

Original Article - Year 2022 - Volume 37 -
Scrotal reconstruction after Fournier's gangrene
Reconstrução escrotal após gangrena de Fournier
ABSTRACT
Introduction: Fournier's gangrene is a polybacterial infection, usually caused by anaerobic and aerobic bacteria, characterized by scrotal and perineal necrotizing fasciitis. Its treatment is based on surgical intervention by excision of the necrotic area and early antibiotic therapy. There are several strategies to reconstruct the defect resulting from debridement, and it should be noted that tissue losses greater than 50% are usually reconstructed with flaps.
Methods: Retrospective analysis of the series of cases of scrotal reconstruction after Fournier's gangrene performed by the authors throughout 2020, totaling eight patients.
Results: The most used flap was thigh fasciocutaneous flap, which presented a partial necrosis rate of 14.29%, without total necrosis. In one of the cases, it was possible to reconstruct a spongy urethra with gracilis muscle without fistulization, preventing the patient from undergoing a definitive urethrostomy. As for complications, the occurrence of minor complications that required simple revision procedures was common. The prevalence of 75% of diabetes mellitus in our series is highlighted, which may have negatively interfered with the healing process.
Conclusion: Scrotal reconstruction with flaps is important to accelerate wound healing from Fournier gangrene debridement and to maintain the pouch aspect necessary for testicular thermoregulation. Our primary option was thigh fasciocutaneous flap, which proved to be safe. And minor complications were frequent in this series, without compromising the final result.
Keywords: Fournier gangrene; Fasciitis; Fasciitis, necrotizing; Scrotum; Reconstructive surgical procedures.
RESUMO
Introdução: Gangrena de Fournier é uma infecção polibacteriana, geralmente causada por bactérias anaeróbias e aeróbias, sendo caracterizada por fasciite necrosante escrotal e perineal. Seu tratamento é embasado em intervenção cirúrgica com excisão da área necrótica e antibioticoterapia precoces. Diversas são as estratégias de reconstrução do defeito resultante do desbridamento, devendo ser salientado que perdas teciduais maiores do que 50% costumam ser reconstruídas com retalhos.
Métodos: Análise retrospectiva da série de casos de reconstrução escrotal após gangrena de Fournier procedidos pelos autores ao longo de 2020, totalizando oito pacientes.
Resultados: O retalho mais utilizado foi o fasciocutâneo de coxa, que apresentou taxa de necrose parcial de 14,29%, sem necrose total. Em um dos casos foi possível reconstruir uma uretra esponjosa com músculo grácil sem fistulização, evitando que o paciente fosse submetido a uma uretrostomia definitiva. Quanto às complicações, foi comum a ocorrência de intercorrências menores que necessitaram de procedimentos revisionais simples. Destaca-se a prevalência de 75% de diabetes mellitus em nossa casuística, o que pode ter interferido negativamente no processo cicatricial.
Conclusão: A reconstrução escrotal com retalhos é importante para acelerar a cicatrização da ferida proveniente do desbridamento de gangrena de Fournier e para manter o aspecto de bolsa necessário para a termorregulação do testículo. Nossa opção primária foi o retalho fasciocutâneo de coxa, que se mostrou seguro. Pequenas intercorrências foram frequentes nesta série, sem comprometimento do resultado final.
Palavras-chave: Gangrena de Fournier; Fasciite; Fasciite necrosante; Escroto; Procedimentos cirúrgicos reconstrutivos.
INTRODUCTION
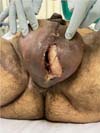
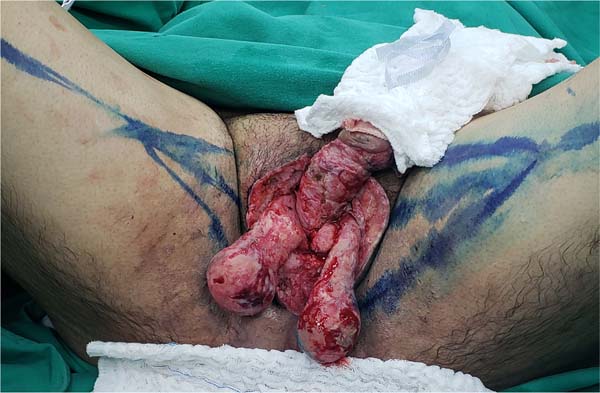
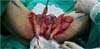
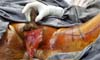
Fournier’s gangrene (Figure 1) is a term that was first described in 1883 by Alfred Fournier to designate necrotizing fasciitis that affects the scrotum and perineum. It has a polybacterial etiology, usually caused by anaerobic and aerobic bacteria1. It is an infection of rapid progression, with a high potential for severity (high rates of morbidity and mortality), being more common in males2. Its risk factors are diabetes mellitus, alcoholism, obesity, local trauma, perianal and perineal infections, and surgical procedures in the region1. The treatment is based on surgical intervention with early excision of the necrotic area and antibiotic therapy, which may require reapproaches with the expansion of the debrided area2.
There are several strategies for reconstructing the bloody area resulting from debridement. Small wounds with tissue loss of up to 50% of the scrotum can generally be treated with secondary intention healing, primary synthesis and skin grafting. Larger losses are usually treated using skin, fasciocutaneous or myocutaneous flaps2.
In this article, the authors’ reconstructive strategies after the debridement of eight patients with Fournier’s gangrene will be analyzed, with the fasciocutaneous thigh flap as the first option.
OBJECTIVE
To evaluate the outcome of scrotal reconstructions performed by the authors after debridement of Fournier’s gangrene and whether there are any complicating factors such as comorbidities and/or alteration of laboratory tests.
METHODS
The authors performed a retrospective analysis of the series of cases of scrotal reconstruction after Fournier’s gangrene throughout 2020 (Table 1). In all cases, one or both testicles were exposed. Medical records, photo files, albumin, and complete blood count tests were accessed immediately before the reconstructive surgical stage.
| Patient | Age | GL | Hb | CRP | Comorbidities | Technique | Complications | Revision |
|---|---|---|---|---|---|---|---|---|
| W.R.G. | 46 | 10100 | 9.3 | 129.82 | SAH | Bilateral fasciocutaneous thigh flaps | Dehiscence | Two z-plasties, resection of excess skin |
| S.H.M.F. | 47 | 2786 | 7.46 | 35.8 | DM | Unilateral thigh fasciocutaneous flap | No complications | None |
| G.M.A. | 60 | 11540 | 10.65 | 42.5 | SAH, DM, CAD | Gracilis myocutaneous flap | Partial skin island necrosis | Debridement |
| R.A.P. | 46 | 4312 | 10.03 | 2.6 | Alcoholism | Unilateral thigh fasciocutaneous flap | Epidermolysis | None |
| R.L.A. | 74 | 12800 | 9.28 | 149.8 | SAH, MD | Primary closure | Dehiscence | None |
| J.B.L. | 48 | 6100 | 10.6 | 122 | DM | Unilateral thigh fasciocutaneous flap | Partial necrosis | Debridement and edge reapproximation |
| A.F.S | 51 | 6940 | 9.8 | 30.7 | SAH, MD | Unilateral thigh fasciocutaneous flap thigh | Epidermolysis | Debridement and edge reapproximation |
| R.D.G.F. | 48 | 6140 | 11.9 | 6.3 | SAH, DM, asthma | Unilateral thigh fasciocutaneous flap | Dehiscence | None |
GL=WBC total (WBC/microL); Hb=hemoglobin (g/dL); CRP=C-reactive protein (mg/L); SAH=systemic arterial hypertension); DM=diabetes mellitus; CAD=coronary artery disease
The total number of patients was eight, and the primary surgical option was the fasciocutaneous thigh flap, which was used on six occasions. The two exceptions were due to a urethral injury or inadequate clinical conditions for a larger reconstruction.
RESULTS
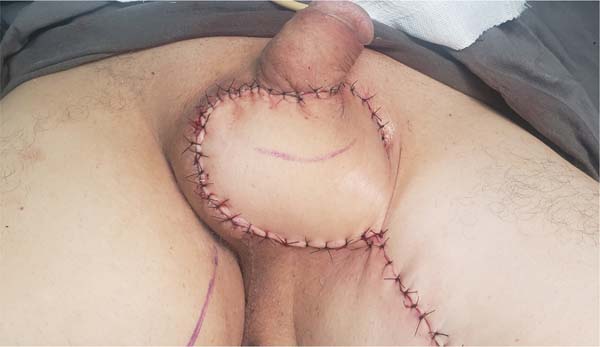
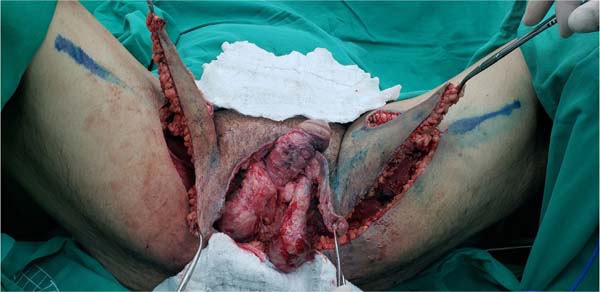
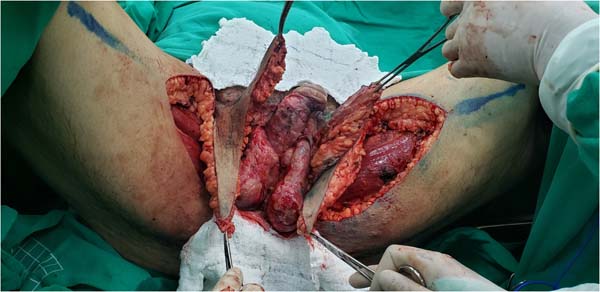
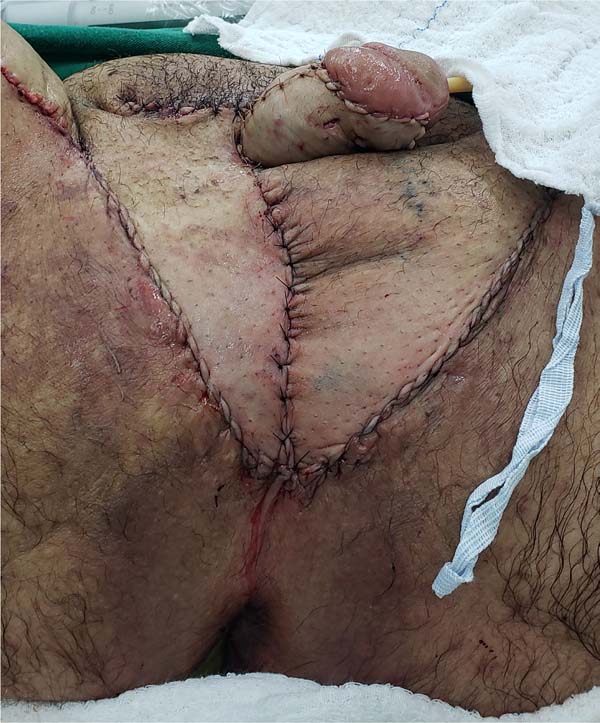
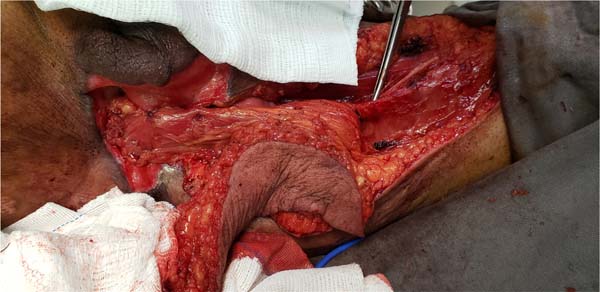
The authors’ first option for making the neoscrotum after debridement of Fournier’s gangrene was the unilateral thigh fasciocutaneous flap (Figures 2 to 5). Using two flaps from both thighs was reserved for a patient with a more extensive open wound (Figures 6 to 10). There was no case of total necrosis. One of the seven flaps performed evolved with partial necrosis, which is equivalent to a rate of vascular damage of 14.29%.
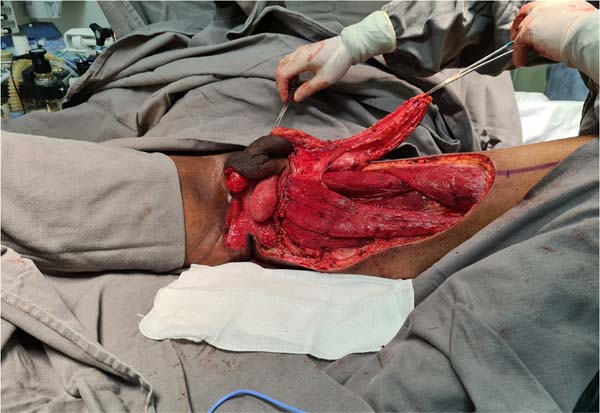
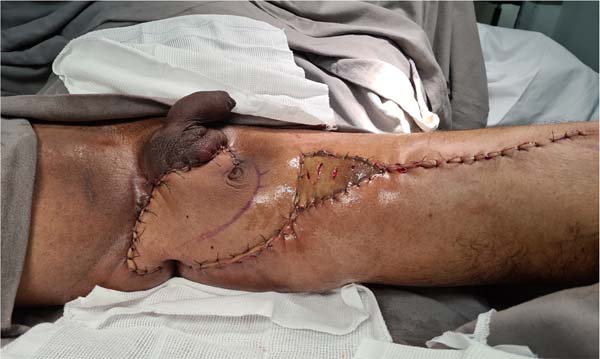
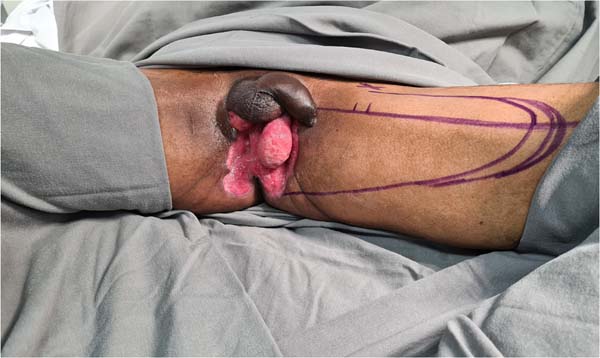
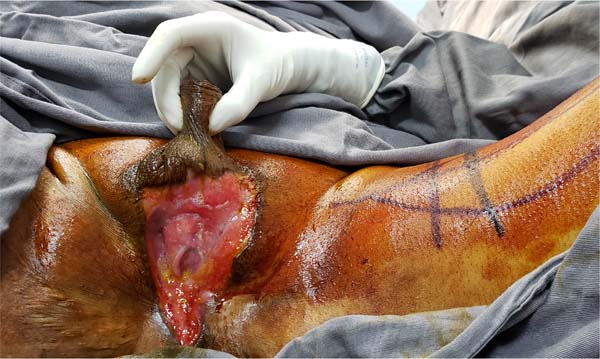
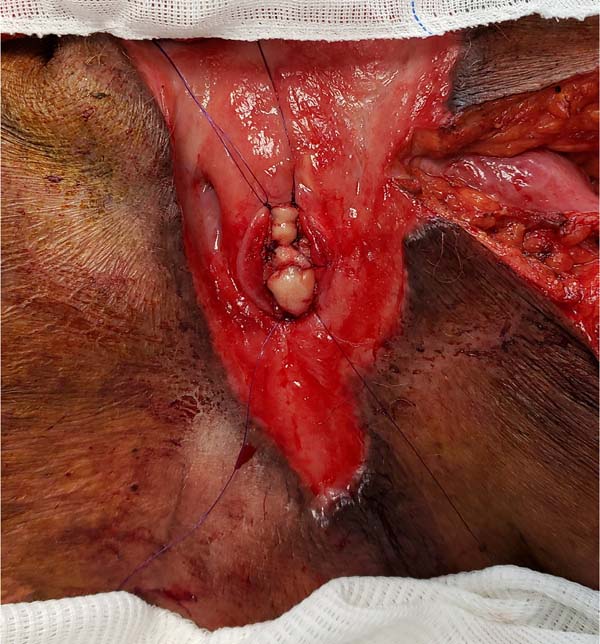
Another flap used in the series was the gracilis myocutaneous flap due to a urethral injury (Figures 11 to 14). There was an evolution to partial suffering of the island of skin, but the muscle tissue remained viable, making it possible to remove the urethral indwelling bladder probe and obtain a good urinary stream.
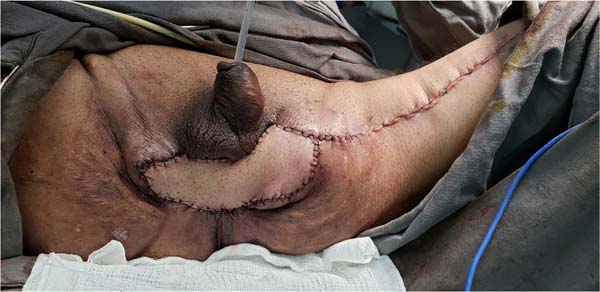
And in one of the patients, we opted for the primary synthesis of the wound edges post-Fournier because he was elderly, hypertensive, diabetic, malnourished and with significant anemia, which made reconstruction using flaps unfeasible.
In addition to the two already mentioned partial necroses, five cases had minor complications: three dehiscences and two epidermolysis. As a result, four of the eight patients underwent simple revision procedures: three debridements, two of which also had the edges reapproximated, and one improvement in the aesthetic appearance through resection of excess skin and two zetaplasties.
It should be noted that the average time between the initial debridement and the reconstructive stage was 29 days. The average age of the eight patients was 52 years and six months.
As for comorbidities, the most frequent were diabetes mellitus and arterial hypertension, with respective prevalences of 75% and 62.50%. Asthma, coronary artery disease and alcoholism were also reported in 1/8 of the cases, which corresponds to a prevalence of 12.50% for each of these disorders. Regarding the preoperative revisions of the reconstructions, the averages of global leukocytes, hemoglobin and C-reactive protein were, respectively: 7590 leukocytes/microL, 9.88g/dL and 64.94mg/L.
DISCUSSION
The fasciocutaneous flap of the thigh was our main reconstructive choice because it has a reliable vascular supply with a good range of rotation, thin skin, does not leave exposed scars, is easy to perform technically, and because it preserves the musculature. On the other hand, color incompatibility, low skin sensitivity1, and possibly inadequate thickness have been described in very obese patients.
The initial step in its marking is to draw a line from the pubic tubercle to the medial condyle of the tibia, which is the insertion site of the “pars anserina.” The vascular pedicle is then preserved in the superomedial region, and the flap length is determined according to the amount of tissue required to perform the transposition.
In most cases, using only one flap was preferred because the scrotal defects were smaller and to shorten the surgical time. The disadvantages of the unilateral flap are mentioned: the lack of mimicry of the median raphe and the greater chance of the tip suffering with the increase in the length X width ratio. Two of the five cases of unilateral thigh fasciocutaneous flap presented distal epidermolysis, while one evolved with partial necrosis. Probably something that contributed to this necrosis was the patient’s disrespect for postoperative rest.
A possible technical refinement of the thigh fasciocutaneous flap is using only one perforator of the medial circumflex femoral artery1,2. Other flaps that repair a scrotal defect are superficial circumflex iliac artery perforator flap3, free or pedicled greater omentum flap4,5, bilateral gracilis muscle flap6,7, anterolateral thigh flap8, inguinal flap (McGregor’s)9 and associated flaps to the use of expander10.
The main disadvantages of some of these techniques, which prevented them from being our choices, are high morbidity from laparotomy or laparoscopy and the possibility of inguinal hernia with the use of a great omentum flap, need for a skin graft for the omentum techniques and the bilateral gracilis muscle flap; possibility of tissue expander extrusion when it is positioned close to a contaminated wound.
Rarely, there is urethral involvement due to Fournier’s gangrene, given that the vascular supply of the urethra is different compared to the skin, subcutaneous tissue and fascia1. As muscle flaps increase oxygen tension and, consequently, reduce the chance of urinary fistulization, we preferred the gracilis myocutaneous flap in cases in which urethral reconstruction was necessary. This muscle is Mathes and Nahai type II, with the main vascular contribution being the medial femoral circumflex artery, which is located approximately 6-10 cm from the pubic tubercle1.
A jugal mucosal graft was also used on the posterior wall of the injured spongy urethra. The skin island of the myocutaneous flap was used to close the scrotal wound but evolved with partial necrosis and subsequent need for debridement. Perhaps an option with less probability of intercurrences would be the gracilis muscle flap associated with a partial skin graft instead of the gracilis myocutaneous flap. The balance was extremely positive since the chances of a definitive urethrostomy were not small.
In the case we primarily repaired the scrotal wound, the initial choice was early dehospitalization and postponement of reconstruction in better clinical conditions. However, the patient’s social context did not allow this strategy. This highlights the difficulty and complexity of managing surgical reconstructions in public health, where a vulnerable population is more frequent than in private services. We believe that this is a determining factor for surgical outcomes.
Other factors that may have had an unfavorable impact on the patients’ evolution are 1) High prevalence of comorbidities, especially diabetes mellitus; 2) Maintenance of an inflammatory state at the time of reconstruction, as evidenced by the C-reactive protein value; 3) Presence of anemia.
It is noteworthy that, concerning simpler reconstructive options, healing by secondary intention takes time and results in a poor aesthetic appearance6; while skin grafting promotes a desirable thin coverage, its fixation in the perineal region is difficult. In addition, the graft can adhere to the testicles and cause contractures that hinder the cremasteric reflex necessary for the testicles not to be affected by external conditions10. So, although there is no consensus on the best surgical option, flaps accelerate the healing process and maintain the aspect of the scrotum necessary for thermoregulation of the testicle2.
CONCLUSION
Scrotal reconstruction with flaps is important to accelerate wound healing from Fournier’s gangrene debridement and to maintain the pouch appearance necessary for testicular thermoregulation. Our primary option was the thigh fasciocutaneous flap, which proved safe, with a partial necrosis rate of 14.29% and without total necrosis. It was also possible to reconstruct a spongy urethra with gracilis muscle without fistulization, preventing the patient from undergoing a definitive urethrostomy. As for complications, the occurrence of minor intercurrences that require simple revision procedures is common. This may result from important associated comorbidities and patients’ clinical conditions during reconstructive plastic surgery.
REFERENCES
1. Coskunfirat OK, Uslu A, Cinpolat A, Bektas G. Superiority of medial circumflex femoral artery perforator flap in scrotal reconstruction. Ann Plast Surg. 2011;67(5):526-30.
2. Mello DF, Helene Júnior A. Scrotal reconstruction with superomedial fasciocutaneous thigh flap. Rev Col Bras Cir. 2018;45(1):e1389.
3. Han HH, Lee JH, Kim SM, Jun YJ, Kim YJ. Scrotal reconstruction using a superficial circumflex iliac artery perforator flap following Fournier’s gangrene. Int Wound J. 2016;13(5):996-9.
4. Delgado R, Ciudad P, Espinoza FB, Lopez J. Minimal invasive laparoscopic harvest of the greater omental flap for Fournier’s gangrene scrotal reconstruction. J Plast Reconstr Aesthet Surg. 2019;72(2):335-54.
5. Ng D, Tang CB, Kadirkamanathan SS, Tare M. Scrotal reconstruction with a free greater omental flap: A case report. Microsurgery. 2010;30(5):410-3.
6. Katusabe LJ, Balumuka D, Hodges A. Scrotal reconstruction with a pedicled gracilis muscle flap after debridement of Fournier’s gangrene: a case report. East Afr Med J. 2013;90(11):375-8.
7. Banks DW, O’Brien 3rd DP, Amerson JR, Hester Jr TR. Gracilis musculocutaneous flap scrotal reconstruction after Fournier gangrene. Urology. 1986;28(4):275-6.
8. Yu P, Sanger JR, Matloub HS, Gosain A, Larson D. Anterolateral thigh fasciocutaneous flap island flaps in perineoscrotal reconstruction. Plast Reconstr Surg. 2002;109(2):610-6. Discussion 617-8.
9. Ghahestani SM, Hekmati P, Karimi S. A new technique of scrotoplasty following total scrotal destruction by raised rotated perineal flaps with de epithelialized borders. Urol J. 2019;16(2):221-3.
10. Atik B, Tan O, Ceylan K, Etlik O, Demir C. Reconstruction of wide scrotal defect using superthin groin flap. Urology. 2006;68(2):419-22.
1. Hospital Metropolitano Odilon Behrens, Cirurgia Plástica, Belo Horizonte, MG, Brazil
2. Hospital Metropolitano Odilon Behrens, Cirurgia Geral, Belo Horizonte, MG, Brazil
3. Hospital Metropolitano Odilon Behrens, Urologia, Belo Horizonte, MG, Brazil
LRAS Analysis and/or interpretation of data, Final approval of the manuscript, Data collection, Conceptualization, Conception and design of the study, Project Management, Investigation, Methodology, Conducting operations and/or experiments, Writing - Preparation of the original, Writing - Review and Editing, Supervision, Validation, Visualization.
CRC Writing - Preparation of the original, Writing - Revision and Editing.
LFA Writing - Preparation of the original, Writing - Revision and Editing.
JP Writing - Preparation of the original, Writing - Revision and Editing.
JVMC Writing - Preparation of the original, Writing - Revision and Editing.
LSM Conceptualization, Conception and design of the study, Carrying out operations and/or experiments.
BFB Final approval of the manuscript, Supervision, Validation, Visualization.
Corresponding author: Leandro Ricardo de Aquino Santos Av. Professor Alfredo Balena, 189, 10º andar, Santa Efigênia, Belo Horizonte, MG, Brazil. Zip code: 30130-103, E-mail: leandroras@yahoo.com.br
Article received: November 25, 2021.
Article accepted: July 11, 2022.
Conflicts of interest: none.












 Read in Portuguese
Read in Portuguese
 Read in English
Read in English
 PDF PT
PDF PT
 Print
Print
 Send this article by email
Send this article by email
 How to Cite
How to Cite
 Mendeley
Mendeley
 Pocket
Pocket
 Twitter
Twitter