

Original Article - Year 2021 - Volume 36 -
5-year revision (2015-2019) of immediate alloplastic reconstruction in Hospital and University Center of Coimbra, Portugal
Revisão de 5 anos (2015-2019) da reconstrução aloplástica imediata no Centro Hospitalar e Universitário de Coimbra, Portugal
ABSTRACT
Introduction: With breast cancer being the most prevalent malignancy worldwide, conservative treatment is of tremendous importance. Nevertheless, in many cases, mastectomy remains the indicated surgical procedure, and like any other amputation, it carries a significant burden on those patients. In the case of mastectomy, immediate breast reconstruction is the standard of care. Alloplastic reconstruction remains the most widely performed type of immediate breast reconstruction.
Methods: In this article, the authors present a series of 105 cases of immediate alloplastic reconstruction in 5 years from 2015 to 2019 in Centro Hospitalar e Universitário de Coimbra, Portugal. It includes curative and risk-reducing mastectomies performed by oncologic gynecologists. The reconstruction options offered by the plastic reconstructive team included both direct-to-implant reconstruction and two-stage reconstruction with the use of tissue expanders.
Results: Data regarding the oncologic disease, type of mastectomy, patient selection criteria and immediate and late postoperative outcomes with different techniques of immediate reconstruction were collected, analyzed, and compared to literature. In our study, body mass index was the single most significant predictor of complications and, its impact was statistically significant.
Conclusion: The results obtained represent an essential step to improving care quality for women undergoing breast reconstruction.
Keywords: Breast neoplasms; Experimental breast neoplasms; Segmental mastectomy; Mammography; Breast implants.
RESUMO
Introdução: Como o câncer de mama é a doença maligna mais prevalente em todo o mundo, o tratamento conservador é de extrema importância. No entanto, em muitos casos, a mastectomia continua sendo o procedimento cirúrgico indicado e, como qualquer outra amputação, leva um fardo significativo para essas pacientes. No caso da mastectomia, a reconstrução imediata da mama é o tratamento padrão. A reconstrução aloplástica continua sendo o tipo mais amplamente realizado de reconstrução mamária imediata.
Métodos: Neste artigo, os autores apresentam uma série de 105 casos de reconstrução aloplástica imediata em 5 anos de 2015 a 2019 no Centro Hospitalar e Universitário de Coimbra, Portugal. Inclui mastectomias curativas e redutoras de risco realizadas por ginecologistas oncológicos. As opções de reconstrução oferecidas pela equipe de reconstrução plástica incluíram tanto a reconstrução direta no implante quanto a reconstrução em dois estágios com o uso de expansores de tecido.
Resultados: Dados sobre a doença oncológica, tipo de mastectomia, critérios de seleção das pacientes e resultados pós-operatórios imediato e tardio com diferentes técnicas de reconstrução imediata foram coletados, analisados e comparados com a literatura. Em nosso estudo, o índice de massa corporal foi o único preditor mais significativo de complicações e seu impacto foi estatisticamente significativo.
Conclusão: Os resultados obtidos representam uma etapa essencial para a melhoria da qualidade da assistência à mulher em reconstrução mamária.
Palavras-chave: Neoplasias mamárias; Neoplasias mamárias experimentais; Mastectomia segmentar; Mamografia; Implantes mamários.
INTRODUCTION
Immediate breast reconstruction after mastectomy has undeniable benefits, both aesthetic and psychological, avoiding a stigmatizing procedure with clear repercussions on the quality of life of cancer patients or women at high risk of developing breast cancer1.
Approximately one in eight women in the United States develops breast cancer, with 200,000 new cases diagnosed per year2. Following the trend towards more frequent conservative surgery, there is also an increasing trend for immediate breast reconstruction following mastectomy. Reconstruction rates increased from 11.6% to 36.4% for unilateral mastectomies and 36.0% to 57.2% regarding bilateral mastectomies between 1998 and 2011, respectively3. The American Society of Plastic Surgeons estimated that 109,256 women underwent breast reconstruction in 2016 in the USA alone4. The most frequent immediate breast reconstruction is alloplastic. Alloplastic reconstruction includes two-stage with the use of tissue expanders and direct-to-implant (DTI) reconstruction5.
Major complications implying reoperation and reconstruction failure are reported to be as high as 20% to 35%4. Therefore, quality assessment and evaluation of surgical outcomes are mandatory to improve clinical practice. Patient’s risk factors such as obesity, smoking, radiation, and the use of acellular dermal matrices influence the rate of complications6. The pandemic and increasing proportion of obesity mean that a significant number of these patients will have an additional risk of postoperative complications, as pointed in literature, with a commitment to the feasibility of reconstruction6.
Evaluating breast reconstruction outcomes in this population is a challenge due to the length of time necessary to complete the reconstruction process and the number of variables that may interfere with the long-term results.
The most frequent complications related to implant-based breast reconstruction are skin necrosis and infection, frequently leading to additional surgeries and compromising the optimal timing of adjuvant therapies2.
The overall 5-year survival rate after mastectomy is 98.7%. Yet and, according to English literature, most women submitted to mastectomy still do not undergo breast reconstruction7.
OBJECTIVE
The purpose of the study is to evaluate immediate and late postoperative outcomes, comparing different types of immediate reconstruction and identifying risk factors for complications of immediate alloplastic reconstruction in Hospital and University Center of Coimbra (CHUC - Centro Hospitalar e Universitário de Coimbra), Portugal.
These results represent an important step to improve the quality of care for women undergoing breast reconstruction.
METHODS
This retrospective study evaluated women who underwent immediate alloplastic reconstruction following mastectomy at a tertiary faculty medical center over five years between 2015 and 2019. Patients were selected if they had undergone mastectomy with implant-based reconstruction (DTI or two-stage with tissue expander). Patients who underwent delayed breast reconstruction were excluded from this study.
Clinical data including age, comorbidities, smoking status, neoadjuvant chemotherapy and body mass index (BMI) were collected from medical records. Comorbidities included obesity, hypertension, coronary artery disease, and diabetes.
Surgical collected variables were the type of reconstruction (two-stage versus DTI), laterality (unilateral or bilateral procedure), and acellular dermal matrix. Surgical teams were composed of gynecologic oncologists and plastic surgeons.
Clinically relevant early and late complications were analyzed and compared according to the type of reconstruction. Early complications included infection, necrosis of mastectomy flaps/nipple-areolar complex (NAC), hematoma, seroma or extrusion/dehiscence. Late complications comprised late seroma, malposition or rotation of the implant, capsular contracture, chronic pain, and lymphedema. Seroma was defined as any fluid collection that developed after drain removal or daily output above 30cc during more than ten days. Infection was defined as any patient receiving antibiotics beyond the expected postoperative course or restarting antibiotics for a suspected infection or erythema. Capsular contracture was defined as Baker capsular contracture classification of grade III and IV8.
Breast reconstruction failure was defined as a complication resulting in the removal of an implant or tissue expander. The need for implant removal was evaluated based on the cause. Further reconstructive options were later given to these patients.
Trend data on BMI, categorized as normal, overweight and obese, were analyzed using logistic regression.
Statistical analysis was performed using SPSS version 23.0. Categorical variables were analyzed using the chi-square test and continuous variables with Student’s t-test. The significance level was set at α=0.05 (95% confidence interval).
This observational study was developed in Hospital and University Center of Coimbra (CHUC - Centro Hospitalar e Universitário de Coimbra), submitted to the CHUC ethics commission with the reference number 210/CES.
RESULTS
Our assay comprises a retrospective study of immediate alloplastic breast reconstruction in CHUC in 5 years, from 2015 to 2019. In this period, a total of 500 patients underwent breast reconstruction by the plastic surgery department. From this sample, 132 women underwent immediate breast reconstruction after undergoing mastectomy for breast cancer or in a preventive manner by the gynecology oncology team.
Most of these patients underwent immediate alloplastic reconstruction comprising a sample of 105 patients selected for this article. Therefore, immediate alloplastic reconstruction comprised about 80% of total immediate reconstruction (with 20% being autologous) and about 21% of total breast reconstruction in our department. The average patient age was 48.5±8.2 [27-71] years. 87.6% (n=92) underwent therapeutic mastectomy for breast cancer, predominant invasive ductal carcinoma (44,8%, n=47), followed by ductal carcinoma in situ (24.8%, n=26), and invasive lobular carcinoma (13.3%, n=14). Additionally, five women were submitted to contralateral prophylactic mastectomy in the same operative time of total therapeutic mastectomy. 12.4% (n=13) had risk-reducing (prophylactic) mastectomy.
Most patients had unilateral breast reconstruction (84.8% [n=89]). Bilateral reconstruction was performed in 16 women (15.2%); 6 were risk-reducing mastectomies, 5 had bilateral breast cancer, and the remaining five were performed in a context of contralateral risk-reducing mastectomy.
Total mastectomy was performed in 66 patients (62.9%), of which three were bilateral; skin-sparing mastectomy in 17 cases (16.2%), of which 2 were bilateral, both risk-reducing; and nipple-sparing mastectomy in 16 (15.2%), of which five were bilateral. In addition, six women were submitted to total mastectomy and contralateral nipple-sparing mastectomy.
41.9% (n=44) of patients underwent immediate breast reconstruction using direct-to-implant technique, while 58.1% (n=61) underwent 2-stage reconstruction with expander. Acellular dermal matrix (ADM) was used in 26.7% (n=27) of breast reconstructions. The statistical comparison showed a significant increase in direct-to-implant technique vs. expander over the years (from 19.0% in 2015 to 52.4% in 2019).
Secondary/complementary procedures
43% (n=45) patients had undergone secondary procedures on the reconstructed breast alone or in combination. There were 26 NAC reconstruction, 24 lipofilling, 2 cases of mastopexy, and four scar revisions. 40% (n=42) of our patients underwent contralateral symmetrization either by reduction mammoplasty or mastopexy (n=39) or by breast augmentation (n=3).
Most common indications for revisions included improving soft-tissue contour irregularities. Lipofilling has become a common adjunct to enhance contours and camouflage the periphery of the implant (n=25).
Complications
The average patient admission time was days 9.5±5.0 [2-28]. The overall complications rate was 47.6% (n=50).
Early complications occurred in 32.3% (n=34) and included infection (n=10), partial necrosis of mastectomy flaps (n=6) and complete necrosis (n=4), hematoma (n=8), seroma (n=12), and extrusion/dehiscence (n=5). Total failure of reconstruction occurred in 8 cases.
Late complications were less frequent, affecting 20.0% (n=21) patients. Comprised late seroma (n=3), malposition or rotation of the implant (n=2), capsular contracture (n=7), chronic pain (n=6), and lymphedema (n=2). Implant replacement was required in 3 cases.
Overall complication rates, both early and delayed, are stated in Table 1.
| Early complications | N | % |
|---|---|---|
| Seroma/prolonged drainage | 12 | 11.4 |
| Hematoma | 8 | 7.6 |
| Necrosis of mastectomy flaps or NAC | 10 | 9.5 |
| Extrusion | 5 | 4.7 |
| Infection | 10 | 9.5 |
| Late complications | N | % |
| Late seroma | 3 | 2.8 |
| Malposition, rotation of the implant | 2 | 1.8 |
| Capsular contracture | 7 | 6.6 |
| Chronic pain | 6 | 5.7 |
| Lymphedema | 2 | 1.8 |
NAC: nipple-areolar complex
Minor complications such as suture exposure, delayed healing and epidermolysis were usually self-resolving with conservative treatment.
Two patients were managed by revision of the implant, and three required implant exchange. Twenty patients had a complete failure of the alloplastic reconstruction. Of these, 12 were offered autologous reconstruction (4 deep inferior epigastric artery perforator (DIEP), 5 atissimus dorsi (LD), 2 thoracodorsal artery perforator (TDAP), and 1 transverse rectus abdominis myocutaneous (TRAM). In addition, eight women did not want further reconstruction, and 2 had a recurrence of the oncologic disease.
Statistical comparison showed a significant increase in overall complications for patients in the direct-to-implant technique versus two-stage tissue expander-based immediate reconstruction (59.1% [n=26] vs. 39.3% [n=24], p=0.046).
The average BMI was 24.8±4.0 [18-37] kg/m2. 59.1% of women had normal weight (BMI 18.5-24.9kg/m2), 24.7% were overweight (BMI 25.0-29.9kg/m2), and 16.1% were obese (BMI≥30.0kg/m2).
The rate of complications was significantly higher in the group of obese women compared to women with normal weight (80.0% vs. 40.0%, p=0.006) and overweight (80% vs. 43.5%, p=0.026), mainly at the expense of initial complications (66.7% vs. 23.6%, p=0.002; 66.7 vs. 26.1%, p=0.013). Overweight women had no more complications compared to women of normal weight. The incidence of late complications was also not significantly different among all groups. BMI as a predictive factor for complications did not reach statistical significance, but the cutoff of 23.5kg/m2 was associated with better sensitivity (56.8%) and specificity (53.1%) together. The cutoff for obesity (BMI>30kg/m2) was associated with a specificity of 95.9%, despite a reduced sensitivity value (15.9%). Comparison of complications across BMI indexes is stated in Table 2.
DISCUSSION
As stated above, immediate alloplastic reconstruction can be either direct-to-implant or two-stage with the use of an expander and implant.
Direct-to-implant
In selected patients, this approach offers benefits over the two-stage breast reconstruction such as good symmetry with small breasts, fewer surgeries, faster return to everyday life, and avoidance of the period of expansion. It also adds psychological benefits9 - the feeling that the patient never wholly lost the breast and overall cost savings - do it all in one procedure10-12. The limitations of DTI are breast size, higher risk for skin or nipple necrosis is technically more demanding to make it right in one procedure, and the risk of postoperative radiation negatively affecting the outcome.
| Comparing weight to complications: |
|---|
| Normal weight vs. Excess weight -> p=0.799 |
| Normal weight vs. Obesity --> p=0.006 ---> Statistically significant |
| Excess weight vs. Obesity --> p=0.026 ---> Statistically significant |
| Comparing weight to early complications: |
| Normal weight vs. Excess weight --> p=0.498 |
| Normal weight vs. Obesity -> p=0.001 ---> Statistically significant |
| Excess weight vs. Obesity -> p=0.02 ---> Statistically significant |
| Comparing weight to late complications: |
| Normal weight vs. Excess weight --> p=0.966 Normal weight vs. Obesity --> p=0.791 Excess weight vs. Obesity --> p=0.785 |
BMI: Body Mass Index
The ideal candidate is a healthy non-smoker with small cup breasts who desires a similar or slightly larger size, with minimal ptosis, to do a prophylactic mastectomy or to treat an early-stage disease with a low likelihood for postoperative adjuvant therapy.
The main limitation in DTI is providing adequate, stable soft-tissue coverage for an implant in a new mastectomy pocket.
Women with larger size and ptotic breasts may be candidates for skin reduction mastectomy (usually in T pattern) with direct-to-implant reconstruction; this procedure increases the risk of NAC necrosis.
In our center, patients with a history of breast radiation and those likely to require post-mastectomy radiation have traditionally been offered autologous reconstruction.
The plane chosen in our center mainly was the partial submuscular coverage using ADM to cover the lower pole in a dual-plane fashion.
Usually, after creating the pocket for the implant, the muscle is advanced inferiorly until the desired upper pole contour is achieved. The matrix is then trimmed to create a tight and supportive pocket and sutured to the lower pole to function as a pectoral expansion down to the inframammary fold (IMF) in a dual-plane fashion.
ADM has been routinely used in DTI reconstruction. The two brands of ADM that were most often employed in our department/hospital were Strattice® and Native®.
Some patients with well-vascularized mastectomy flaps were given a subcutaneous or pre-pectoral reconstruction usually combined with ADM wrapped around the implant. For this technique, Surgimend® was chosen as the preferred ADM due to its increased flexibility and support compared to the former. However, this technique can cause significant stress to the lower pole mastectomy flaps leading to soft-tissue necrosis in the short term and significant thinning in the long term.
Total submuscular coverage is usually challenging to achieve because it limits the size of an implant that can be placed and does not allow for a natural fill of the lower pole. Therefore, it was reserved for expander placement and not for DTI.
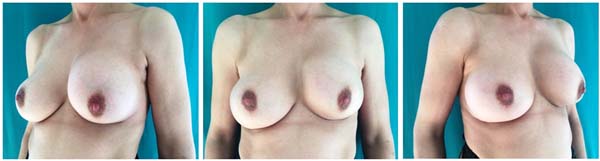
Clinical case 1 depicts a 45 years old patient diagnosed with an invasive carcinoma on the left breast. The patient had a previous breast augmentation 20 years before and had a left breast capsular contraction (preoperative - Figure 1). The patient underwent bilateral NAC sparing mastectomy and an axillary lymphadenectomy on the left side. Immediate DTI reconstruction was performed with 460cc implants and ADM in a dual-plane fashion. Figure 2 depicts the final result 1-year after.
Clinical case 1: immediate DTI breast reconstruction
Two-stage immediate reconstruction
Because it involves two surgical procedures, this technique increases the chances of creating a better result. It is technically more straightforward and has broader indications. It causes less strain on the mastectomy flaps due to lower expansion volumes and, therefore, less risk of skin necrosis. Compared with the DTI, its disadvantages are a delayed outcome due to the expansion period and the need for one more surgery.
The ideal patients are healthy non-smokers who have good quality expandable chest wall skin and soft tissues.
Its absolute contraindications are the lack of available expandable skin or underlying bony support to withstand the forces of the overlying process of expansion. Therefore, we do not routinely offer this reconstruction to patients that underwent or will undergo radiotherapy. Instead, these patients were offered autologous reconstruction.
Markings
Markings are made with the patient in the sitting position, with both oncologic and reconstructive teams present. Anatomic landmarks that must be drawn on the patient include the chest midline, medial, and superior breast borders, and lateral mammary fold (LMF) and IMF.
The chosen incision is based on various factors, including the preoperative size and shape of the breast, the desired postoperative breast size and position, and the location of pre-existing scars.
Despite helping to achieve the desired reconstructive result, markings should allow the surgeon to carry out a safe oncologic mastectomy.
Plane chosen
The plane chosen in our center was preferably total submuscular coverage to cover the expander.
Dual-plane was occasionally used. When chosen, the dual plane technique was usually combined with ADM to cover the inferior pole.
Pre-pectoral was only seldom used as an expansion of the lower pole can cause significant stress to the mastectomy flaps leading to soft-tissue necrosis in the short term and significant thinning in the long term.
Due to losing the lateral border because of the large mastectomy pocket, anterior serratus flaps are frequently used to control the lateral position of the expander and define the LMF or anterior axillary line.
Incision
The most often used incision is a transverse ellipse, which provides the opportunity to decrease the size of the skin envelope with minimal risk for skin flap compromise. It also helps to conceal the scar under the brassiere.
In nipple-sparing mastectomies, most often, an inferior periareolar incision was used. The type of mastectomy, the importance of gentle tissue handling, preservation of the IMF and the serratus fascia, and minimizing unnecessary lateral dissection of the breast pocket are crucial factors to consider.
Drains
In our center, we usually place a drain within the submuscular/ADM pocket. A second drain is placed along the inframammary crease in the subcutaneous plane and brought out through a separate incision in the anterior axillary line. Drains are maintained until output decreases below 30cc. Antibiotics are routinely prescribed for one week after or until the drains are removed.
Expansion period
Expansion usually begins one month after surgery, and volumes are limited by discomfort and signs of stress to the skin (blanching). Expansion is generally made in 3 to 5 visits to the outpatient clinic. Exchange to implant is usually performed from 6 months to 1-year post-surgery.
Implant choice
Size selection begins during the initial consultation. First, chest wall dimensions must be accurately measured, focusing on breast width, height, and projection, allowing the surgeon to estimate breast volume.
According to literature, a small overcorrection from the mastectomy weight is suggested to accommodate the laxity created in the skin envelope due to the mastectomy13. Mostly high-profile implants were used for maximal projection.
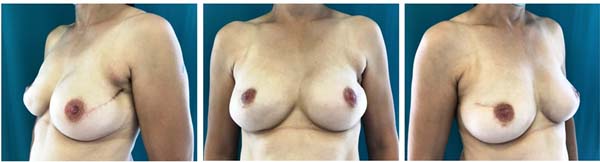
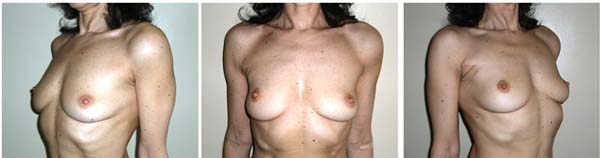
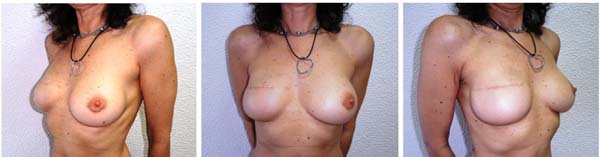
An example of a patient that underwent two-stage immediate reconstruction is depicted in clinical case 2, a 46 years old patient diagnosed with an invasive ductal carcinoma on the right breast (preoperative - Figure 3). The patient underwent a total mastectomy and two-stage immediate reconstruction with an expander and later a 270cc implant. The left breast was augmented with a 180cc implant. Figure 4 depicts the result 2-years after. The patient did not wish to reconstruct the NAC.
Clinical case 2: two-stage immediate reconstruction
Comparing complications to literature
In some articles, major complications have been reported with an overall incidence as low as 6% each13,14.
In other series, individual complications including implant loss, skin necrosis requiring re-operation, infection, hematoma, seroma, and capsular contracture were as low as 2%13,14. In our department, complication rates were somewhat like some literature series, with slightly higher percentage of seroma formation, infections (9.5%), and hematoma formation (7.6%).
Comparing the reconstructions after NAC-sparing mastectomy
After NAC-sparing mastectomies, another series of 500 consecutive one-stage and two-stage reconstructions showed overall low complication rates and lower than 10% nipple loss. In addition, the risk of infection was 3.3%12.
In our center, there were two cases of total nipple necrosis and one case of infection hence making a prevalence of 9.5 % and 4.5%, respectively, for each complication.
The most extensive multi-institutional report comparing early complications of direct-to-implant reconstruction with two-stage reconstruction found a higher rate of overall complications (6.8% compared with 5.4%) and prosthesis failure (1.4% compared with 0.8%) in direct-to implant reconstruction. However, no significant difference was found concerning infection, re-operation, or major medical complications14.
In our center, despite the occurrence of a higher percentage of complications with the one-stage reconstruction (56.8%) versus the two-stage reconstruction (39.3%), we have failed to demonstrate any statistical significance between expander and implant reconstruction in terms of complications: expander (two-stage) vs. DTI 39.3% vs. 56.8%, p=0.077 (ns).
Special considerations
Patients treated in 2019 have yet to develop late complications. Some complications like seroma and even late complications like lymphedema and chronic pain may not have been registered in our records, leading to underestimating the number of cases.
Lymphedema is not a complication of breast reconstruction but instead a complication of mastectomy. Still, the authors decided it was relevant to register the number of occurrences.
CONCLUSION
Regardless of its many advantages, immediate breast reconstruction is not a straightforward procedure and has some limitations compared with delayed reconstruction.
Factors like skin flap viability are of extreme importance to the procedure’s success. In addition, patients should be aware that the surgical team ultimately decides whether to perform immediate reconstruction in the operating theatre.
Signed consent should always be obtained previously, explaining that immediate alloplastic reconstruction may not be possible and consequently deferred to a delayed setting.
Occasionally the reconstructive team might decide to perform a two-stage immediate reconstruction instead of a DTI reconstruction when mastectomy flaps are of dubious viability. Consent should always include the possibility of partial or complete necrosis of NAC and mastectomy flaps, and failure of reconstruction.
Despite being widely performed, it remains a high-risk procedure with a high likelihood of developing complications. In our series, 47% of patients developed some complication, even if a minor one.
Our higher rate of revisions compared to literature (40.5%) was partly due to considering the revisions and the secondary procedures altogether. These include reconstruction of NAC, lipofilling, revisions of scar, liposuction and mastopexy, and usually were performed in the same surgery.
Managing complications
Postoperative complications must be managed aggressively and in a timely fashion. Seromas and hematomas must be drained immediately to prevent excess tension on the overlying skin flaps and minimize long-term implant malposition.
Skin flap necrosis must be followed closely and, if not healing quickly, should be excised and closed primarily to avoid the possibility of implant exposure. Skin edge necrosis (2-5mm) can often be managed with debridement and closure under local anesthesia. Larger areas usually require the removal of the implant.
What to improve?
There is a statistically significant p-value when comparing the incidence of early complications in the obese population with a BMI above 30. However, that was not true for overweight patients with a BMI between 25 and 30. Therefore, one way to decrease the complication rates is to select patients with a BMI below 30.
Further selecting patients with normal or lower than 30 BMI might be a way to decrease the percentage of complications. Overweight and obese patients should be encouraged to lose weight and can more safely undergo delayed reconstruction. Further investigation still must be done to discover a proper cutoff of BMI.
Other behavioral factors such as smoking, hypertension, and diabetes mellitus cause a negative impact on complication rates. Patients should be encouraged to cease smoking as vasoconstriction causes a deleterious effect on the mastectomy flaps and wound healing. Blood glucose levels should also be strictly controlled. Hypertension and especially poorly controlled hypertensive patients are at increased risk of developing a hematoma. Unfortunately, not enough data was available to assess the statistical significance of these risk factors in this essay.
The authors’ opinion is that patients previously submitted to radiotherapy or who will likely receive adjuvant radiotherapy should not be candidates for alloplastic immediate reconstruction. It should be offered delayed autologous reconstruction instead.
New trends favoring alloplastic reconstruction in these patients after improving the quality of flaps with lipofilling are beyond this article’s scope. Due to fenestrations in the ADM and permeability of the mastectomy pocket, the submuscular drain may not be necessary. Many centers are using only one drain. Reducing the number of drains might play a role in decreasing the rate of infection.
Regarding ADM use, and even though most infected/extruded implants in DTI reconstruction were associated with ADM13,14, there is not sufficient data for this fact to be statistically significant.
In conclusion, alloplastic reconstruction remains the gold standard in immediate breast reconstruction. It allows achieving aesthetically satisfying results that endure many years of the patient’s life. However, this is not without its limitations, especially when treating young women with long life expectancies. These women are expected to undergo multiple procedures throughout their life, such as implant replacement, and many will eventually develop capsular contracture.
Other complications might also arise, such as the breast implant-associated anaplastic large cell lymphoma (BIA-ALCL), a malignancy though very rare that is gaining the spotlight in plastic surgery conferences all over the world once was most certainly overlooked and underdiagnosed. These complications are part of the burden of carrying a breast implant for life.
Because of all this, it is essential to further invest in immediate autologous reconstruction and routinely offering this option to younger patients, especially with the state-of-the-art DIEP flap.
REFERENCES
1. Filip CL, Jecan CR, Raducu L, Neagu TP, Florescu IP. Immediate versus delayed breast reconstruction for postmastectomy patients. Controversies and solutions. Chirurgia (Bucur). 2017 Jul/Aug;112(4):378-86.
2. Gfrerer L, Mattos D, Mastroianni M, Weng QY, Ricci JA, Heath MP, et al. Assessment of patient factors, surgeons, and surgeon teams in immediate implant- based breast reconstruction outcomes. Plast Reconstr Surg. 2015 Feb;135(2):245e-52e.
3. Wilkins EG, Hamill JB, Kim HM, Kim JY, Greco RJ, Qi J, et al. Complications in postmastectomy breast reconstruction one-year outcomes of the mastectomy reconstruction outcomes consortium (MROC) Study. Ann Surg. 2018 Jan;267(1):164-70.
4. Berlin Nl, Tandon VJ, Qi J, Kim HM, Hamill JB, Momoh AO, et al. Hospital variations in clinical complications and patient-reported outcomes at 2 years after immediate breast reconstruction. Ann Surg. 2019 May;269(5):959-65.
5. Azouz V, Lopez S, Wagner DS. Surgeon-controlled comparison of direct-to-implant and 2-stage tissue expander-implant immediate breast reconstruction outcomes. Ann Plast Surg. 2017 Mar;80(3):212-6.
6. Rudolph M, Moore C, Pestana IA. Operative risk stratification in the obese female undergoing implant-based breast reconstruction. Breast J. 2019 Nov;25(6):1182-6. DOI: https://doi.org/10.1111/tbj.13434
7. Ilonzo N, Tsang A, Tsantes S, Estabrook A, Ma AMT. Breast reconstruction after mastectomy: a ten-year analysis of trends and immediate postoperative outcomes. Breast. 2017 Apr;32:7-12.
8. Azouz V, Lopez S, Wagner DS. Surgeon-controlled comparison of direct-to-implant and 2-stage tissue expander-implant immediate breast reconstruction outcomes. Ann Plast Surg. 2018 Mar;80(3):212-6.
9. Davila AA, Mioton LM, Chow G, Wang E, Merkow RP, Bilimoria KY, et al. Immediate two-stage tissue expander breast reconstruction compared with one-stage permanent implant breast reconstruction: a multi-institutional comparison of short-term complications. J Plast Surg Hand Surg. 2013 Oct;47(5):344-9.
10. Blacam C, Momoh AO, Colakoglu S, Slavin SA, Tobias AM, Lee BT. Cost analysis of implant-based breast reconstruction with acellular dermal matrix. Ann Plast Surg. 2012 Nov;69(5):516-20.
11. Gdalevitch P, Ho A, Genoway K, Alvrtsyan H, Bovill E, Lennox P, et al. Direct-to-implant single-stage immediate breast reconstruction with acellular dermal matrix: predictors of failure. Plast Reconstr Surg. 2014 Jun;133(6):738e-747e.
12. Colwell AS, Damjanovic B, Zahedi B, Medford-Davis L, Hertl C, Austen Junior WG. Retrospective review of 331 consecutive immediate single-stage implant reconstructions with acellular dermal matrix. Plast Reconstr Surg. 2011 Dec;128(6):1170-8.
13. Salzberg CA, Ashikari AY, Koch RM, Chabner-Thompson E. An 8-year experience of direct-to- implant immediate breast reconstruction using human acellular dermal matrix (AlloDerm). Plast Reconstr Surg. 2011 Feb;127(2):514-24.
14. Salzberg CA. Focus on technique: one-stage implant-based breast reconstruction. Plast Reconstr Surg. 2012;130(5 Suppl 2):95S-103S.
1. Hospital and University Center of Coimbra,
Coimbra, Portugal, Portugal.
JBF Analysis and/or data interpretation, Conception and design study, Conceptualization, Data Curation, Final manuscript approval, Methodology, Project Administration, Writing - Original Draft Preparation, Writing - Review & Editing.
RM Analysis and/or data interpretation, Writing - Review & Editing.
CD Writing - Review & Editing.
SS Analysis and/or data interpretation, Conceptualization, Formal Analysis, Investigation, Methodology, Writing - Original Draft Preparation.
Corresponding author: João Baltazar Ferreira, Rua Av Bissaya Barreto, Unidade Queimados, Blocos de Celas HUC, Coimbra, Portugal, Zip Code 3000-075, E-mail: joao_cbf@msn.com
Article received: February 21, 2021.
Article accepted: April 19, 2021.
Conflicts of interest: none.
Institution: Hospital and University Center of Coimbra, Coimbra, Portugal.









 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter