

Case Reports - Year 2011 - Volume 26 -
Reversed hemisoleus flap for wound coverage in the distal third of the leg
Retalho hemissolear reverso na reconstrução de defeito do terço distal da perna
ABSTRACT
Reconstruction of the distal third of the leg represents a challenge for many plastic surgeons. Although microsurgical flaps have been the method of choice for this reconstruction, many hospitals do not have equipment or microsurgical staff trained for this type of procedure. Moreover, the patient's clinical condition does not allow a more complex surgery in some cases. This study reports two cases of reconstruction of the distal third of the leg with reverse flap of the soleus muscle, based on the perforators of the posterior tibial artery, as an alternative to microsurgical flaps. The reverse soleus flap had an excellent outcome with short surgical duration, easy implementation, excellent resolution, and low morbidity of the donor area.
Keywords: Lower extremity. Soft tissue injuries. Surgical flaps. Muscle, skeletal.
RESUMO
A reconstrução do terço distal da perna representa um desafio para muitos cirurgiões plásticos. Usualmente, os retalhos microcirúrgicos têm sido considerados de escolha para essas reconstruções; no entanto, muitos hospitais ainda não dispõem de equipamentos ou equipe microcirúrgica treinada nesse tipo de procedimento, além dos casos em que as condições clínicas do paciente não permitem uma cirurgia de maior porte. O presente trabalho propõe o relato de dois casos de reconstrução do terço distal da perna com retalho reverso do músculo solear, baseado nas perfurantes da artéria tibial posterior, como alternativa aos retalhos microcirúrgicos. O retalho solear reverso apresentou excelente resultado, com pequeno tempo cirúrgico, fácil realização, excelente resolubilidade e pouca morbidade da área doadora.
Palavras-chave: Extremidade inferior. Lesões dos tecidos moles. Retalhos cirúrgicos. Músculo esquelético.
Reconstruction of the distal third of the leg represents a challenge for many plastic surgeons. Although the microsurgical flap has been the method of choice for this reconstruction1-5, many hospitals do not have equipment or microsurgical staff trained for this type of procedure. In other cases, the patients are not candidates for microsurgical reconstruction because of their clinical conditions, and the surgeon is therefore required to use alternative treatments1-5.
Often, defects in the lower third of the leg quickly result in the exposure of relevant structures such as bone and tendon, the correction of which requires the performance of a safe reconstruction with a well-vascularized tissue3,4.
The soleus muscle is located in the posterior region of the leg, inferior to the gastrocnemius muscles, and is classified as type II according to the classification of Mathes and Nahai. Its major pedicle is the posterior tibial artery, and the perforating branches of this artery are the secondary pedicles3,4.
The soleus muscle is frequently used for the reconstruction of defects of the middle third of the leg, based on its major pedicle. However, the viable use of the soleus muscle in a reverse manner, based on its secondary pedicles, has been described by several authors for the reconstruction of defects of the lower third of the leg as an alternative to the use of microsurgical flaps1-8.
An advantage of using the hemisoleus flap rather than the entire soleus muscle flap is the preservation of plantar flexion of the foot performed by the lateral portion of the muscle, which is left in its original location. Moreover, the medial flap has a greater rotation angle than that of a conventional soleus muscle flap1-4. The medial part of the muscle is supplied in its whole length by perforators of the posterior tibial artery. Because of this constant arterial supply, the medial part of the soleus muscle is viable as a flap distally based in a reverse manner1-4.
This study reports two cases of reconstruction of defects of the lower third of the leg with the use of the reverse hemisoleus flap.
CASE REPORTS
Surgical Technique
The patients were placed in the supine position during the procedure. An incision was made in a line 2 cm medial to the medial edge of the tibia; this incision provided wide access to the soleus muscle (Figure 1A). The muscle was dissected, and the secondary vascular pedicles were identified in the distal portion in order to provide a good arc of rotation. The muscle was subsequently divided longitudinally along the median raphe and downward, at the level of the distal perforators, and separated from the Achilles tendon. From the median raphe, the medial portion was dissected from the lateral and was sectioned in the joint between the proximal and middle thirds (Figure 1B). The medial muscle was transferred to the locality of the defect as a reverse hemisoleus flap while avoiding tension and was fastened with 4.0 nylon thread (Figure 1C). The donor area was primarily closed with separate 4.0 nylon sutures, and a suction drain was placed (Figure 1D). During a second surgery, skin grafting was performed over the open area of the muscle flap. Subsequently, the patient was oriented for rest with the limb elevated for 4 to 5 days to avoid edema and congestion in the flap.
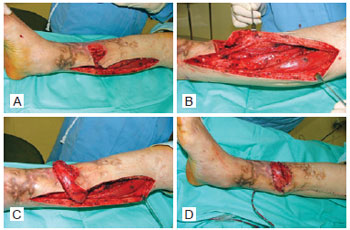
Figure 1 - Surgical technique. In A, area of the debrided lesion and medial lesion in the leg for access to the soleus muscle. In B, exposure and dissection of the soleus muscle. In C, rotation of the medial portion of the soleus muscle and coverage of the lesion area. In D, primary synthesis of the donor area and coverage of the previous exposed area by the reverse soleus muscle.
Case 1
A 26-year-old male patient had a lesion in the distal third of the right leg that had not healed for one year following a car accident. During the physical examination, a lesion of 6 cm × 5 cm (30 cm2) was identified with bone exposure in its central portion (Figure 2). On August 15, 2005, the patient underwent wide debridement of the lesion, including the exposed bone portion, in which reconstruction of the defect was performed with the reverse soleus muscle flap according to the described technique. The patient was discharged on the second postoperative day. The flap showed total survival and was grafted on the seventh postoperative day, resulting in total integration of the skin graft. The lesion has not recurred up to the present date.
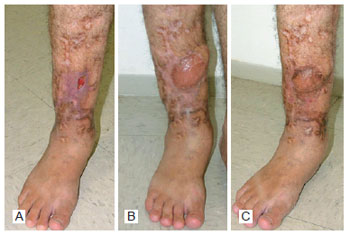
Figure 2 - Case 1. In A, preoperative period, revealing the ulcerated lesion with bone exposure. In B, postoperative period of three months. In C, postoperative period of nine months.
Case 2
A 19-year-old male patient had a lesion in the distal third of the right leg that had not healed for more than three years following a car accident, in which he had suffered a tibial fracture with vascular lesion of the popliteal artery. Vascular reconstruction was performed immediately after the trauma with grafting of the saphenous vein of the popliteal artery to the tibiofibular trunk. During the physical examination, a lesion of 4 cm × 12 cm (48 cm2) was identified with bone exposure in the central portion. Arteriography of the right lower limb, performed before the reconstruction, revealed absence of distal vascular impairment but presence of significant obstructions in the vascular graft. On March 30, 2009, the patient underwent reconstruction of the defect with the reverse soleus muscle flap. At the moment of flap production, atrophy of the entire posterior muscles of the leg was observed; however, the hemisoleus flap production was suitable for coverage of the bone defect. The patient was discharged on the second postoperative day. The flap showed total survival and was grafted 21 days after the surgery, resulting in total integration of the skin graft.
DISCUSSION
The reverse hemisoleus muscle flap, initially proposed by Tobin in 1985, involves the use of the medial part of the soleus muscle for reconstruction of the medial and distal parts of the lower limb with narrow tibial exposures and irrigation based on the posterior tibial artery perforators1,2.
In these cases, the use of the medial region of the soleus muscle is preferable because of its larger rotation arch, excellent irrigation, and lower functional sequelae in the donor area when compared to the use of the entire soleus muscle or even the gastrocnemius. This flap is easily prepared and can be ready in a period of up to two hours, thus reducing the risk of procedure morbidity in at-risk patients3.
Both proximal and distal portions of the soleus muscle can be used for small proximal tibial defects of the distal third of the leg, generally at a distance of more than 5 cm from the medial malleolus. For more distal defects, the proximal portion of the soleus muscle can be used in a reversed manner, often for coverage of the medial malleolus3.
In this study, we used the distal flap of the soleus muscle in a reverse manner, based on the distal perforators of the posterior tibial artery, in two cases with long-term tibial exposure with areas of 30 cm2 and 48 cm2. The use of the flap was successful in both cases. The procedure was performed in a quick and safe manner, and extensive morbidity was not observed in the donor area. The defect with exposure of the relevant area was suitably covered, and the patient did not have to undergo the prolonged surgical procedures of a microsurgical flap. However, this coverage was only possible because of the small size of the exposure, and it may be safer to use a microsurgical flap in cases with larger defects.
The reverse hemisoleus flap can be used for defects of up to 50 cm2, but flap impairment is possible in cases where these measures are exceeded. This flap should not be used for patients with significant peripheral vascular disease or in some cases of diabetes3-5.
In addition to the advantages already discussed, another relevant point is the hospital cost of the procedures. Thornton et al.7 compared the hospital costs between the reverse soleus flap and microsurgical flaps in patients with similar profiles and defects and observed that the hospitalization time, surgical time, hospital expenses, and the use of the intensive care unit were significantly lower in the group of patients undergoing soleus flap reconstruction. Therefore, when this type of reconstruction is possible, it constitutes the first choice for these authors.
Beck et al.8 compared several flaps for treatment of defects in the middle third of the leg by using the gastrocnemius muscle, fasciocutaneous flaps, free flaps, and reverse soleus flap. The reverse soleus was the only flap in this series that did not present complications, and the authors concluded that it is an excellent option when its use is possible.
Schierle et al.9, who observed several cases of necrosis of this flap, inferred that the retrograde blood supply in the distal portion of the flap continues to be problematic even when the "critical perforators" are preserved. In these cases, the authors applied the angiosomes principles proposed by Taylor and Palmer in 1987 and concluded that this procedure can help resolve this limitation and improve the outcome of the distally based hemisoleus flap. Recent experiments with single perforator flaps have assured surgeons that the flap can be elevated and transferred with only one or two perforators, according to the angiosomes principles.
In cases of fasciocutaneous flaps, in which the reverse sural artery is used, the major limitation is venous congestion; this leads to problems in flap viability associated with compression of the pedicle when a subdermal tunnel is used for transposition and positioning10. The major disadvantages are unsightly scars in the donor area of the flap and lateral hypoesthesia of the foot10. The reverse soleus flap is safer in this regard because venous congestion of the flap is absent. Furthermore, the wide rotation arc enables better aesthetics of the donor area without the discomfort of exposure of the donor area for at least two weeks, which is required when using fasciocutaneous flaps.
CONCLUSIONS
The reverse hemisoleus flap is safe, well-vascularized, easy to prepare, and is well-implemented in cases of small defects of the distal third of the leg that require good coverage of essential structures. The reported cases demonstrated excellent resolution, good progress, and insignificant sequelae in the donor area. The authors propose that the reverse hemisoleus muscle flap is a good option for select reconstructions performed in the lower third of the leg.
REFERENCES
1. Pu LL. The reversed medial hemisoleus muscle flap and its role in reconstruction of an open tibial wound in the lower third of the leg. Ann Plast Surg. 2006;56(1):59-63.
2. Pu LL. Soft-tissue coverage of an open tibial wound in the junction of the middle and distal thirds of the leg with the medial hemisoleus muscle flap. Ann Plast Surg. 2006;56(6):639-43.
3. Pu LL. Soft-tissue reconstruction of an open tibial wound in the distal third of the leg: a new treatment algorithm. Ann Plast Surg. 2007;58(1):78-83.
4. Pu LL. Successful soft-tissue coverage of a tibial wound in the distal third of the leg with a medial hemisoleus muscle flap. Plast Reconstr Surg. 2005;115(1):245-51.
5. Pu LL. Further experience with the medial hemisoleus muscle flap for soft-tissue coverage of a tibial wound in the distal third of the leg. Plast Reconstr Surg. 2008;121(6):2024-8.
6. Kauffman CA, Lahoda LU, Cederna PS, Kuzon WM. Use of soleus muscle flaps for coverage of distal third tibial defects. J Reconstr Microsurg. 2004;20(8):593-7.
7. Thornton BP, Rosenblum WJ, Pu LL. Reconstruction of limited soft-tissue defect with open tibial frature in the distal third of the leg: a cost and outcome study. Ann Plast Surg. 2005;54(3):276-80.
8. Beck JB, Stile F, Lineaweaver W. Reconsidering the soleus muscle flap for coverage of wounds of the distal third of the leg. Ann Plast Surg. 2003;50(6):631-5.
9. Schierle CF, Rawlani V, Galiano RD, Kim JY, Dumanian GA. Improving outcomes of the distally based hemisoleus flap: principles of angiosomes in flap design. Plast Reconstr Surg. 2009;123(6):1748-54.
10. Garcia AMC. Retalho sural reverso para reconstrução distal da perna, tornozelo, calcanhar e do pé. Rev Bras Cir Plást. 2009;24(1):96-103.
1. Doctoral candidate in Surgery, full member of the Brazilian Society of Plastic Surgery (SBCP), preceptor of Medical Residency in Surgery at Hospital Geral de Fortaleza, Fortaleza, CE, Brazil.
2. Aspiring member of the SBCP, resident physician at the Plastic Surgery Service of Hospital Geral de Fortaleza, Fortaleza, CE, Brazil.
3. Full member of the SBCP, head of clinic and head of the Plastic Surgery Service of Hospital Geral de Fortaleza, Fortaleza, CE, Brazil.
Correspondence to:
Marcus Vinicius Ponte de Souza Filho
Rua Nenê Gonçalves Barreira, 70 - Casa 9 - Cambeba
Fortaleza, CE, Brazil - CEP 60822-145
E-mail: mvponte@ig.com.br
Submitted to SGP (Sistema de Gestão de Publicações/Manager Publications System) of RBCP (Revista Brasileira de Cirurgia Plástica/Brazilian Journal of Plastic Surgery).
Paper received: February 1, 2010
Paper accepted: April 6, 2011
Study conducted at Hospital Dr. Waldemar de Alcântara - Hospital Geral de Fortaleza - Health Secretary of the State of Ceará (SESA), Fortaleza, CE, Brazil.


 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter