

Case Report - Year 2026 - Volume 41Issue 1
Hand Reimplantation: A Case Report in a BrazilianTertiary Hospital
Reimplante de mão: Um relato de caso em um hospital terciário
ABSTRACT
The hand plays a crucial role as an organ of communication and environmental interaction. Its absence causes irreversible deficits in social and professional life activities, even with the use of modern prostheses. Most victims of hand trauma in Brazil are male and economically active. Traumatic hand amputation requires skillful surgical treatment to achieve functional recovery and spare the amputated extremity. The medical team must have these goals in mind after saving the patient's life. Although aesthetics is within the treatment goals, one should prefer a functional, useful hand with pincer function. In this work, we report a case of hand replantation using a microsurgical technique at the Instituto Dr. José Frota, a tertiary hospital in Fortaleza, Ceará, Brazil.
Keywords: arm injuries; arteriovenous anastomosis; exercise therapy; finger phalanges; hand; hand injuries; median nerve; microsurgery; replantation; tendon injuries
RESUMO
A mão tem função importante como órgão de comunicação e de interação com o ambiente. Sua ausência causa déficit irreversível nas atividades da vida social e profissional, mesmo com o uso das próteses modernas. A maioria das vítimas de traumatismos na mão no Brasil é do sexo masculino e em plena idade produtiva. A amputação traumática de mão requer tratamento cirúrgico hábil para alcançar recuperação funcional e salvar a extremidade amputada. Este deve ser o objetivo da equipe médica, depois de resguardada a vida do paciente. Embora a estética esteja dentro dos objetivos de tratamento, deve-se priorizar uma mão funcional e útil, com função de pinça. Neste trabalho relatamos um caso em que foi utilizado a técnica microcirúrgica para realizar um reimplante de mão no hospital terciário Instituto Dr. José Frota em Fortaleza, Ceará, Brasil.
Palavras-chave: ferimento em braço; anastomose arteriovenosa; terapia por exercicio; dedos e falanges; mão; ferimento em mão; nervo mediano; microcirurgia; reimplante; ferimento em tendões
Introduction
In 1962, Malt performed the world’s first successful replan-tation in Boston and, in 1963, Ch’em reimplanted a forearm in Shanghai. The vessel’s diameter was greater than 2 milli-meters, and the suture threads were not appropriate. Experimental reports of limb replantation attempts date from the beginning of the last century. In Brazil, Ely et al. reported the first replantation in 1968, in Porto Alegre.1 The first hand replantation in Latin America took place in 1971, in São Paulo, by the plastic surgeon Marcus Castro Ferreira and his team.2 This same team also performed the first finger replantation on the continent, 2 years later. It was sensible that the hand came before the finger: the smaller the limb, the greater the difficulty of replantation.
The hand plays a crucial role as an organ of communica-tion and environmental interaction. Its absence causes irre-versible deficits, even with the use of modern prostheses, in social and professional life activities. Most hand trauma victims in Brazil are male and economically active. Traumatic hand amputation requires skillful surgical treatment to achieve functional recovery and spare the amputated ex-tremity. The medical team must have these goals in mind after saving the patient’s life. Although aesthetics is within the treatment objectives, one should prioritize a functional, useful hand with pincer function.3
Moreover, the physical and psychological sequelae result-ing from amputations can significantly impact patients’ quality of life, requiring medical and multidisciplinary inter-ventions to minimize damage and promote full recovery.
Such interventions entail substantial costs for treatment and rehabilitation. These costs have a significant global dimension, reflecting not only the financial resources direct-ed towards medical care, but also the social and economic burden related to the physical, emotional, and social con-sequences for amputee patients.
Therefore, it is crucial to analyze this replantation case at a referral hospital for a better understanding of the extent of the issue, identifying risk factors, and enhancing treatment strategies.
Objective
The present study aimed to report descriptively the technical approach and outcomes of a patient who underwent hand replantation.
Materials and Methods
This observational, descriptive, cross-sectional, analytical, and retrospective study used forms completed by hand replantation patients, findings from direct interviews, and active data retrieval from medical records in the database of the Instituto Doutor José Frota (IJF), a major tertiary hospital in Fortaleza, Ceará, Brazil.
Results
Case Report
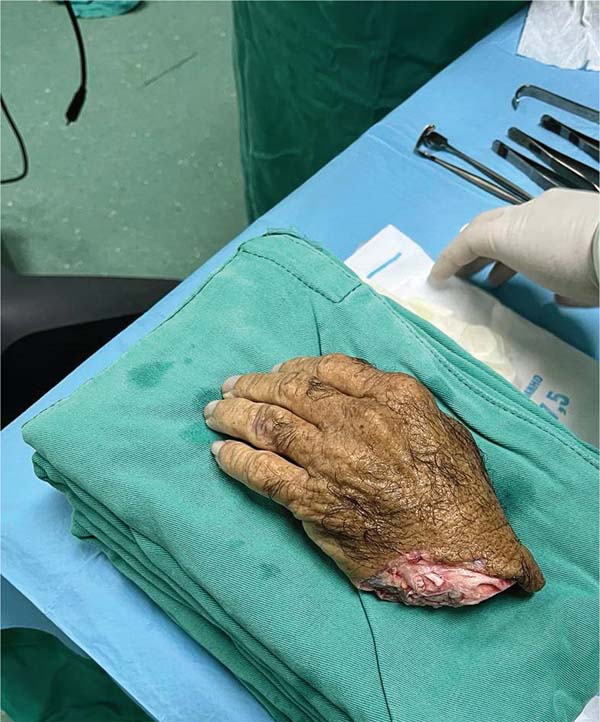
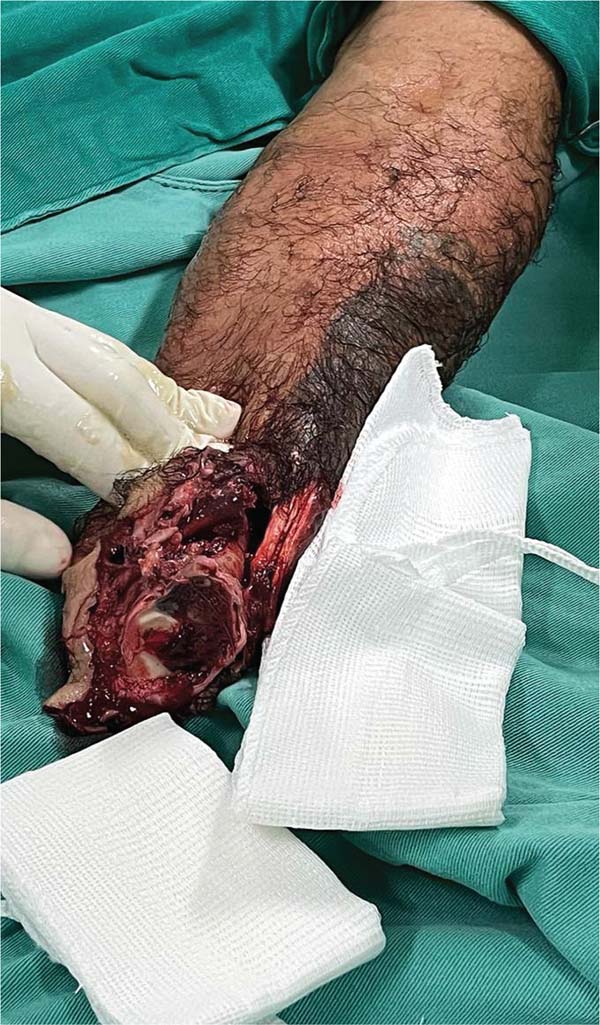
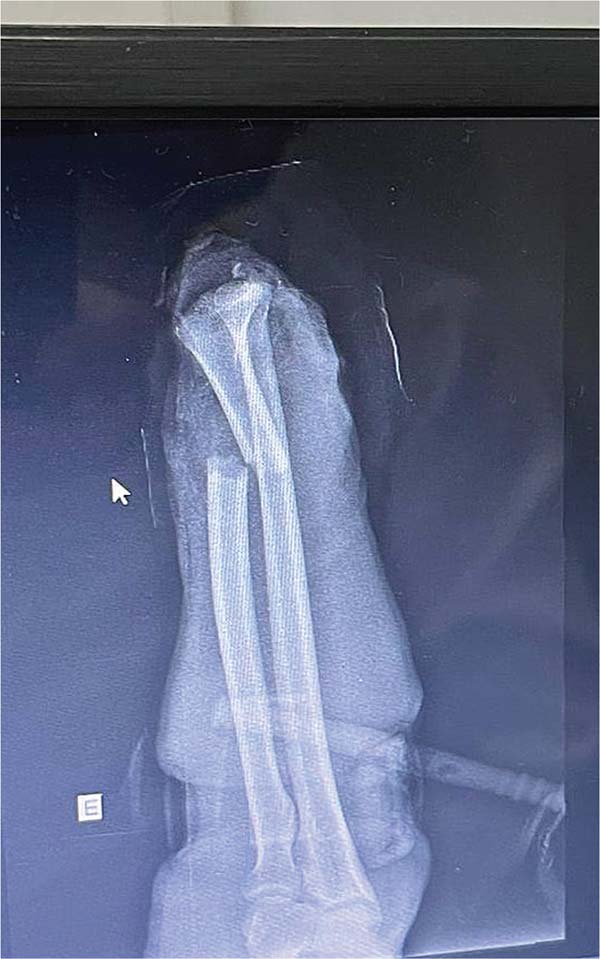
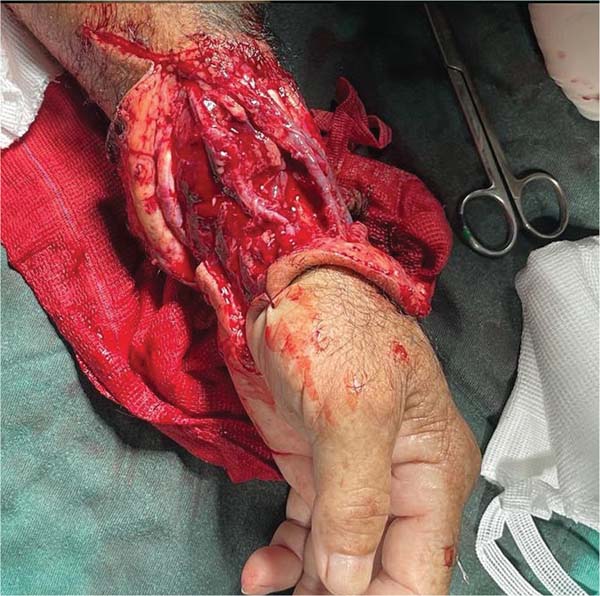
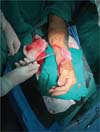
A 56-year-old patient (IPB), male, married, born and living in Fortaleza, was admitted to the hospital following an accident involving a saw in a butcher shop. He presented with a total amputation of his left hand at the wrist level with bone and tendon exposure. The patient arrived with a tourniquet on his left arm and his amputated hand in an ice-filled contain-er. He reported that the accident had occurred approximately 40 minutes before. On examination, he was stable but mod-erately pale due to significant blood loss, with no loss of consciousness, and a heart rate close to 110 bpm, indicating grade 2 hypovolemic shock. There were no signs of abrasions or trauma to other limbs (►Figs. 1-3).
The medical team must ask for the injury location and the time elapsed between the lesion and primary care (clean or contaminated wound).3 The recommended initial step is to wrap the wound (i.e., proximal stump of the amputated extremity) with a clean cloth or sterile compress, followed by local compression with a crepe bandage. The amputated segment should be thoroughly washed with 0.9% saline solution, wrapped in a clean compress, and placed in an ice-filled container. Cooling (4°C) increases the time until tissue damage from 3 to 6 hours under normal conditions to 12 to 24 hours. However, tissue damage may occur earlier depending on the amount of muscle tissue involved. The time between trauma and revascularization should not exceed 6 hours.
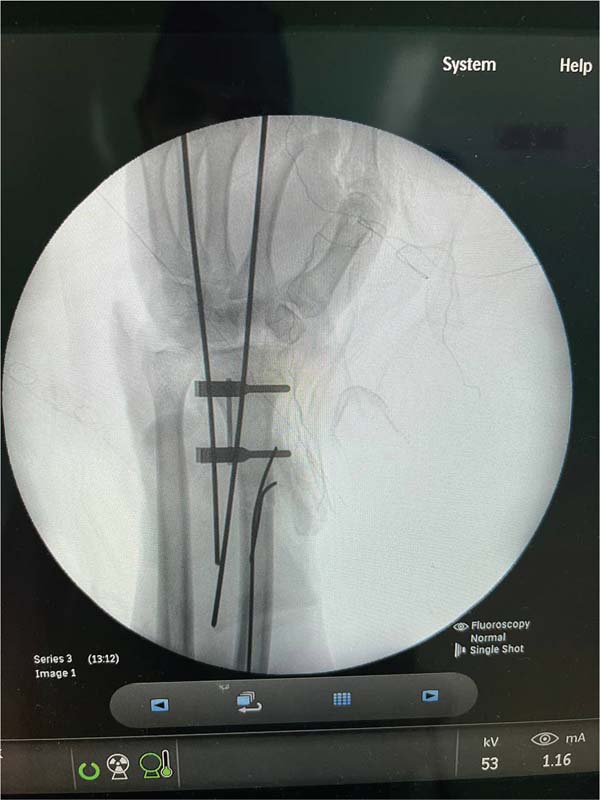
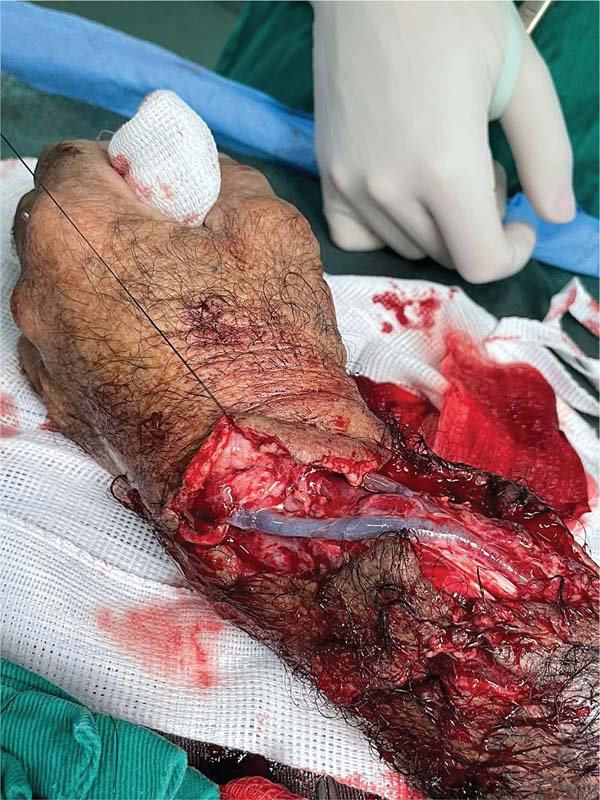
After initial measures according to the Advanced Trauma Life Support (ATLS) protocol, we performed the following surgical steps: vascular stump dissection with identification of the radial and ulnar arteries, and the ulnar and median nerves; heparinization of the blood vessels of the amputated extremity; bone fixation of the radius and wrist block with Kirschner wires; primary microvascular anastomoses of the radial and ulnar arteries and three dorsal veins; suture of the median and ulnar nerves under microscope guidance; and, finally, an en bloc flexor tenorrhaphy and skin grafting over the wound due to tissue loss (►Figs. 4-7).4
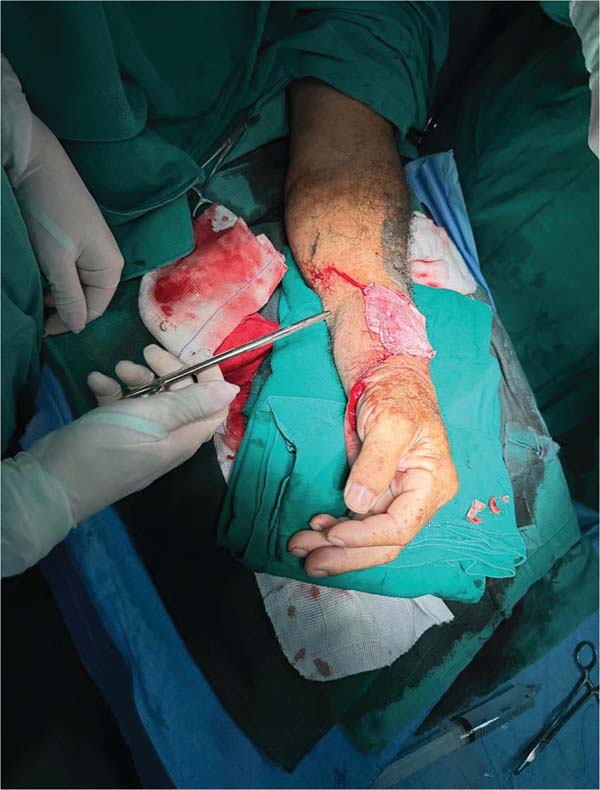
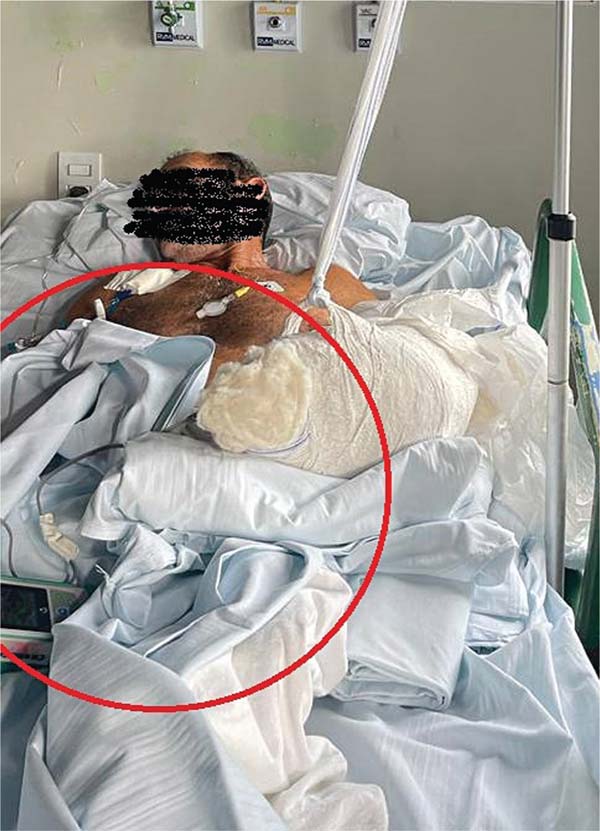
The patient presented with good hand perfusion and required temporary immobilization due to the fragility of the anastomoses. Pulse oximetry was monitored during hospitalization. The patient was cooperative throughout the admission, leading to a better outcome. After 10 days under observation, the patient was discharged from the hospital with instructions for care and outpatient follow-up (►Fig. 8).
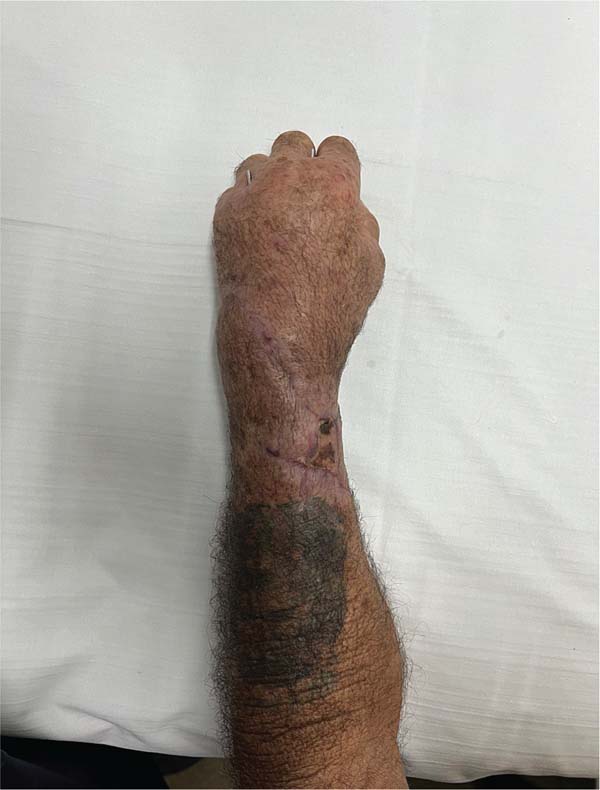
During a follow-up outpatient visit, the patient reported significant difficulty in starting physical therapy through the public healthcare system, which delayed rehabilitation. The patient was satisfied with not losing the limb, but he was experiencing difficulty in mobilization even during simple activities (►Figs. 9,10).
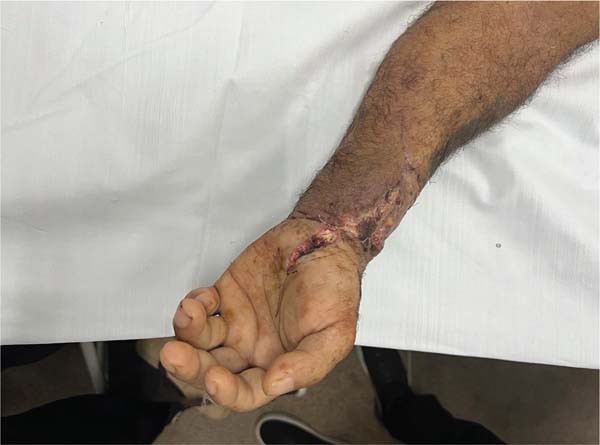
After 6 months, the patient underwent a tendon transfer, involving the removal of a segment of the flexor carpi radialis to reconstruct the extensor carpi ulnaris, potentially allow-ing better wrist flexion and range of motion. During outpa-tient follow-up, the range of motion improved, but not enough to support full movements due to inadequate physi-cal therapy assistance (►Figs. 11,12).
Discussion
Several systemic challenges hinder the management of hand replantation cases in Brazil, starting with the logistical challenges of time and distance required for the replantation, the window of opportunity is small, with rapid transport and highly specialized hospital infrastructure often lacking out-side larger centers. The unequal distribution of microsur-geons and multidisciplinary teams, restricted access to referral centers, and the lack of well-defined protocols for triage and transfer only exacerbate this problem.
Economic and political issues further complicate this matter. The high cost of materials, staff, and the lengthy rehabilitation required are often not covered by public budgets or supplementary health insurance plans. As such, many services opt for cheap, quick solutions, like amputation and subsequent prosthesis.
In the United States, the trend of performing fewer replantation procedures in adult patients has also gained momentum. The current focus on cost-effectiveness and postoperative quality of life has led to a more pragmatic paradigm: in many cases, adaptation with a modern pros-thesis is considered to provide functional and psychological outcomes as good as or even better than replantation, especially when the latter is incomplete, has a poor indica-tion, or when rehabilitation is deemed inadequate.
However, this trend requires careful interpretation in countries such as Brazil, where access to quality prosthetics and rehabilitation remains scarce. There is a risk of adopting an economic logic from more developed countries without providing proper treatment for the local population.
Conclusion
Even over 50 years after the first case, we still face difficulties in replantation procedures due to their delicate nature, the unavailability of an emergency microsurgery service due to a lack of specialized personnel capable of providing salvage surgery for a traumatized limb, and the absence of multidis-ciplinary support with physical therapy and psychological support during limb rehabilitation. These are key barriers to successful treatment. With no proper rehabilitation, even the best surgical technique becomes an empty promise.
REFERENCES
1. Ely JB, Pereira Filho OJ, Mendes PRS, Lee KH, Vasconcellos ZAA. Evolução e avaliação de 2 pacientes submetidos a reimplante total de membro superior. um de Porto Alegre em 1968 (primeiro reimplante do Brasil - meio século) e outro de Bruxelas em 1980. Rev Bras Cir Plást 2018;33(Suppl 1):133-135. Doi: 10.5935/2177-1235.2018RBCP0070
2. Costa CA, Cabral PHO, Pinto PL, Pinheiro MJC Júnior, Santos NJN, Birolini D. Initial experience with hand replantation after trau-matic amputation in a nonspecialized center. J Vasc Bras 2006;5 (04):321-324
3. Monir JG, Cooke H, Jagiella-Lodise O, McQuillan T, Wagner E, Zelenski NA. Trends in Digit Replantation and Revision Amputa-tion in the United States From 2009 to 2019. J Hand Surg Glob Online 2024;6(06):855-860. Doi: 10.1016/j.jhsg.2024.07.012
4. Silva JB, Ramos RM, Muñiz AR, Ferdinando MP. Trauma da mão. Parte 2. Rev AMRIGS 2014;58:291-301
1. Plastic Surgery Service, Hospital Instituto Doutor José Frota, Fortaleza, CE, Brazil
Address for correspondence David Christian Rodrigues Pereira, Rua Costa Sousa 100, Ap 802, Torre 2, Bairro Benfica, Fortaleza, CE, Brazil, CEP: 60020-300 (e-mail: dayvid0309@hotmail.com).
Article received: July 21, 2024.
Article accepted: August 26, 2025.
Editor-in-Chief: Dov Charles Goldenberg.
Conflict of Interests
The authors have no conflict of interests to declare.






 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter