

Articles - Year 2002 - Volume 17 -
Aesthetic Plastic Surgery in Patients Infected with the Human Immunodeficiency Virus (HIV) - Is There Consensus?
Cirurgia Plástica Estética em portadores do Vírus da Imunodeficiência Humana (HIV) - existe consenso?
ABSTRACT
HIV-positive patients today are using antiretroviral and other medications capable of preventing opportunistic infections so it may well take 15 years before the disease develops. Better chances of surviving free of clinical disease and longer survival have led to behavioral changes. As patients become more aware and are better informed in relation to HIV they seek to lead a "near normal" life. Even HIV-positive patients with imminent signs of disease are among those seeking plastic surgeons because they wish to look younger or fix physical flaws. We searched the literature for recent studies and discussions of this issue, in statistical and epidemiological data, or details of perisurgical precautions being taken against HIV contamination. We also conducted a survey of surgeons' approaches to HIV patients among members of the Brazilian Society of Plastic Surgery in Rio de Janeiro.
Keywords: Plastic surgery; aesthetic; HIV; AIDS; occupational exposure
RESUMO
Atualmente, um portador do HIV, em uso de anti-retrovirais e outras medicações capazes de prevenir infecções oportunistas, pode passar 15 anos até desenvolver a doença. A melhora na sobrevida desses pacientes, sem doença clínica, proporciona uma mudança comportamental e os torna mais conscientes, mais bem esclarecidos sobre a enfermidade, em busca de uma vida "próxima do normal". Os cirurgiões plásticos se deparam com pacientes soropositivos, ou mesmo com sinais iminentes de doença, que manifestam o desejo de rejuvenescer ou melhorar imperfeições físicas. Neste trabalho, procura-se identificar estudos e discussões recentes sobre o tema na literatura, dados estatísticos e epidemiológicos, além de cuidados na prevenção da contaminação pelo HIV no peroperatório. Foi realizada uma enquete junto a cirurgiões da Sociedade Brasileira de Cirurgia Plástica - Regional do Rio de Janeiro - para avaliar a conduta desses profissionais diante desses pacientes.
Palavras-chave: Cirurgia plástica; estética; HIV; SIDA; exposição ocupacional
In 1993, the Center for Disease Control and Prevention (CDC), in the United States, reviewed concepts and definitions in relation to Acquired Immunodeficiency Syndrome (AIDS). Certain evidential factors were taken as the most likely and the most basic pointers in diagnostic investigation. Certain secondary infections occur so infrequently, or are so rare in the non-immnnodepressed population, that they were included in CDC's classification for the diagnosis of HIV/AIDS(1). One of the consequences of this review was that HIV-positive patients could be diagnosed earlier in the course of the disease. In fact, the efforts to identify patients faster and more accurately have been reflected in slower progression from becoming HIV-positive to showing AIDS symptoms. Elaborate use of antiretroviral and other medications capable of preventing opportunistic infections, added to improved diagnostic and epidemiological identification, has changed the approach to AIDS in recent years.
HIV-positive patients may now remain symptom-free for several years, and the period from exposure to development of the disease may last up to 15 years. During the different phases of HIV infection, patients may have to undergo several surgical procedures, ranging from lymphnode biopsies to extensive tumorectomies. Almost all these interventions are due to unquestionable diagnostic necessity or are aimed at guiding treatment, and they are often emergencies.
The noticeable improvements in life expectation of HIV-positive patients, free from clinical diseases, have led them to change their behavior. The prospects for living longer and enjoying far better quality of life have clearly improved greatly over the last few years. So patients have become more aware and better informed, do not underestimate their limits, and aspire to a life that is objectively "near-normal".
There are some impressive reports to be found in the literature. Last year, 207 in every 100,000 people in Brazil were operated on for cosmetic reasons. The patients seeking this kind of surgery were very heterogeneous in composition. Plastic surgeons are being sought by HIV-positive patients, even when thev have imminent signs of the disease, who wish to look vounger or be treated for physical imperfections.
Bearing that scenario in mind, the objective of this paper is to bring together recent statistical and epidemiological data found in the literature, and survey the prevention of HIV contamination, which is currently a controversial issue for plastic surgery clinics. Should HIV-positive patients be operated for aesthetic purposes? What are the implications of the surgery? Is there an occupational risk for surgeons and theatet personnel? Lastly, we conducted an opinion survey among surgeons belonging to the Brazilian Society of Plastic Surgery in Rio de Janeiro.
MATERIALS AND METHODS
A computerized search of the literature published in the last 15 years was conducted, using MEDLINE, LILACS, and the Internet. Additional related materials were collected from newspaper and magazine articles, presentations at scientific conferences, and websites.
A simple and practical questionnaire, with short questions and objective answers, was given to surgeons belonging to the Brazilian Society of Plastic Surgery in Rio de Janeiro, as shown in the charts bellow.
RESULTS
There are extremely large numbers of HIV-positive people around the world. As this complex illness develops, surgeons are treating increasing numbers of patients with surgical problems, both related to the infection by HIV and otherwise(2). Generalized lymphadenopathy is a common example that is frequently found among the symptoms. Lvmphnode biopsies are done every day in general hospitals and provide relevant diagnostic information. Patients with thrombocytopenic purpura associated with immune deficiency do not respond to corticotherapy as well as HIV-negative patients with idiopathic thrombocytopenic purpura(2). As a result, these patients have to undergo splenectomy in order to control the thrombocytopenia. Anorectal procedures are the most frequent surgeries carried out on HIV-infected male homosexual patients(2).
So far, no prospective study has been capable of assessing surgical morbidity and mortality and comparing HIV-positive and HIV-negative patients(2). Generally speaking, the papers published show the benefits of different surgical treatments for HIV-infected patients and do not report higher incidence of complications in wounds(3-5). Good clinical records, physical examinations, and laboratory tests provide appropriate information about the general status of patients. An HIV-positive person with good muscular mass probably runs the same risk of complications in healing of wounds as an HIV-negative person(2). Some studies have attempted to relate CD4 counts with complications in healing of wounds and sepsis but the conclusions are controversial. However, a study carried out in Detroit, Michigan, USA, noted that major abdominal surgery patients with CD4 counts of under 200/ml presented more perioperative mortality (38%) than patients with relatively higher CD4. counts(6).
The risk of HIV transmission after a lesion by an injection needle contaminated with HIV infected blood is 0.3%(7-9). However, the risk after a suture needle stick lesion is unknown. The risk of transmission increases depending on certain circumstances:
• 5 times, if blood is visible on the needle or if the procedure involves injecting an artery or vein;
• 6 times, if the patient has advanced AIDS (and presumably a high viral load).
• 16 times, if the injection-needle causes a deep wound in the soft tissue;
Although more fear is expressed in relation to procedures in HIV-positive patients, the risk of occupational contamination from hepatitis C or R is 10 times and 100 times greater, respectively(10,11).
Tokars et al. (12) have shown that percutaneous lesions with needles and blades during surgical procedures occurred regularly in 6.9% of the 1,382 surgeries evaluated.
The risk of HIV transmission is 80 times less in healthcare professionals with needle-stick injuries after prophylactic administration of zidovudine(13).
A large-scale survey of surgical patients showed that 16.7 % of all samples sent for transfusion screening or cross-match testing presented serologic evidence of viral infection (HIV, HBV, HCV), of which 5.6% were HIV-positive(14). It is known, therefore, that the greater the seroprevalence among patients and the greater the number of needle-stick injuries, the greater the risk of occupational transmission of HIV.
Among the preventive strategies for healthcare professionals, the following are worth mentioning:
1. Precautions in infection control: blood must be treated as a toxic substance(8). The contact of patient blood with the skin and mucous tissues of healthcare professionals is unacceptable. Protective goggles, masks, impermeable gowns and shoe-covers are basic accessories. Double gloving reduces the risk of exposure related to defects by approximately 17%(8).
2. Changes in surgical techniques; reducing the incidence of intraoperative occupational exposure requires care and attention to details. Avoiding passing pointed and sharp instruments from hand to hand, positioning them appropriately on the materials table, and the use of staplers instead of suture in the areas of difficult manipulation are methods that reduce the chances of accidents, Some surgeons use their own fingers to protect tissues or organs under the surgical level. This practice is obsolete and extremely dangerous. However, surgical techniques vary from one surgeon to another and are used so as to obtain the best results for each patient individually.
3. Preoperative anti-HIV testing: in spite of the endless discussions about this issue, even regarding the possibility of discrimination in the treatment of HIV-positive patients, current studies show that prophylaxis and therapy of opportunistic infections benefit symptom-free or minimally symptomatic patients. Therefore, the arguments for preoperative testing prevail over any other argument against it. In fact, prior knowledge from testing provides little protection for theater personnel since it does not reveal the existence of other infectious agents (hepatitis viruses, for example). In principle, all patients should be treated as if they were infected, so test results would not change behavior in the operating room(2).
4. Non-surgical treatment: when planning treatment, surgeons should weigh risks in relation to the potential benefit of surgery. If they conclude and believe that the procedure will have a positive effect on the life of the patient, they should provide it as planned.
Out of the 75 plastic surgeons who answered the questionnaire, 45 had been practicing in the specialty for more than 10 years. The results of the survey are shown in figures 1 to 5.
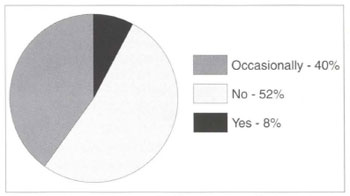
Fig. 1 - Do you request anti-HIV test as part of your preoperative routine?
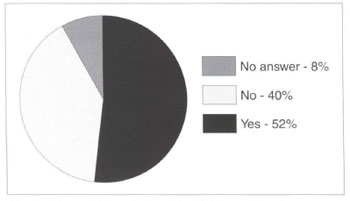
Fig. 2 - Has an HIV-positive patient (without disease) ever come to see you?
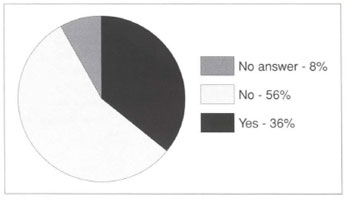
Fig. 3 - Are HIV-positive patients at greater risk of post-operative infection?
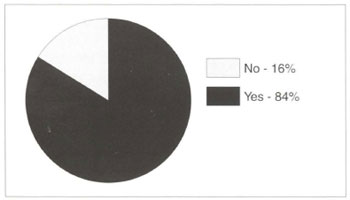
Kig. 4 - Should HIV-positive patients undergo aesthetic surgery?
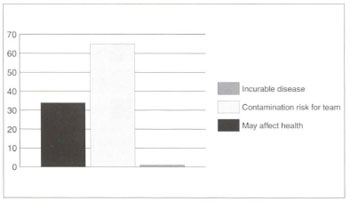
Fig. 5 - Aesthetic surgery should not he done because...
DISCUSSION AND CONCLUSION
In September 1991, the Annual Meeting of the American Society of Plastic and Reconstructive Surgeons came to following decision:
"Discrimination against HIV-infected patients requesting elective plastic surgery cannot be supported... Patients denied procedures based on HIV immunological tests will be legally defended in accusations of discrimination against the physician"(16,17).
Many members of the society questioned this position and expressed dissatisfaction. Smith(18) discussed the ethics and morality of the issue and argued that this "unnecessary procedure" threatened the safety of surgical personnel, as well as that of surgeons and their families, .Petro(19) drew attention to the relevance of aesthetic plastic surgery in promoting well-being and contributing to individual success in our society. Therefore plastic surgeons boost self-esteem and improve quality of life, which places it in the same situation as other specialties. Other arguments raised included the survival of HIV-positive patients and the position of specialists from other areas on the issue.
In Brazil, the Ministry of Health, state health departments and the Federal and State Boards of Medicine have posed legislation and drafted several opinions and resolutions on AIDS. Some of the highlights refer to diagnostic criteria(20,21,22), biosafery standards, confidentiality, and comprehensive care for HIV-positive patients as moral imperatives for medical practice and healthcare institutions(21,22). They also address issues related to the disease in pregnant women and newborns(23). However, there were no statements addressing the issue of aesthetic plastic surgery and HIV/AIDS.
It is not the intention of this paper to determine a consensus as to how aesthetic plastic surgery should approach the issue of HIV-positive patients. The aim here is to discuss the issue openly and objectively so that it becomes easier to find a position in line with medical ethics and professional principles.
The survey, in spite of its simplicity and sampling, revealed some very interesting points. Anti-HIV testing appears not to have influenced the conduct of the plastic surgeons interviewed, since only a small percentage include it in routine preoperative evaluation. Nevertheless, many surgeons do tend to test on the basis of clinical-epidemiological evidence observed during the initial evaluation of candidates for surgery. Another finding was that significant numbers of HIV-positive patients are going to plastic surgery clinics. A substantial percentage of surgeons in this brief study have already met with this situation, and the great majority agrees that these patients may undergo aesthetic surgery. On the basis of the literature referred to above, everyday experience perhaps suggests that the incidence of postoperative complications in HIV-positive patients does not differ from that of patients described as "normal". Slightly over half the physicians interviewed do not believe there is a greater risk, of postoperative infection.
The findings in the literature show the complexity of the issue. AIDS is still a feared disease and has an inexorable course. It tends to become chronic and remains incurable.
Occupational risk statistics are no more than estimates. The data are still tentative, mainly because of the very diverse variables. This srudy did not find any statistical data specifically for patients undergoing plastic surgery.
HIV testing (with consent) may benefit patients more than surgical personnel, because, as described above, it does not reveal the presence of other infectious agents that pose greater risk of surgical contamination. As to prophylaxis for surgeons, the most sensible conclusion is to follow prevention strategies and treat all patients as potentially infected, with HIV testing if they present risk factors for infection, or if they spontaneously say they are favorable to testing. HIV patients may be operated for aesthetic purposes; however, they should undergo extensive multidisciplinary evaluation. Crucially, patients should be in good clinical condition; there should be a surgical plan and expectations should be in line with the real potential.
REFERENCES
1. Lewin-Smith MR, Klassen MK, Frankel SS, Nelson AM. Pathology of human immunodeficiency virus infection: infectious conditions. Ann Diagn Pathol. 1998;2(3):181-94.
2. Schecter, W. Surgery in Patients with HIV. From: URL: http://www.hivinsite.com - University of California, San Francisco; 1997.
3. Hewitt WR, Sokol TP, Fleishner PR. Should HIV status alter indications for hemorrhoidectomy? Dis Colon Rectum. 1996;39:615-8.
4. Burke EC, Orloff SL, Freise CE, et al. Wound healing after anorectal surgery in HIV-infected patients. Arch Surg. 1991;126:1267-70.
5. Buehrer JL, Wever DJ, Meyer AA, et al. Wound infection rates after invasive procedures in HIV-1 seropositive versus HIV-1 seronegative hemophiliacs. Ann Surg. 1990;211:492-8.
6. Albaran RG. CD4 cell counts predict abdominal surgery outcome in HIV-positive patients. Arch Surg. 1998;133:626-31.
7. Henderson DK, Saah AJ, Zak BJ, et al. Risk of nosocomial infection with human T-cell lymphotropic virus (Type III/lymphadenopathy-associated virus) in a large cohort of intensively exposed health care workers. Ann Intern Med. 1987;104:644-7.
8. Gerberding JL, Little C, Tarkington A, et al. Risk of exposure of surgical personnel to patients blood during surgery at San Francisco General Hospital. N Engl J Med. 1990;322:1788-93.
9. Centers For Disease Control: Update: Acquired immunodeficiency syndrome and human immunodeficiency virus infection among health-care workers. MMWR. 1988;37:229-39.
10. URL: http://www.riscobiologico.org/
11. Updated U.S. Public Health Service Guidelines for the Management of Occupational Exposures to HBV, HCV, and HIV and Recommendations for Postexposure Prophylaxis. June 29, 2001 / 50(RR11); 1-42.
12. Tokars JL, Bell DM, et al. Percutaneous injuries during surgical procedures. JAMA. 1992;267(21):2899-904.
13. Centers For Disease Control: Case control study of HIV seroconversion in health care workers after percutaneous exposure to HIV infected blood - France, United Kingdom, and the United States. MMWR. 1995;44:929-33.
14. Montecalvo MA, Lee MS, De Palma H, et al. Seroprevalence of human immunodeficiency virus-1, hepatitis B virus, in a Brooklyn maintenance hemodialysis unit: Preliminary observations. ASAIO J. 1995;34:194-5.
15. Schecter W. HIV and Surgery. Occupational risk and responsibility. San Francisco Med. 1990;63:14-6.
16. Board of Directors of the American Society of Plastic and Reconstructive Surgeons. Plast Surg News. 1992; Janeiro, p.3.
17. Goldwyn RM. AIDS, Aesthetic Surgery, and the Plastic Surgeon. Plast Reconstr Surg. 1992;90(6):1061-4.
18. Smith C. AIDS policy should reflect conviction of membership. Plast Surg News. 1992; March.
19. Petro J. Reply. Plast Surg News. 1992; March.
20. Parecer CFM 10/1987.
21. Resolução CREMERJ 35/1991.
22. Resolução CFM 1359/1992.
23. Parecer CFM 11/1992.
I. Graduate student at the Carlos Chagas Medical Post-Graduation Institute, Resident Member of the Brazilian Society of Plastic Surgery.
II. Assistant professor. Senior Member of the Brazilian Society of Plastic Surgery.
III. Head professor. Senior Member of the Brazilian Society of Plastic Surgery and Academia Nacional dc Medicina.
Ivo Pitanguy Study Center - Santa Casa de Misericórdia do Rio de Janeiro - Ward 38 - Professor Ivo Pitanguy's Plastic Surgery Service - Pontifícia Universidade Católica do Rio de Janeiro and Carlos Chagas Medical Post-Graduation Institute.
Address for correspondence:
Richard Robadey, MD
R. Dona Mariana, 65
22280-020 - Rio de Janeiro - RJ - Brazil
Phone: (55 21) 2537-5812
e-mail: ceip@visualnet.com.br


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter