

Case Report - Year 2018 - Volume 33 -
Reconstruction of the humerus and rehabilitation of the elbow using an osteomyocutaneous scapular flap: a case report
Reconstrução de úmero e reanimação do cotovelo com retalho osteomiocutâneo da escápula: relato de caso
ABSTRACT
INTRODUCTION: We report a case of reconstruction of the proximal third of the right humerus and rehabilitation of the elbow in a 20-year-old male patient who was injured in an automobile accident and developed bone necrosis of 5 cm at the proximal third of the humerus and avulsion of the brachial biceps.
METHODS: A scapular bone flap was used, together with a latissimus dorsi myocutaneous flap, using subscapular vessels for the pedicle.
RESULTS: The patient had excellent postoperative course, presenting in the 2-month postoperative period with bone consolidation and initiation of elbow flexion.
CONCLUSIONS: This flap modality is a safe and useful option for bone reconstruction.
Keywords: Elbow; Humerus; Myocutaneous flap; Superficial muscles of the back; Osteonecrosis.
RESUMO
INTRODUÇÃO: No presente trabalho, relatamos um caso de reconstrução do terço proximal do émero direito e reanimação do cotovelo de um paciente masculino, de 20 anos, vítima de acidente automobilístico, com necrose óssea de 5 cm no terço proximal do úmero e avulsão do bíceps braquial.
MÉTODOS: Utilizamos o retalho ósseo da escápula, associado ao retalho miocutâneo do grande dorsal, tendo como pedículo os vasos subescapulares.
RESULTADOS: O paciente teve excelente evolução no pós-operatório, apresentando-se, no pós-operatório de 2 meses, com consolidação óssea e iniciando a flexão do cotovelo.
CONCLUSÕES: Perante a utilização do retalho descrito, concluímos que esta modalidade de retalho se insere no arsenal dos retalhos ósseos de maior segurança nas reconstruções ósseas em geral.
Palavras-chave: Cotovelo; Úmero; Retalho miocutâneo; Mésculos superficiais do dorso; Oesteonecrose.
Bone flaps from the lateral border of the scapula have been well studied and used in the last three decades, mainly subsequent to the first anatomical studies that focused on this bone donor area and described flap elevation with vascularization from branches of circumflex vessels of the scapula1.
These initial studies were subsequently confirmed by another author who thoroughly examined the anatomy of the scapula and contributed to the anatomical knowledge of this region2. In 1986, the largest number of clinical cases was presented, with safe and successful use of the scapular flap in 26 patients3.
In 1988, researchers introduced a second vascular pedicle to the lateral border of the scapula, originating not only from the circumflex scapular artery, but also the thoracodorsal artery and its angular branches4.
In the 1990s, a series of 36 anatomical dissections was published, confirming previous studies. The findings were applied in 8 patients who underwent a pedicled transfer of the scapular flap using 2 separate pedicles5. Following these initial studies, applications of the lateral scapular border flap have continued to expand, and have been successfully used in bone reconstruction of the limbs and face6,7.
Anatomical considerations
1. The circumflex scapular system: The lateral border of the scapula is vascularized primarily by two systems or pedicles. The most important are represented by the circumflex scapular artery, a branch of the subscapular artery that supplies collateral branches to neighboring muscles along its path inside the triangular space, and periosteal and medullary branches to the lateral border of the scapula.
2. The thoracodorsal system: The angular branches of the thoracodorsal artery have been described as the vascular supply to the tip of the scapula, as well as for the lateral border via an anastomotic network between the angular vessels and osseous branches of the scapular circumflex system4.
Based on these studies, we report a case in which we used a bone flap from the free border of the scapula for reconstruction of the upper third of the humerus, along with a latissimus dorsi musculocutaneous flap to restore elbow flexion, using a subscapular pedicle with scapular and thoracodorsal circumflex arteries.
OBJECTIVE
The objective of this study was to report a case of reconstruction of the proximal third of the humerus and rehabilitation of the elbow using a scapular bone flap, together with a musculocutaneous latissimus dorsi flap with a single pedicle including subscapular vessels.
METHODS
This case report describes a patient who was treated at the Hospital das Clínicas de Fernandópolis, in Fernandópolis, SP, Brazil in 2001. A review of the literature was performed using books and national and international publications obtained by consulting four databases: MEDLINE (National Library of Medicine, USA), LILACS (Literatura Latino-Americana e do Caribe de Informação em Ciências da Saéde), BIREME, and the Pan-American Health Organization (PAHO/WHO) databases, along with queries to the PubMed portal.
Abstracts pertinent to the theme were identified in the databases and the selected articles were read in their entirety to identify different treatment methods used for musculoskeletal reconstruction and discuss the applicability of osteomyocutaneous scapular flap, a complex procedure of extreme technical difficulty.
This case report was approved by the Research Ethics Committee of the Faculty of Medicine of São José do Rio Preto - FAMERP.
CASE REPORT
This case describes a 20-year-old male patient who was injured in an automobile accident 1 year prior, with avulsion of the brachial biceps and an exposed fracture of the proximal third of the right humerus. The patient presented with exposure and necrosis of 5 cm at the proximal third of the humerus, in addition to inability to flex the elbow. He had undergone 3 bone curettage procedures and was on continuous antibiotic therapy for 1 year (Figure 1).
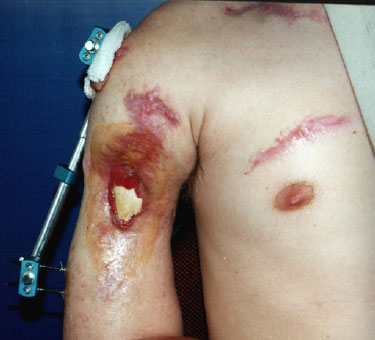
Figure 1. Preoperative aspect showing exposure and bone necrosis at the proximal third of the humerus, in addition to destruction of the flexor muscles of the forearm.
We decided to perform an osteomyocutaneous scapular and latissimus dorsi flap for bone reconstruction of the humerus and rehabilitation of the elbow. The flap was transferred with a pedicle to the subscapular artery using a double pedicle (circumflex artery of the scapula and thoracodorsal artery), taking care to avoid devascularizing the teres major or denervating the serratus anterior to prevent scapular winging (Figures 2 and 3).
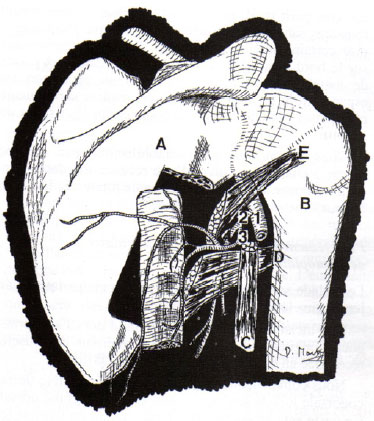
Figure 2. Drawing showing the layout of flap elevation and vascularization. A: Scapula; B: Humerus; C: Long head of the triceps; D: Teres major muscle; E: Teres minor muscle; 1: Axillary artery; 2: Subscapular artery; 3: Circumflex scapular artery; 4: Thoracodorsal artery.
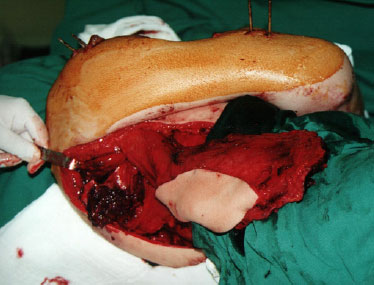
Figure 3. Intraoperative aspect, patient in left lateral decubitus. Note the lateral border of the right scapula already elevated, along with the latissimus dorsi muscle and overlying skin.
The patient had an excellent postoperative course, and presented at the 2-month follow-up with bone consolidation and initiation of elbow flexion (Figure 4).
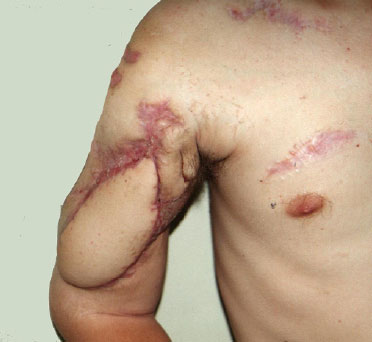
Figure 4. 2-month postoperative aspect showing the reconstructed area and the patient initiating flexion of the elbow.
DISCUSSION
A bone flap from the lateral border of the scapula presents great advantages in the reconstruction of the humerus compared to that from other bone sources commonly used for this purpose, such as the iliac flap and the fibular flap:
- Proximity to the receiving area: the flap can be transposed in a pedicled manner, without the need of microsurgical technique;
- Safety: the subscapular system is, without dispute, the most widely used for flap preparation and implementation, with large published studies showing its safety and limited anatomical variation;
- Diversity of possible elevations: no other flap area offers greater diversity of possible flaps, starting from a scapular and parascapular cutaneous flap, through a flap of the serratus anterior muscle and the muscular, musculocutaneous, and osteomyocutaneous flap (with the tenth rib) of the latissimus dorsi, up to the association of these flaps with the lateral scapular border flap;
- Quality of bone transferred: the lateral border of the scapula is a richly vascularized cancellous bone, making its use for reconstruction superior to that of the rib;
- The presence of a long pedicle: this provides a wide arc of rotation to this flap and greater safety and ease for free transfers.
CONCLUSION
Considering the use of a flap from the lateral scapula border described in this report, together with numerous anatomical and clinical studies already published, we conclude that the osteomyocutaneous scapular flap is an excellent option in cases of large tissue loss in the upper limb. It can safely be raised pedically, as demonstrated, and can also be associated with transposition of the latissimus dorsi and overlying skin. The pedicle is easily dissected and visualized; moreover, in addition to the scapula, the rib can be used as a donor bone source. This bone flap, in addition to a flap from the iliac crest and fibula, is safely and commonly used in bone reconstruction in general, and especially in the upper limb.
COLLABORATIONS
HRPF Analysis and/or interpretation of data; statistical analyses; final approval of the manuscript; conception and design of the study; completion of surgeries and/or experiments; writing the manuscript or critical review of its contents.
JAF Writing the manuscript or critical review of its contents; completion of surgeries and/or experiments.
JAF Completion of surgeries and/or experiments.
GM Completion of surgeries and/or experiments.
REFERENCES
1. Téot L, Bosse JP, Moufarrege R, Papillon J, Beauregard G. The scapular crest pedicled bone graft. Int J Microsurg. 1981;3:257-62.
2. dos Santos LF. The vascular anatomy and dissection of the free scapular flap. Plast Reconstr Surg. 1984;73(4):599-604. PMID: 6709742 DOI: http://dx.doi.org/10.1097/00006534-198404000-00014
3. Swartz WM, Banis JC, Newton ED, Ramasastry SS, Jones NF, Acland R. The osteocutaneous scapular flap for mandibular and maxillary reconstruction. Plast Reconstr Surg. 1986;77(4):530-45. PMID: 3952209 DOI: http://dx.doi.org/10.1097/00006534-198604000-00003
4. Deraemaecker R, Thienen CV, Lejour M, Dor P. The serratus anterior scapular free flap: a new osteomuscular unit for reconstruction after radical head and neck surgery. In Proceedings of the Second International Conference on Head and Neck Cancer; 1988 Jul 31-Aug 5; Boston, MA, USA.
5. Coleman JJ 3rd, Sultan MR. The bipedicled osteocutaneous scapula flap: a new subscapular system free flap. Plast Reconstr Surg. 1991;87(4):682-92. PMID: 2008466 DOI: http://dx.doi.org/10.1097/00006534-199104000-00013
6. Frodel JL Jr, Funk GF, Capper DT, Fridrich KL, Blumer JR, Haller JR, et al. Osseointegrated implants: a comparative study of bone thickness in four vascularized bone flaps. Plast Reconstr Surg. 1993;92(3):449-55. DOI: http://dx.doi.org/10.1097/00006534-199309000-00010
7. Funk GF. Scapular and parascapular free flaps. Facial Plast Surg. 1996;12(1):57-63. DOI: http://dx.doi.org/10.1055/s-2008-1064494
1. Universidade Estadual Paulista Campus de Botucatu, Botucatu, SP, Brazil
2. Faculdade de Medicina de Fernandópolis, Unicastelo, Fernandópolis, SP, Brazil
3. Colégio Brasileiro de Cirurgiões, Rio de Janeiro, RJ, Brazil
4. Hospital das Clínicas de Fernandópolis, Fernandópolis, SP, Brazil
5. Sociedade Brasileira de Ortopedia, São Paulo, SP, Brazil
Institution: Hospital das Clínicas de Fernandópolis, Fernandópolis, SP, Brazil.
*Corresponding author:
Humberto Regis de Paula Faleiros
Avenida Amadeu Bizelli, 979
Centro - Fernandópolis, SP, Brazil - Zip Code 15600-000
E-mail: betofaleiros@yahoo.com
Article received: February 13, 2012.
Article accepted: January 26, 2018.
Conflicts of interest: none.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter