

Case Report - Year 2019 - Volume 34 -
Sequels of burns in the face: autologous skin graft breast-face , a treatment option. Case report
Sequelas de queimadura em face: enxerto cutâneo autólogo mama-face, uma opção de tratamento. Relato de caso
ABSTRACT
Introduction: Burns are one of the most severe traumatic injuries and their treatment requires a multidisciplinary approach, where the role of the plastic surgeon is vital. The plastic surgeon is entrusted with the challenging goal of restoring the skin's protective function and simultaneously recovering the aesthetic aspect of the burnt area.
Case report: A 27-year-old woman underwent a mastopexy with inclusion of implants, where the skin removed from the breast was used as a full-thickness graft in the mandibular and submental area for the treatment of a scar. The patient showed complete integration of the graft, and no areas of epidermolysis were observed. The aesthetic results were excellent, and the patient was completely satisfied; moreover, an improvement in the dyschromic and hypertrophic cicatricial areas was observed.
Conclusion: An autologous graft using breast skin is a good alternative for the treatment of sequelae of burns on the face and provides excellent aesthetic results.
Keywords: Burns; Scar; Skin; Breast; Face
RESUMO
Introdução: As queimaduras constituem uma das lesões traumáticas mais graves e seu
tratamento requer uma abordagem multidisciplinar, em que o papel do
cirurgião plástico é fundamental. Restabelecer a função de proteção da pele,
mas também recuperar a estética da área, queimada são objetivos desafiadores
que o cirurgião plástico procura atingir.
Relato de Caso: Paciente feminino de 27 anos submetida a mastopexia com inclusão de
implantes, em que se aproveitou a pele retirada da mama para realizar um
enxerto de espessura total em região mandibular e submentoniana para
tratamento de cicatriz. A paciente teve uma integração completa do enxerto,
sem evidenciar-se áreas de epidermólise. Os resultados estéticos foram
excelentes, conseguindo a satisfação da paciente e melhoria das áreas
discrômicas e hipertróficas cicatriciais.
Conclusão: O enxerto autólogo a partir da pele da mama constitui uma boa alternativa
para o tratamento de sequelas de queimaduras em face, possibilitando ótimos
resultados estéticos.
Palavras-chave: Queimaduras; Cicatriz; Pele; Mama; Face
INTRODUCTION
Burns are a type of injury that occurs predominantly at home, mainly in the kitchen and, generally, affects children. Burns may cause significant damage, sometimes resulting in psychological problems and even social consequences for the patients, their families, and the people with whom they are in contact. Burns may also leave scars, contractures, and other types of sequelae that limit physical function and lead to changes in the quality of life. Mastopexy with implants, may provide the necessary material for skin grafting, besides improving the degree of breast ptosis. Women with sequelae of burns on the face may benefit from an autologous breast-face skin grafting.
OBJECTIVES
Full-thickness skin grafts are often preferred when it is necessary to cover face defects. Generally, the donor areas in such cases include the scalp, neck, pre- and post-auricular region, nasolabial sulcus, supraclavicular region, and eyelids. This study aimed to report the results of reconstruction of sequelae of burns on the face using a full-thickness skin graft obtained from an atypical region, in this case the breast, after mastopexy.
CASE REPORT
This case report was assisted by the author of this work in the Prof. Ronaldo Pontes Plastic Surgery Service. A 27-year-old woman residing in the city of Niterói, Rio de Janeiro, Rio Grande do Norte, came to an evaluation appointment due to a burn sequela on the face. When she was 3 years old, the patient experienced burns caused by a fire after throwing a bottle of alcohol into a barbecue area. She had lesions on her face, cervical region, and left leg.
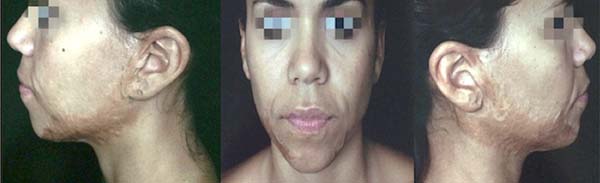
Cicatricial retraction was noted in the noble areas affected, and she visited the plastic surgery department for the treatment of the sequelae 24 years after the accident (Figure 1).
At the time, she also complained of mammary ptosis and a nodule in the left breast diagnosed 2 months ago (Figure 2). The patient was admitted for the surgical procedure. Initially, mastopexy was performed and mammary implants were used; the skin was resected, and a nodule in the left breast was excised and sent for anatomopathological study.
Subsequently, 155-mL polyurethane silicone implants were bilaterally implanted. During this procedure, a full-thickness skin graft from the breast was removed; the graft was adequately prepared and preserved in 0.9% physiological saline solution until the recipient bed was prepared (Figure 3).
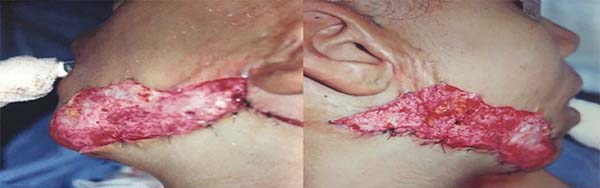
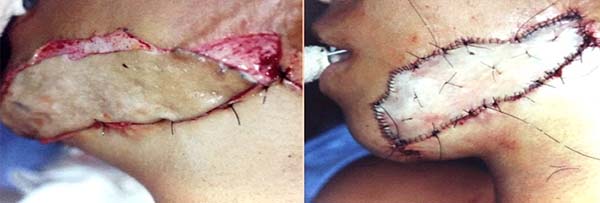
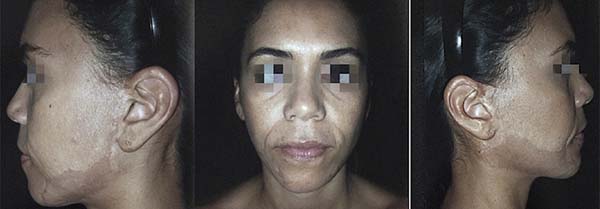
The skin from the burn scars from the mandibular to the pre-auricular regions and the scar on the chin was excised, and the recipient bed with a favorable aspect for grafting was prepared. Soon after, the autologous breast-face skin graft was set in the recipient areas (Figure 4). At the end of the procedure, an occlusive Brown’s dressing was applied. The histopathological results of left breast nodule showed adenofibrosis mastopathy and from the resected scars, only scarring proliferation of collagen fibers. The evolution was good, and the aesthetic results after 5 years, both in the donor and in the recipient areas, were satisfactory (Figure 5).
The results obtained in the autologous breast-face graft in a female patient submitted to mastopexy with implants made at the same time as the surgical correction of burns sequelae in the face were satisfactory. A significant improvement in the texture of the face scar tissue was observed (Figure 5), with a decrease in dyschromia and scar retraction.
DISCUSSION
Burns are still regarded as the most devastating aggression experienced by a human being, and includes physical and psychological scarring, as well as metabolic and functional changes1,2. The incidence of the sequelae of burns is increasing, perhaps due to patient survival after the acute phase, which has increased in recent years3. In Brazil, burns are the fourth leading cause of death by accident in children, and the seventh for hospital admission4. The standard procedure, as a first option, to cover full-thickness defects of the skin caused by trauma or surgery is autologous skin grafting5.
Skin grafting is the transfer of autologous skin cells that are arranged in the anatomical order, but do not have an intact blood supply. The following three phases are commonly described during the integration of grafts: (1) plasmatic imbibition, (2) revascularization, and (3) maturation. During plasmatic imbibition, oxygen and nutrients diffuse through the plasma between the graft and the wound bed and nourish it in the early days before the graft revascularizes. This passive absorption of plasma in the wound bed causes edema, which is resolved when revascularization is achieved. Revascularization is essential for the long-term survival of skin grafts. This process starts within 24-48 h after grafting, and this neovascularization is characterized by the growth of new vessels in the graft from the receiving area.
Complete maturation of skin grafts is achieved in at least 1 year, and this process may continue for several years in burn victims. Skin scars may continue to improve over several years; hence, a prolonged conservative treatment is usually considered. The remodeling phase of wound healing is the longest and may last from months to several years6.
The quality of the wound bed is extremely important for the successful integration of skin grafts; moreover, functional and aesthetic reconstruction of the skin may depend on the quality of the wound bed. The expected degree of wound contraction is inversely proportional to the amount of dermis in the skin graft. Full skin grafts that include the whole epidermis and dermis, as used in our patient, maximally restrict the contractile forces and produce excellent cosmetic results. The main complications associated with skin grafting are hematoma and seroma formation, infection, failure of integration, and contraction of the wound6.
Historically, the face is considered difficult to treat in the immediate post-burn period7 due to several factors: the difficulty in assessing the depth, the value of each millimeter preserved and because some initial results with early excision and even grafting on thin skin were disappointing8. The complications of facial burns may be infections, cicatricial retractions, and impairment of the features of the face, such as the eyelids, nose, and lips9.
Contractures of the cervical region cause considerable problems, including the restriction of a vast range of movements and aesthetic impairments10. In contrast, the aesthetic procedures performed on the breast are usually classified as breast augmentation, reduction mammoplasty, and mastopexy. The main aim is to improve the shape, symmetry, and the volume of the breasts. Breast surgery is performed to preserve the blood supply to the adenopapillary complex11. Many techniques and refinements have been made in recent decades, with different types of treatment goals and degree of ptosis, hypomastia, and hypertrophy, increasing the popularity of this procedure during that period12-14.
In this report, we describe the results of facial reconstruction with an autologous full-thickness breast-face skin graft after mastopexy with implants, wherein satisfactory aesthetic results were obtained.
CONCLUSION
In this study, the use of a full-thickness graft from an atypical location was described. A full-thickness skin graft from the breast was derived simultaneously with surgical grafting performed on the face. Female patients with sequelae of burns on the face and with a history of mammary ptosis may benefit from an autologous breast-face skin graft after the completion of mastopexy with implants.
COLLABORATIONS
|
GHP |
Analysis and/or data interpretation, conception and design study, data curation, final manuscript approval, methodology, project administration, supervision, visualization, writing - original draft preparation, writing - review & editing. |
|
CTRP |
Analysis and/or data interpretation, conception and design study, data curation, methodology, visualization, writing - original draft preparation, writing - review & editing. |
|
FSMCF |
Data curation, visualization, writing - original draft preparation. |
|
MRLP |
Analysis and/or data interpretation, visualization, writing - original draft preparation. |
|
CABP |
Contribution: Analysis and/or data interpretation, Visualization, Writing - Original Draft Preparation. |
|
LAVG |
Analysis and/or data interpretation, Visualization, Writing - Original Draft Preparation, Writing - Review & Editing. |
REFERENCES
1. Oliveira KC, Penha CM, Macedo JM. Perfil epidemiológico de crianças vítimas de queimaduras. Arq Med ABC. 2007;32(2):55-8.
2. Costa DM, Abrantes MM, Lamounier JA, Lemos ATO. Estudo descritivo de queimaduras em crianças e adolescentes. J Pediatr (Rio J). 1999;75(3):181-6.
3. Vana LPM, Fontana C, Ferreira MC. Algoritmo de tratamento cirúrgico do paciente com sequela de queimadura. Rev Bras Queimaduras. 2010;9(2):45-9.
4. Gimeniz-Paschoal SR, Nascimento EM, Pereira DM, Carvalho FF. Ação educativa sobre queimaduras infantis para familiares de crianças hospitalizadas. Rev Paul Pediatr. 2007;25(4):331-6. DOI: https://doi.org/10.1590/S0103-05822007000400006
5. Nery ALV, Porter KE, Freire RF, Baptista NS, Esberard F, Souza THS, et al. Nova abordagem no tratamento de lesões complexas: uso de matriz de regeneração dérmica. Rev Bras Queimaduras. 2011;10(2):66-70.
6. Neligan PC. Cirurgia plástica: princípios. Rio de Janeiro: Elsevier; 2015.
7. Kung TA, Gosain AK. Pediatric facial burns. J Craniofac Surg. 2008;19(4):951-9. DOI: https://doi.org/10.1097/SCS.0b013e318175f42f
8. Abdelnour R, Chassagne JF, Brice M, Rahme J. Early excision and grafting in facial burns. Rev Stomatol Chir Maxillofac. 1986;87(2):97-101.
9. Lima Junior EM, Novaes FN, Piccolo NS, Serra MCVF. Tratado de queimaduras no paciente agudo. São Paulo: Atheneu; 2008. 646 p.
10. Lin JY, Tsai FC, Yang JY, Chuang SS. Double free flaps for reconstruction of postburn anterior cervical contractures--use of perforator flaps from the lateral circumflex femoral system. Burns. 2003;29(6):622-5. DOI: https://doi.org/10.1016/S0305-4179(03)00132-3
11. Schwartzman E. Die technik der mammaplastick. Chirurgie. 1930;2:932-43.
12. Lejour M. Vertical mammaplasty and liposuction of the breast. Plast Reconstr Surg. 1994;94(1):100-14.
13. Pitanguy I. Hipertrofias mamárias: estudo crítico da técnica pessoal. Rev Bras Cir. 1966;56:263.
14. Baroud R, Lewis JR. The augmentation reduction mammaplasty. Clin Plast Surg. 1976;3(2):301-8.
1. Serviço de Cirurgia Plástica Prof. Ronaldo
Pontes, Hospital Niterói Dor, Niterói, RJ, Brazil.
Corresponding author: Gisela Hobson Pontes, Avenida Epitácio Pessoa, 846, Ipanema, Rio de Janeiro, RJ, Brazil., Zip Code: 22410-090. E-mail: giselapontes@uol.com.br
Article received: September 10, 2018.
Article accepted: October 04, 2018.
Conflicts of interest: none.








 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter