

Original Article - Year 2017 - Volume 32 -
Immediate breast reconstruction using permanent expanders
Reconstrução imediata de mama com uso de expansores permanentes
ABSTRACT
INTRODUCTION: Breast cancer has become increasingly prevalent, resulting in a greater number of patients undergoing mastectomies. Post-mastectomy immediate reconstruction is an important alternative treatment in the various stages of breast reconstruction.
METHODS: A retrospective study was conducted with 34 patients who underwent mastectomy or adenomastectomy, with or without preservation of the areola-papillary complex, followed by immediate reconstruction using a permanent expander. The expander used was of the Becker type 35 and anatomically shaped, having a volume ranging from 365 to 565 ml, with the 460-ml expander being the most frequently used.
RESULTS: The results were considered "highly satisfactory" by 85% of the patients. The complication rate was 17.6%; two patients had skin necrosis on the edges of the surgical wound, two patients presented scar retraction in the surgical wound, one patient presented seroma, and only one patient had expander loss because of late infection after the start of chemotherapy. Thirteen patients underwent radiotherapy, of whom 53% (n = 7) had mild radiodermatitis and 30% (n = 4) had moderate radiodermatitis without other complications.
CONCLUSION: Immediate reconstruction using definitive expanders presents a good treatment option for patients who will undergo total or partial mastectomy.
Keywords: Breast; Mammoplasty; Breast neoplasms; Devices for tissue expansion.
RESUMO
INTRODUÇÃO: O câncer de mama tem se tornado cada vez mais prevalente e com isso maior é o número de pacientes submetidas a mastectomias. A reconstrução imediata pós-mastectomia é uma alternativa importante de tratamento nas diversas etapas da reconstrução mamária.
MÉTODOS: Estudo retrospectivo de 34 pacientes submetidas à mastectomia ou adenomastectomia, com ou sem preservação do complexo aréolo-papilar seguida de reconstrução imediata com uso de expansor permanente. O expansor utilizado foi do tipo Becker 35, de formato anatômico, com volume variando de 365 ml a 565 ml, sendo mais utilizado o de 460 ml.
RESULTADOS: O resultado foi considerado muito satisfatório por 85% das pacientes, a taxa de complicações foi de 17,6%, sendo que duas pacientes apresentaram necrose de pele nos bordos da ferida operatória, duas pacientes apresentaram retração cicatricial na ferida operatória, uma paciente apresentou seroma e somente uma paciente teve perda do expansor por infecção tardia após início da quimioterapia. Treze pacientes realizaram radioterapia, 53% (n = 7) apresentaram radiodermite leve e 30% (n = 4) radiodermite moderada, sem outras complicações.
CONCLUSÃO: A reconstrução imediata com o uso de expansores definitivos apresenta uma boa proposta de tratamento às pacientes que serão submetidas a mastectomias totais ou parciais.
Palavras-chave: Mama; Mamoplastia; Neoplasias da mama; Dispositivos para expansão de tecidos.
Breast cancer has become increasingly prevalent and are being diagnosed earlier. With this, the number of patients undergoing mastectomies has become even greater. According to the Department of Informatics of the Unified Health System, since 2008, more than 63,500 women have undergone mastectomy throughout the country, a number that equals one surgery every 40 minutes in the last 5 years.
The modern era of breast reconstruction using tissue expanders started with Radovan in the late 1970s and early 1980s1. Since then, not only the surgical technique of implantation of the expander/implants, but also the devices themselves have been greatly improved2. In the 1980s, a new advancement in breast reconstruction was brought about with the development of the permanent expander by Hilton Becker3.
Post-mastectomy immediate reconstruction is an important alternative treatment in the various stages of breast reconstruction. Considered as a safe and acceptable procedure, it has not shown any evidence of cancer injury and may be suggested for patients with disease stages 0, I, and II4,5.
OBJECTIVE
The objective of this study was to demonstrate the author's experience and to analyze a series of cases in which patients subjected to total mastectomy or adenomastectomy had immediate reconstruction of their breasts with the use of Becker permanent expanders, regarding surgical technique, evolution, advantages and disadvantages, aesthetic result, and complications.
METHODS
A retrospective study was conducted with 34 patients who underwent mastectomy or adenomastectomy, with or without preservation of the aortic-papillary complex (APC), followed by immediate breast reconstruction using a permanent expander at the Hospital da Luz, São Paulo, SP, Brazil between January 2013 and December 2014. The base of the operated breast and the contralateral breast were used as indicators of the volume of the expander to be used. The expander used was of the Becker type 35 and anatomically shaped, having a volume ranging from 365 to 565 ml, with the 460-ml expander being the most frequently used. All the patients were duly informed and signed an informed consent form. The work followed the principles of the Declaration of Helsinki.
For the insertion of the expander, submuscular gaps were made by elevating the pectoralis major in continuity with the rectus abdominis and anterior serratus muscles. After insertion of the implant in this submuscular plane, the border of the pectoralis was closed, joining this muscle to the serratus, for total muscular coverage of the implant. The remote valve was placed on the subcutaneous side. All the patients used subcutaneous aspiration drainage in the area removed by mastectomy for about 1 week.
The expansions were performed in a weekly program, under aseptic conditions, in an outpatient setting. Expansion usually began in the second week after surgery and was performed until symmetry was achieved or until the volume desired by the patient was reached, for posterior symmetrization of the breasts.
RESULTS
The mean age of the patients was 45 years (range, 28-68 years). All the reconstructions were immediate and performed on the right in 16, on the left in another 16, and bilaterally in 2. Thirteen patients (38%) underwent radiotherapy. The mean time of the expansion was 5 weeks, respecting the individual characteristics of patients and concomitance of chemotherapy.
The result was considered "highly satisfactory" by 85% of the patients. Similarity with the natural breast was more easily achieved in the cases of small breasts and with preservation of the APC. Even in the cases with complications, the patients also evaluated the result as "satisfactory" and "good" after resolution of the condition. No complications occurred regarding the valves. The symmetrization of the opposite breast was performed after 6 months on an average (Figures 1 and 2).
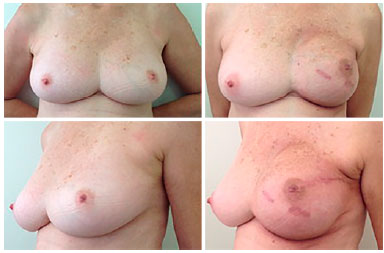
Figure 1. Appearance before and after mastectomy with preservation of the areola-papillary complex and reconstruction immediately, in the seventh month, and in the fourth month after radiotherapy.
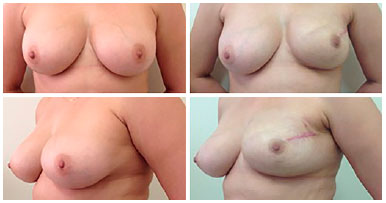
Figure 2. Appearance before and after adenomastectomy with preservation of the areola-papillary complex and reconstruction immediately and in the third month after operation. Radiotherapy was not necessary.
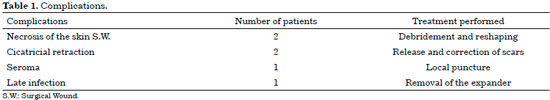
The complication rate was 17.6%. Two patients presented skin necrosis on the edges of the surgical wound, caused by excessive surgical manipulation and/or excessive traction during mastectomy. Resections were necessary for the necrosis and wound, without loss of the expander. Both cases presented partial loss of the APC, but with good evolution and satisfactory final results.
Two patients presented scar retraction in the surgical wound, one of them with a need for reoperation to release the retractions and aesthetic improvement of the scar, without evidence of capsular retraction and without the need to change the expander. One patient presented with seroma, which was resolved with local punctures and showed good improvement after the end of the expansions. One patient had late infection after chemotherapy, extrusion, and expander removal (Table 1).
Of the 13 patients who underwent radiotherapy, all had their expansions completed before the beginning of the sessions, 53% (n = 7) had mild radiodermatitis and 30% (n = 4) had moderate radiodermatitis. All with good evolution. None of the patients had a capsular contracture, and changing the expander was not necessary (Figures 3 and 4).
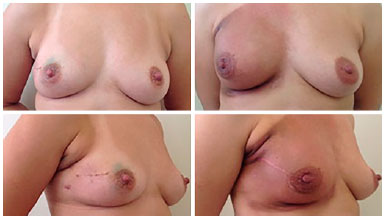
Figure 3. Appearance before and after adenomastectomy with preservation of the areola-papillary complex and reconstruction immediately and in the fifth month after operation, and 1 month after radiotherapy, still with evidence of intense radiodermatitis.
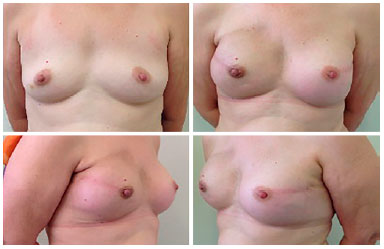
Figure 4. Appearance before and after bilateral adenomastectomy with preservation f the areola-papillary complex, in the 10th postoperative month, and in the second month after radiotherapy.
DISCUSSION
The number of reconstructions with breast expanders has increased, mainly owing to the increasingly early diagnosis of cancer cases. Younger patients have shown to be more demanding for a reconstruction as soon as possible and opt for immediate reconstruction, despite knowing the possible risks if radiotherapy is needed6,7.
The permanent expander allows its submuscular placement with adequate technical ease, low risk of complications, and highly satisfactory results. In addition, progressive expansion of the musculature provides a more graceful breast contour. Other advantages include the fact that it does not cause damage and scarring in other areas of the body, the low surgical time, and possibility of manipulation of breast volume. Moreover, autologous flaps can still be used when necessary8-10.
The complication rate was similar to that found in the literature8-10, with most complications being minor. Thus, they did not interfere with the final result. Radiotherapy, historically known as a major complication factor, caused only radiodermatitis, without major morbidity and complications. Considering that some cases are only indicated for radiotherapy after anatomopathological analysis, that is, after the time to decide whether the reconstruction will be immediate or late.
CONCLUSION
Immediate reconstruction using definitive expanders presents a good treatment option for patients who will undergo total or partial mastectomy, especially in the early stages of the disease. The procedure is simple and safe, with high satisfaction rates and low complication rates. Even when no information is available about the need for radiotherapy, reconstruction using definitive expanders can be performed and is a good option, as the complication rate from radiotherapy is also low.
COLLABORATIONS
GFP Final approval of the manuscript; conception and design of the study; completion of surgeries and/or experiments; writing the manuscript or critical review of its contents.
LVSP Completion of surgeries and/or experiments; writing the manuscript or critical review of its contents.
REFERENCES
1. Radovan C. Breast reconstruction after mastectomy using the temporary expander. Plast Reconstr Surg. 1982;69(2):195-208. PMID: 7054790 DOI: http://dx.doi.org/10.1097/00006534-198202000-00001
2. Spear SL, Spittler CJ. Breast reconstruction with implants and expanders. Plast Reconstr Surg. 2001;107(1):177-87. DOI: http://dx.doi.org/10.1097/00006534-200101000-00029
3. Pedroso DB, Daher JC, Cammarota MC, Benedik Neto A, Faria CADC, Cintra Junior R. Expansores permanentes de Becker. Rev Bras Cir Plást. 2010;25(Supl):1-102.
4. Guimarães GS, Daher JC, Cammarota MC. Reconstrução mamária com expansor permanente: uma outra alternativa. Rev Bras Cir Plást. 2008;23(2):75-81.
5. Oliveira CF. Reconstrução mamária com implante expansor definitivo: experiência pessoal. Rev Bras Cir Plást. 2013;28(1):78-84. DOI: http://dx.doi.org/10.1590/S1983-51752013000100014
6. Becker H. Breast reconstruction using an inflatable breast implant with detachable reservoir. Plast Reconstr Surg. 1984;73(4):678-83. PMID: 6709750 DOI: http://dx.doi.org/10.1097/00006534-198404000-00031
7. Mansel RE, Horgan K, Webster DJ, Shrotria S, Hughes LE. Cosmetic results of immediate breast reconstruction post-mastectomy: a follow-up study. Br J Surg. 1986;73(10):813-6. PMID: 3768653 DOI: http://dx.doi.org/10.1002/bjs.1800731018
8. Becker H. The expandable mammary implant. Plast Reconstr Surg. 1987;79(4):631-7. PMID: 3823256 DOI: http://dx.doi.org/10.1097/00006534-198704000-00023
9. Malata CM, McIntosh SA, Purushotham AD. Immediate breast reconstruction after mastectomy for cancer. Br J Surg. 2000;87(11):1455-72. DOI: http://dx.doi.org/10.1046/j.1365-2168.2000.01593.x
10. Leal PR, Cammarota MC, Palma L, Sbalchiero J. Reconstrução imediata de mama: avaliação das pacientes operadas no Instituto Nacional de Câncer no período de junho de 2001 a junho de 2002. Rev Bras Mastol. 2003;13(4):149-58.
1. Hospital da Luz, São Paulo, SP, Brazil
2. Sociedade Brasileira de Cirurgia Plástica, São Paulo, SP, Brazil
Institution: Hospital da Luz, São Paulo, SP, Brazil.
Corresponding author:
Gustavo Felipe Pasqual
Rua Jaguarari, 4980, casa 86
Natal, RN, Brazil - Zip Code 59064-500
E-mail: pasqual.gu@yahoo.com.br
Article received: April 12, 2017.
Article accepted: September 23, 2017.
Conflicts of interest: none.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter