

Special Article - Year 2011 - Volume 26 -
Skin substitutes: current concepts and a new classification system
Substitutos cutâneos: conceitos atuais e proposta de classificação
ABSTRACT
Complex wounds are characterized by complete loss of cutaneous cover. The most common plastic surgery technique is the autogenous skin graft; however, the amount of material available from donor areas is often limited. The development of synthetic or biological products as skin substitutes is therefore an area of interest. The present study aimed to classify the different types of skin substitutes available based on three criteria: the skin layer to be replaced, which can be categorized into epidermal (E), dermal (D), and dermal-epidermal composites (C); the durability in the wound bed, which can be temporary (T) or permanent (P); and the origin of the material, subdivided into biological (b), biosynthetic (bs), and synthetic (s).
Keywords: Tissue engineering. Cells, cultured. Skin, artificial.
RESUMO
Feridas complexas podem resultar na perda completa do revestimento cutâneo. A solução consagrada pela cirurgia plástica é a enxertia de pele autógena, porém há casos em que ocorre escassez de área doadora cutânea, um problema ainda não totalmente solucionado. Assim, atualmente há muito interesse por materiais sintéticos ou biológicos que possam ser utilizados como substitutos cutâneos. O objetivo deste estudo foi introduzir uma forma mais didática de agrupar diferentes tipos de substitutos cutâneos. Acreditamos que esses produtos podem ser classificados de forma mais abrangente se forem divididos segundo três critérios: camada substituída da pele, subdivididos em epidérmicos (E), dérmicos (D) e compostos dermoepidérmicos (C); duração no leito da ferida, subdivididos em temporários (T) e permanentes (P); e origem do material constituinte, subdivididos em biológicos (b), biossintéticos (bs) e sintéticos (s).
Palavras-chave: Engenharia tecidual. Células cultivadas. Pele artificial.
The complete loss of cutaneous cover can occur as a result of different conditions including burns, trauma, infections, autoimmune diseases, and complex wounds1. The loss of the cutaneous barrier increases the risk of infection, water loss, and hypothermia, which increases morbidity, the cost and length of hospitalization and in some cases, can result in death. The most commonly used plastic surgery technique is the allogeneic skin graft. However, the amount of donor area skin is often limited. The development of synthetic or biological products as skin substitutes is therefore of interest2.
One of the current options for the treatment of major skin losses is the use of skin substitutes, which can be of synthetic (generated by tissue engineering) or of human origin, such as allografts (derived from cadaver skin) and xenografts (derived from animal skin). The selection of appropriate skin substitutes is determined by the type, size, and depth of the wound as well as by comorbidities, patient preference, and the experience of the surgeon.
The allogeneic skin graft can be used to assess the suitability of the recipient bed. A good integration of this graft is indicative of a greater chance of successful autografting and a lower risk of autogenous tissue loss. This fact may be especially important in severe burns or in extensive trauma3.
The first attempt to produce a skin substitute from cultured epidermal cells was described in 1974 by Rheinwald and Green4, who cultured a small fragment of healthy skin until a sufficient keratinocyte lamina was produced for wound coverage. Although the concept of "producing skin" is technologically innovative, there are disadvantages to the use of this procedure such as a grafting delay of approximately 3 to 4 weeks (time required for epithelium development), fragility, lower resistance to infection, and a greater risk of graft loss. The success of this type of graft depends on the presence of remaining or transported dermal elements on the wound bed, and these factors have motivated new research efforts to develop skin substitutes2.
Skin substitutes are a heterogeneous group of biological and/or synthetic elements that enable the temporary or permanent occlusion of wounds. Although dermal substitutes can vary from skin xenografts or allografts to a combination of autologous keratinocytes over the dermal matrix, their common objective is to achieve the greatest possible similarity with the patient's skin5,6.
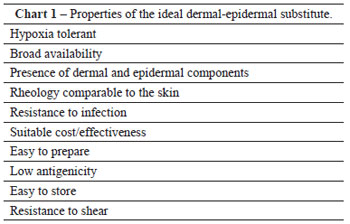
The ideal skin substitute should have properties comparable to those of human skin, as described in Chart 1.
An increased demand for skin substitutes brought about the need for suitable storage methods and a concern about preserving tissue quality. This led to the development of methods for the preservation of skin, such as cryopreservation, which aims to maintain the viability of the cell and the tissue architecture, and exposure to high concentrations of glycerol, which generates tissue with non-viable cells and intact protein structure7. The use of preservatives also reduces the antigenic load of the material. Although this effect is mainly associated with high concentration glycerol preservation, it is also possible to achieve a reduction in antigenicity with cryopreservation, which decreases the immunological response generated as a consequence of tissue transplantation8.
Several skin substitutes are currently available for a variety of applications, which enables the choice of a suitable substitute for each clinical application based on their advantages and disadvantages.
Although there are several classifications for skin substitutes9,10 and a recent review of this subject by Lazic and Falanga11, the most accepted classification is the one proposed by Balasubramani et al.12, in 2001, and modified by Kumar13, in 2008, which divides skin substitutes into class I, class II, and class III.
Class I - Temporary and Impervious Dressing Materials
Class I skin substitutes function as an epidermal barrier and despite lacking cell components, they perform some of the functions of this skin layer. They are often temporary and impervious, and function as a mechanical barrier against bacteria and to prevent water loss. This class includes:
a) Single layer materials:
biological products - amniotic membrane14; synthetic materials - membrane or synthetic polymer films (Opsite®, Hydrofilm®, Tegaderm®); biosynthetic (Nexfill® - Fibrocel); biocellulose layers and Veloderm®; biocellulose layers derived from sugar cane, foam, or polymeric spray (simple or silver Mepilex®, Mepilex Ag®, indicated for treatment of partial skin lesions).
b) Double layer materials produced by tissue engineering:
Transcyte® - semi-impermeable substitute composed of nylon mesh coated with porcine collagen with nonviable neonatal foreskin fibroblasts. These cells proliferate and synthesize matrix proteins (fibronectin, type I collagen, tenascin, proteoglycans and glycosaminoglycans) and growth factors. Their use enables the patient's epithelial cells to migrate to the wound15.
Class II - Single Layer Durable Skin Substitutes
a) Epidermal substitutes:
EpiDex® - epidermal substitute generated by autologous keratinocytes cultured from scalp hair follicles. Approximately 50 to 100 strands of hair, including the root, are collected from the patient's scalp, often from the supra-auricular region, and sent to the laboratory for cell culture. Pluripotent stem cells differentiate into keratinocytes that are grown in discs measuring 1 cm in diameter and reinforced with a silicone membrane, which are then grafted onto the wound bed16,17.
b) Dermal substitutes, which are composed of a substance similar to the dermis with processed skin or manufactured as dermal collagen matrix and other matrix proteins:
Swine collagen membranes: 1. OASIS Wound Matrix® is a dermal regeneration matrix derived from swine jejunum submucosa18,19 processed for removal of cell components, leaving a structure composed of glycosaminoglycans, fibronectin, proteoglycans, and growth factors. It is commonly used in lower limb wound treatment. It can be stored at room temperature20.
2. Permacol®, which is a derivative of porcine dermis collagen and elastin, is an acellular matrix that is non-alergenic21,22 and similar to the concept of the AlloDerm®3 allograft.Dermal matrices of bovine origin: 1. Matriderm® is composed of extracellular proteins (collagen and elastin) and is used for the treatment of full thickness burns in association with skin grafting23.
2. PriMatrix® is an acellular dermal extracellular matrix composed of extracellular proteins and collagen of types I and III. It is recommended for the coverage of complex wounds.Dermal matrices of human origin: 1. Alloderm® is an acellular dermal matrix with natural biological components derived from human cadaver skin. These grafts are cryopreserved, lyophilized, and glycerated for complete removal of cells, as well as removal of antigenic materials and pathogenic microorganisms24.
Class III - Composite Skin Substitutes
a) Human skin substitutes:
Allogeneic skin grafts - Gibson and Medawar25 described the distinction between the integration of autografts and allografts, defining the concept of immune rejection. Allografts are used at cool temperatures and remain in the lesion until their rejection. This results in an initial clinical improvement due to the simple occlusion of the wound. As long as the tissue is not recognized as foreign by the recipient's immune system, allografts act as autogens, triggering revascularization and signaling to the underlying bed regarding the wound occlusion. This decreases both inflammatory and vascular responses (granulation tissue), which are typical of wounds undergoing second intention healing. The improvement in blood supply increases the efficiency of macrophages and enhances the digestion of eventual pathogens present in the region26. However, the process of rejection is associated with local alterations such as edema and a decline in the quality of the granulation tissue, as well as systemic changes such as fever, irritation, and anorexia. To reduce the risk of deleterious immunological effects, allogeneic skin should only be used as a biological dressing, and skin replacements are required every five days (always anticipating the beginning of the rejection process)26. Allogeneic skin grafts prepared with high concentration glycerol result in the disappearance of cellular components (immunogen), which enable this skin to act as a dermal matrix.
b) Produced by tissue engineering:
Integra® is a synthetic skin substitute that is acellular and bilaminar. It was developed by Burke et al.27as a dermal analogue composed of bovine matrix collagen and chondroitin-6-sulphate recovered by a thin layer of silastic (epidermal analogue), which controls the loss of fluids and reduces bacterial invasion. The dermal matrix allows the movement of fibroblasts and capillaries from the recipient bed, thus stimulating repair with a dermal-equivalent structure. Gradually, the collagen is reabsorbed and structured into a new matrix within 3 to 6 weeks. After that, the silastic lamina can be removed. Integra® is mainly used for the coverage of deep wounds in full or partial thickness burns with insufficient donor material. Other possible indications are the reconstruction of tissues after excision of post-burn scarring contractures, chronic ulcers, and traumatic wounds27. The main advantages of this material are that it provides immediate coverage of large and extensive post-scarectomy areas, its availability, and that it reduces morbidity in donor areas due to the use of thinner grafts. In addition, it reduces the formation of hypertrophic scars (as it inhibits the inflammatory response), and provides better functional outcomes in joints and extremities. This material is also associated with good results because it forms a more elastic tissue when compared to the exclusive use of skin grafts28. The main disadvantages of this material are its high cost, the requirement of proper training for its correct use, and a high risk of the development of hematoma or seroma, which causes the loss of the component when applied immediately after debridement5. Biobrane® is a biosynthetic skin substitute composed of a bilaminated membrane formed by nylon mesh filled with type I porcine collagen (dermal analogue) and covered by a thin lamina of silicone (epidermal analogue). It has small pores that allow the drainage of the transudate, and is considered a semi-impermeable substitute. This material enables fibroblasts and capillaries to invade the wound and repair the dermal defect. Reepithelialization is possible due to the presence of keratinocytes at the wound's edge5. Its major indications are for the treatment of superficial and medium clean burns of partial thickness that are not caused by chemicals or petroleum-based products, the temporary coverage of donor areas in partial skin grafts, and the protection of autogenous mesh grafts29.
Within the concept of tissue engineering, an alternative for the treatment of complex wounds is the association of skin substitutes with keratinocytes in culture:
Orcel®, which contains live human cells, is a dual cellular matrix layer in which epidermal keratinocytes and human dermal fibroblasts are cultivated in two separate layers of type I bovine collagen. Dermal fibroblasts from the donor are cultivated on the internal side of the bovine collagen matrix, and keratinocytes from the same donor are cultivated on the exterior. Orcel® functions as a biocompatible reabsorbable matrix, which provides a favorable environment for the migration of the host cells, due to cytokines and growth factors secreted by the allogeneic fibroblasts. According to the manufacturer, approximately 2 or 3 weeks after the application there should be no traces of allogeneic DNA in the wound5. Apligraft® is a bilaminar structure formed by type I bovine collagen gel populated by live neonatal fibroblasts coated with a layer of epithelial cells (neonatal keratinocytes)30. It is indicated for the treatment of chronic ulcers. According to a published study 31, this substitute was the only one of a series of dermal substitutes and autogenous skin grafts to provide statistically significant results in the treatment of venous ulcers in combination with a system of multi-layer compression.
Although we recognize the validity of this classification, it is limited by the inclusion of certain materials in Kumar's class I that should be considered as dressings. Therefore, the present study proposes a more didactic grouping of the different types of skin substitutes available that are most often mentioned in the literature.
METHODS
Proposed Classification of Skin Substitutes Used in the Plastic Surgery Service of FMUSP
A comprehensive classification of skin substitutes is proposed based on their categorization according to three criteria: the skin layer to be replaced, which is subdivided into epidermal (E), dermal (D) and dermal-epidermal composites (C); the durability in the wound bed, which is divided into temporary (T) and permanent (P); and the origin of the grafting material, which is divided into biological (b), biosynthetic (bs), and synthetic (s) (Figure 1).
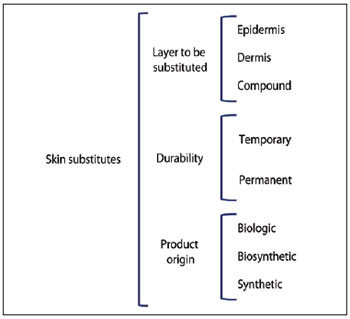
Figure 1 - Classification of skin substitutes proposed by the Plastic Surgery Service of Hospital das Clínicas of the School of Medicine of Universidade de São Paulo.
According to this classification, temporary (T) products refer to those that remain in the wound for the period of time necessary to modulate and improve the characteristics of the lesion, and are replaced by autogenous grafts. Permanent (P) materials are those that restore part or the total structure of the skin, and remain on the wound bed even after a possible grafting of autogenous skin for complete coverage of the lesion. Biologic substitutes (b) are those generated with biologic materials such as human or animal tissue, and synthetic (s) materials are produced in the laboratory with the aim of recreating the structure of the skin. Biosynthetic materials (bs) are those formed by a combination of synthetic components with elements of biological origin.
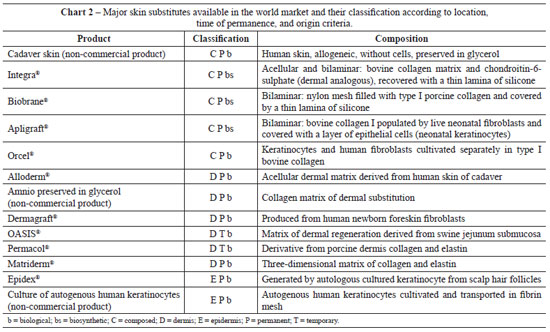
Chart 2 shows the most commonly used skin substitutes and their respective characteristics.
DISCUSSION
Skin substitutes play an important role in plastic surgery, in particular in the treatment of burns and other complex wounds, as they are a valuable resource for the restoration of cutaneous continuity5.
A review of the different types of skin substitutes available in the international market (there are few representatives in Brazil) revealed that their indications are quite accurate, although the cost-effectiveness of these materials should always be considered carefully, especially in Brazil, where they are marketed at a high cost. Despite the benefits of treatment with skin substitutes, their use is not covered by the Unified Health System (SUS), which makes their application difficult for the general population. The use of skin substitutes for the treatment of wounds is limited to certain hospitals (mainly University hospitals and private clinics), either as part of a research protocol or when the cost is assumed by the patient.
Considering the recent increase in the availability of skin substitutes in the world market and based on the fact that the incorporation of these techniques could benefit a significant number of patients, we reviewed the current literature on this subject, with special emphasis on studies seeking to systematize these products, and we describe currently accepted classifications such as that proposed by Kumar13.
Because the current classifications of skin products fail to group all the available products and define their indications, we proposed a new classification method that we consider to be more comprehensive and that may have a more practical application for plastic surgery. We included the culture of autogenous keratinocytes as an epidermal substitute (definitive) of biological origin, which had not been addressed in the classification by Kumar, and new products such as Dermagraft® were grouped with the already existing set.
Dermagraft® is a product manufactured from human neonatal foreskin fibroblasts, which are seeded in a matrix of bioabsorbable polyglactin. Fibroblasts proliferate, filling existing empty spaces in the matrix, and secrete collagen, other matrix proteins, growth factors, and cytokines, thus creating a three-dimensional dermal substitute containing live cells. Epidermal elements are present in this product32.
Our classification included the criterion of durability of the skin substitute on the wound bed. The literature is not clear on how to conceptualize such durability. Some researchers use the permanence of residues of the product in this bed as a measure of durability, as it seems that many of these products do not act primarily as tissue or cell replenishers, but as a stimulus for tissue repair, or they function as agents capable of releasing signals in the wound12.
The present literature review revealed that the use of biological materials (cadaver skin and cultivated tissues) for commercial ends is more liberal outside Brazil, where there is no specific legislation on these products and their study and application is therefore limited.
The Cell Culture Laboratory of the Plastic Surgery Service of Hospital das Clínicas of the School of Medicine of Universidade de São Paulo (HCFMUSP) has been developing cell culture techniques for many years to improve the clinical safety of dermal-epidermal substitutes for use in humans. In 2001, we published the first clinical transplant of cultivated epithelium33, and since then great efforts have been made to improve research in this area.
The keratinocyte cultivation technique utilized in this study was first described by Rheinwald and Green34, who produced stable human epithelium laminae for transplant. In this technique, the skin is digested by proteolytic enzymes that break down cell adhesion proteins and release a suspension of keratinocytes and fibroblasts. Keratinocytes reproduce in culture flasks over a single layer of fibroblasts under controlled proliferation rates, while the signaling required for the coordinated multiplication of keratinocytes remains functional. Cultured keratinocyte autografts have been used in association with dermal matrices for the treatment of burns, lower limb ulcers, mucosal defects, or after excision of giant congenital nevus33. The isolated transplant of cultivated keratinocytes has been associated with several problems such as low rate of integration to the recipient bed, sensitivity to infection and, in particular, fragility of the epithelial coverage, as the basal membrane reconstruction is poor and lacks the dermal component to provide greater structural stability to the new tissue. The cultivation of keratinocytes on an acellular dermal matrix has been described by many authors, and the objective of this type of tissue engineering is to obtain a tissue with improved quality, lower friability, and increased resistance to trauma6, or a tissue that is more similar to "artificial skin."
Similar to Lazic and Falanga11, we believe that the bioengineering of this tissue may result in great advances in the clinical and/or surgical treatment of wounds, as it will provide more knowledge of therapeutic agents that may interfere with the preparation of the bed of such wounds.
The identification of materials and the use of cell culture for the generation of skin substitutes is currently an area of active research, not only to identify the best type of skin substitute for each situation, but also to develop new products to cover wounds, reduce deformities, and provide better aesthetic results in less time and with lower costs.
The comprehensive classification proposed in this study aimed to include recent technological innovations to fulfill a need (in future works with specific clinical series) for a better categorization of products as well as the collection of data on their effectiveness supported by solid evidence.
REFERENCES
1. Ferreira MC, Tuma P Jr, Carvalho VF, Kamamoto F. Complex wounds. Clinics (São Paulo). 2006;61(6):571-8.
2. Atiyeh BS, Costagliola M. Cultured epithelial autograft (CEA) in burn treatment: three decades later. Burns. 2007;33(4):405-13.
3. Catena F, Ansaloni L, Gazzotti F, Gagliardi S, Di Saverio S, D'Alessandro L, et al. Use of porcine dermal collagen graft (Permacol) for hernia repair in contaminated fields. Hernia. 2007;11(1):57-60.
4. Rheinwald JG, Green H. Growth of cultured mammalian cells on secondary glucose sources. Cell. 1974;2(4):287-93.
5. Shores JT, Gabriel A, Gupta S. Skin substitutes and alternatives: a review. Adv Skin Wound Care. 2007;20(9 Pt 1):493-508.
6. Paggiaro AO, Isaac C, Bariani G, Mathor M, Herson MR, Ferreira MC. Construção de equivalente dermo-epidérmico in vitro. Rev Soc Bras Cir Plást. 2007;22(3):153-7.
7. Arrunátegui G. Enxertos combinados de derme alógena residual, preservada em glicerol, sobreposta por pele autógena, como cobertura definitiva de queimaduras profundas: relatos de caso [dissertação de mestrado]. São Paulo: Faculdade de Medicina da Universidade de São Paulo; 2006.
8. Mackie DP. The Euro Skin Bank: development and application of glycerol-preserved allografts. J Burn Care Rehabil. 1997;18(1 Pt 2):S7-9.
9. Atiyeh BS, Gunn SW, Hayek SN. State of the art in burn treatment. World J Surg. 2005;29(2):131-48.
10. Horch RE, Kopp J, Kneser U, Beier J, Bach AD. Tissue engineering of cultured skin substitutes. J Cell Mol Med. 2005;9(3):592-608.
11. Lazic T, Falanga V. Bioengineered skin constructs and their use in wound healing. Plast Reconstr Surg. 2011;127(Suppl 1):75S-90S.
12. Balasubramani M, Kumar TR, Babu M. Skin substitutes: a review. Burns. 2001;27(5):534-44.
13. Kumar P. Classification of skin substitutes. Burns. 2008;34(1):148-9.
14. Paggiaro AO. Efeitos da radiação ionizante em membranas amnióticas gliceroladas empregadas como substrato ao cultivo de epitélio [tese de doutorado]. São Paulo: Faculdade de Medicina da Universidade de São Paulo; 2011.
15. Kumar RJ, Kimble RM, Boots R, Pegg SP. Treatment of partial-thickness burns: a prospective, randomized trial using Transcyte. ANZ J Surg. 2004;74(8):622-6.
16. Ortega-Zilic N, Hunziker T, Läuchli S, Mayer DO, Huber C, Baumann Conzett K, et al. EpiDex® Swiss field trial 2004-2008. Dermatology. 2010;221(4):365-72.
17. Hafner J, Kuhne A, Trueb RM. Successful grafting with EpiDex in pyoderma gangrenosum. Dermatology. 2006;212(3):258-9.
18. Brown-Estris M, Cutshall W, Hiles M. A new biomaterial derived from small intestinal submucosa and developed into a wound matrix device. Wounds. 2002;14:150-66.
19. Demling R, Niezgoda J, Haraway G, Mostow E. Small intestinal submucosa wound matrix and full thickness venous ulcers. Wounds. 2004;16;18-23.
20. Niezgoda JA, Van Gils CC, Frykberg RG, Hodde JP. Randomized clinical trial comparing OASIS wound matrix to regranex gel for diabetic ulcers. Adv Skin Wound Care. 2005;18(5 Pt 1):258-66.
21. Harper C. Permacol: clinical experience with a new biomaterial. Hosp Med. 2001;62(2):90-5.
22. Parker DM, Armstrong PJ, Frizzi JD, North JH Jr. Porcine dermal collagen (Permacol) for abdominal wall reconstruction. Curr Surg. 2006;63(4):255-8.
23. Haslik W, Kamolz LP, Nathschläger G, Andel H, Meissl G, Frey M. First experiences with the collagen-elastin matrix Matriderm as a dermal substitute in severe burn injuries of the hand. Burns. 2007;33(3):364-8.
24. Wainwright DJ. Use of an acellular allograft dermal matrix (AlloDerm) in the management of full-thickness burns. Burns. 1995;21(4):243-8.
25. Gibson T, Medawar PB. The fate of skin homografts in man. J Anat. 1943;77(Pt 4):299-310.
26. Shuck JM, Pruitt BA Jr, Moncrief JA. Homograft skin for wound coverage. A study of versatility. Arch Surg. 1969;98(4):472-9.
27. Burke JF, Yannas IV, Quinby WC Jr, Bondoc CC, Jung WK. Successful use of a physiologically acceptable artificial skin in the treatment of extensive burn injury. Ann Surg. 1981;194(4):413-28.
28. Groos N, Guillot M, Zilliox R, Braye FM. Use of an artificial dermis (Integra) for the reconstruction of extensive burn scars in children. About 22 grafts. Eur J Pediatr Surg. 2005;15(3):187-92.
29. Cassidy C, St Peter SD, Lacey S, Beery M, Ward-Smith P, Sharp RJ, et al. Biobrane versus duoderm for the treatment of intermediate thickness burns in children: a prospective, randomized trial. Burns. 2005;31(7):890-3.
30. Falanga V, Sabolinski M. A bilayered living skin construct (APLIGRAF) accelerates complete closure of hard-to-heal venous ulcers. Wound Repair Regen. 1999;7(4):201-7.
31. Jones JE, Nelson EA. Skin grafting for venous leg ulcers. Cochrane Database Syst Rev. 2005;(1):CD001737.
32. Marston WA, Hanft J, Norwood P, Pollak R; Dermagraft Diabetic Foot Ulcer Study Group. The efficacy and safety of Dermagraft in improving the healing of chronic diabetic foot ulcers: results of a prospective randomized trial. Diabetes Care. 2003;26(6):1701-5.
33. Herson MR, Mathor MB, Altran S, Capelozzi VL, Ferreira MC. In vitro construction of a potential skin substitute through direct human keratinocyte plating onto decellularized glycerol-preserved allodermis. Artif Organs. 2001;25(11):901-6.
34. Rheinwald JG, Green H. Serial cultivation of strains of human epidermal keratinocytes: the formation of keratinizing colonies from single cells. Cell. 1975;6(3):331-43.
1. Full professor of the Discipline of Plastic Surgery at Hospital das Clínicas of the School of Medicine, Universidade de São Paulo (HC-FMUSP), São Paulo, Brazil.
2. Doctor, head of the Tissue Bank of the Central Institute of HCFMUSP, São Paulo, Brazil.
3. Doctor, head of the Laboratory of Cell Culture of the Department of Plastic Surgery at HCFMUSP, São Paulo, Brazil.
4. Resident physician of the Discipline of Plastic Surgery at HCFMUSP, São Paulo, Brazil.
5. Resident physician of the Discipline of General Surgery at HCFMUSP, São Paulo, Brazil.
Correspondence to:
Cesar Isaac
Av. Doutor Arnaldo, 455 - sala 1.360 - Pinheiros
São Paulo, SP, Brazil - CEP 01246-903
E-mail: cesaris@plastica.fm.usp.br
Submitted to SGP (Sistema de Gestão de Publicações/Manager Publications System) of RBCP (Revista Brasileira de Cirurgia Plástica/Brazilian Journal of Plastic Surgery).
Paper received: July 25, 2011
Paper accepted: August 13, 2011
Study conducted at Hospital das Clínicas of the School of Medicine, Universidade de São Paulo, São Paulo, Brazil.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter