

Original Article - Year 2019 - Volume 34 -
Fat grafting: Lipofragmentation X Liposuction
Enxerto de gordura: lipofragmentado X lipoaspirado
ABSTRACT
Introduction: Aiming to obtain autogenous and injectable
lipografts from resected tissues in dermolipectomies, this
study proposes a new method for harvesting and processing
adipose tissue through a specific fragmenting device. The main
objective was to establish a comparative analysis of the quality
and viability characteristics of the new lipofragmentation
technique and those of the well-known liposuction technique,
widely accepted as a viable source of fat grafting. In vivo
and in vitro assays were designed to evaluate the biological
behavior of the samples to guide new and possible human
studies with clinical applications.
Methods: A post-bariatric
patient who underwent abdominal dermolipectomy had her
surgical specimen resected, which was divided into four parts
that underwent liposuction and lipofragmentation, with and
without prior infiltration. All samples were centrifuged and
distributed for assays with assessments involving histological
analysis, immunohistochemistry, flow cytometry, cell culture,
and xenograft injection on the back of 10 Wistar rats, which
was evaluated after six weeks for mass, volume, and histological
features.
Results: The structural characteristics and biological
behaviors of fragmented, dry, and infiltrated fat samples were
similar to those of liposuction samples.
Conclusions: Fat
fragmentation transformed the subcutaneous cellular tissue of
dermolipectomies into a new, viable injectable lipograft variant,
with biological characteristics similar to those of traditional
liposuction. Although still preliminary, our results support
further investigations to optimize the technique and improve fat
grafting and its possible applications in regenerative medicine.
Keywords: Adipose tissue; Transplants; Plastic surgery; Bioprosthesis; Graft survival.
RESUMO
Introdução: Com o objetivo de obter lipoenxerto autógeno e injetável de tecido ressecado em dermolipectomias, este estudo propõe um novo método para colheita e processamento do tecido adiposo, através de um dispositivo fragmentador específico. O principal objetivo foi estabelecer uma análise comparativa das características de qualidade e viabilidade do novo lipofragmentado em relação ao já conhecido lipoaspirado, amplamente aceito como fonte viável de lipoenxerto. Ensaios in vivo e in vitro foram delineados para avaliar o comportamento biológico das amostras, a fim de orientar novos e possíveis estudos em humanos com aplicações clínicas.
Métodos: Uma paciente pós-bariátrica que foi submetida a dermolipectomia abdominal teve sua peça cirúrgica ressecada e dividida em quatro partes que foram submetidas a Lipoaspiração e Lipofragmentação, sem e com infiltração prévia. Todas as amostras foram submetidas a centrifugação e então distribuídas para os ensaios que envolveram avaliação histológica, imunohistoquímica, citometria de fluxo, cultura celular e ainda a injeção de xenoenxerto no dorso de 10 ratos Wistar, retirados após seis semanas para avaliação de massa, volume e características histológicas.
Resultados: As amostras de gordura fragmentada, seca e infiltrada, mostraram características estruturais e comportamento biológico semelhantes aos das amostras de lipoaspirado.
Conclusões: A fragmentação da gordura transformou o tecido celular subcutâneo das dermolipectomias em uma nova variante de lipoenxerto injetável e viável, com características biológicas semelhantes àquelas do lipoaspirado tradicional. Embora ainda preliminares, nossos resultados embasam a realização de novas investigações buscando otimizar a técnica com vistas ao aprimoramento da enxertia gordurosa e suas possíveis aplicações na medicina regenerativa.
Palavras-chave: Tecido adiposo; Transplantes; Cirurgia plástica; Bioprótese; Sobrevivência de enxerto
INTRODUCTION
The possibility of fat reinjection through cannula has transformed autologous fat grafting into a convenient and effective tool to restore volume and subcutaneous contouring in several clinical situations1,2. Currently, there are several technical possibilities for each step in the fat grafting process, but there is no absolute and uniform consensus that can guarantee the best efficacy and predictability in the integration of these grafts. Recently, two systematic literature reviews revealed the current stage of evidence-based fat grafting, seeking to elucidate the effects of different harvesting, processing, and reinjection methods on fat graft integration rates. Interestingly, very few variables apply to the harvesting method, including different types and sizes of cannulas, but they have always been studied in different liposuction techniques3,4.
Fat transfer has been increasingly used in the gluteus and mammary contour, but the volumetric limitation of liposuction as a method of material collection may represent a formal impediment for many patients, especially in the post-bariatric population. Large amount of weight loss promotes the emptying of subcutaneous cellular tissues, which makes liposuction less effective in these cases, either due to established tissue laxity or the small amount of remaining fat. Thus, the need to restore the best volume in localized areas often results in technical difficulty or even the impossibility to obtain sufficient fat through liposuction. Paradoxically, dermolipectomies performed for suspension and body tightening in these patients invariably produce undesirable discharge of viable fat tissue incorporated in surgical resections5.
To better obtain the autologous and injectable fat grafts from dermolipectomy surgeries, we propose a new method for harvesting and processing adipose tissue through a shredder that can convert almost all subcutaneous cell tissues into viable fat grafts6.
OBJECTIVE
The objective of this study was to establish an analytical comparison between the characteristics and biological behavior of the new “fragmented fat” and the already established “liposuction” procedures, when used as a graft. In vitro and in vivo observations were designed to establish and evaluate parameters that objectively prove the viability of the fragmented fat graft and support future studies and clinical applications in humans.
METHODS
The scientific design of this project was properly protocoled and approved by the ethics committees of the Botucatu School of Medicine - Paulista State University (UNESP) for human (CAAE 73646217.7.0000.5411) and animal research (CEUA 1240/2017) between September 2017 and March 2018.
An adult female patient, with significant weight loss after bariatric surgery, underwent an anterior abdominal anchor dermolipectomy. The infra-umbilical region of her surgical specimen used and medially divided into two parts. The left half received subcutaneous infiltration of 400 mL Klein needle saline solution (t = tumescent), while the right half was kept dry without any infiltration (d = dry). Each half was then vertically divided into two parts, resulting in four different pieces that were subjected to the two different graft harvesting techniques (Figure 1a). Both lateral portions received liposuction by syringe with 2-mm cannula (liposuction: dry and tumescent [LAd and LAt, respectively]), while the two central portions had their skin resected by scalpel and the fatty tissue divided into smaller pieces that were then subjected to the new method of fragmentation (lipofragmentation: dry and tumescent [FFd and FFt, respectively]).
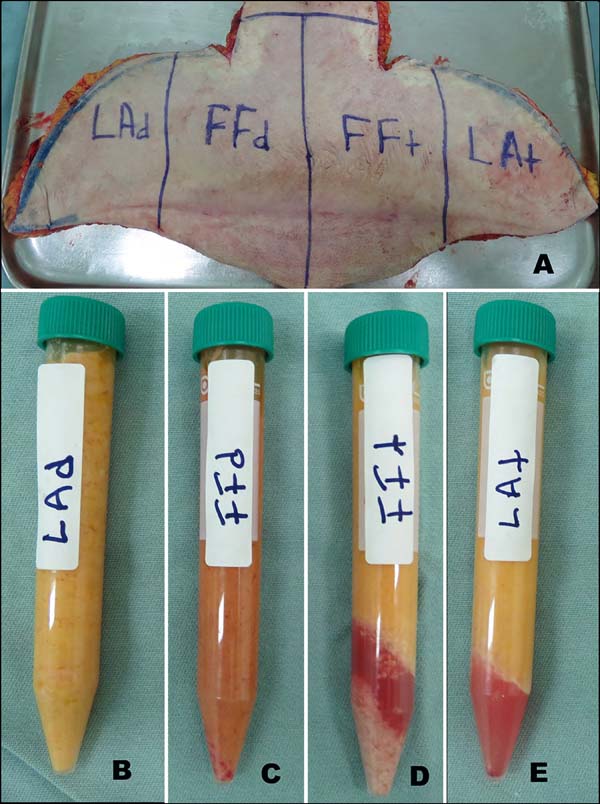
All the four samples obtained at the end were centrifuged (1,200 rpm for 3 minutes) and distributed for in vivo and in vitro assays (Figures 1b, c, d, e). Each of the four adipose tissue samples (FFd, FFt, Lad, and LAt) was grouped and labeled as a different color (blue, red, green, and black, respectively) to preserve blind manipulation during the subsequent experimental phases until the results were finally ready for recording and interpretation.
Fat Fragmentation
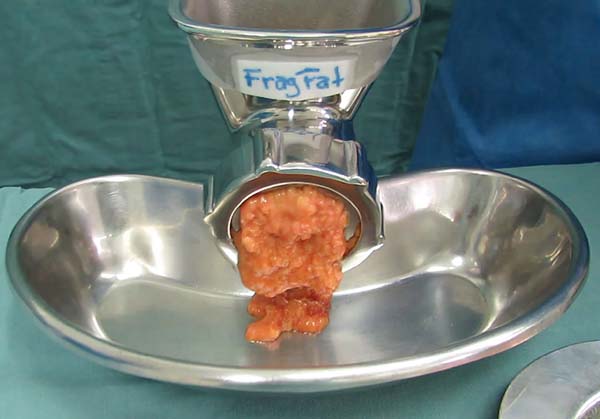
The proposed shredder is a hand-held apparatus (Figure 2), made of stainless steel (autoclavable) and designed to receive proximal portion pieces of fatty tissue in a cylindrical chamber (Figure 2a), which are gradually carried by a central helical structure (Figure 2b) towards a distal cutting device consisting of a star-shaped rotational blade (Figure 2c) and a stationary multi-perforated plate (Figure 2d). Finally, a threaded ring holds the structures in place (Figure 2e). Using the crank handle, as the (skinless) pieces of fat are pushed forward by the auger toward the distal cutting device, the tissue projects through plate holes and is immediately and continuously sectioned into small fragments by the rotational blade. The degree of fragmentation is determined by the hole diameter in the multi-perforated plate, providing ideal consistency for lipoinjection according to different cannula sizes and their internal diameters. In this experiment, we used a distal plate with 2-mm holes to obtain lipograft under conditions similar to liposuction that was collected through a 2-mm diameter cannula (Figure 3).
In Vitro Study
All samples of fragmented fat (lipofragmentation) and liposuction were subjected to routine histology including immunohistochemistry, viable cell count, flow cytometry, and stromal vascular fraction cell culture. Samples in the in vitro study were made available through 1 ml syringes through a 2 mm cannula, in exactly the same way as in the in vivo protocol.
Histological Assessment Each sample (3 g fat) was immediately fixed in 10% buffered formaldehyde, concentrated by gravity filtration on porous paper, processed in different grades of alcohol and xylol, embedded in paraffin, cut to 5 microns thick and subjected to H&E staining. Immunohistochemical characterization was obtained by using the primary stromal progenitor marker CD34. The histological slides were observed and compared by an experienced pathologist seeking to analyze possible architectural tissue distortion, adipocyte degeneration and immunohistochemical pattern.
Biological Assessment The protocol used for enzymatic dissociation was as detailed in previous publications7,8. Each of the 4 samples collected (10 g) was added to 30 mL of filtered Collagenase solution (GibcoTM) using the following ingredient ratio: 3 mg of Collagenase type 2 per gram of tissue and 1 mL of Hank’s balanced saline (GibcoTM) per mg Collagenase + 3.5% bovine serum albumin (Sigma Aldrich™). The 50 mL tubes, filled with 10 g of tissue and 30 mL of filtered Collagenase solution, were submerged in a 37 °C water bath for 30 min under constant agitation until the solution became homogeneous. The samples were subjected to double-layer gauze filtration and re-centrifuged at 120 rpm for 10 minutes, the digested fat fractions remained in the supernatant while the stromal pellet condensed at the bottom. The viability of the suspended cells was evaluated by the Trypan Blue9,10 (Sigma Aldrich™) technique. The culture of enzymatically dissociated cells and phenotyped by flow cytometry aimed to evaluate the prevalence of possible and distinct progenitor populations, comparing their biological behavior among groups11.
In this study, 104 cells/mL were seeded in 6-well plates containing DMEM F12 culture medium (Gibco™) supplemented with streptomycin, penicillin, amphotericin B (Gibco™), and 20% fetal bovine serum. Cells were monitored daily by inverted phase contrast microscope (Axiovert A1 - Carl Zeiss™).
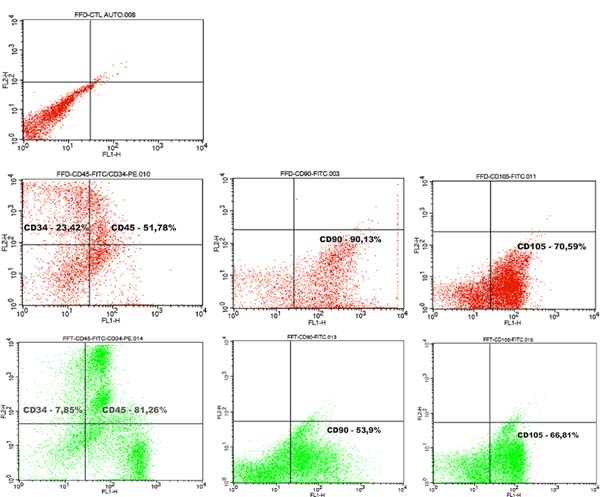
According to a joint definition of the International Federation for Adipose Therapeutics and Science (IFATS) and the International Society for Cellular Therapy (ISCT)12, characterization of mesenchymal stem cells by flow cytometry requires a minimal phenotypic expression pattern that provides positivity for some markers (we used CD90 and CD105) and negativity for others (we use dCD34 and CD45)12. In this study, the evaluation of surface molecular expression was performed using FACScalibur BD equipment and Cell Quest Pro software using anti-human FITC CD45 (368507 Biolegend), anti-human PE CD34 (343505 Biolegend), FITC anti-human CD90 (Thy 1) (328107 Biolegend), and FITC anti-human CD105 (323203 Biolegend), with their respective control isotopes.
In Vivo study
In order to compare the integration of lipograft from liposuction and lipofragmentation in both dry and infiltrated groups, the different samples obtained were labeled with different colors (blue, red, green, and black) and distributed in 1 mL syringes, which were immediately taken from the operating room to the experimental laboratory, where they were injected into the dorsal subcutaneous tissue of 10 Wistar rats under anesthesia and sterile conditions. Two small punctures were positioned in the rats’ dorsal midline and using 2 mm diameter cannulas 1 mL of each sample (FFd, LAd, FFt, and LAt) were re-injected subcutaneously, grafting them equally on each of the quadrants in a clockwise rotation protocol of sample placement for each new animal. The rats were marked by numbers (ear method) and each injected graft sample was properly recorded by its color and location. The animals were kept under standard environmental conditions and daily received ventral subcutaneous injections of cyclosporine (2 mg/kg) to reduce the immune response against xenograft13. After 6 weeks, all rats were sacrificed and the remaining fat from the grafts was surgically removed for a comparative evaluation of mass and volume, as well as routine histological preparation for H&E and Masson’s trichrome stained slides. Each slide had areas randomly chosen for blind histological evaluation, seeking to classify the presence of intact fat cells, cysts and vacuoles, inflammation (lymphocyte and macrophage infiltration), fibrosis, and neovascularization (capillary density). The presence of each of these variables were graded on a scale from 0 to 5, where: 0, absent; 1, Minimum; 2, Minimum to moderate; 3, Moderate; 4, Moderate to extensive; 5, Extended14.
RESULTS
The fragmentation process was effective in transforming the pieces of dermolipectomy fat tissue into an injectable fat grafting texture (Figure 3). All samples of fat material obtained by liposuction and lipofragmentation were subjected to centrifugation resulting equally in a discreet superior oily layer. Both samples from the infiltrated group (LAt and FFt) formed a liquid layer after centrifugation, which as well as the oily layer were removed from the material to be studied, as described by Coleman15,16. The infiltrated fragmented fat presented an inferior visible and sedimented layer (pellet) that was not observed in the infiltrated liposuction and was not included in the study material. The dry group material, liposuction and lipofragmentation, had no liquid layer or lower pellet (Figures 1b, c, d, e).
Histological Assessment and Immuno-histochemistry
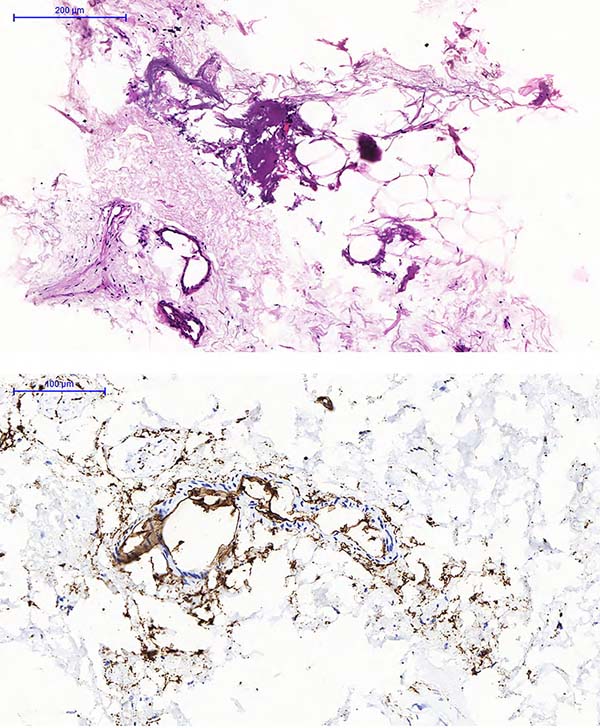
A blind analysis of both dry and infiltrated groups of both liposuction and lipofragmentation material showed similar histological structural characteristics regardin g tissue architecture and cellular integrity. Immunohistochemistry showed large number of CD34 labeled cells widely distributed between both liposuction and lipofragmentation tissues. The histology of the sedimented material obtained after centrifugation of the infiltrated lipofragmentation (pellet) revealed adipocytes amid a large amount of vascular and stromal matrix, demonstrating high CD34 labeled cells (Figure 4).
Counting of Viable Cells and Flow Cytometry
Although there was a significant difference in the number of nucleated cells among samples, their viability did not vary significantly (Table 1). Trypan Blue test analysis showed no statistically significant difference in cell viability between liposuction and lipofragmentation samples in both the dry and infiltrated groups. Immunophenotyping of samples by flow cytometry showed that in both the dry and infiltrated groups, liposuction and lipofragmentation also showed similar behavior with the markers used in the study (Figures 5 and 6). The cells’ analytical distribution by each marker in the different preparations showed no statistically significant difference (Table 1).
| Mean of Fluorescence Intensity (%) | |||||||
|---|---|---|---|---|---|---|---|
| Ctle Auto | Ctke ISO | CD45-FITC | CD34-PE | CD90-FITC | CD105-FITC | ∑ Number of cells analyzed | |
| FFd | 6 | 11.91 | 52.98 | 51.81 | 92.22 | 69.09 | 11.095 |
| FFt | 5.07 | 6.64 | 84.12 | 57.67 | 55.98 | 65.42 | 20.000 |
| LAd | 2.61 | 3.4 | 61.39 | 63.78 | 51.52 | 37.23 | 20.000 |
| LAt | 6.09 | 4.21 | 56.14 | 78.33 | 70.67 | 68.68 | 20.000 |
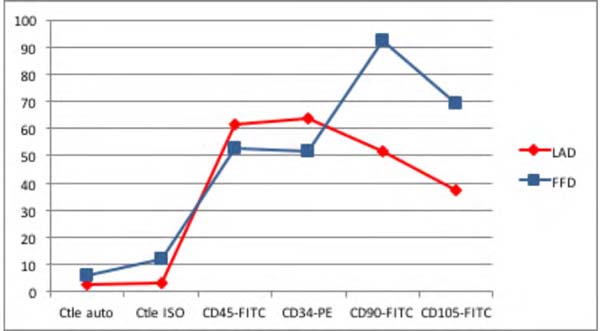
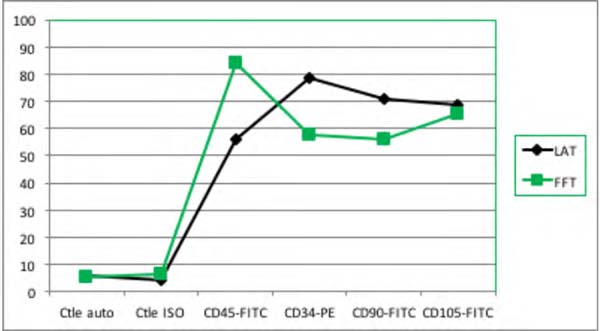
Among Dry group samples, the lipofragmentation technique showed the best performance for markers CD90 and CD105, obtaining a higher quantification of mesenchymal stem cells. On the other hand, in the infiltrated group, the lipofragmentation showed better performance for CD45 markers, while liposuction was better for CD34. Figure 7 shows the representation of immuno-phenotypic analysis for AD-MSC surface markers in the different samples.
Fat-derived Stem Cell Culture
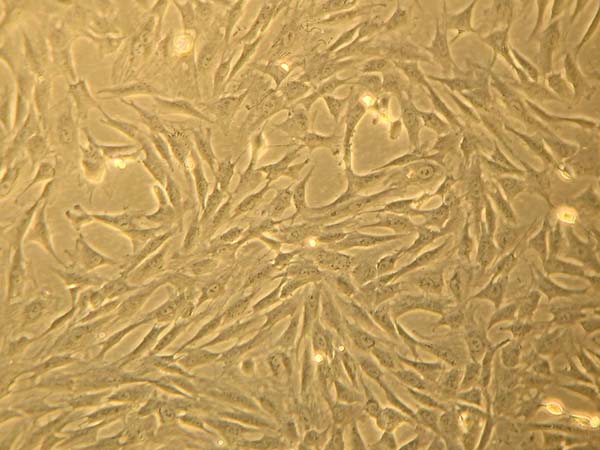
Liposuction and lipofragmentation samples in both the dry and infiltrated groups showed similar parameters in cell culture, with standard regular expansion. The adhesion rate at 72 hours was 25% for FFd samples, which differed significantly from the other samples that reached 10%. Likewise, 100% cell confluence also occurred earlier in the FFd sample. Furthermore, the final appearance of fibroblastic populations did not differ between studied samples (Figure 8).
Lipograft Integration - Mass and Volume Analysis
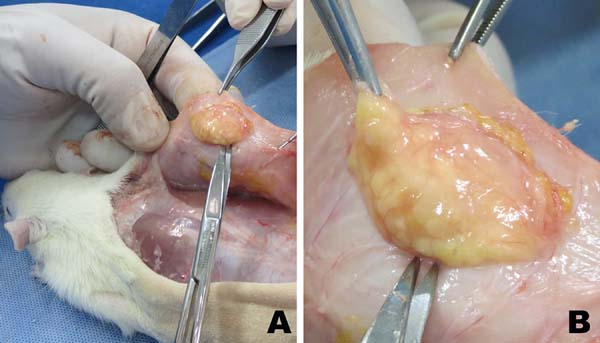
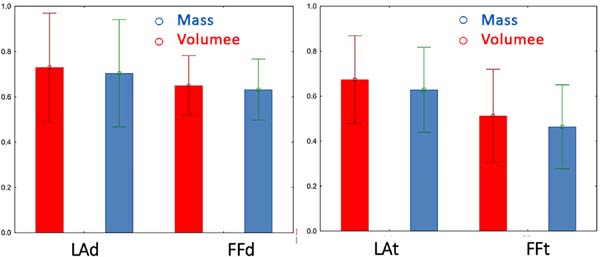
Six weeks after fat grafting, all the 10 rats were sacrificed and had their remaining grafts in the dorsal regions surgically removed (Figure 9). Student’s t-tests for independent samples were used for analysis of mass and volume of obtained pieces, to compare the retention and behavior of lipofragmentation and liposuction in both dry (FFd X LAd) and infiltrated (FFt X LAt) groups. The mean and standard deviation (SAS® for Windows v. 9.3) were calculated with the production of graphic illustration (Statistica® for Windows v. 10) with a significance level set at 5% (p <0.05).
DRY: Lipofragmentation X Liposuction In the group where the fat was harvested and processed without previous infiltration, the mean retained volume of lipofragmentation was 0.65 ± 0.13, while that in the liposuction group was 0.73 ± 0.24 (p=0.37). In contrast, the mean retained mass after lipofragmentation was 0.63 ± 0.13, while that after liposuction was 0.70 ± 0.24 (p=0.41). Hence, there were no statistically significant differences in the final mass and volume of grafts by dry lipofragmented and liposuction grafts (Figure 10).
INFILTRATE: Lipofragmentation X Liposuction The mean volume retained in grafts of the harvested group after infiltration of the pieces after lipofragmentation was 0.51 + 0.21, while that after liposuction was 0.67 + 0.20 (p=0.09). The mean retained mass after lipofragmentation was 0.46 + 0.19, while that after liposuction was 0.63 + 0.19 (p=0.06). There was no statistically significant difference in the final mass and volume retention rates of lipografts obtained by infiltrate lipofragmentation and liposuction (Figure 10).
Lipograft Integration - Histological Analysis
A widescreen digital scanner equipment (3DHistech®) and Pannoramic Viewer for Windows v. 1.15 software were used to handle slides and to aid in grading histological variables on H&E staining, except for fibrosis that was accessed by Masson’s trichrome staining. Data statistical treatment obtained by microscopic assessment of grafts retained in the dry group (FFd and LAd) showed no difference in relation to fibrosis inflammation and neovascularization. However, dry liposuction showed a higher degree of cellular integrity and lower degree of cysts and vacuoles when compared to dry lipofragmentation. In the infiltrated group (FFt and LAt), there was no difference in cell integrity, inflammation and neovascularization, but lipofragmentation had fewer cysts or vacuoles and higher fibrosis compared to liposuction. The results were shown as mean and standard deviation (Student’s t-test), and p < 0.05 was considered for statistical significance (Table 2).
| Lipofragmentation Dry | Liposuction Dry | p | |||
| Mean | Standard Deviation | Mean | Standard Deviation | ||
| Cellular Integrity | 1.8 | 0.63 | 3.0 | 0.94 | 0.0036 |
| Cysts/Vacuoles | 3.4 | 1.26 | 2.3 | 0.82 | 0.0333 |
| Inflammation | 2.7 | 0.67 | 2.3 | 0.82 | 0.2502 |
| Fibrosis | 2.1 | 0.74 | 1.9 | 0.74 | 0.5520 |
| Neovascularization | 2.1 | 0.88 | 2.2 | 1.03 | 0.8180 |
| Lipofragmentation Infiltrate | Liposuction Infiltrate | p | |||
| Mean | Standard Deviation | Mean | Standard Deviation | ||
| Cellular Integrity | 2.3 | 1.16 | 3.4 | 1.26 | 0.0577 |
| Cysts/Vacuoles | 3.2 | 0.79 | 1.8 | 0.79 | 0.0009 |
| Inflammation | 2.3 | 0.67 | 2.3 | 0.95 | 1.000 |
| Fibrosis | 1.9 | 1.2 | 3.1 | 0.88 | 0.0197 |
| Neovascularization | 2.0 | 0.47 | 2.4 | 0.97 | 0.2603 |
DISCUSSION
Since we are proposing a new methodology for graft harvesting and processing, the scope of this experiment was to promote a structural and biological comparison between the new “lipofragmentation” and the already recognized “liposuction” procedures. We used the same donor area from a single person to eliminate interpersonal variability in fat quality regarding its regenerative potential and subsequent fat grafting retention17. The skin resection with scalpel and the fat piece division into smaller pieces allowed the subcutaneous full thickness to be used, including fat layers and connective tissue, the latter usually not incorporated by conventional liposuction.
The shredder can use different sizes in the distal multi-perforated plate holes (we used 2 mm diameter holes) to allow injection of the collected material through different cannula sizes, according to different areas to be grafted such as face, breasts and buttocks.
Although this was not a specific target of our method, it seems quite clear that lipofragmentation requires less time and physical effort on the part of the surgeon, obtaining higher amounts of fat than traditional liposuction, especially if we consider the post-bariatric patient with sparse and hollow fat layers.
Tumescent infiltration was initially developed to improve the liposuction18 technique, but some studies have shown its potential adverse effects that may impact the better integration of fat grafts19-23. As this is a reality in liposuction, we chose to include a group of tumescent infiltration because there are reports that such infiltration could negatively or positively impact graft biology and viability3, which was not observed in the present study. We consider as an intrinsic bias of our method the fact that in the initial surgical specimen demarcation to be a source for graft harvesting, the paraumbilical (median) regions contain more perforating vessels and a denser fascia of Scarpa than the lateral areas of the abdomen. Samples from medial regions may present denser cell suspensions than lateral areas, which could in theory justify some difference in the composition and biology of extracted grafts.
Considering that we do not have the so-called nude mice in our laboratories, we used Wistar rats with daily cyclosporine application to promote desirable immunosuppression as previously described by Ferreira et al24. We recognize the athymic rat as the most appropriate model for this type of fatty xenograft research and look forward to using them in future trials. Hence, reducing the amount of fat injected as well as extending graft integration time to 12 weeks25.
The observation of our in vitro and in vivo assays has shown that lipofragmentation had structural and biological characteristics very similar to those of liposuction. Recently, evidence of lipografts’ dynamic and regenerative nature has emerged from different areas of plastic surgery as well as cellular and molecular biology, including the possibility of direct transplantation of fat-derived stem cells including their biological niche, even without their formal isolation in cultivation medium not only to increase graft retention but also as distinct sources of cell therapy26,27. Flow cytometry with a surface panel of specific markers, as well as cell viability tests helped to distinguish and confirm possible stromal vascular fraction populations present in lipofragmented material without statistical difference in relation to liposuction material, showing that the new method preserved and did not cause significant damage to these important structures.
The mechanisms involved in the fragmentation process probably incorporates more than just fatty cellular content, but also its scaffolds. Following centrifugation, the infiltrated lipofragmentation formed an evident lower pellet consisting of mature adipocytes surrounded by a rich stromal web with blood vessels and nucleated cells, including progenitor stem cells. The fact that we did not include this sedimented material in the infiltrated lipofragmentation samples could, in theory, justify its slightly lower integration after 6 weeks. Although that stromal tissue was not separated and visually identified in the dry lipofragmentation samples, it is quite reasonable to imagine that it should have been incorporated into the FFd samples, which had the best integration rates. Subsequent investigations will be crucial in determining the real potential of lipofragmentation stromal content in the graft enrichment and probable clinical applications. Future studies with this material may also explore some modern concepts of improvement of tissue healing as well as site-specific regenerative medicine by using the perivascular scaffold probably incorporated in this new form of fat grafting.
CONCLUSION
The methods used showed that the shredder device was able to transform the subcutaneous layers removed in a conventional dermolipectomy into a viable lipograft, and this new type of Fragmented lipograft behaved with similar biological characteristics to those exhibited by the traditional syringe liposuction. Although preliminary, our results may support further studies in humans to extend lipofragmentation as an alternative to fatty grafting as well as possible clinical applications for wound healing and regenerative medicine.
COLLABORATIONS
|
FHM |
Analysis and/or data interpretation, Conception and design study, Conceptualization, Data Curation, Final manuscript approval, Formal Analysis, Investigation, Methodology, Project Administration, Realization of operations and/or trials, Resources, Supervision, Validation, Visualization, Writing - Original Draft Preparation, Writing - Review & Editing |
|
FV |
Analysis and/or data interpretation, Conception and design study, Conceptualization, Final manuscript approval, Methodology, Project Administration, Supervision, Visualization, Writing - Original Draft Preparation, Writing - Review & Editing |
|
ED |
Analysis and/or data interpretation, Conception and design study, Conceptualization, Formal Analysis, Investigation, Methodology, Project Administration, Realization of operations and/or trials, Resources, Supervision, Writing - Original Draft Preparation, Writing - Review & Editing |
|
MACD |
Analysis and/or data interpretation, Conception and design study, Conceptualization, Final manuscript approval, Investigation, Methodology, Project Administration, Realization of operations and/or trials, Supervision, Writing - Original Draft Preparation |
|
MAG |
Conception and design study, Conceptualization, Data Curation, Formal Analysis, Investigation, Methodology, Realization of operations and/or trials |
|
JMG |
Data Curation, Investigation, Methodology, Realization of operations and/or trials |
|
RRR |
Data Curation, Investigation, Methodology, Realization of operations and/or trials |
|
HCN |
Data Curation, Investigation, Methodology, Realization of operations and/or trials |
REFERENCES
1. Illouz YG. The fat cell “graft”: a new technique to fill depressions. Plast Reconstr Surg. 1986;78:122-123. DOI: https://doi.org/10.1097/00006534-198607000-00028
2. Bircoll M, Novack BH. Autologous fat transplantation employing liposuction techniques. Ann Plast Surg. 1987;18:327-329. DOI: https://doi.org/10.1097/00000637-198704000-00011
3. Strong AL, Cederna PS, Rubin JP, Coleman SR, Levi B. The current state of fat grafting: a review of harvesting, processing, and injection techniques. Plast Reconstr Surg. 2015 Oct;136(4):897-912. PMID: 26086386 DOI: https://doi.org/10.1097/PRS.0000000000001590
4. Sinno S, Wilson S, Brownstone N, Levine SM. Current thoughts on fat grafting: using the evidence to determine fact or fiction. Plast Reconstr Surg. 2016 Mar;137(3):818-824. DOI: https://doi.org/10.1097/01.prs.0000479966.52477.8b
5. Mendes FH, Viterbo F. Abdominoplasty after massive weight loss. In: Avelar JM, ed. New concepts on abdominoplasties and further aplications. New York: Springer; 2016. p. 356-388.
6. Mendes FH, Viterbo F, Deffunne E, et al. Fragmented fat: a new method for harvesting and processing of lipograft. J Plast Reconstr Aesthet Surg. 2019 Jun;72(6):1030-1048. PMID: 30824381 DOI: https://doi.org/10.1016/j.bjps.2019.02.001
7. Zuk PA, Zhu M, Muzuno H, et al. Multilineage cells from human adipose tissue: implications for cell-based therapies. Tissue Eng. 2001 Apr;7(2):211-28. DOI: https://doi.org/10.1089/107632701300062859
8. Carvalho AM, Alves AL, Golim MA, et al. Isolation and immunophenotypic characterization of mesenchymal stem cells derived from equine species adipose tissue. Vet Immunol Immunopathol. 2009 Dec;132(2-4):303-6. DOI: https://doi.org/10.1016/j.vetimm.2009.06.014
9. Strober W. Trypan blue exclusion test of cell viability. Curr Protoc Immunol. 2015 Nov;111(1):A3.B.1-3. DOI: 10.1002/0471142735.ima03bs111
10. Boschert MT, Beckert BW, Puckett CL, Concannon MJ. Analysis of lipocyte viability after liposuction. Plast Reconstr Surg. 2002 Feb;109(2):761-765;discussion:766-7. DOI: https://doi.org/10.1097/00006534-200202000-00055
11. Mushahary D, Spittler A, Kasper C, Weber V, Charwat V. Isolation, cultivation and characterization of human mesnchymal stem cells. Cytometry A. 2018 Jan;93(1):19-31. DOI: https://doi.org/10.1002/cyto.a.23242
12. Bourin P, Brunnell BA, Castella L, et al. Stromal cells from the adipose tissue-derived stromal vascular fraction and culture expanded adipose tissue-derived stromal stem cells: a joint statement of the International Federation for Adipose Therapeutics and Science (IFATS) and the International Society for Cellular Therapy (ISCT). Cytotherapy. 2013 Jun;15(6):641-8. DOI: https://doi.org/10.1016/j.jcyt.2013.02.006
13. Fritz WD, Swartz WM, Rose S, et al. Limb allografts in rats immunosuppressed with cyclosporine A. Ann Surg. 1984;199(2):211-5.
14. Li K, Gao J, Zhang Z, et al. Selection of donor site for fat grafting and cell isolation. Aesthetic Plast Surg. 2013 Feb;37(1):153-8. PMID: 23232729 DOI: https://doi.org/10.1007/s00266-012-9991-1
15. Coleman SR. Long-term survival of fat transplants: Controlled demonstrations. PMID: 8526158 Aesthetic Plast Surg. 1995;19(5):421-425.
16. Coleman SR. Structural fat grafting: More than a permanent filler. Plast Reconstr Surg. 2006 Sep;118(3 Suppl):108S-120S. DOI: https://doi.org/10.1097/01.prs.0000234610.81672.e7
17. Fisher C, Grahovac TL, Schafer ME, Shippert RD, Marra KG, Rubin JP. Comparison of harvest and processing techniques for fat grafting and adipose stem cell isolation. Plast Reconstr Surg. 2013 Aug;132(2):351-61. PMID: 23584621 DOI: https://doi.org/10.1097/PRS.0b013e3182958796
18. Klein JA. Tumescent technique for local anesthesia improves safety in large- volume liposuction. Plast Reconstr Surg. 1993 Nov; 92(6):1085-1098. DOI: https://doi.org/10.1097/00006534-199311000-00014
19. Agostini T, Lazzeri D, Pini A, et al. Wet and dry techniques for structural fat graft harvesting. Plast Reconstr Surg. 2012 Aug;130(2):331e-339e. PMID: 22495217 DOI: https://doi.org/10.1097/PRS.0b013e3182589f76
20. Moore Junior JH, Kolaczynski JW, Morales LM, et al. Viability of fat obtained by syringe suction lipectomy: Effects of local anesthesia with lidocaine. Aesthetic Plast Surg. 1995;19:335-339. DOI: https://doi.org/10.1007/BF00451659
21. Livaoğlu M, Buruk CK, Uraloğlu M, et al. Effects of lidocaine plus epinephrine and PMID: 22777468 prilocaine on autologous fat graft survival. J Craniofac Surg. 2012 Jul;23(4):1015-8.
22. Shoshani O, Berger J, Fodor L, et al. The effect of lidocaine and adrenaline on the viability of injected adipose tissue: An experimental study in nude mice. J Drugs Dermatol. 2005 May/Jun;4(3):311-6. PMID: 15898286
23. Keck M, Zeyda M, Gollinger K, et al. Local anesthetics have a major impact on viability of preadipocytes and their differentiation into adipocytes. Plast Reconstr Surg. 2010 Nov;126(5):1500-5. PMID: 21042106 DOI: https://doi.org/10.1097/PRS.0b013e3181ef8beb
24. Ferreira LM, Borsanyi JP, Bemhain P, et al. Rat limb allotransplantation: Efficacy of subtherapeutic dose combination immunotherapy with cyclosporine and RS-61443. Rev Hosp São Paulo Esc Paul Med. 1995;6(1-2):15-9.
25. Kato H, Mineda K, Eto H, et al. Degeneration, regeneration, and cicatrization after fat grafting: dynamic total tissue remodeling during the first 3 months. Plast Reconstr Surg. 2014 Mar;133(3):303e-313e. PMID: 24572875
26. Galie M, Pignatti M, Scambi I, Sbarbati A, Rigotti G. Comparison of different centrifugation protocols for the best yield of adipose-derived stromal cells from lipoaspirates. Plast Reconstr Surg. 2008 Dec;122(6):233e-234e. PMID: 19050511 DOI: https://doi.org/10.1097/PRS.0b013e31818d2326
27. Rigotti G, Marchi A, Galie M, et al. Clinical treatment of radiotherapy tissue damage by lipoaspirate transplant: a healing process mediated by adipose- derived adult stem cells. Plast Reconstr Surg. 2007 Apr;119(5):1409-22;discussion:1423-4. DOI: https://doi.org/10.1097/01.prs.0000256047.47909.71
1. Faculdade de Medicina de Botucatu, Universidade Estadual Paulista, Botucatu, SP,
Brazil.
Corresponding author: Flavio Henrique Mendes Rua Claudio Manoel da Costa, Nº 65, Jardim Ariano, Lins, SP, Brazil. Zip Code: 16400-464. E-mail: mendesmd@fhmendes.com.br
Article received: July 16, 2019.
Article accepted: August 2, 2019.
Conflicts of interest: none.
Institution: Faculdade de Medicina de Botucatu, Universidade Estadual Paulista, Botucatu, SP, Brazil.












 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter