

Original Article - Year 2018 - Volume 33 -
Perception of nasal reduction by radix and tip augmentation rhinoplasty
Percepção da redução nasal pela rinoplastia de aumento do radix e da ponta
ABSTRACT
INTRODUCTION: A straight bridge has always been the aesthetic ideal. Simple hump removal, the classical and most commonly applied method, can have aesthetic and functional consequences. However, great resistance to augmentation procedures persists because most patients request reduction and the benefits of improving nasal balance are counterintuitive. An augmented nose can look smaller, a particular benefit in patients with thick, inelastic skin or a large lower nose. On the other hand, decreased size perception after raising of the radix and tip is very common but has not been measured to date.
METHODS: This study created graphic and real interventions to achieve a straight bridge through radix and tip raising and analyzed how patients and independent observers perceive these changes. A sample of 42 sequential rhinoplasty patients was analyzed, including nine cases of primary surgery and dorsal convexity.
RESULTS: There was a 6.5% mean augmentation after graphic computing intervention but a perception of size reduction (p = 0.004). There was a 1% mean augmentation after rhinoplasty and an overall size reduction perception.
CONCLUSION: Correction of the nasal dorsum, making a straight bridge through slightly increasing radix and tip, creates the perception of a decreased nose size.
Keywords: Rhinoplasty; Size perception; Nose; Nasal cartilage.
RESUMO
INTRODUÇÃO: O dorso reto tem sido sempre um ideal na rinoplastia estética. A simples remoção da giba tem sido o método clássico e mais utilizado, mas pode ter consequências estéticas e funcionais adversas. Ainda existe grande resistência a procedimentos de aumento, porque a maioria dos pacientes solicitam redução e porque os benefícios de melhoria do equilíbrio nasal pelo aumento não são intuitivos. Um nariz aumentado pode parecer menor, o que é um benefício em particular em pacientes com pele espessa ou com o aspecto de terço inferior grande. Por outro lado, a percepção de redução com o aumento do radix e da ponta é muito comum, embora nunca tenha sido medida.
MÉTODOS: Esse estudo cria intervenções gráficas e reais para criar um dorso reto por meio do aumento do radix e da ponta e analisa como os pacientes e observadores independentes percebem as modificações. Analisou-se uma amostra de 42 casos consecutivos de rinoplastia. Desses, foram incluídos os que tinham dorso convexo e eram cirurgias primárias, restando 9 casos.
RESULTADOS: Houve aumento médio de 6,5% no tamanho do nariz na após a modificação gráfica, enquanto houve percepção de redução do nariz (p = 0,004). Houve aumento médio de 1% após a rinoplastia, enquanto houve percepção de redução.
CONCLUSÃO: A retificação do dorso nasal pelo aumento do radix e da ponta causa percepção de redução do nariz.
Palavras-chave: Rinoplastia; Percepção de tamanho; Nariz; Cartilagens nasais.
A straight bridge has always been the aesthetic ideal for rhinoplasty surgeons and patients1-3. Hump removal is the classical and most commonly applied method4-7; however, consensus is lacking8,9. It might yield known aesthetic and functional consequences, like internal valve insufficiency, inverted "V," supra-tip deformity, and other complications10,11.
Systematic hump removal is still used to correct dorsal convexity. This is possibly due to surgeons' resistance to performing augmentation procedures. This resistance might have several causes. The fear of a size augmentation perception when patients generally request nose reduction is possibly among them12.
On the other hand, several authors have already spoken about concepts that lead to the perception of a reduced consequence of size augmentation in some areas. Constantian, for example, affirmed that bottom-heavy unbalanced noses tend to appear better and look smaller after radix augmentation, which alters the nasal proportion13,14. This may be due to the size contrast illusion phenomenon as shown in Figure 115-17.
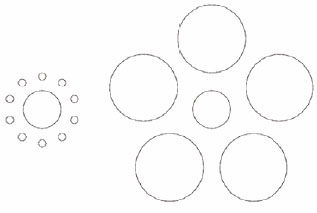
Figure 1. Example size contrast optical illusion. The center circle appears smaller on the right side than on the left side, but the two are the same size.
However, the current literature fails to provide objective data to support this. Thus, the question that motivates this study is: does the dorsal hump correction obtained by raising the radix and tip cause the perception of a nose size reduction?
OBJECTIVE
To evaluate whether the dorsal hump correction obtained by raising the radix and tip causes the perception of a nose size reduction.
METHODS
This study was designed to evaluate the size perception of the nose after tip and radix augmentation procedures to achieve a straight bridge. Forty-two sequential patients were operated upon by the same surgeon between December 2013 and November 2014 in Fortaleza-Ceará-Brazil. Fifteen men (36%) and 27 women (64%) 22-55 years of age (mean, 37.7 years; standard deviation [SD], 8.45 years). Twelve patients with a dorsal convexity on the proximal and medium third who were candidates for a first rhinoplasty were chosen. We excluded one patient who was lost to follow-up and two in whom the dorsal convexity persisted after surgery.
All determinations of the Helsinki agreement were observed and all patients were provided informed consent. The authors have no disclosures to declare.
The central idea was to perform an intervention that changed the shape of the nose, determine whether there was reduction or increase in size, and identify if it resulted in a reduction or augmentation perception.
All patients underwent two-dimension digital photographic documentation of both profiles18,19 captured with a 10-Megapixel Canon Rebel XP dSLR camera with an 18-55-mm lens fixed in 55 mm. The nose subject was approximately 75 cm away from the lens. Images were stored in JPEG format. Patients were oriented to look forward naturally20,21. Five shots were taken of each profile.
We used the area of the nose in the profile view picture for the size measurement. To access the nasal area, we used UTHSCSA Image Tool 3.0 software to draw the nasal perimeter22. Externally, the line followed the transition from the nose contour to the blue background. Internally, we used the following known points as landmarks to create an arbitrary limit from the nose to the face: nasion3; subnasale24; and alar-cheek junction18.
We drew two points 15 mm apart from each other as horizontally as possible in the lower third of the noses to calibrate the software, which then calculated the nasal area in square millimeters. This method of registry is represented in Figure 2.
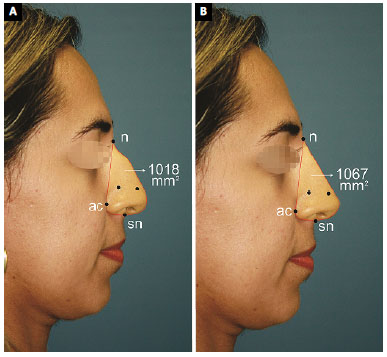
Figure 2. A: Case 9. Images before and after the intervention created by computer graphics. There was an increase of the radix and tip without lowering of the dorsum; B: The red line delimits the perimeter of the nose. The nasal area is shown in square millimeters. The two black dots are 15 mm apart and are used to calibrate the program.
To evaluate satisfaction, all patients filled in the Rhinoplasty Outcome Evaluation (ROE), which was translated to Brazilian Portuguese and validated, at the preoperative evaluation25,26. This is a six-item questionnaire. Each item has a five-category Likert scale. ROE score ranges from 0 (most unsatisfied) to 100 (most satisfied)25.
After the registration phase, we divided the study cohort into two branches. One of them underwent an intervention via graphic computing and the other underwent an actual rhinoplasty. We called the first computer-assisted intervention stage and the second rhinoplasty stage.
Computer-Assisted Intervention Stage
We used DoctorViewTM software (version 3.5.1.583; Data Tech) to modify one randomly chosen image for each patient. We raised the radix and tip until a straight bridge was reached. We did not lower the dorsum in any case. The software paired pre- and postintervention pictures side-by-side in identical positions and sizes.
To determine whether the intervention significantly increased the nasal area (NA), we applied Student's t-test for paired samples. All analyses were performed using SPSS software (version 22; IBM SPSS).
Paired images were presented on a high-definition 32-inch screen to six independent non-medical observers who were unaware of the study purposes. They were asked to answer the following question, marking an X next to the best choice.
Relative to the nose in the left side image, the nose in the right side image is:
(-2) much smaller; (-1) a little smaller; (0) the same size; (1) a little bigger; (2) much bigger.
We used a one-sample Student's t-test to evaluate whether there was a size reduction perception.
Rhinoplasty Intervention Stage
In parallel, we analyzed size perceptions after rhinoplasty. All patients were operated on by the same surgeon using a closed approach under general anesthesia following the techniques described by Constantian8 and Sheen and Sheen27 with a few personal adaptations. The closed approach offers a benefit that the open approach does not: the ability to appreciate and adjust proportion changes intraoperatively.
All patients underwent radix or total dorsal grafts made by septal or ear cartilage. All of them underwent cartilage tip grafting. Small dorsal lowering procedures were accomplished in seven cases (cases 1, 2, 3, 5, 6, 7, and 9).
Figures 3, 4, 5, 6, 7, and 8 show pre- and postoperative images and the specific maneuvers used in each case.
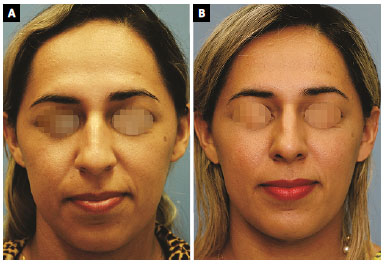
Figure 3. A: Preoperative frontal view of case 9; B: Frontal view 12 months after closed rhinoplasty. The central portion of the septum was removed using a Killian incision. An intercartilaginous incision was performed, lowering of the dorsum, with Fomon scissors, and a small retraction of the cartilaginous dorsum without opening of the ceiling with a #11 scalpel blade. A radix graft with stalked septal cartilage was performed and adhered with fresh blood33. Multiple Sheen grafts were applied to the tip. The caudal septum was trimmed as the final step. No strut-like grafts or sutures were placed in the tip cartilage. No osteotomy was performed.
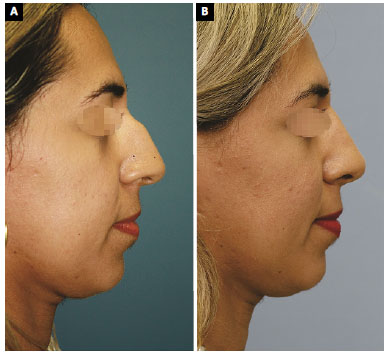
Figure 4. A: Case 9. Preoperative profile view; B: Case 9. Profile view 12 months after rhinoplasty. The technique was described above.
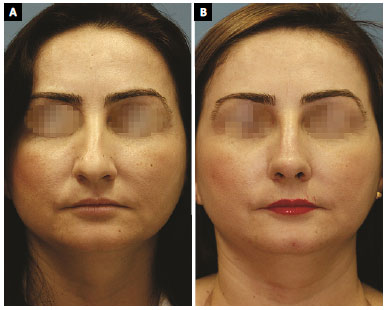
Figure 5. A: Case 8. Preoperative frontal view; B: Frontal view 12 months after closed rhinoplasty. The central portion of the septum was removed using a Killian incision. The right conchal cartilage was harvested using the posterior approach. An intercartilaginous incision was performed with Fomon scissors to lower the dorsum. The cartilaginous dorsum was not retracted. A radix graft was performed with chopped septal cartilage and adhered using fresh blood33. Caudal repositioning of the lateral crus of lower lateral cartilage was performed using the technique described by Constantian. Multiple Sheen grafts were applied to the tip. The caudal septum was trimmed as the final step. No strut-like grafts or sutures were placed in the tip cartilage. No osteotomy was performed.
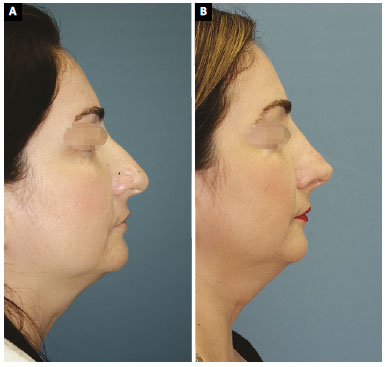
Figure 6. A: Case 8. Preoperative profile view. 6B. Case 8. Profile view 12 months after the rhinoplasty. Technique described above; B: Case 8. Profile view, 12 months after rhinoplasty. Technique described above.
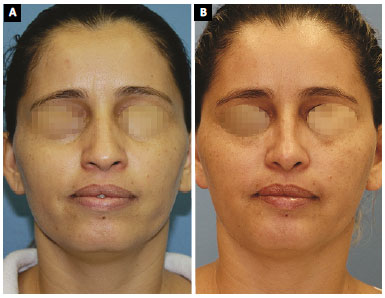
Figure 7. A: Case 7. Frontal view; B: Frontal view 12 months after the closed rhinoplasty. The central portion of the septum was removed using a Killian incision. Resection of the cranial portion of the lateral crus was made using a transcartilaginous incision. Reduction of the cartilaginous back was performed using Fomon scissors. The cartilaginous dorsum was slightly recessed with a #11 scalpel blade without opening of the ceiling. A radix graft with double linear septal cartilage was performed in the proximal portion. A double-tip graft was made without fixation with sutures. An internal low-high osteotomy was performed. There were no struts or sutures from the tip cartilage.
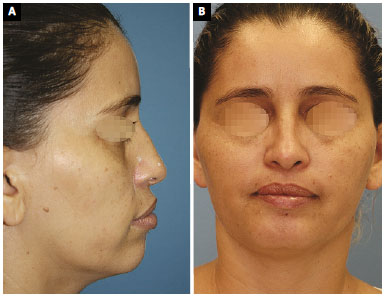
Figure 8. A: Case 7. Preoperative profile view; B: Case 7. Profile view 12 months after the rhinoplasty.
Photographs were taken 90 days after the intervention by the same method used previously (five shots of each profile per patient) and the nasal areas were calculated as already described.
We calculated nasal area from all of 10 images of each patient and then calculated the mean nasal area for each patient. Thereafter, we applied two-sample Student's t-test to evaluate whether the rhinoplasty actually increased the nasal areas.
To evaluate the nasal size perception, each patient judged their own case. The exact point of time of the analysis was 90 days after surgery, and all pre- and postoperative pictures in the frontal, profile, and oblique views were freely available to them on a 32-inch high-definition screen.
Patients were asked to answer the following question:
Relative to the preoperative period, your nose is:
(-2) much smaller; (-1) a little smaller; (0) the same size; (1) a little bigger; or (2) much bigger.
This question was the same as that asked in the computer-assisted stage.
We used the Wilcoxon test to confirm the assumption that patients found their noses smaller after surgery. The statistical analysis performed with SPSS software (v. 22, SPSS) for values of α = 0.05.
Patients also answered the ROE questionnaire again 90 days after the rhinoplasty. Two-sample Student's t-test was applied to the statistical analyses.
RESULTS
Nine cases met the inclusion criteria. All were women 24-37 years old (mean, 31.7 years; SD, 8.64 years). Only cases 1, 4, and 9 had low radix according to Gunter and Hackney's definition. Only case 4 had low radix according to Constantian's definition.
Computer-assisted intervention stage results
There was size augmentation in all cases (mean, 6.5%; range, 2.2-13.9%) and the mean NA shifted from 935.56 mm2 (SD = 104.089) to 997.11 mm2 (SD = 123.301) after the intervention (p = 0.001).
Yet, there was size reduction perception, as 37 (68%) of the 54 fulfilled questionnaires were in the reduction perception categories (-2 or -1), while eight (15%) were in the augmentation perception categories (1 or 2).
The mean result of all questionnaires also pointed toward a statistically significant reduction perception (mean = -0.6222; SD = 0.5333; p = 0.004).
Dividing the sample in two groups, using the percentage augmentation median (4,8%) as the cut-off point, group A (cases 3, 4, and 5) was above and group B (cases 1, 2, and 7) was below the median. In this manner, group A had a greater size augmentation (mean, 11.2%) than group B (mean, 3%) but less of a size reduction perception (mean, -0.3) than group B (mean, -1.1) (p = 0.11).
We created the two groups using the size perception median as the cut-off point (-0.7). Group A (cases 4, 6, 7, and 8) was above the median and group B (cases 1, 2, 5, and 9) was below the median. Group A had less of a size reduction perception (mean, -0.4) than group B (mean, -1.2), but group A had a greater augmentation (mean, 7.9%) than group B (mean, 4.3%; p = 0.1).
Rhinoplasty intervention stage results
The mean nasal area shifted from 950.61 mm2 (SD, 101.59) to 957.38 mm2 (SD, 97.51) in this phase with no statistical significance within this sample (p = 0.392). However, there was a size reduction perception in eight of the nine (89%) cases (mean, -1.44; p = 0.004).
The mean ROE shifted from 23 to 79.2 (p < 0.001). Patients in the -2 (much smaller) perception category showed less of a satisfaction increase (mean, 395%) than patients in the -1 (a little smaller) perception category (mean, 564% in ROE score).
Patients who underwent augmentation in the nasal area had a larger increase in the ROE score than the patients whose nasal areas were diminished after rhinoplasty (498% versus 364%).
Therefore, we verified nasal area augmentation in both periods of the study, although it could be a random result in the real intervention branch, while there was size reduction perception in both phases.
We also verified that patients were more satisfied with their noses in the postoperative period, but we could not correlate the degree of ROE score increase to either the presence of real augmentation or reduction or the category of the size reduction perception (-1 or -2).
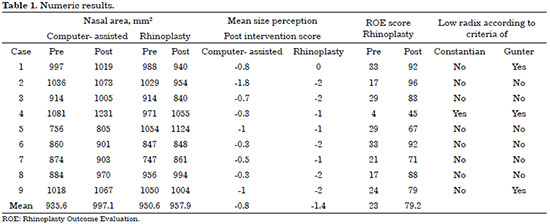
Table 1 shows all of the numeric results.
DISCUSSION
Although it is known that structural augmentation improves contour and respiration in rhinoplasty28, high resistance persists from both surgeons and patients to accept augmentation procedures, particularly in the dorsum. Thus, the classical dorsal hump treatment is removal6.
This resistance may be due to several reasons: possible complications like infections, displacement, visibility, distortion, and others28. However, the fact that patients want to reduce their noses and not augment them29 might be a significant source of misgiving as well.
Under these circumstances, series like Foda's7 show no dorsal augmentation in any of his 500 cases despite the most common diagnosis being dorsal hump. The question that comes to our minds is: Was there any patient in which low radix was the main cause of the dorsal hump?
Becker and Pastorek6 increased the radix in 5-10% of cases. On the other hand, in one of his series, Constantian found that 38% of his 50 primary cases and 93% of his 150 secondary cases had low radix or low dorsum8,30. This reinforces the idea that there must be high resistance against augmentation rhinoplasty.
Constantian speaks extensively about balance concepts and affirms that bottom-heavy noses look not only better but also smaller once the radix is raised8,13,14,30. These concepts could be very heartwarming for those surgeons who wish to go against the general reduction idea but fear patient reactions. Nevertheless, literature fails to provide definitive objective evidence that they are right.
That is why the idea of testing size perception in a more objective manner was considered for this study. Once the objective is to test the size perception relative to shape, not to test any surgical technique, we chose to use computer-assisted augmentation as the intervention instead of real surgery to build the main frame of the trial. Using rhinoplasty as the intervention, on the other hand, would approximate the study to the applicable reality. Thereby, we developed the idea of having both computer-assisted and rhinoplasty stages in the study.
Regarding the register method, we chose digital photography, which is considered valid for pre and postoperative evaluations19,23,31. Despite its differences to reality, the resulting bias is present in both pre- and postintervention images, diminishing its influence.
Term size was chosen because we found it greatly related to patients' desire to reduce the nose, which is a general and not specific request29. Profile nasal area is the measurement that best represents the size regarding maneuvers from which we wish to evaluate the results (radix and tip rise).
Since there was no specific methodology to evaluate size perception in the literature, we built a scale with five categories based on the already available tools such as ROE. It is also a Likert scale, as others commonly used32.
We found a mean size increase of 6.5% (SD, 3.65%) after computer-assisted intervention, while there was an evident size reduction perception (mean, -0.6222; SD, 0.5333; p = 0.004). Although there are no similar studies, this result is compatible to some other publications, like those of Constantian, who says that nasal base looks smaller with radix augmentation and that tip grafts make noses not only look but become shorter8,14).
In a different situation, there was no shortening maneuver in the computer-assisted intervention, what leads us to the conclusion that there might be a perception of size reduction even without a real reduction in nasal length.
Considering that size augmentation caused the perception of size reduction, can we say that there is a correlation between the degree of augmentation and the degree of reduction perception? Probably not, as we found that the patients who had more augmentation (above the median [4.8%]) showed less of a perception of size reduction than patients who had less augmentation (below the median [-0.3 versus -1.1]).
Likewise, the group that had a more evident perception of size reduction (below the median, -0.7) had a smaller degree of augmentation than the group that had a less evident perception of size reduction (4.3% versus 7.9%). This way, the perception of size reduction possibly loses its strength beyond some degree of augmentation, but the present data are insufficient to produce a consistent assumption.
We intended to approximate our data to the surgical reality when the real branch was created. Although the use of rhinoplasty cases brings us closer to reality, it does not remove the need for a graphic computing intervention branch. Otherwise, it would be necessary to analyze a much bigger sample to obtain statistically significant data due to the inherent bias of real cases.
One of the main sources of bias is the lack of reproducibility of the photography positioning method18. Differences greater than 10% in the nasal area appear even in pictures taken on the same day due to small changes in patient position. It does not happen in the computer-assisted branch because the software uses the same image in the same position to compare status before versus after the intervention.
The use of rhinoplasty as an intervention also provided a satisfactory evaluation and enabled comparison to the virtual branch of the study, which led us to some other conclusions.
The mean size augmentation in this branch was smaller (1%) than that in the computer-assisted branch (6.5%). There was even a reduction in four of the nine cases, possibly due to nose shortening and/or dorsum lowering (proceeded in seven of nine cases). Considering that the p value was 0.392 for the size augmentation, this may be a random result and one cannot say that rhinoplasty systematically increased nose size.
On the other hand, the lack of statistical significance could be due to positioning bias, and it is possible that a larger sample could get to a more statistically significant result. Just as we cannot affirm that this surgical approach increases noses, we cannot say that it decreases them. Still, even if there is reduction, it is not as great as in the traditional method to correct the nasal hump, the routine removal.
The statistical significance for the perception of size reduction was at the same level after rhinoplasty and after computer-assisted intervention (p = 0.004), even with a smaller number of evaluations (nine versus 54). This perception tendency was even stronger than in the virtual phase, as 56% were in the -2 category and 33% were in the -1 category. This is possibly related to the fact that there was less augmentation, which reinforces the hypothesis that the perception of size reduction loses its strength after a certain point. In fact, we cannot confirm or refute this.
Emotional evolvement is another possible reason for the stronger perception of size reduction in this phase. In this case, the more satisfied with the outcome, the stronger the perception of size reduction. Otherwise, we cannot affirm that, as the patients who reported a small reduction (mean ROE increase, 564%) were more satisfied than those who reported a larger reduction (mean ROE increase, 395%).
This study shows that these shape modifications leads to a size reduction perception, even with actual size augmentation. Although it is supported by the literature, other authors based their conclusions on their observations without performing a specific confirmation study8,13,14,27,28.
A small chin might accentuate the perception of a super projected nose28, and nasal grafts influence nasal base size directly or indirectly27. Furthermore, Constantian affirmed that the higher the dorsum, the smaller the appearance of the nasal base and that tip grafts cause visual and real shortening effects14.
Size contrast illusions are a possible explanation for this15-17. Thus, a lack of volume in some region of the nose might lead to an exaggerated perception of some other area sizes. Likewise, low radix patients might tend to perceive a large nasal base, so radix augmentation would be helpful to achieve better nasal balance.
However, this study may raise a question that goes beyond. Considering that only one patient had low radix, even if we exclude this case, we achieve roughly the same results, so it is possible that radix and tip augmentation are helpful to correct large size illusions and create diminishing illusions for patients with dorsal convexity without low radix.
Together with his definition of ideal position, Gunter said that surgeons should use their aesthetic judgment to find an appropriate radix position.
Therefore, the findings of this study might be useful to increase the confidence and awareness of surgeons who choose to use augmentation grafts that the simple existence of dorsal convexity makes the patient a possible candidate for radix and tip grafting.
CONCLUSION
Our results show that correcting the nasal dorsum by creating a straight bridge and increasing the radix and tip creates the perception of a decreased nose size.
COLLABORATIONS
EATF Analysis and/or interpretation of data; statistical analyses; final approval of the manuscript; conception and design of the study; completion of surgeries and/or experiments; writing the manuscript or critical review of its contents.
JGLF Analysis and/or interpretation of data; final approval of the manuscript.
FRFT Analysis and/or interpretation of data; final approval of the manuscript; writing the manuscript or critical review of its contents.
REFERENCES
1. Constantian MB. Toward refinement in rhinoplasty. Plast Reconstr Surg. 1984;74(1):19-32. PMID: 6739597 DOI: http://dx.doi.org/10.1097/00006534-198407000-00003
2. Burget GC, Menick FJ. The subunit principle in nasal reconstruction. Plast Reconstr Surg. 1985;76(2):239-47. PMID: 4023097 DOI: http://dx.doi.org/10.1097/00006534-198508000-00010
3. Rohrich RJ, Muzaffar AR, Janis JE. Component dorsal hump reduction: the importance of maintaining dorsal aesthetic lines in rhinoplasty. Plast Reconstr Surg. 2004;114(5):1298-308. DOI: http://dx.doi.org/10.1097/01.PRS.0000135861.45986.CF
4. Joseph J. Treatise on rhinoplasty. Berl Klin Wochenschr. 1907;44:470.
5. Joseph J. Cartographer Rhinoplasty and facial plastic surgery with a supplement on mammaplasty and other operations in the field of plastic surgery of the body: an atlas and textbook. Phoenix: Columella Press; 1987.
6. Becker DG, Pastorek NJ. The radix graft in cosmetic rhinoplasty. Arch Facial Plast Surg. 2001;3(2):115-9. DOI: http://dx.doi.org/10.1001/archfaci.3.2.115
7. Foda HM. External rhinoplasty: a critical analysis of 500 cases. J Laryngol Otol. 2003;117(6):473-7. DOI: http://dx.doi.org/10.1258/002221503321892325
8. Constantian MB. Rhinoplasty: craft and magic. St Louis: Quality Medical Publishing; 2009.
9. Gunter JP, Rohrich RJ, Adams WP Jr. Dallas Rhinoplasty: Nasal Surgery by the Masters. 2nd ed. St. Louis: Mosby; 2007.
10. Sheen JH. A new look at supratip deformity. Ann Plast Surg. 1979;3(6):498-504. DOI: http://dx.doi.org/10.1097/00000637-197912000-00003
11. Constantian MB. The incompetent external nasal valve: pathophysiology and treatment in primary and secondary rhinoplasty. Plast Reconstr Surg. 1994;93(5):919-31. DOI: http://dx.doi.org/10.1097/00006534-199404001-00004
12. Pochat VD, Alonso N, Meneses JVL. Avaliação funcional e estética da rinoplastia com enxertos cartilaginosos. Rev Bras Cir Plást. 2010;25(2):260-70.
13. Constantian MB. An alternate strategy for reducing the large nasal base. Plast Reconstr Surg. 1989;83(1):41-52. PMID: 2909077 DOI: http://dx.doi.org/10.1097/00006534-198901000-00009
14. Constantian MB. Distant effects of dorsal and tip grafting in rhinoplasty. Plast Reconstr Surg. 1992;90(3):405-18. DOI: http://dx.doi.org/10.1097/00006534-199209000-00007
15. Aglioti S, DeSouza JF, Goodale MA. Size-contrast illusions deceive the eye but not the hand. Curr Biol. 1995;5(6):679-85. PMID: 7552179 DOI: http://dx.doi.org/10.1016/S0960-9822(95)00133-3
16. McCready D. On size, distance, and visual angle perception. Percept Psychophys. 1985;37(4):323-34. PMID: 4034350 DOI: http://dx.doi.org/10.3758/BF03211355
17. Bruno N. When does action resist visual illusions? Trends Cogn Sci. 2001;5(9):379-82.
18. Farkas LG, Bryson W, Klotz J. Is photogrammetry of the face reliable? Plast Reconstr Surg. 1980;66(3):346-55. PMID: 7422721
19. Nechala P, Mahoney J, Farkas LG. Digital two-dimensional photogrammetry: a comparison of three techniques of obtaining digital photographs. Plast Reconstr Surg. 1999;103(7):1819-25. PMID: 10359240 DOI: http://dx.doi.org/10.1097/00006534-199906000-00002
20. Madsen DP. Natural Head Position: A Photographic Method and an Evaluation of Cranial Reference Planes in Cephalometric Analysis [Thesis]. Adelaide: The University of Adelaide, School of Dentistry; 2007.
21. Pereira AL, De-Marchi LM, Scheibel PC, Ramos AL. Reproducibility of natural head position in profile photographs in children aged 8 to 12 years old, with and without an auxiliary cephalostat. Dental Press J. Orthod. 2010;15(1):65-73.
22. Kim HS, Noh SU, Han YW, Kim KM, Kang H, Kim HO, et al. Therapeutic effects of topical application of ozone on acute cutaneous wound healing. J Korean Med Sci. 2009;24(3):368-74. DOI: http://dx.doi.org/10.3346/jkms.2009.24.3.368
23. Guyuron B. Precision rhinoplasty. Part I: The role of life-size photographs and soft-tissue cephalometric analysis. Plast Reconstr Surg. 1988;81(4):489-99. PMID: 3347657 DOI: http://dx.doi.org/10.1097/00006534-198804000-00001
24. Hochman B, Castilho HT, Ferreira LM. Padronização fotográfica e morfométrica na fotogrametria computadorizada do nariz. Acta Cir Bras. 2002;17(4):258-66. DOI: http://dx.doi.org/10.1590/S0102-86502002000400011
25. Alsarraf R. Outcomes research in facial plastic surgery: a review and new directions. Aesthetic Plast Surg. 2000;24(3):192-7. DOI: http://dx.doi.org/10.1007/s002660010031
26. Izu SC, Kosugi EM, Brandão KV, Lopes AS, Garcia LB, Suguri VM, et al. Normal values for the Rhinoplasty Outcome Evaluation (ROE) questionnaire. Braz J Otorhinolaryngol. 2012;78(4):76-9. PMID: 22936141 DOI: http://dx.doi.org/10.1590/S1808-86942012000400015
27. Sheen JH, Sheen AP. Aesthetic Rhinoplasty. 2nd ed. St Louis: Mosby Incorporated; 1987.
28. Dresner HS, Hilger PA. An overview of nasal dorsal augmentation. Semin Plast Surg. 2008;22(2):65-73. DOI: http://dx.doi.org/10.1055/s-2008-1063566
29. Hormozi AK, Toosi AB. Rhinometry: an important clinical index for evaluation of the nose before and after rhinoplasty. Aesthetic Plast Surg. 2008;32(2):286-93. PMID: 18026781 DOI: http://dx.doi.org/10.1007/s00266-007-9057-y
30. Constantian MB. Four common anatomic variants that predispose to unfavorable rhinoplasty results: a study based on 150 consecutive secondary rhinoplasties. Plast Reconstr Surg. 2000;105(1):316-31. DOI: http://dx.doi.org/10.1097/00006534-200001000-00051
31. Aksu M, Kaya D, Kocadereli I. Reliability of reference distances used in photogrammetry. Angle Orthod. 2010;80(4):670-7. DOI: http://dx.doi.org/10.2319/070309-372.1
32. Munshi J. A method for constructing Likert scales [Internet]; 2014. [acesso 2018 Jan 30]. Disponível em: http://www.academia.edu/6621299/A_Method_for_Constructing_Likert_Scales DOI: http://dx.doi.org/10.2139/ssrn.2419366
33. Öreroglu AR, Çakır B, Akan M. Bone dust and diced cartilage combined with blood glue: a practical technique for dorsum enhancement. Aesthetic Plast Surg. 2014;38(1):90-4. DOI: http://dx.doi.org/10.1007/s00266-013-0256-4
1. Sociedade Brasileira de Cirurgia Plástica, São Paulo, SP, Brazil
2. Universidade Federal do Ceará, Fortaleza, CE, Brazil
3. Clínica Eduardo Furlani, Fortaleza, CE, Brazil
4. Hospital do Coração e Pulmão de Messejana, Fortaleza, CE, Brazil
Institution: Clínica Eduardo Furlani, Fortaleza, CE, Brazil.
Corresponding author:
Eduardo Antonio Torres Furlani
Rua Barbosa de Freitas, 1990 - Aldeota
Fortaleza, CE, Brazil - Zip Code 60170-021
E-mail: eduardo@eduardofurlani.com.br
Article received: March 20, 2017.
Article accepted: January 26, 2018.
Conflicts of interest: none.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter