

Original Article - Year 2017 - Volume 32 -
Rhinophyma: analysis of the shave excision technique
Rinofima: análise da técnica cirúrgica por Shave Excision
ABSTRACT
INTRODUCTION: The rhinophyma is an extremely stigmatizing condition for a patient. The first descriptions of this disease dates back to the time of Hippocrates, which was popular known as alcoholic nose or nasal elephantiasis is responsible for generating a huge deformity in the nose. This deformity derives from a process of hyperplasia and hypertrophy of the sebaceous glands in nasal skin associated with fibrosis and dilated local blood vessels and connective tissue. Surgery is considered the treatment of choice for aesthetic improvement of the injury.
METHODS: This was a retrospective study based on analysis of results from 11 patients (10 men and 1 woman) who underwent treatment for rhinophyma between January 2010 to January 2016 at the Plastic Surgery Service of the Teaching Hospital of Federal University of Juiz de Fora and Clinical Plastic Center.
RESULTS: Of 11 patients who underwent surgery, a 72-year-old man had basal expansive invasive carcinoma with positive surgical margins after pathological examination of the surgical specimen, however, the patient had pathological free margins after reoperation. Other 3 patients had hypercromy in the intervention region during the immediate postoperative.
CONCLUSION: Despite technological advances, the removal of the injury with a cold scalpel technique and the use of postoperative dressings are highly efficient, when combined, provide excellent aesthetic results with low complication rates and high rates of patients' satisfaction, whom mostly had improvement in quality of life after the procedure.
Keywords: Reconstructive surgical procedures; Rhinophyma; Nose diseases.
RESUMO
INTRODUÇÃO: Rinofima é uma condição estigmatizante para o indivíduo portador. Descrita desde a época de Hipócrates, a doença, popularmente conhecida como nariz de alcoólatra ou elefantíase nasal, é responsável por gerar uma enorme deformidade no nariz. Oriunda de um processo de hiperplasia e hipertrofia das glândulas sebáceas da região cutânea nasal, associadas à fibrose e dilatação dos vasos sanguíneos e tecido conjuntivo locais. O tratamento cirúrgico é considerado o procedimento de escolha para melhoria estética.
MÉTODOS: Estudo retrospectivo baseado na análise dos resultados de 11 pacientes, sendo dez homens e uma mulher, submetidos a tratamento do rinofima entre janeiro de 2010 e janeiro de 2016 no serviço de Cirurgia Plástica do Hospital Universitário da Universidade Federal de Juiz de Fora e Clínica Plastic Center.
RESULTADOS: Dos 11 pacientes operados, um homem de 72 anos apresentou carcinoma basocelular invasor expansivo com margens cirúrgicas comprometidas após análise anatomopatológica da peça cirúrgica, obtendo resultado anatomopatológico de margens livres após reoperação. Outros três pacientes apresentaram hipercromia na região de intervenção durante o pós-operatório imediato, mas obtiveram resultados satisfatórios 6 meses após procedimento.
CONCLUSÕES: Apesar dos avanços tecnológicos atuais, a retirada da lesão com bisturi frio e aplicação dos curativos pós-operatórios ainda demonstram ser altamente eficazes quando associadas, proporcionando excelentes resultados estéticos, com baixos índices de complicação e altos índices de satisfação dos pacientes, que em sua maioria obtiveram melhora da qualidade de vida após o procedimento.
Palavras-chave: Procedimentos cirúrgicos reconstrutivos; Rinofima; Doenças nasais.
Rhinophyma, which also known as the alcoholic nose or nasal elephantiasis, among others names, have been reported since the period of Hippocrates and such reports have remained throughout centuries, including the representation in the artistic world when in 1490 Domenico Ghirlandaio painted "An old man and his Grandson" containing a man with a nose suggesting the disease1. This disease has a strong association with alcoholism and rosacea, and some authors consider the final form of this latter2,3.
The disease occurs with hyperplasia and hypertrophy of the nasal skin sebaceous glands associated with fibrosis and dilatation of local blood vessels and connective tissue. These changes are responsible for given a tuberous aspect and darker color to the region (Figure 1).
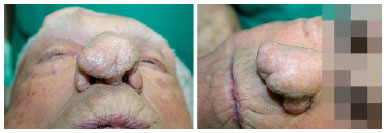
Figure 1. Patients with large deformities in the nose due to rhinophyma.
The disease affects mainly middle-aged and elderly men with history of alcoholism, and it affects about 5-10% of the population4, and/or rosacea that has values ranging from 0.5 to 10% of prevalence. Some studies report proportions of this disease of 12 men to 1 woman2. Other causes cited include a positive family history of rhinophyma, excessive sun exposure, high consumption of spicy foods and caffeine. All these factors may cause facial flushing and rosacea, and they constitute predisposing factors to the onset of the injury5.
It is also important to note that tuberous lesions have been associated with cases of malignant neoplasms such as basal cell carcinoma, which can affect 10% of patients, squamous cell carcinoma, and angiosarcoma, but these two latter are rare. Therefore, after surgical resection, each part must be analyzed based on the pathology2,3,6.
Clinical treatment is still little effective, but there are reports of good results with the use of isotretinoin before the onset of fibrosis7,8. However, little or no results were observed regarding fibrotic injury retract. For this reason, surgery is considered the gold standard, and this procedure have been done with the most diverse forms such as dermoablation, using high frequency equipment (Radiofrequency) and resection with cold scalpel9.
OBJECTIVE
To report evolution and results achieved using the shave excision technique in a group of patients with rhinophyma.
METHODS
This is a retrospective study based on analysis of the results from 11 patients (10 men and 1 woman). Patients ranged from 45 to 90 years, who underwent rhinophyma treatment between January 2010 and January 2016 in the Plastic Surgery at the Teaching Hospital of the Federal University of Juiz de Fora and a Plastic Center Clinic, using cold scalpel and membrane dressings to porous cellulose regeneration.
The procedure is done with sedation associated with local anesthetics (2% lidocaine + 0.5% bupivacaine combined with adrenaline 1/200,000). Local resection is done after asepsis and antisepsis with 2% chlorhexidine and tumescent infiltration of the injury, which facilitates the handling and resection of the affected area. We used 15 and/or 22 cold slides, ranging from type, size and nasal region of the injury. After surgical resection of rhinophyma, the nose is compressed with gauze moistened in anesthetic solution with adrenaline for about 5 minutes. After decompression, an electrocoagulation is used to perform hemostasis of the larger vessels.
Dressing begins with porous cellulose membrane or ointments based on zinc oxide, vitamins A and D, covered with dry gauze and microporous tape. Both dressing options are maintained for five to seven days and when removed were indicated the use of moisturizing cream and sunscreen on the spot.
RESULTS
Of the 11 patients who underwent surgery, 10 had satisfactory results without complications related to anesthesia, bleeding or infections on surgical site. Three patients complained about hyperchromia of the operated area that evolved satisfactorily 6 months after surgery.
A 72-year-old male with invasive basal cell carcinoma on his left lateral border of the nose, with surgical margins compromised after initial anatomicopathological examination of the surgical specimen, and reoperation for margin expansion 15 days after the initial procedure. Subsequently, a new anatomopathological result revelead a free margins after the reintervention (Figure 2).
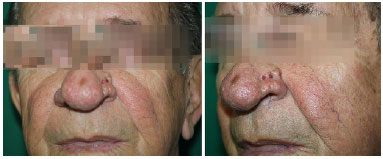
Figure 2. Ulcerative injuries in left lateral nasal margin, with positive results of basal cell carcinoma determined after anatomopathological analysis.
A 103-year-old patient with advanced rhinophyma did not undergo surgery because of lacking of patient and family interest and due to comorbidities of the patient that contraindicated the procedure. For this reason, the patient underwent only resection of basal cell carcinoma (BCC) and spindle cell carcinoma (SCC) on the face, and the rhinophyma was not removed.
The only female patient, aged 48 years, also had bilateral axillary and inguinal hydrosadenitis. She underwent several surgical procedures because of the suppurative hydrosadenitis recurrence.
All patients were evaluated 7, 15 and 30 days after the surgery. All patients returned for consultation between three and six months. All patients had satisfactory aesthetic results, and no new interventions were needed.
DISCUSSION
Several forms of surgeries have been used to treat rhinophyma. These procedures are always done with the aim to reduce complications before and after surgery and achieve the best aesthetic result. Today, most commonly used methods are: dermoablation, electrocoagulation, high frequency equipment (radiofrequency) and cold excision (shave excision), which was the focus of our study2,3,6,9.
Despite the small sample size, eleven cases, our findings are in agreement with literature data, regarding the incidence of malignancy and occurrence among men and women2.
Despite the existence of better techniques, using modern technologies, we opted for simple treatment that is easy to reproduce in a teaching service, present good results and does not require costly technological devices, which is Brazil is often unavailable in public health services (Figure 3).
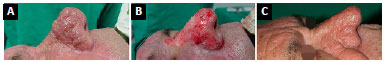
Figure 3. A: Preoperative profile; B: Intraoperative; C: Six months after surgery.
The great advantage of using the shave excision technique is the best visualization of the nasal bed area; this procedure enable to observe the nasal bed, without the presence of hypertrophied sebaceous glands5.
This technique main challenge is bleeding, even if the use of intumescent anesthetic solution with 1/200,000 adrenaline solution and manual compression of the nose. Bleeding may difficult to continue the surgery5.
The use of cellulose membrane dressings or IV gauze with zinc oxide ointments, vitamin A and D, provides a painless and comfortable post-operative without the need of daily or frequent dressing exchanges.
CONCLUSION
Despite the current technological advances, removal of lesion using cold scalpel and application of postoperative dressings, when associated, still highly effective and it provides excellent aesthetic results. The use of cold scalpel also present low complication rates and high satisfaction rates from patients. Most of patients report improvement in their quality of life after the procedure. Despite all advances, this technique use recurrence rate must be taken into account and this fact must be informed to the patient before the procedure.
COLLABORATIONS
MTD Analysis and/or interpretation of data; conception and design of the study; completion of surgeries and/or experiments; writing the manuscript or critical review of its contents.
MPDC Analysis and/or interpretation of data; statistical analyses; final approval of the manuscript; conception and design of the study; completion of surgeries and/or experiments; writing the manuscript or critical review of its contents.
MCD Analysis and/or interpretation of data; statistical analyses; conception and design of the study; completion of surgeries and/or experiments.
GVD Analysis and/or interpretation of data; statistical analyses; final approval of the manuscript; conception and design of the study; writing the manuscript or critical review of its contents.
LDC Analysis and/or interpretation of data; statistical analyses.
LVD Analysis and/or interpretation of data; statistical analyses.
LDC Analysis and/or interpretation of data; statistical analyses.
GASM Analysis and/or interpretation of data; statistical analyses.
REFERENCES
1. Ghirlandaio D. The complete works [Internet]. 2016 [cited 2016 Sep 7]. Available from: http://www.domenico-ghirlandaio.org/
2. Costa TC, Firme WAA, Brito LMR, Vieira MBG, Leite LAS. Rinofima: opções cirúrgicas utilizadas no Serviço de Cirurgia Plástica do Hospital Agamenon Magalhães - PE. Rev Bras Cir Plást. 2010;25(4):633-6. DOI: http://dx.doi.org/10.1590/S1983-51752010000400012
3. Sperli EA, Freitas JOG, Fischler R. Rinofima: tratamento com equipamento de alta frequência (radiofrequência). Rev Bras Cir Plást. 2009;24(4):504-8.
4. Vargas D, Oliveira MAF, Araujo EC. Prevalência de dependência alcoólica em serviços de atenção primária à saúde de Bebedouro, São Paulo, Brasil. Cad Saúde Pública. 2009;25(8):1711-20. DOI: http://dx.doi.org/10.1590/S0102-311X2009000800007
5. Sarifakioglu N, Sarifakioglu E. Simple, easy, and still effective treatment option in severe rhinophyma: shave and paste. Dermatol Ther. 2013;26(2):168-9. DOI: http://dx.doi.org/10.1111/j.1529-8019.2013.01542.x
6. Pitanguy I, Caldeira AML, Alexandrino A, Trevino MN. Rinofima considerações clínico-cirúrgicas. Rev Bras Cir. 1984;74(2):101-10.
7. Ertl GA, Levine N, Kligman AM. A comparison of the efficacy of topical tretinoin and low-dose oral isotretinoin in rosacea. Arch Dermatol. 1994;130(3):319-24. PMID: 8129410 DOI: http://dx.doi.org/10.1001/archderm.1994.01690030051008
8. Marsden JR, Shuster S, Neugebauer M. Response of rosacea to isotretinoin. Clin Exp Dermatol. 1984;9(5):484-8. DOI: http://dx.doi.org/10.1111/j.1365-2230.1984.tb00842.x
9. Wetzig T, Averbeck M, Simon JC, Kendler M. New rhinophyma severity index and mid-term results following shave excision of rhinophyma. Dermatology. 2013;227(1):31-6. PMID: 24008235 DOI: http://dx.doi.org/10.1111/j.1365-2230.1984.tb00842.x
1. Sociedade Brasileira de Cirurgia Plástica, Belo Horizonte, MG, Brazil
2. Universidade Federal de Juiz de Fora, Juiz de Fora, MG, Brazil
3. Faculdade de Ciências Médicas e da Saúde de Juiz de Fora, Juiz de Fora, MG, Brazil
Institution: Hospital Universitário, Universidade Federal de Juiz de Fora, Juiz de Fora, MG, Brazil.
Corresponding author:
Marilho Tadeu Dornelas
Rua Dom Viçoso, 20
Juiz de Fora, MG, Brazil - Zip Code 36026-390
E-mail: marilho.dornelas@ufjf.edu.br
Article received: January 15, 2017.
Article accepted: July 9, 2017.
Conflicts of interest: none.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter