

Case Report - Year 2019 - Volume 34 -
Elastic suture: a treatment option for extensive skin loss
Sutura elástica: uma opção no tratamento de extensas perdas cutâneas
ABSTRACT
Extensive skin loss presents major challenges for plastic surgeons, making it necessary to develop different techniques to close extensive wounds. In this context, the elastic suture technique was performed in two patients at the Independência Hospital of the Divina Providência Group in Porto Alegre. This alternative technique was fast and effective and had a low cost. The technique is divided into two stages: the elastic suture itself, which consists of the approximation of the wound edges with the aid of an elastic band; and closure of the skin already approximated in the previous stage. The elastic suture is a highly safe and simple closure technique with the ability to approximate the edges of extensive wounds, avoiding the use of more complex techniques in some cases.
Keywords: Suture techniques; Bottom edge; Wounds and injuries; Rubber; Healing
RESUMO
Em meio a tantos desafios aos quais os cirurgiões plásticos são impostos quando se trata de grandes perdas cutâneas, faz-se necessário o desenvolvimento de diferentes métodos de fechamento de grandes feridas. Assim sendo, foi realizada a técnica da sutura elástica em dois pacientes do Hospital Independência do grupo Divina Providência em Porto Alegre, uma alternativa que se demonstrou rápida, eficaz e de baixo custo. A técnica é dividida em duas etapas, a primeira com a sutura elástica propriamente dita - na qual consiste na maior aproximação dos bordos com auxílio de um elástico -, e a segunda com o fechamento da pele já aproximada pela fase anterior. Assim sendo, com o uso da técnica nesses dois pacientes, foi possível concluir que a sutura elástica é uma técnica de fechamento simples, com grande segurança e funcionalidade para aproximação de bordos de grandes feridas, evitando, em alguns casos, o uso de técnicas mais complexas.
Palavras-chave: Técnicas de sutura; Extremidade inferior; Ferimentos e lesões; Borracha; Cicatrização
INTRODUCTION
Extensive skin loss in the lower limbs presents great treatment challenges. These lesions are caused by extensive trauma, exposed fractures, vasculopathies, and neoplasms and are characterized by difficulty approximating wound edges, which can lead to aesthetic and functional damage1.
The treatment options range from primary closure to reconstruction using distant flaps. Some plastic surgeons specialize in this area and perform different techniques to close the lesions depending on their extension. In this context, the elastic suture was included in the therapeutic strategy for lower-limb reconstruction, a technique divided into two surgical times: the aid of an elastic sutured into the skin that approximates the wound edges; and the removal of this elastic and the wound edges sufficiently approximated so only a simple suture closes the wound. This mechanism uses the biomechanical properties of the skin with the aid of only a sterile elastic band. The elastic suturing was performed in two patients at the Independência Hospital of Porto Alegre, RS.
The present study aimed to describe the elastic suture technique and confirmed its safe applicability in cases of skin loss in the lower limb based on the description of two surgical cases and a literature review.
METHODS
The present study consists of two case reports of patients treated at the Independência Hospital of the Divina Providência Group in Porto Alegre, RS, in 2017. Based on the surgical method used, a literature review was conducted using the Google Scholar, PubMed, and Lilacs databases. The abstracts that were relevant for the topics were initially identified and selected; subsequently, the open access articles that clearly addressed the elastic suture treatment were reviewed.
Two patients were selected for the two stages of the procedure. The first stage includes the elastic suture and consists of debridement of the wound edges and suturing of the sterile elastic into the most superficial layer of the skin. The elastic was fixed to the skin with a mononylon thread, and was interlaced and sutured back into the skin. This process was repeated until the wound edges were approximated in all affected areas. One week after this first stage, the elastic was removed and the wound was fully closed with mononylon 3.0 thread.
CASE REPORTS
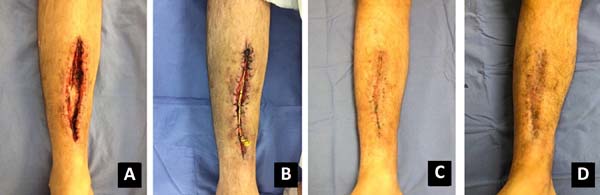
G.L.S.N., 24-year-old man. The patient suffered a motorcycle accident
in October 2014 and required surgical treatment for a right tibial
shaft fracture. The postoperative course was successful and he was
discharged. In July 2017, the patient returned to the hospital
complaining of progressive exposure of the synthetic material with
signs of a site infection. Thus, the plaque was removed in July
2017. However, the patient had an extensive surgical wound that
required debridement and assessment by the plastic surgeon. The
lesion size in the anterior region of the right leg was 15 ×
4.3 cm (Figure 1). The patient
then underwent elastic suturing to cover the lesion. The first stage
of the procedure was performed in August 2017; in the second stage 1
week later, the wound already measured 15 × 1.1 cm, which
made the primary suturing possible, and the patient was discharged 4
days after the second surgery. The patient’s condition progressed
well, the surgical wound healed completely, and he was discharged
from the plastic surgery team’s outpatient clinic in February
2018.
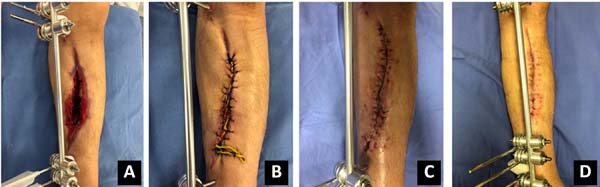
N.D.S., 45-year-old woman. The patient was suicidal in October 2017
accidentally injured her left leg with a shotgun blast.
Consequently, she had an exposed fracture in the left tibia and
fibula with a lesion in the anterior region of the leg measuring 17
× 4.5 cm (Figure 2). An
orthopedic procedure to treat the fractures of both bones of the leg
using an external fixator was conducted and an assessment by the
plastic surgeon was requested. Elastic suturing was indicated and
performed in December 2017 in two stages, and the wound’s width had
decreased to 1.2 cm 1 week later. The patient progressed adequately
after plastic surgery and continues to be followed up at the
hospital outpatient clinic.
DISCUSSION
After the technique was performed, the lesion healed as well as with the use of grafts and flaps since collagen is the main structure of the healing process, as it is constantly produced and degraded by fibroblasts and exerts tensile strength and supports the tissue. Throughout the basic stages, the produced collagen is replaced by the formation of cross-links between the fibers2. Therefore, the elastic suture works at this healing stage, facilitating and accelerating this wound tensile process.
In addition, during the first 24–36 hours, epithelial cells are produced and migrate to the central area of the lesion and induce another force that favors closure of the wound edges. However, the elastic suture is more effective during the maturation stage of the wound healing process since the wound is then under constant contraction due to the movement of all the surrounding thick skin, reducing the area of the disordered scar tissue2.
The tensile suture technique helps prevent the excessive productions of collagen and epithelial tissue, which cause scarring defects due to the differentiation of fibroblasts to myofibroblasts. Moreover, use of the elastic suture in elderly patients can overcome the lack of tissue flexibility, while the progressive decrease in collagen production can be beneficial in the wound healing maturation stage in diabetic patients since most wound healing stages are impaired by high blood glucose levels3.
The biomechanical principle of tissue tensile strength is the main mechanism explored in the elastic suture technique. The distribution of the tensile strength of the skin increases metabolic activity, which promotes vessel development and collagen fiber proliferation for tissue healing. Moreover, the viscoelastic properties of the skin allow gradual extension by a continuous traction–creep phenomenon3. Since primary closure of lesions is the first treatment choice whenever possible, the healing process associated with elastic suturing leads to this primary closure at the end of the procedure.
The comparison of two techniques of elastic suturing demonstrated that fixation of the elastic subcutaneously and in the superficial fascia spared the tissue from necrosis. Raskin’s technique in 19934 proposed fixation of the interlaced elastic directly on the wound edges, whereas the technique of Leite et al. in 19965 proposed fixation of the elastic subcutaneously and in the superficial fascia3,6. We used Raskin’s technique in both cases of the present study.
CONCLUSION
The outcomes of our two patients were very positive and corroborated findings already described in the literature. This technique was effective, low cost, fast, and safe and resulted in good wound healing. In addition, it did not leave a second scar in the donor area as occurs with graft use.
COLLABORATIONS
|
DSF |
Final manuscript approval, project administration, realization of operations and/ or trials, supervision, writing - original draft preparation, writing - review & editing. |
|
ALP |
Analysis and/or data interpretation, conception and design study, data curation, final manuscript approval, realization of operations and/or trials, writing - original draft preparation, writing - review & editing. |
|
YPS |
Analysis and/or data interpretation, conception and design study, data curation, final manuscript approval, formal analysis, methodology, writing - review & editing. |
REFERENCES
1. Magalhães MAB, Petroianu A, Martins SGO, Resende V, Alberti LR, Barbosa AJA, et al. Fechamento de grandes feridas com fita elástica de borracha em coelhos. Rev Col Bras Cir. 2015;42(1):56-61.
2. Tazima MFGS, Vicente YAMVA, Moriya T. Biologia da ferida e cicatrização. Medicina (Ribeirão Preto). 2008;41(3):259-64. DOI: http://dx.doi.org/10.11606/issn.2176-7262.v41i3p259-264
3. Vidal MA, Mendes Junior CES, Sanches JA. Sutura elástica - uma alternativa para grandes perdas cutâneas. Rev Bras Cir Plást. 2014;29(1):146-50.
4. Raskin KB. Acute vascular injuries of the upper extremity. Hand Clin. 1993;9(1):115-30.
5. Leite NM, Reis FB, Cristian RW. Rev Bras Ortop. Tratamento de ferimentos deixados abertos com o método de sutura elástica. 1996;31(8):687-9.
6. Santos ELN, Oliveira RA. Sutura elástica para tratamento de grandes feridas. Rev Bras Cir Plást. 2012;27(3):475-7. DOI: http://dx.doi.org/10.1590/S1983-51752012000300026
1. Hospital Independência, Porto Alegre, RS,
Brazil
2. ULBRA, Canoas, RS, Brazil.
Corresponding author: Douglas Severo Fraga Av. Andarai, nº 566, apto 1110 - Passo D’ areia, Porto Alegre, RS, Brazil Zip Code 91350-110 E-mail: fragadp@ig.com.br / drdouglasfraga@gmail.com
Article received: May 15, 2018.
Article accepted: November 11, 2018.
Conflicts of interest: none.




 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter