

Case Reports - Year 2002 - Volume 17 -
Serious Microstomia Resulting from Burn by Caustic Soda: Case Report
Microstomia Grave Decorrente de Queimadura por Soda Cáustica: Relato de Caso
ABSTRACT
This study reports the case of a patient with serious microstomia resulting from burn by eaustie soda. It describes a technique for oral commissuroplasty used to treat this important tissue deformity. It also includes a literature review of the topie.
Keywords: Labial commissure; burn; commissuroplasty
RESUMO
É relatado o caso de um paciente com microstomia grave decorrente de queimadura por soda cáustica, sendo descrita a técnica de comissuroplastia oral utilizada para o tratamento desta importante deformidade tecidual. É feita também uma revisão bibliográfica sobre o assunto.
Palavras-chave: Comissura labial; queimaduras; comissuroplastias
The lesions that affect labial commissures may result from microstomia (reduced size of the mouth), regarded as a serious problem that causes significant cosmetic and functional losses (feeding, speech and oral hygiene). These deformities usually require surgical treatment and multidisciplinary follow-up (dental and speech). They generally affect children at pre-school and school ages(1).
They are rarely caused by congenital factors. However, when this occurs, the main factors are recessive epidermolysis bullosa dystrophica(2), sclerodermia(3), Freeman/Sheldon Syndrome(4,5) and mandibular agenesia(6). They usually result from acquired causes, especially from electrical, thermal and chemical burns (caustic soda, for example)(7), trauma (animal bites), surgical resection of tumors, and after labial reconstruction (for example, following the Estlander technique)(8) .
In addition to the existing microstomia, the formation of a hypertrophic scar with contracture may lead to ectropion of the lower lip which, combined with functional hypotonicity of the orbicular muscle, causes major impairments to speech, mastication, oral hygiene and tendency to sialorrhea(7,9,10).
OBJECTIVE
The objective of this study is to report the case of a 36 year-old patient, who had serious microstomia for 34 years as the result of an accidental burn by caustic soda, focusing particularly on the reconstruction of the oral commissures using the Kazanjian technique(10). It also aims to report other techniques that may be used in the treatment of this deformity.
CASEREPORT
O.F.S., a 36 year-old man, mulatto, single, illiterate, rural inhabitant and gas station worker, born and living in the interior of the state of São Paulo, reported that when he was two years old his mouth and lips were burnt due to accidental contact with caustic soda. It evolved, reducing the size and opening of his mouth, causing difficulties in eating and in oral hygiene. He denied sialorrhea. He denied having ingested the caustic soda and does not remember how long he was in contact with the substance. He did not receive any kind of medical care. He denied any other clinical history, having used or been allergic to medication or any previous surgeries. He reported having had toothache, which was treated with painkillers, without any type of specific dental care.
At the physical exam he weighed 52 kg (114 pounds), was 1.60 m tall (5.2 ft), and spoke with a nasal voice, which was difficult to understand; no changes were verified in the general and physical exam.
The examination of the oral region and buccal cavity revealed scars around both oral commissures, with bilateral perioral fibrosis and poor facial expression (smile, for example), absence of vermilion in the lateral regions and around the commissures, with regular vermilion in the central region. He was diagnosed with serious microstomia, with only a 2 cm mouth opening (Figs. 2a-b). The poor examination of the oral cavity, limited by the minimal mouth opening, revealed normal mobility of the tongue, with bad positioning of the teeth and poor dental hygiene. Laboratory and complementary tests were normal. The patient was referred to surgery; with local anesthesia and sedation.
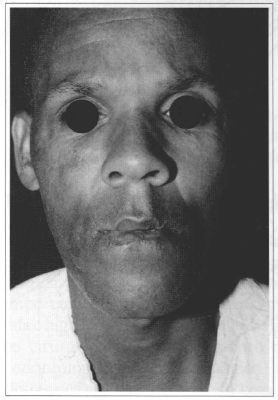
Fig.2a - Preoperative period. In a resting position it is not possible to realize how seriousthe microstomia is.
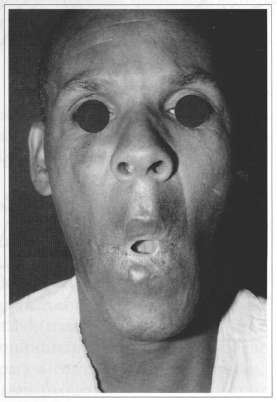
Fig. 2b - Preoperative period. Serious microstomia resulting from burn by caustic soda.
The reconstruction of the oral commissures was performed using the Converse technigue (1959), also known as Kazanjian (Fig. 1). Commissures were repositioned, based on the interpupillary distance, measured through a vertical line at the level of the pupils (Fig. 3). A triangular-shaped area (Fig. 4) was obtained after drawing two straight lines with methylene blue, one towards the upper lip and another one towards the lower lip, ending on the lateral regions of the existing vermilions.
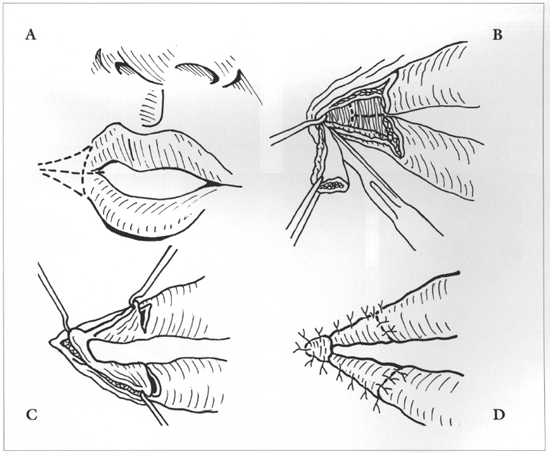
Fig. 1 - Converse-Kazanjian Technique, 1959. a) Marking skin incisions. b) Excision of skin and subcutaneous layers exposing the oral mucosa, with incisions marked on the mucosa. c) After the incision, lifting of the three mucous flaps. d)Mucous flaps sutured on the skin border. Note the mucous flap on the mouth angle.
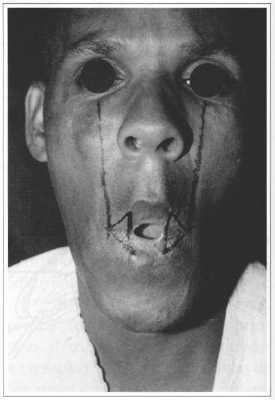
Fig. 3 - Marking the position of the neocommissures, based on normal interpupillary distance.
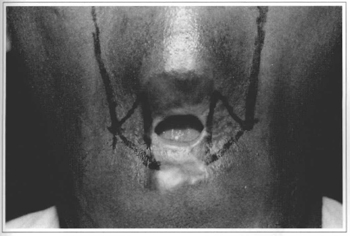
Fig. 4 - Scarring and subcutaneous tissues, with part of the orbicular muscle to be resected, on the area limited by the triangle.
Cutaneous and subcutaneous scarring tissue and part of the orbicular muscle (Fig. 5) were removed from the area inunediately adjacent to the vermilion marked with methylene blue. The incisions to be performed in the oral mucosa were marked with methylene blue, distributed in the following manner (Fig. 6):
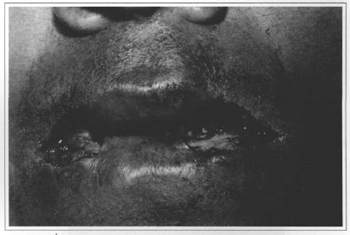
Fig. 5 - Resulting bilateral bleeding area after the removal of the scar tissue.
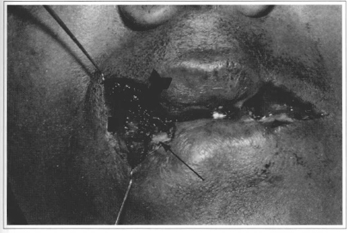
Fig. 6 - Marking the mucous flaps on the right. Note the lateral (small thick arrow) , inferior (thin arrow) and superior (big thick arrow) flaps.
a) One horizontal incision in the oral mucosa until 1 cm from the lateral end of the skin incision;
b) a curved incision at this point, forming three mucous flaps: one lateral, one superior and one inferior;
c) flaps were advanced and sutured to the cutaneous borders, with 5/0 silk, tension-free Gillies sutures (Figs. 7-9).
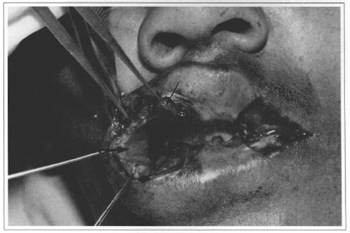
Fig. 7 - Making the mucous flaps: lateral (big thin arrow); inferior (thick arrow) and superior (small thin arrow) flaps.
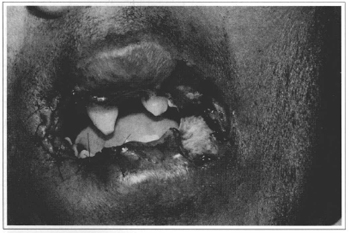
Fig. 8 - Mucous flaps sutured to the skin forming the right oral neocommissure and marking the mucous flaps for the reconstruction of the left oral commissure.
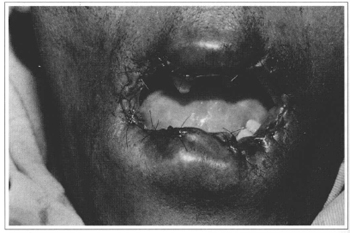
Fig. 9 - Final suture, showing the reconstruction of oral commissures.
There were no complications during or after surgery, and the patient was discharged on the first postoperative day. He was instructed to stay on a liquid diet for the first 15 post-operative days, with dental care follow-up, which impraved his oral hygiene significantly. Sutures were removed on the 10th post-operative day. After that period, the patient received speech therapy, which considerably impraved his speech and mouth occlusion and opening movements. Three months after the surgery, the patient presented significant impravement, both aesthetically and functionally (eating and speech), with a 5.5 cm horizontal mouth opening, and a 3.5 cm vertical mouth opening (Figs. 10 and 11).
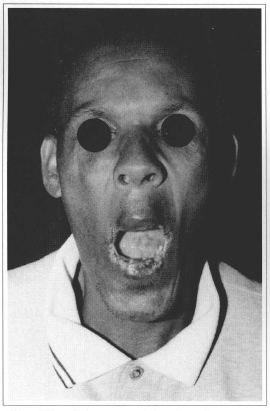
Fig. 10 - Three month post-operative period. Note the marked improvement in mouth opening.
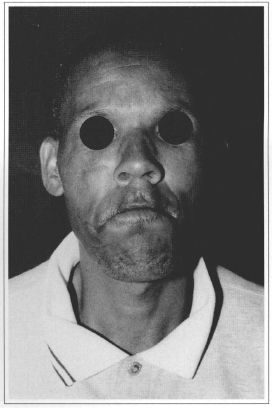
Fig. 11 - Three month post-operative period. Note the good oral occlusion and good functioning of the orbicular muscle.
DISCUSSION
Microstomias usually affect children and adolescents. The many existing degrees of deformity result from hypertrophic scarring processes and perioral scarring contractures, which commonly occur after burns(11).
Microstomias may range from light to serious, cause aesthetic impairment and, most importantly, functional losses, such as difficulties in speech, facial expression (oral opening, smile), feeding and oral hygiene, in addition to serious psychological problems(11).
Many surgical procedures have been described for the reconstruction of labial commissures. In 1831, Dieffenbach advanced superior, inferior and lateral mucosa flaps, after triangular resection of the scar(12).
In 1954, Kazanjian and Roopenian described two methods, the choice of which depended on the amount of remaining untouched vermilion (buccal mucosa and vermilion flaps)(13).
In 1959, Conserve modified the Dieffenbach technique (known as the Kazanjian technique, better understood as Converse-Kazanjian)(10,13).
In 1972, Fairbanks and Dingman divided the vermilion obliquely in minute flaps(14) and, in 1979, Brusati used a u-shaped cheek flap to reconstruct the vermilion of the commissure(15). Su, in 1980(16), Jackson, in 1985(3), and Berlet et al., in 1993(12), described several vermilion and mucosa buccal flaps, so as to reduce the level of postoperative relapses, which, according to Canady and Bardach(17), are more usual with vermilion sliding flaps.
Most authors prefer to start with a more conservative approach, such as the use of oral splints(18), perioral physical therapy(7,10) or even minor interventions such as z-plasty, skin grafts and commissurotomies(7), with the aim of avoiding further deformities (some authors prefer to recur to these procedures six months after the lesion, when the scar is already mature, and the real aesthetic and functional deficits may be better assessed) (17). Unfortunately, many patients do not receive these previous treatments, and require more complex surgical treatment, also indicated in serious cases or in those that are refractory to an initial treatment(11).
Both moderate and serious cases usually require several surgical stages, preferably local flaps, usually compound (cutaneous-muscular-mucous )(8,ll), as already mentioned before, and less frequently, regional and distant flaps, such as, for example, nasolabial(13), lingual(19), deltopectoral fasciocutaneous(10), and temporal muscle(20) flaps due to poor aesthetic results and to a greater number of complications.
In this case, we used the Kazanjian technique, described in 1959 (initially described by Dieffenbach and modified by Converse) (10,13), as it was easily performed, could be done with local anesthesia, and had a history of good aesthetic and functional results in our facility.
We realized that, similarly to Converse's initial descriptions, lateral flaps prevent postoperative contractures, improving functional recovery with lower risk for relapse, a condition which, when presem, increases the complexity of new surgery and, in that manner, increases the likelihood of an unfavorable outcome.
This technique was also chosen due to the fact that the speech therapy team was able to provide better follow up on patients in the post-operative period, which permitted quicker and better recovery of facial expression movements.
It should be stressed that the reconstruction of commissures is complex, and may result in bulging, postcontracture relapses, irregularities on the cutaneousmucosa line, functional deficit (poor muscular reconstruction), sialorrhea and angular cheilitis(6), fortunately not found in this patient.
We had already had both slight and serious complications in previous cases operated on, using the Kazanjian technique, mainly due to the misuse of the method by our surgical team. However, as we operated on new cases and improved our surgical skills, we realized that a key factor in the occurrence of post surgical relapses was the size and thickness of the lateral mucous flap, which should not, in any way, be tense when sutured on the cutaneous borders.
Most of the surgical procedures used to treat microstomias are appropriate and yield good results; however, they fall far short of providing a fully satisfactory commissure, both aesthetically and functionally(8).
In that manner, each case should be carefully assessed, diagnosed and studied, so as to attain the best outcome possible, and to give patients back an acceptable appearance and, above all, improve their functioning, particularly speech and feeding.
CONCLUSION
The lesions that destroy labial commissures cause both aesthetic and functional deficits, and frequently result in microstomia, a deformity that is often disabling to patients.
Surgical treatment, in one or more phases, aims to improve the lost functions and to attain the best possible aesthetic outcome. We considered the main techniques used for the reconstruction of labial commissures, focusing particularly on the Converse technique (also known as Kazanjian), as it is easily performed and yields good results.
Surgical planning should be strictly followed and the plastic surgeon should minimize the deformity, thus restoring the patient's normal relationship with society. It is also crucial to provide good guidance, education and preventive measures, so as to reduce the number of factors that may cause deformities in the oral commissures.
REFERENCES
1. Pitanguy I, et al. Considerações sobre queimaduras elétricas do lábio. Rev Bras Cir. 1986; 76 (4): 231- 42.
2. Travis SP et al. Oral and gastrointestinal manifestations of epidermolysis bullosa. Lancet. 1992; 340(8834-5): 1505-6.
3. Martins WD. Queiloplastia para correção de microstomia secundária por queimaduras química. Dens. 1987;3(1):5-7.
4. Millner MM, Mutz ID, Rosenkrang W. Whistling face syndrome - a case report and literature review. Acta Paediatr Hung. 1991;31(3):279-89.Review.
5. Ferreira LM, Minami E, Andrews JM. Freeman-Sheldon Syndrome: Surgical correction of microstomia. Br J Plast Surg. 1994;47(3):201-2.
6. Diaz JH, Guarisco JL, Lejeune FE JR. Perioperative management of pediatric microstomia. Can J Anaesth. 1991;38(2):217-21.
7. Mehra p, Caiazzo A, Bestgen S. Bilateral oral commissurotomy using buccal mucosa flaps for management of microstomia: report of a case. J Oral Maxillofac Surg. 1998;56:1200-3.
8. Ono I, Ariga K, Gunji H, et al. A method with three triangular flaps as a secondary operative procedure after a reconstruction of the lower lip by Estlander's method. Plast Reconstr Surg. 1992;90(4):700-6.
9. Pitanguy I, et al. Queimaduras elétricas do lábio. Rev Bras Cir. 1979;69(516): 181-93.
10. Kazanjian VH, Roopenian A. The treatment of lip deformities resulting from electric burns. Am J Surg. 1954;88:884.
11. Johns FR, Sandler NA, Ochs MW. The use of a triangular pedicle flap for oral commissuroplasry: report of a case. J Oral Maxillofac Surg. 1998;56:228-31.
12. Berlet AC, Ablaza VI, Servidio P. A refined technique for oral commissurotomy: J Oral Maxillofac Surg. 1993;51(12):1400-3.
13. Converse JM. Techniques for the repair of defects of the lips and cheeks. In: Converse JM, editor. Reconstructive plastic surgery: 2. ed. Philadelphia: WB Saunders; 1977. Vol. 3, p.1544-94.
14. Fairbanks GR, Dingman RO. Restoration of the oral commissure. Plast Reconstr Surg. 1972;49(4):411-3.
15. Brusati R. Reconstruction of the labial comissure by a sliding U-shaped cheek fiap.J Maxillofac Surg. 1979;7:11-4.
16. Su CT, Manson PN, Hoopes JE. Electrical burns of the oral comissure: treatment results and principles of reconstruction. Ann Plast Surg. 1980; 5(4):251-9.
17. Canady JW, Thompson SA, Bardach J. Oral commissure burns in chindren. Plast Reconstr Surg. 1996;97( 4) :738-45.
18. Khan Z, Banis JC Jr. Oral commissure expansion prasthesis. J Prasthet Dent. 1992;67(3):383-5.
19. Donelan MB. Reconstruction of electrical burns ofthe oral commissure with a ventral tongue flap.Plast Reconstr Surg. 1995;97(7):1155-63.
20. La Trenta GS, Grant RI, Haworth RD, et al. Punetional reconstruction for severe postburn microstomia. Ann Plast Surg. 1992;29(2):178-81.
I - Senior Member of the Brazilian Society of Plastic Surgery. Full Member of the Brazilian College of Surgeons. Member of the International College of Surgeons. Plastic Surgeon at Mandaqui Hospital Complex.
Study performed at the Cosmetic and Reconstructive Plastic Surgery Facilities of Mandaqui Hospital Complex, São Paulo, Brazil
Address for correspondence:
Eduardo Mordjikian, MD
Av. Pavão, 955 Cj. 71
04516-012 - São Paulo - SP Brazil
Phone: (55 11)5044-0250 - Fax: (55 11)5535-49
e-mail: mordjik@uol.com.br


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter