is damaged by mechanical (flap traction during the detachment) and thermal trauma (electrocautery; Figure 4).

Figure 4. Devitalized fat tissue that is removed by friction using dressing.
A retrospective review was conducted by analyzing the electronic medical records of 183 patients who underwent the procedure, performed as a routine technique by the surgical team and during an abdominoplasty performed between May 2011 and August 2015. During the procedure, no fixation points were made on the flap and a vacuum drain was placed with an outlet to the inguinal crease, as described by the authors. In the immediate postoperative period and up to 1
month after surgery, use of a body shaper was recommended.
RESULTS
Of the patients, 98.7% showed no postoperative complications and 1.3% developed a seroma, which was treated with puncture, drainage, and compression. Hematomas or infections were not observed.
DISCUSSION
Seroma continues to be a frequent complication of abdominal plastic surgery. A large area of detachment, use of electrocautery, and frequent association of liposuction in private practice favor their formation. A study on this subject is still ongoing, but the emergence of multiple techniques indicates that a definitive prevention procedure was still not found.
According to a literature review, no procedure as detailed as that described herein has been previously reported. However, this study loses significant statistical power owing to its retrospective nature, the longstanding routine practice of the surgical team, and the lack of comparison to another technique that prevents seroma formation.
Washing and mechanical debridement of the abdominal wall and posterior surface of the dermal-adipose flap by using dressings can be useful for detecting the weakest points in the blood vessels and eliminating the superficial fatty tissue damaged by the mechanical and thermal traumas caused by the detachment. Thus, a more effective hemostasis can be attained, in addition to a more viable tissue free of any excess that favors the accumulation of liquids or secretions.
The authors present a simple and easy-to-reproduce approach that may decrease the incidence of seroma after abdominoplasty.
COLLABORATIONS
ES Approved the final version of the manuscript, elaborated and designed the study, and performed the surgeries and/or experiments.
RFMR Analyzed and/or interpreted the data, performed the statistical analyses, approved the final version of the manuscript, and wrote the manuscript and/or critically reviewed its content.
PZ Realized surgeries and/or experiments.
JM Analyzed and/or interpreted the data, elaborated and designed the study, and wrote the manuscript and/or critically reviewed its content.
COU Approved the final version of the manuscript.
REFERENCES
1. Khan S, Teotia SS, Mullis WF, Jacobs WE, Beasley ME, Smith KL, et al. Do progressive tension sutures really decrease complications in abdominoplasty? Ann Plast Surg. 2006;56(1):14-20.
2. American Society of Plastic Surgeons. National Clearinghouse of Plastic Surgery Statistics. [cited 2016 Nov 8]. Available from: https://www.plasticsurgery.org/news/plastic-surgery-statistics
3. Skillman JM, Venus MR, Nightingale P, Titley OG, Park A. Ligating perforators in abdominoplasty reduces the risk of seroma. Aesthetic Plast Surg. 2014;38(2):446-50.
4. Beer GM, Wallner H. Prevention of seroma after abdominoplasty. Aesthet Surg J. 2010;30(3):414-7.
5. Hafezi F, Nauhi AH. Abdominoplasty and seroma. Ann Plast Surg. 2002;48(1):109-10.
6. Chaouat M, Levan P, Lalanne B, Buisson T, Nicolau P, Mimoun M. Abdominal dermolipectomies: early postoperative complications and long-term unfavorable results. Plast Reconstr Surg. 2000;106(7):1614-8; discussion 1619-23.
7. Andrades P, Prado A, Danilla S, Guerra C, Benitez S, Sepulveda S, et al. Progressive tension sutures in the prevention of postabdominoplasty seroma: a prospective, randomized, double-blind clinical trial. Plast Reconstr Surg. 2007;120(4):935-46.
8. Antonetti JW, Antonetti AR. Reducing seroma in outpatient abdominoplasty: analysis of 516 consecutive cases. Aesthet Surg J. 2010;30(3):418-25.
9. Schettino AM, Franco D, Franco T, Filho JM, Vendramin FS. Use of autologous fibrin glue (platelet-poor plasma) in abdominal dermolipectomies. Aesthetic Plast Surg. 2012;36(6):1296-301.
10. Uebel CO. Lipoabdominoplasty: revisiting the superior pull-down abdominal flap and new approaches. Aesthetic Plast Surg. 2009;33(3):366-76.
11. Bercial ME, Sabino Neto M, Calil JA, Rossetto LA, Ferreira LM. Suction drains, quilting sutures, and fibrin sealant in the prevention of seroma formation in abdominoplasty: which is the best strategy? Aesthetic Plast Surg. 2012;36(2):370-3.
12. Sucupira E, Matta R, Zuker P, Matta J, Uebel CO. Inguinal Fold as a Closed-Suction Drain Exit Site in Abdominoplasty. Aesthetic Plast Surg. 2015;39(6):1022-4.
13. Baroudi R, Ferreira CA. Seroma: how to avoid it and how to treat it. Aesthet Surg J. 1998;18(6):439-41.
14. Di Martino M, Nahas FX, Barbosa MV, Montecinos Ayaviri NA, Kimura AK, Barella SM, et al. Seroma in lipoabdominoplasty and abdominoplasty: a comparative study using ultrasound. Plast Reconstr Surg. 2010;126(5):1742-51.
15. Kim J, Stevenson TR. Abdominoplasty, liposuction of the flanks, and obesity: analyzing risk factors for seroma formation. Plast Reconstr Surg. 2006;117(3):773-9.
16. Kulber DA, Bacilious N, Peters ED, Gayle LB, Hoffman L. The use of fibrin sealant in the prevention of seromas. Plast Reconstr Surg. 1997;99(3):842-9.
17. Costa-Ferreira A, Rebelo M, Silva A, Vásconez LO, Amarante J. Scarpa fascia preservation during abdominoplasty: randomized clinical study of efficacy and safety. Plast Reconstr Surg. 2013;131(3):644-51.
18. Saldanha OR, De Souza Pinto EB, Mattos WN Jr, Pazetti CE, Lopes Bello EM, Rojas Y, et al. Lipoabdominoplasty with selective and safe undermining. Aesthetic Plast Surg. 2003;27(4):322-7.
19. Fang RC, Lin SJ, Mustoe TA. Abdominoplasty flap elevation in a more superficial plane: decreasing the need for drains. Plast Reconstr Surg. 2010;125(2):677-82.
20. Mladick RA. Progressive tension sutures to reduce complications in abdominoplasty. Plast Reconstr Surg. 2001;107(2):619.
21. Hamra ST. Circunferential Body Lift. Aesth Surg J. 1999;19(3):244-50.
22. Pollock H, Pollock T. Progressive tension sutures: a technique to reduce local complications in abdominoplasty. Plast Reconstr Surg. 2000;105(7):2583-6.
1. Sociedade Brasileira de Cirurgia Plástica, São Paulo, SP, Brazil
2. Hospital Santa Casa da Misericórdia do Rio de Janeiro, Rio de Janeiro, RJ, Brazil
3. Clínica Essendi, Rio de Janeiro, RJ, Brazil
4. Pontifícia Universidade Católica, Porto Alegre, RS, Brazil
5. Hospital São Lucas, Pontifícia Universidade Católica do Rio Grande do Sul, Porto Alegre, RS, Brazil
6. Instituto Materno-Infantil Perinatal, Recife, PE, Brazil
Institution: Serviço de Cirurgia Plástica, Hospital São Lucas, Pontifícia Universidade Católica do Rio Grande do Sul, Porto Alegre, RS, Brazil.
Corresponding author:
Renato Franz Matta Ramos
Avenida Ipiranga, 630 - Menino Deus
Porto Alegre, RS, Brazil Zip Code 90160-090
E-mail: renatomatta82@hotmail.com
Article received: January 29, 2016.
Article accepted: October 30, 2016.
Conflicts of interest: none.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter