

Review Article - Year 2020 - Volume 35 -
Fat embolism syndrome secondary to the use of polymethylmethacrylate in bioplasty: a systematic review
Síndrome da embolia gordurosa secundária ao uso de polimetilmetacrilato na bioplastia: uma revisão sistemática
ABSTRACT
Fat embolism syndrome (FES) is defined as the presence of fatty emboli, not only in the pulmonary system, but also in the systemic circulation, with inflammatory, neurological and cutaneous manifestations. Currently, in cosmetic surgery, the polymethylmethacrylate (PMMA) material is indicated for skin filling techniques used in injectable form in small non-incisional aesthetic procedures, known as bioplasty. The objective of this study was to carry out a systematic review of the literature to show clinical studies that addressed the appearance of fat embolism syndrome in patients who underwent PMMA (polymethylmethacrylate) infiltration in bioplasty. Even with the exhaustion of sources and the expansion of systematic research that followed the precepts of the PRISMA protocol, the answer was only one article that was added to the present study. Unfortunately, no reviews or experimental studies are looking at FES in PMMA infiltration. Most of the available reports are about liposuction and correlate with bone trauma when PMMA use is mentioned. This review serves as a wake-up call for nonscientific studies and reports on the risks of using PMMA in bioplasty, but no reports or articles were obtained related to life-threatening fat embolism.
Keywords: Polymethylmethacrylate; Fat embolism; Dermal fillers; Plastic surgery; Long-term adverse effects.
RESUMO
A síndrome da embolia gordurosa (SEG) é definida como a presença de êmbolos gordurosos, não apenas no sistema pulmonar, como também na circulação sistêmica, com manifestações inflamatórias, neurológicas e cutâneas. Na cirurgia estética, atualmente, o material polimetilmetacrilato (PMMA) apresenta indicação para técnicas de preenchimento cutâneo, utilizado na forma injetável em pequenos procedimentos estéticos não incisionais, conhecidos como bioplastia. O presente estudo teve como objetivo fazer uma revisão sistemática de literatura para mostrar estudos clínicos que abordassem a ocorrência de síndrome da embolia gordurosa em pacientes que se submeteram a infiltração de PMMA (polimetilmetacrilato) na bioplastia. Mesmo com esgotamento de fontes e ampliação da pesquisa sistemática que seguiu os preceitos do protocolo PRISMA, a resposta foi de apenas um artigo que foi adicionado ao presente estudo. Infelizmente não há revisões ou estudos experimentais que contemplem a SEG na infiltração com PMMA. A maioria dos relatos disponibilizados é proveniente de lipoaspiração e correlacionados ao trauma ósseo quando citado o uso de PMMA. Esta revisão serve de alerta para os estudos e relatos não científicos sobre os riscos da utilização de PMMA na bioplastia, mas não se obteve relatos ou relacionados com a embolia gordurosa, potencialmente fatal.
Palavras-chave: Polimetilmetacrilato; Embolia gordurosa; Preenchedores dérmicos; Cirurgia plástica; Efeitos adversos de longa duração
INTRODUCTION
Throughout the world, health practices are moving towards a more preventive approach, showing attitudes that value healthier lifestyles and behaviors based on disease prevention. In this context, it is also recognized that men and women seek strategies to reduce the visible signs of aging1.
Following the example of North America, which currently ranks first, considering the total number of surgical and non-surgical cosmetic and aesthetic procedures performed2. Brazil ranks second, being the first only when considering surgical procedures1,2.
However, in recent years, emphasis has been placed on minimally invasive aesthetic procedures3. This trend culminated in the use of a variety of non-incisional methods to combat the effects of aging, with the increased use of soft tissues in infiltrative facial implants being the most popular4.
Currently, there are a large number of fillers available for this purpose, each with its chemical composition, specific indications, and effectiveness5. This wide range of available materials requires aesthetic specialists and plastic surgeons to choose the appropriate filler for each aesthetic complaint of their patients5,6.
The ideal filler applied to treat signs of aging or to increase soft tissue should provide good cosmetic results and have a long-term effect. It must also be safe, biocompatible, and stable at the implantation site, with low-risk, non-migratory complications6.
According to Lemperle et al., In 20067, all injectable dermal fillers can cause complications. Late side effects can be divided into those caused by insufficient training or technical errors during the injection, and those caused by immune reactions (allergic and non-allergic) to the injected substance. Granuloma formations are rare events that result from type IV hypersensitivity reaction to a foreign body. They usually occur over months to years after the injection3.
Acute complications include those associated with the technique used during application and are mostly local. However, due to a chronic inflammatory reaction, they may appear years after infiltration, with the possibility of remission-reactivation episodes2,4.
The histological reaction is always similar, and the trigger for this sudden stimulation of macrophages may be a systemic infection of the patient. Dermal fillers such as silicone, bovine collagen, ArtecollTM (Hafod B.V, Rotterdam, The Netherlands), and RestylaneTM8 (Q-Med AB, Stockholm, Sweden) have been used worldwide.
Bovine collagen (ZydermTM, ZyplastaTM, McGhan Medical Corporation 3M, USA) was introduced between 1981 and 1983, becoming the standard for injectables9. ArtecollTM (Canderm Pharma Inc., Canada) was distributed between 1994 and 2006, and RestylaneTM (Q-Med AB, Stockholm, Sweden) began its triumphal advance in 19978. Since then, a variety of materials have been introduced, such as RadiesseTM (Merz, Brazil), which is approved for facial bone augmentation and has been used off-label since 2003 for the treatment of wrinkles10; and SculptraTM (Aventis, USA), which is approved for facial lipodystrophy of the human immunodeficiency virus, but has been used to treat wrinkles since 2005. The Food and Drug Administration (FDA - USA) approved RestylaneTM in 2003, HylaformTM (Genzy me Biosurgery, USA) in 2004, CaptiqueTM in 2005 and JuvedermemTM 2006 (both from Allergan, USA) for the treatment of facial wrinkles9.
The polymethylmethacrylate (PMMA) molecule does not have any animal component in its structure, which makes this molecule a biocompatible material and also provides stability even decades after the initial implantation. Its commercial applications are PMMA microspheres suspended in bovine collagen2.
In the context of the indications of the PMMA compound, the filling of grooves, deep wrinkles, scars, dermal defects, soft and bone tissues stands out6. It is also used in restorative procedures for volumetric facial and body correction of lipodystrophy syndrome, a result of the use of antiretrovirals in patients with the human immunodeficiency virus11.
Fat embolism syndrome (FES) is a poorly defined clinical entity that arises from systemic manifestations of fat embolism within the microcirculation. Embolized fat in the capillary beds causes direct tissue damage, in addition to inducing a systemic inflammatory response, which produces pulmonary, cutaneous, neurological, and retinal symptoms. It occurs more frequently after orthopedic trauma, as well as in patients with many clinical conditions, including liposuction, bone marrow transplantation, pancreatitis, however, as observed in the present study, rarely in bioplasty procedures using PMMA12.
OBJECTIVE
The present study aimed to carry out a systematic review of the literature in order to highlight the clinical studies that included FES in patients undergoing PMMA infiltration in bioplasty.
METHODS
Search strategies and eligibility criteria
A search of the PubMed/MEDLINE and LILACS / BVS databases was performed, including articles that addressed the topic “fat embolism syndrome secondary to the use of PMMA in bioplasty.”
We included studies in humans, older than 18 years (adults), whose publication in English was between January 1, 2000, and January 8, 2019, and the text published with full access reported on FES after bioplasty with use. PMMA intervention.
Review articles (meta-analyzes an/or systematics), letters to the editor, case reports, and experimental studies in which the complication after using PMMA did not include FES were not added.
After the response of the electronic databases, a manual search of relevant articles was carried out, since the sample was not adequate. In this way, the search date was extended from January 1970 to January 2019.
The following search terms were included in English: “fat embolism syndrome,” “polymethylmethacrylate,” and “fat embolism syndrome.” In Portuguese: “PMMA,” “polimetilmetacrilato,” “síndrome embolia gordurosa,”
“embolia lipídica.” In Spanish: “PMMA,” “polimetilmetacrilato,” “embolia grasa,” “embolia lipídica.” As protocols, the recommendations of the Preferred reporting elements for systematic reviews and meta-analyzes were followed.
Data extraction
Research data, after extraction, was included, and the authors of this article reviewed controversies. Information such as: authors, year of publication, and country of origin was reviewed to identify and exclude duplicate publications from the same cohort. The extracted data included the total number of patients and injuries, age, sex, and occurrence.
RESULTS
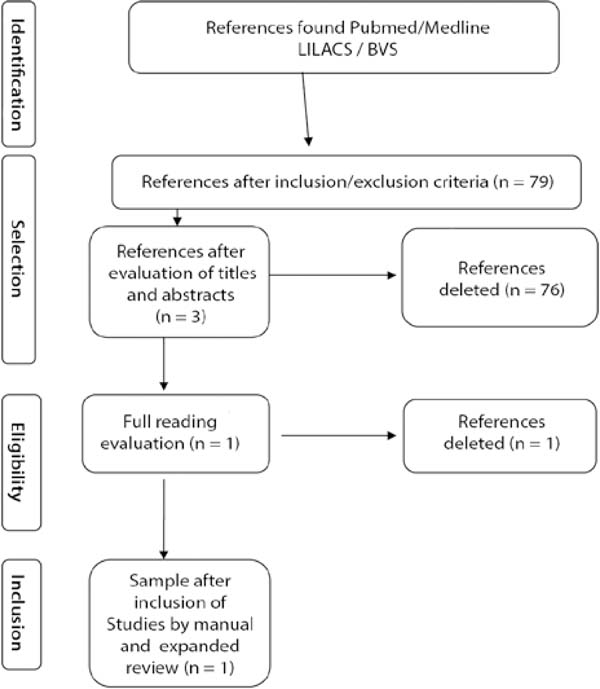
In the PubMed/MEDLINE electronic search, 20 research article references were found. After reading the titles, 18 references were excluded, leaving two references. When read in full, two studies were excluded as they did not include bioplasty and the use of PMMA. The exclusion of these articles was based on the inclusion and exclusion criteria described above.
In the LILACS / VHL database, 59 references to research articles were found (subject index). After reading the titles, 50 references were excluded, leaving nine references. When reading in their entirety, three studies that did not contemplate bioplasty and the use of PMMA were excluded, and the remaining six were also excluded because they are liposuction related studies that do not consider the use of PMMA. The exclusion of these articles was based on the inclusion and exclusion criteria described above.
In this way, a manual search was performed in the three languages (English, Portuguese, and Spanish), and the search date was extended from January 1970 to January 8, 2019. As a result, only one article was available for a complete reading. (Spanish language). The selection criteria are described in Figure 1.
Chart 1 describes the only study selected, by manual search, for this article, in which it presents the authors, the country of origin of the research, the main objectives and the main characteristics of the study.
| Author/year | Country of Origin | Methods and Objectives | Study characteristics |
|---|---|---|---|
| Salgado and Olvera, in 200813. | México | Presentation of clinical case and outcomes. | Clinical case report with outcomes after FES in a post-procedure patient with PMMA infiltration |
Source: Elaborated by the author.
DISCUSSION
The bibliographic search resulted in a single article, according to the descriptors, and the inclusion and exclusion requirements. Unfortunately, there is no significant number of articles that address FES in PMMA infiltration. Most of the available reports come from liposuction and correlate with bone trauma when PMMA use is mentioned.
The subject of the only report was a 26-year-old woman who started the condition 24 hours after PMMA injection into the bilateral gluteal region at a cosmetic clinic. The patient presented fever, anxiety, diaphoresis, headache, dizziness, drowsiness, and dysarthria13.
On physical examination at admission, blood pressure of 110/70mmHg was presented, heart rate of 113 beats per minute, respiratory rate of 21 respiratory incursions per minute, with supplemental support of oxygen by mask and nebulizer; body temperature of 38.4° C, with Glasgow of 12. She was aware13.
Pelvic tomography revealed abundant, diffuse, non-encapsulated material between the skin and the gluteus maximus. Her management was in the Intensive Care Unit, with general support, mechanical ventilation in the volume control in assisted mode. Broad-spectrum antibiotics and anticoagulation with low molecular weight heparin were also prescribed13.
The patient developed pneumonia, systemic inflammatory response syndrome, and cerebral edema. Due to prolonged intubation and inadequate management of secretions, it was necessary to perform a tracheostomy. She had a prolonged clinical evolution; however, satisfactory, allowing her to remain without mechanical ventilation support. The infectious respiratory focus was controlled, and the patient evolved with hemodynamic stability. The patient was discharged after three weeks of hospitalization. In this case report, massive PMMA infiltration destroyed adipose tissue, which, together with the microspheres of this product, provoked fat embolism in the patient13.
The case presented by Salgado and Olvera in 200813 was of non-medical professionals who performed the procedure. This type of practice has generated a public health problem, since most of the time, the subjects do not have medical training, and there are no reliable statistics on the incidence or prevalence of patient complications concerning the substances used. FES was first described in 1862, by Zenker, who visualized fat cells in the pulmonary circulation of a polytraumatized individual after performing a biopsy14. The term FES is a severe consequence of fatty emboli that causes a distinct pattern of symptoms and clinical signs15.
The typical clinical manifestation is the triad of acute respiratory failure, thrombocytopenia, and neurological dysfunction15. No definitive diagnostic criteria or tests have been developed, which makes the diagnosis of FES more difficult. It usually occurs within 48 hours after the trauma or during surgical procedures in most patients12.
There are two main theories for the genesis of fat embolism; they are the mechanical theory and the biochemical theory. The first suggests that the obstruction of the systemic vasculature by fat embolism results from the direct release of the bone marrow into the venous system after the trauma. High intramedullary pressure after trauma causes the release of fat through open venous sinusoid. This embolized fat favors the obstruction of the capillary beds12.
The second theory proposes that the inflammatory response to trauma causes the release of free fatty acids from the bone marrow into the venous system. Elevations in free fatty acids and inflammatory mediators damage the capillary beds. Elevated levels of free fatty acids have been correlated with hypoxemia and the induction of pulmonary inflammation12.
Regarding the therapeutic approach, there is no specific treatment for FES. The procedures are based on clinical support measures, hemodynamic stabilization, volume replacement, nutrition and oxygen therapy or mechanical ventilation with alveolar recruitment in more severe cases14. There is insufficient data to support the initiation of steroid therapy, once FES is established. The proposed mechanism of action is generally an anti-inflammatory agent that reduces perivascular hemorrhage and edema. An experimental study did not show a beneficial effect and there were no prospective, randomized, and controlled clinical studies that demonstrated a significant benefit with its use15.
CONCLUSION
In the current aesthetic situation, there is a significant increase in minimally invasive techniques that favor non-incisional methods, such as the implantation of PMMA, to minimize the effects of aging and correct body defects. It is known that in order to prevent or treat disorders, such as FES with dermal implants, it is essential to know their composition, the physiological reactions of the tissue, the time of absorption, and persistence. There is an urgent need for more studies targeting PMMA in cosmetic procedures, their risks, and clinical cases that identify FES and other potentially fatal postoperative problems for the patient.
COLLABORATIONS
|
CGAO |
Analysis and/or data interpretation, Conception and design study, Conceptualization, Data Curation, Final manuscript approval, Formal Analysis, Investigation, Methodology, Project Administration, Resources, Supervision, Validation, Visualization, Writing - Original Draft Preparation, Writing - Review & Editing |
|
FRS |
Analysis and/or data interpretation, Conceptualization, Final manuscript approval, Investigation, Resources, Supervision, Validation, Visualization |
|
FAAF |
Conceptualization, Data Curation, Final manuscript approval, Supervision, Visualization, Writing - Original Draft Preparation |
|
RZDF |
Final manuscript approval, Data Curation, Conceptualization, Writing - Original Draft Preparation, Supervision, Visualization. |
REFERENCES
1. Chacur R, Menezes HS, Chacur NMBS, Alves DD, Mafaldo RC, Gomes LD, et al. Replacement of gluteal implants by polymethylmethacrylate filler: case report. Case Reports Plast Surg Hand Surg. 2019 Jan;6(1):20-4.
2. Souza TAB, Colomé LM, Bender EA, Lemperle G. Brazilian consensus recommendation on the use of polymethylmethacrylate filler in facial and corporal aesthetics. Aesthetic Plast Surg. 2018 Oct;42(5):1244-51.
3. Vedamurthy M. Beware what you inject: complications of injectables - dermal fillers. J Cutan Aesthet Surg. 2018 Apr/Jun;11(2):60-6.
4. Buck II DW, Alam M, Kim JYS. Injectable fillers for facial rejuvenation: a review. J Plast Reconstr Aesthet Surg. 2009 Jan;62(1):11-8.
5. Parada MB, Cazerta C, Afonso JPJM, Nascimento DIS. Overview and management of fillers complications. Surg Cosmet Dermatol. 2016;8(4):342-51.
6. Vargas AF, Amorim NG, Pitanguy I. Late complications of permanent fillers. Rev Bras Cir Plást. 2009;24(1):71-81.
7. Lemperle G, Rullan PP, Gauthier-Hazan N. Avoiding and treating dermal filler complications. Plast Reconstr Surg. 2006 Oct;118(3 Suppl 1):92S-107S.
8. Pollack SV. Some new injectable dermal filler materials: Hylaform, Restylane, and Artecoll. J Cutan Med Surg. 1999 Dec;(3 Suppl 4):S27-35.
9. Johl SS, Burgett RA. Dermal filler agents: a practical review. Curr Opin Ophthalmol. 2006 Oct;17(5):471-9.
10. Viscusi KS, Hanke CW. Soft tissue augmentation. In: Baran R, Maibach HI, eds. Textbook of cosmetic dermatology. 5th ed. Boca Raton: CRC Press; 2017. p. 473-80.
11. Antonio CR, Antonio JR, Oliveira GB, Alves FT. Polymethylmethacrylate (PMMA) filling in the lower limbs of a patient with lipodystrophy caused by antiretroviral drugs. Surg Cosmet Dermatol. 2014;6(4):373-5.
12. Kwiatt ME, Seamon MJ. Fat embolism syndrome. Int J Crit Illn Inj Sci. 2013 Jan;3(1):64-8.
13. Salgado EG, Olvera RM. Síndrome de embolia grasa secundario a infiltración de polimetilmetacrilato em región glútea. Cir Plast. 2008;18(2):78-80.
14. Jorens PG, Van Marck E, Snoeckx A, Parizel PM. Nonthrombotic pulmonary embolism. Eur Respir J. 2009 Aug;34(2):452-74.
15. Gupta A, Reilly CS. Fat embolism. Contin Educan Aesthetic Crit Care Pain. 2007 Oct;7(5):148-51.
1. Pontifícia Universidade Católica de Minas Gerais,Betim, MG,Brazil.
2 . Hospital Eduardo de Menezes, Departamento de Infectologia, Belo Horizonte, MG,
Brazil.
Corresponding author: Carina Gabriela Andrade Oliveira, Rua Pintarroxo, 157, Bairro Goiânia, Belo Horizonte, Minas Gerais, MG, Brazil. Zip Code: 31950-110. E-mail: carina.andradde@gmail.com
Article received: June 29, 2019.
Article accepted: February 29, 2020.
Conflicts of interest: none.





 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter